Reproductive System, Female
Clitoral Gland - Inflammation
Narrative
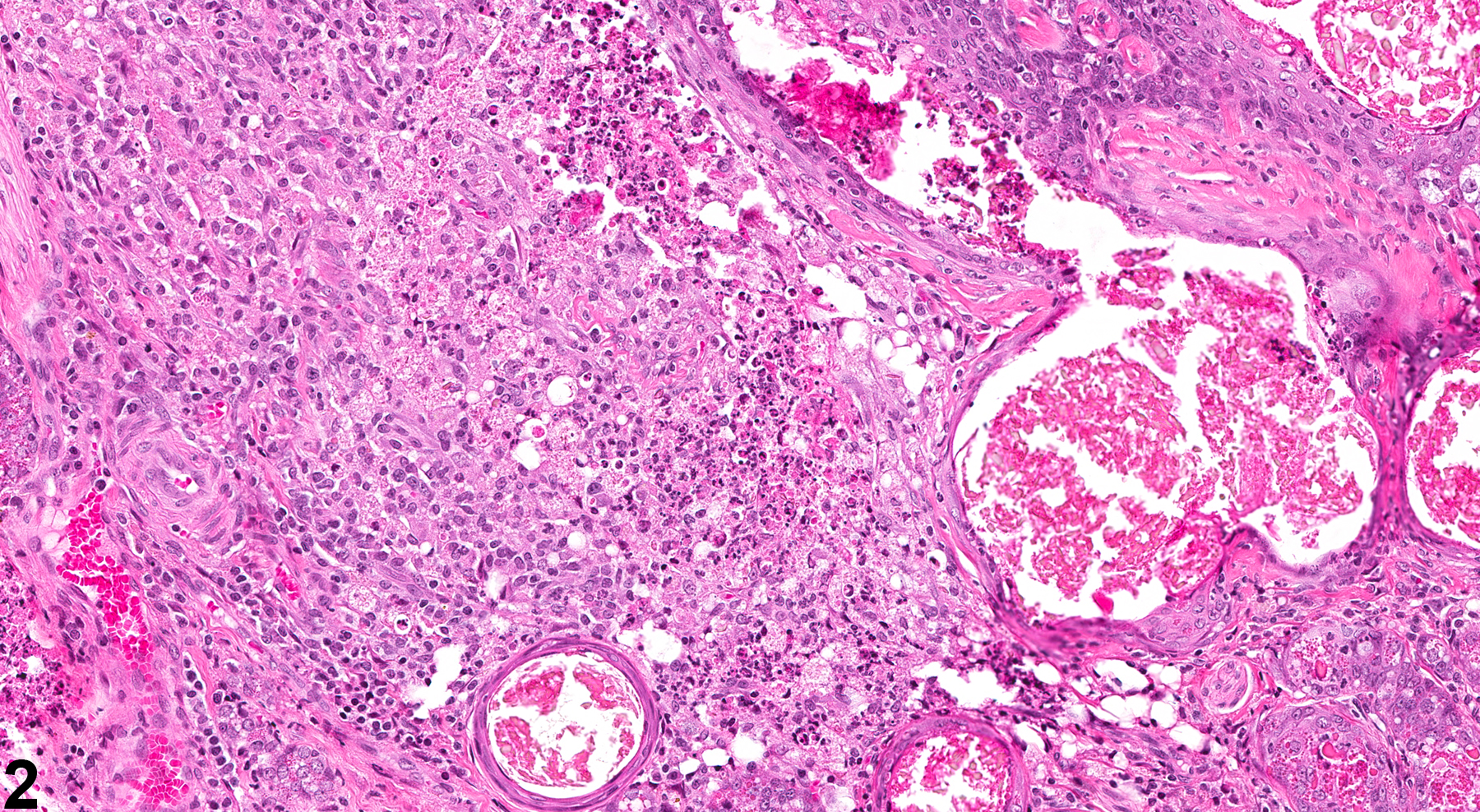
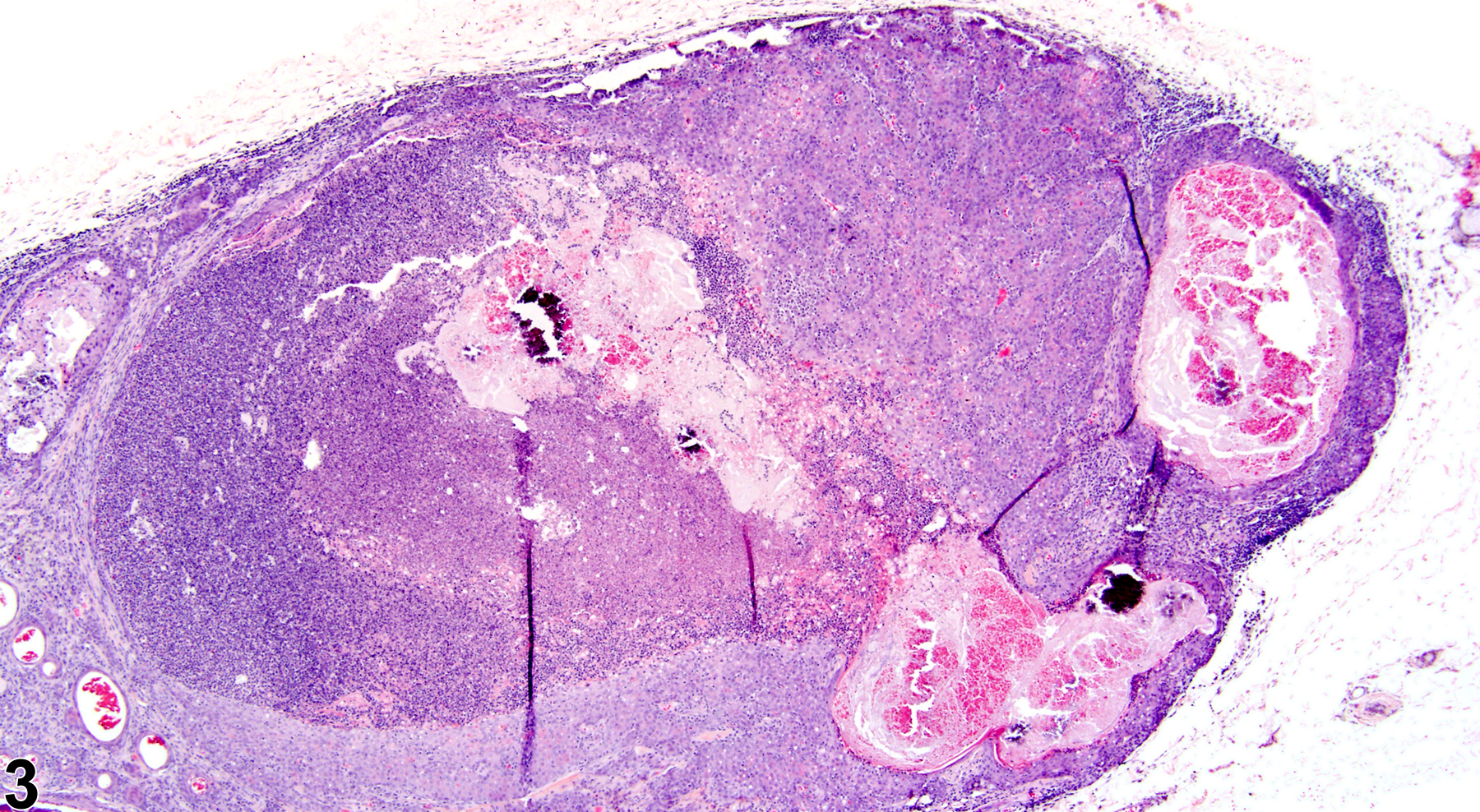
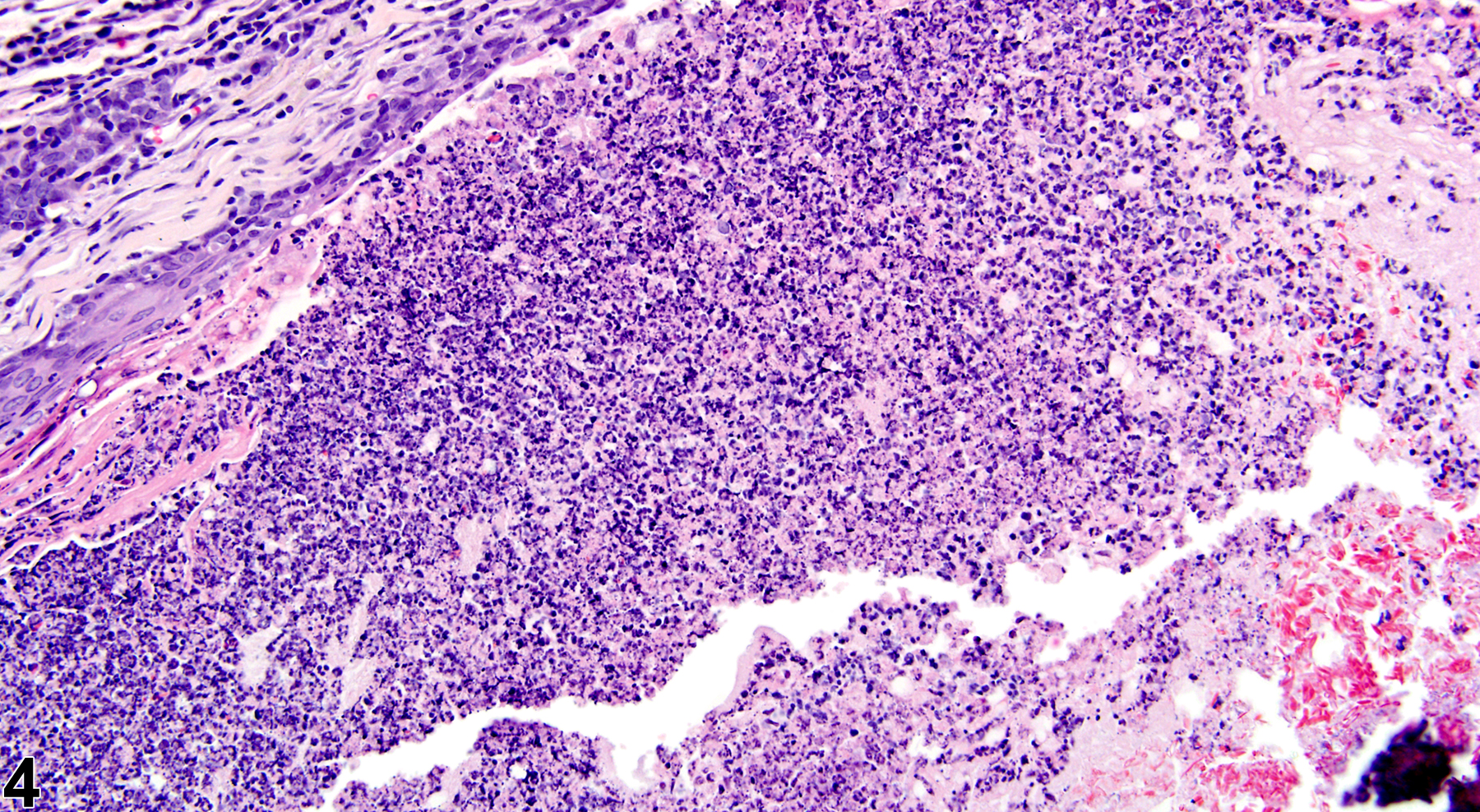
Inflammation in the clitoral gland is commonly seen as a background lesion. It can, however, be associated with treatment (Figure 1, Figure 2, Figure 3 and Figure 4). Granulomatous inflammation is commonly seen in rats, associated with rupture of dilated ducts containing keratin-like material. The type of inflammation should be indicated in the diagnosis. In NTP studies, there are five standard categories of inflammation: acute, suppurative, chronic, chronic active, and granulomatous. In acute inflammation, the predominant infiltrating cell is the neutrophil, though fewer macrophages and lymphocytes may also be present. There may also be evidence of edema or hyperemia. The neutrophil is also the predominant infiltrating cell type in suppurative inflammation, but they are aggregated, and many of them are degenerate (suppurative exudate). Cell debris, both from the resident cell populations and from infiltrating leukocytes, and proteinaceous fluid containing fibrin, fewer macrophages, occasional lymphocytes or plasma cells, and, possibly, an infectious agent may also be present within the exudate. Grossly, these lesions would be characterized by the presence of pus. The tissue surrounding the exudate may contain fibroblasts, fibrous connective tissue, and mixed inflammatory cells, depending on the chronicity of the lesion. Lymphocytes predominate in chronic inflammation. Lymphocytes also predominate in chronic active inflammation, but there are also a significant number of neutrophils. Both lesions may contain macrophages. Granulomatous inflammation is another form of chronic inflammation, but this diagnosis requires the presence of a significant number of aggregated, large, activated macrophages, epithelioid macrophages, or multinucleated giant cells.
If the inflammation occurs as a primary lesion, then it should be diagnosed and given a severity grade. The type of inflammation (e.g., acute, chronic) should be indicated in the diagnosis. If the inflammation is secondary to another lesion (e.g., neoplasia, necrosis), then it should not be diagnosed but should be described in the pathology narrative. Secondary lesions, such as hemorrhage, necrosis, or hyperplasia, should not be diagnosed separately unless warranted by severity.
Copeland-Haines D, Eustis SL. 1990. Specialized sebaceous glands. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman GA, Eustis SL, Elwell MR, Montgomery CA, MacKenzie WF, eds). Academic Press, San Diego, CA, 279-293.
Dixon D, Heider K, Elwell MR. 1995. Incidence of nonneoplastic lesions in historical control male and female Fischer-344 rats from 90-day toxicity studies. Toxicol Pathol 23:338-348.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/7659956National Toxicology Program. 1992. NTP TR-415. Toxicology and Carcinogenesis Studies of Polysorbate 80 (CAS No. 9005-65-6) in F344/N Rats and B6C3F1 Mice (Feed Studies). NTP, Research Triangle Park, NC.
Abstract: https://ntp.niehs.nih.gov/go/7710Seely JC, Boorman GA. 1991. Mammary gland and specialized sebaceous glands. In: Pathology of the Mouse: Reference and Atlas (Maronpot RR, Boorman GA, Gaul BW, eds). Cache River Press, Vienna, IL, 613-635.
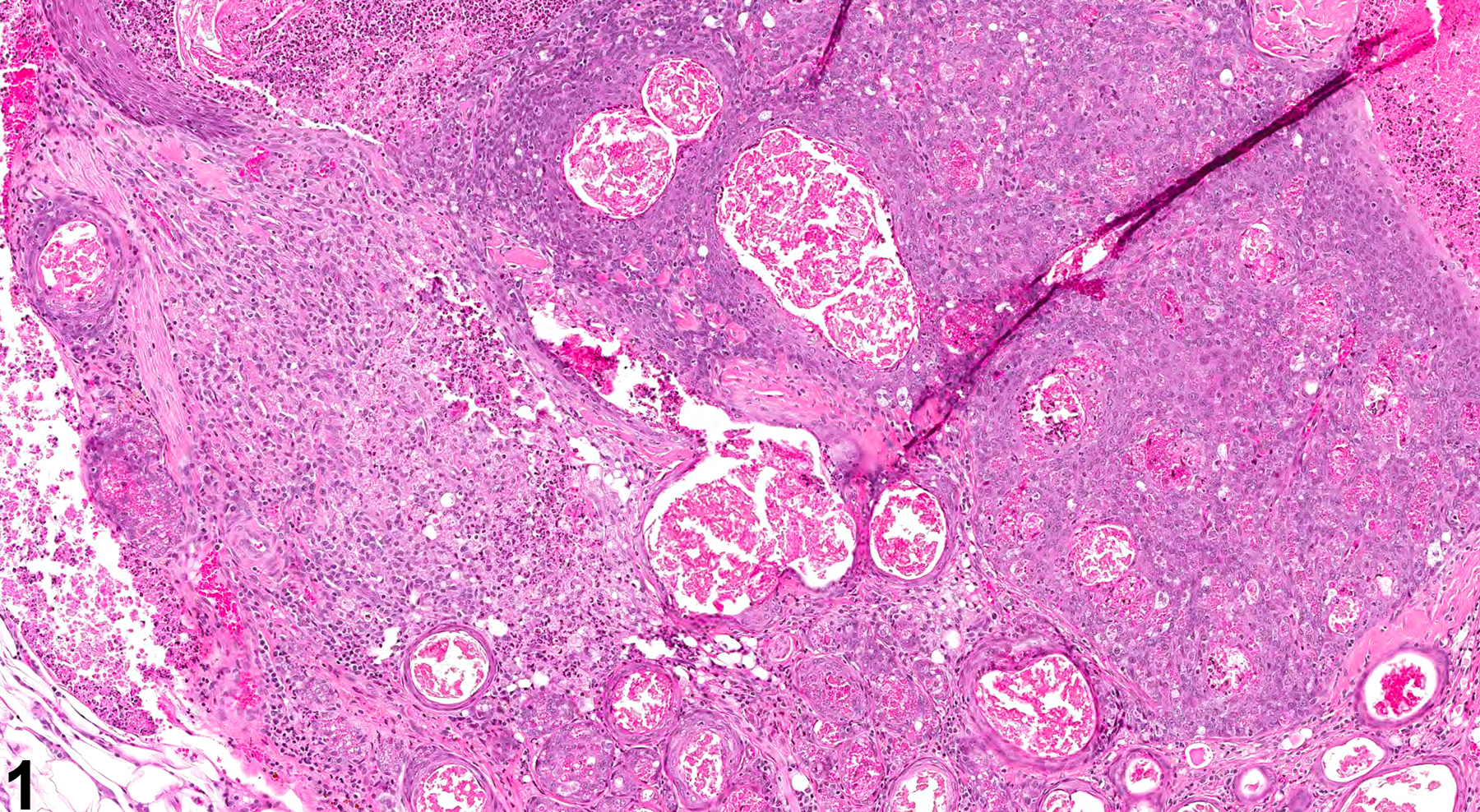
Clitoral gland - Inflammation, Chronic active in a female F344/N rat from a chronic study. An infiltration of lymphocytes, neutrophils, and macrophages is present in the gland parenchyma and around the ducts.