Immune System
Lymph Node - Sinus Erythrocytosis
Narrative
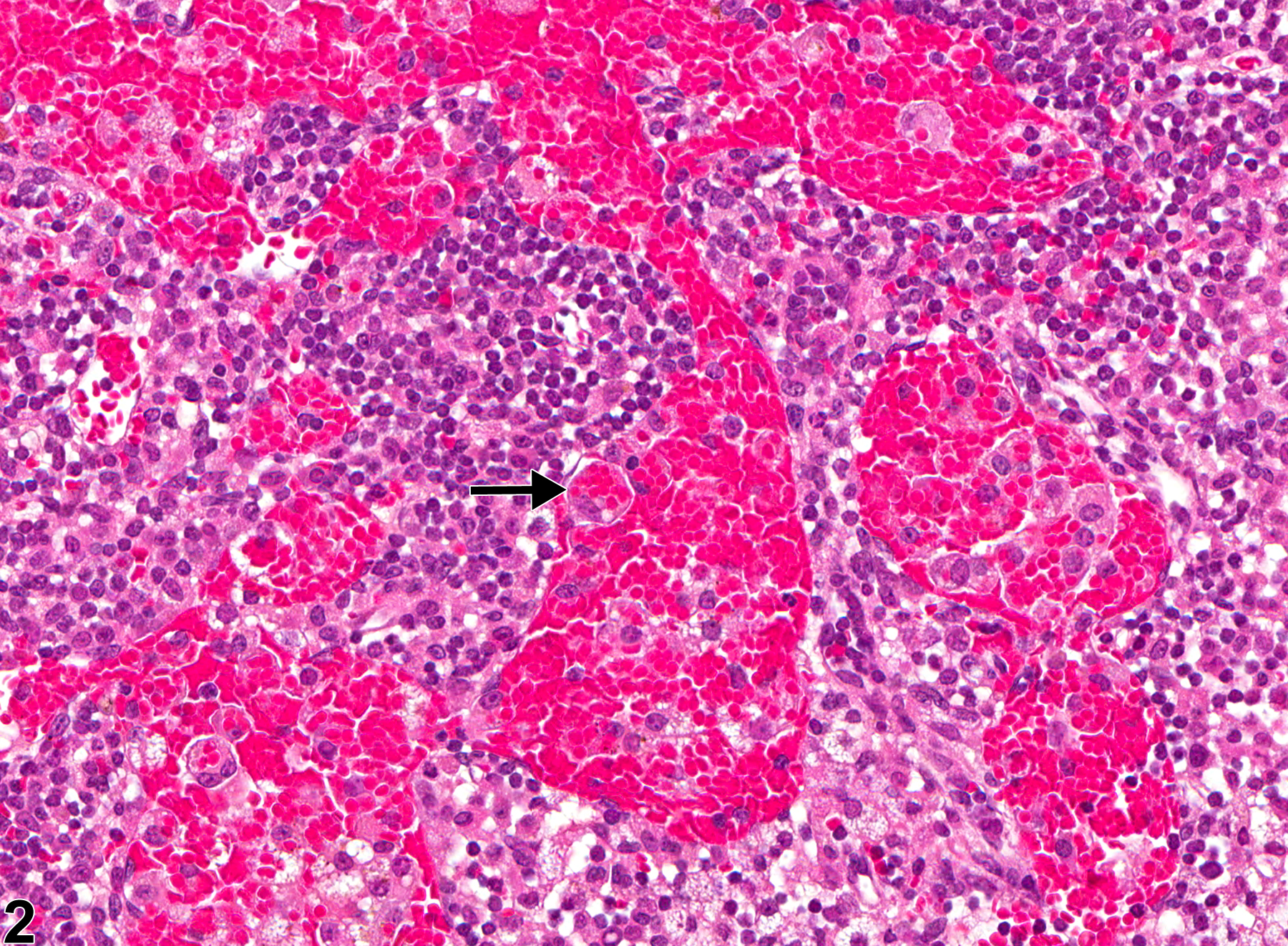
Sinus erythrocytosis is characterized by the presence of erythrocytes within the lymphatic sinuses (Figure 1, arrow). This lesion generally occurs as a result of hemorrhage in organs or tissues drained by the affected node. Acutely, there may be no reaction. In chronic lesions, there may be erythrophagocytosis (Figure 2, arrow), crystallization of hemoglobin from degenerate erythrocytes, and accumulation of hemosiderin pigment within lymphatic sinuses, sinus histiocytes, and medullary cord macrophages. Sinus erythrocytosis must be differentiated from angiectasis, hemorrhage, congestion, hemangioma, and hemangiosarcoma. Differentiation of sinus erythrocytosis and angiectasis may be a challenge, since dilated lymphatic vessels can resemble dilated blood vessels and both are lined by endothelium. Sinus erythrocytosis can be differentiated from primary hemorrhage in that blood is confined to endothelial-lined lymphatic sinuses and not extravasated into the tissue. Congestion is also intraluminal but involves blood vessels that may or may not be dilated (angiectatic). Sinus erythrocytosis can occur throughout the lymph node, which differentiates it from the well-circumscribed, tightly packed, dilated vascular spaces typical of hemangioma. The vascular spaces of hemangioma are lined by endothelium, but endothelial cells are aligned on a thin or broad collagenous stroma. Sinus erythrocytosis is not invasive and does not demonstrate endothelial cell atypia, which differentiates it from hemangiosarcoma. Sinus erythrocytosis must be also differentiated from extravasations of erythrocytes associated with euthanasia (perimortem) or tissue dissection (postmortem). A survey for regions of hemorrhage in the drainage field for the node in question may help to rule in/out sinus erythrocytosis.
Sinus erythrocytosis in lymph nodes should be diagnosed and graded when antemortem evidence (e.g., erythrophagocytosis or hemorrhage in drainage field) for the lesion is present. It should not be diagnosed if extravasations of erythrocytes in a lymph node can be attributed to peri- or postmortem artifact.
Elmore SA. 2006. Histopathology of the lymph nodes. Toxicol Pathol 34:425-454.
Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1892634/Frith CH, Ward JM, Chandra M, Losco PE. 2000. Non-proliferative lesions of the hematopoietic system in rats. In: Guides for Toxicologic Pathology.TP/ARP/AFIP, Washington, DC.
Full Text: https://www.toxpath.org/docs/SSNDC/HematopoieticNonprolifRat.pdfNational Toxicology Program. 2007. NTP TR-535. Toxicology and Carcinogenesis Studies of 4-Methylimidazole (CAS No. 822-36-6) in F344/N Rats and B6C3F1 Mice (Feed Studies). NTP, Research Triangle Park, NC.
Abstract: https://ntp.niehs.nih.gov/go/13651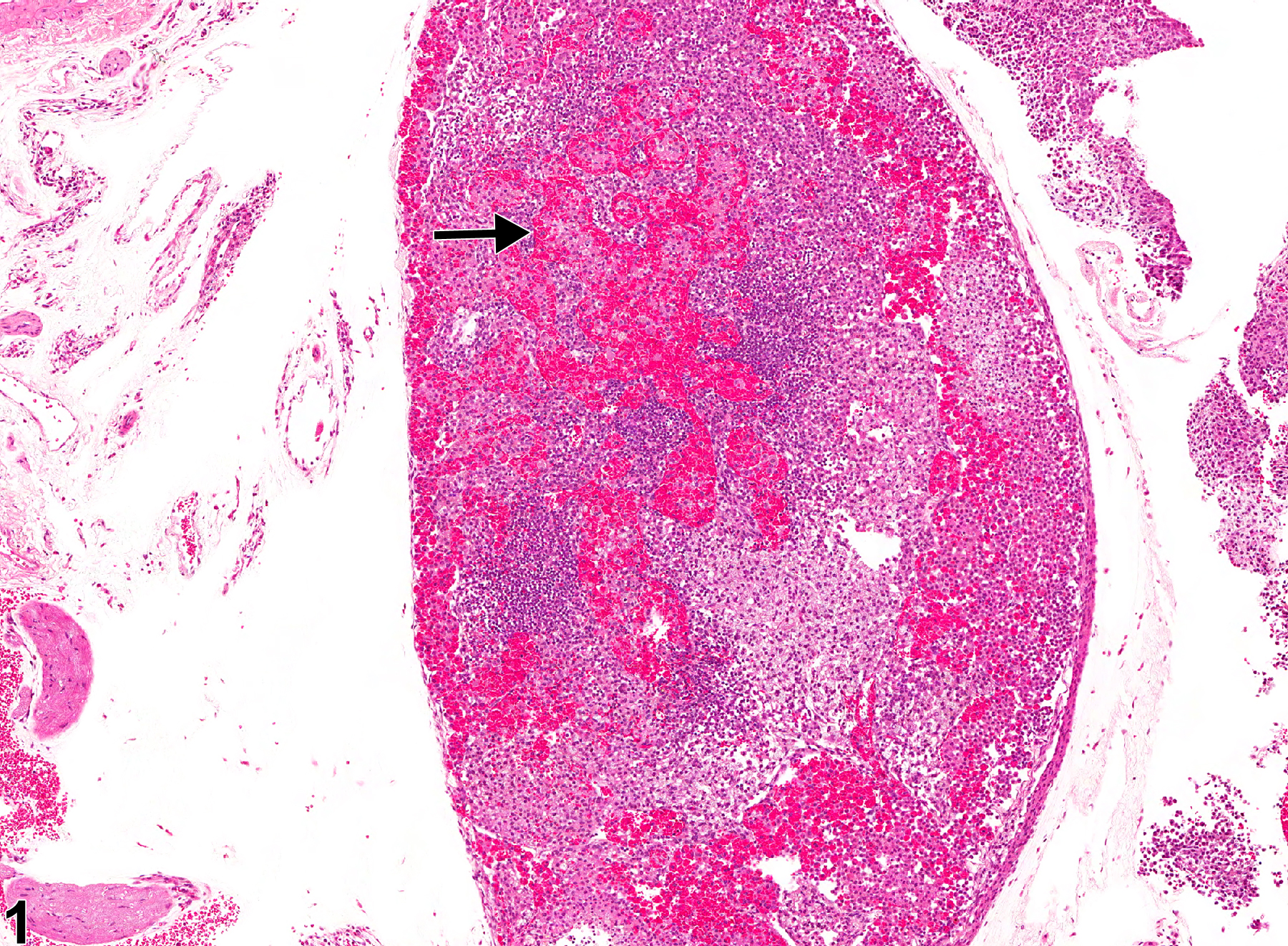
Lymph node - Sinus erythrocytosis in a female B6C3F1/N mouse from a chronic study. The lymphatic sinuses (arrow) of this lymph node are markedly dilated by numerous extravasated erythrocytes.