Immune System
Lymph Node - Pigment
Narrative
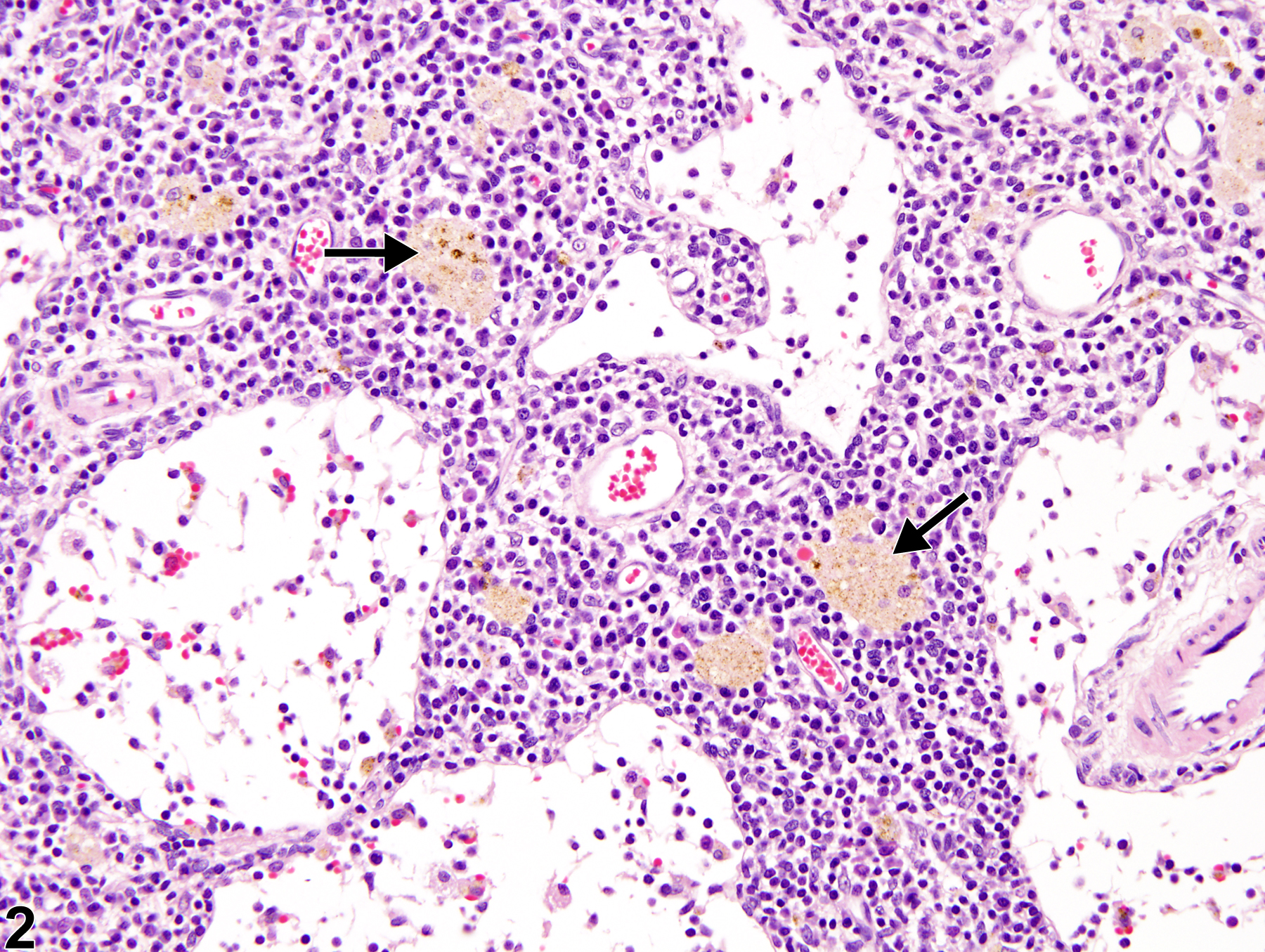
Pigment is a common finding in lymph nodes of control and treated rodents, particularly in the mesenteric and mandibular lymph nodes. Typically, pigment is seen within macrophages of the medullary sinuses and cords and may become increased as an effect of treatment. When specifically related to treatment, exogenous pigment is generally most prominent in lymph nodes regional to the route of test article administration. Hemosiderin (Figure 1, arrows) and ceroid/lipofuscin (Figure 2, arrows) are the most frequently encountered pigments. Hemosiderin is an iron-containing golden-brown granular material, and macrophages containing this pigment are typically observed with sinus erythrocytosis, congestion, or hemorrhage. Lipofuscin is also a yellow-brown, finely granular pigment; however, it is derived mainly from the breakdown products of lipids, such as cell membranes. Ceroid is a variant of lipofuscin that is acid-fast and autofluorescent. Differentiation of these pigments with 100% certainty using only conventional hematoxylin and eosin (H&E) staining is not possible. Hemosiderin can be identified with iron stains such as Perl’s iron and Prussian blue, both of which stain the pigment blue. Ceroid/lipofuscin may be identified with Sudan black B, Schmorl''s reaction, Oil Red O, carbol lipofuscin stain, periodic acid-Schiff, Ziehl-Neelsen acid-fast stain, autofluorescence, or lysosomal acid phosphatase and esterase stains. Melanin is another endogenous pigment that can be found within lymph nodes. This is a normal finding in black mice. Schmorl''s method and dopa-oxidase histochemical stains can be used to identify melanin pigment.
Pigment in lymph nodes should be diagnosed and given a severity grade. However, not all pigments have to be diagnosed, as some are ubiquitous in aging animals or related to some other disease process and not toxicologically meaningful. The pathologist should use his or her judgment in deciding whether deposits of pigment are toxicologically significant or prominent enough to warrant a separate diagnosis. Definitive pigment identification is often difficult in histologic sections, even with a battery of special stains. Therefore, it is recommended that a diagnosis of "pigment" (as opposed to diagnosing the type of pigment, e.g., hemosiderin or lipofuscin) is most appropriate. The pathology narrative should describe the morphologic features of the pigmentation.
Elmore SA. 2006. Enhanced histopathology of the lymph nodes. Toxicol Pathol 34:634-647.
Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1783683/Elmore SA. 2006. Histopathology of the lymph nodes. Toxicol Pathol 34:425-454.
Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1892634/Frith CH, Ward JM, Chandra M, Losco PE. 2000. Non-proliferative lesions of the hematopoietic system in rats. In: Guides for Toxicologic Pathology.TP/ARP/AFIP, Washington, DC.
Full Text: https://www.toxpath.org/docs/SSNDC/HematopoieticNonprolifRat.pdfNational Toxicology Program. 2010. NTP TR-558. Toxicology and Carcinogenesis Studies of 3,3’,4,4’-Tetrachloroazobenzene (TCAB) [CAS No. 14047-09-7] in Harlan Sprague-Dawley Rats and B6C3F1 Mice (Gavage Studies). NTP, Research Triangle Park, NC.
Abstract: https://ntp.niehs.nih.gov/go/33564National Toxicology Program. 2011. NTP TR-565. Toxicology and Carcinogenesis Studies of Milk Thistle Extract (CAS No. 84604-20-6) in F344/N Rats and B6C3F1 Mice. NTP, Research Triangle Park, NC.
Abstract: https://ntp.niehs.nih.gov/go/34807Stefanski SA, Elwell MR, Stromberg PC. 1990. Spleen, lymph nodes, and thymus. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman GA, Eustis SL, Elwell MR, Montgomery CA, MacKenzie WF, eds). Academic Press, San Diego, 369-394.
Ward JM, Mann PC, Morishima H, Frith CH. 1999. Thymus, spleen, and lymph nodes. In: Pathology of the Mouse (Maronpot RR, ed). Cache River Press, Vienna, IL, 333-360.
Ward JM, Reznik-Schüller H. 1980. Morphological and histochemical characteristics of pigments in aging F344 rats. Vet Pathol 17:678-685.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/7423828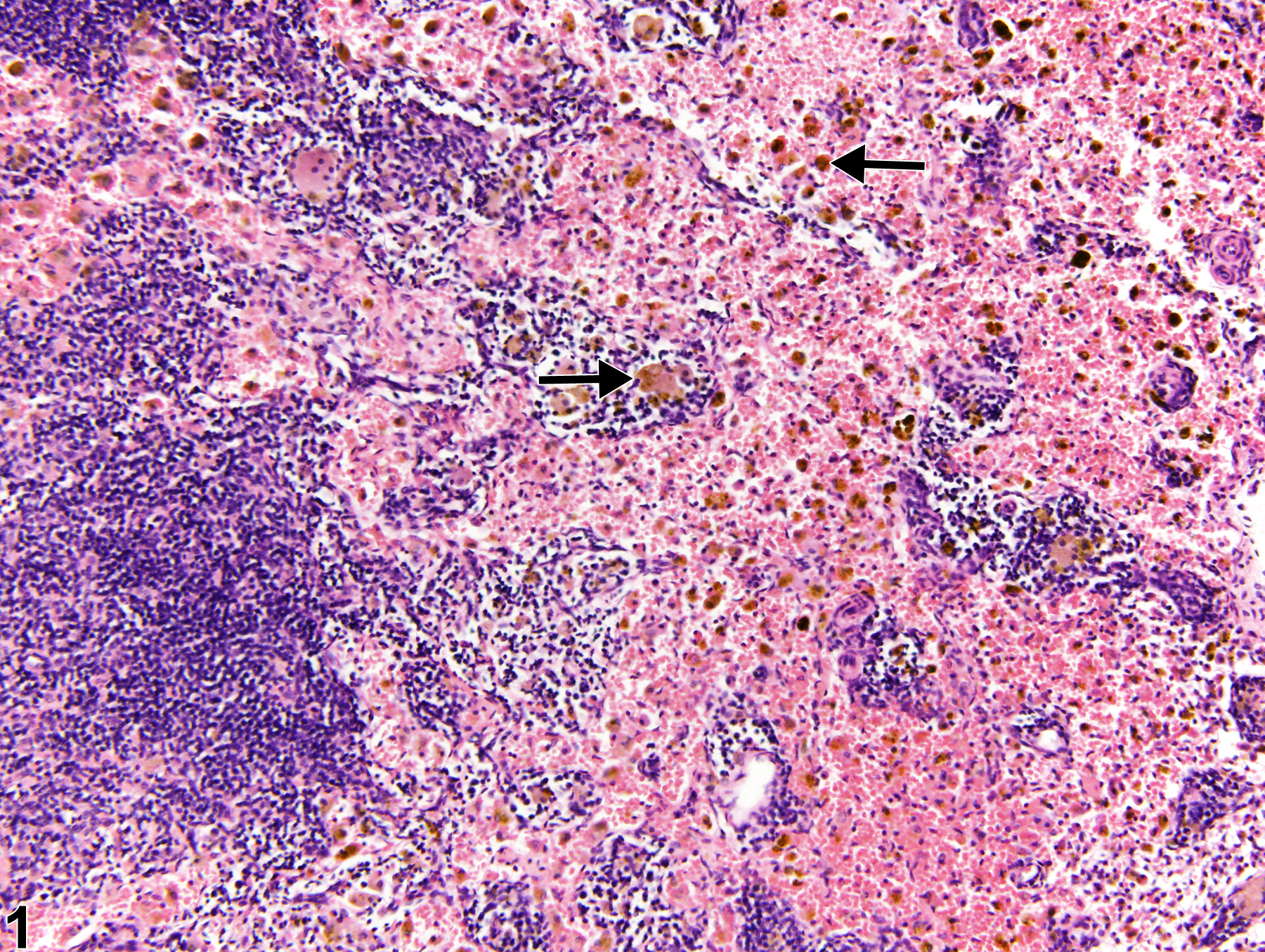
Lymph node, Medullary sinuses - Pigment in a male Harlan Sprague-Dawley rat from a chronic study. Macrophages within the medullary sinuses contain intracytoplasmic golden-brown pigment suggestive of hemosiderin (arrows).