Alimentary System
Oral Mucosa - Inflammation
Narrative
Bertram TA, Markovits JE, Juliana MM. 1996. Non-proliferative lesions of the alimentary canal in rats GI-1. In Guides for Toxicologic Pathology. STP/ARP/AFIP, Washington, DC, 1-16.
Full Text: https://www.toxpath.org/docs/SSNDC/GINonproliferativeRat.pdfKlein-Szanto AJP, Conti CJ, Aldaz CM. 1990. Skin and oral mucosa. In: Handbook of Toxicologic Pathology (Haschek WM, Rousseaux CG, eds). Academic Press, San Diego, CA, 85-119.
Abstract: http://www.sciencedirect.com/science/book/9780123302151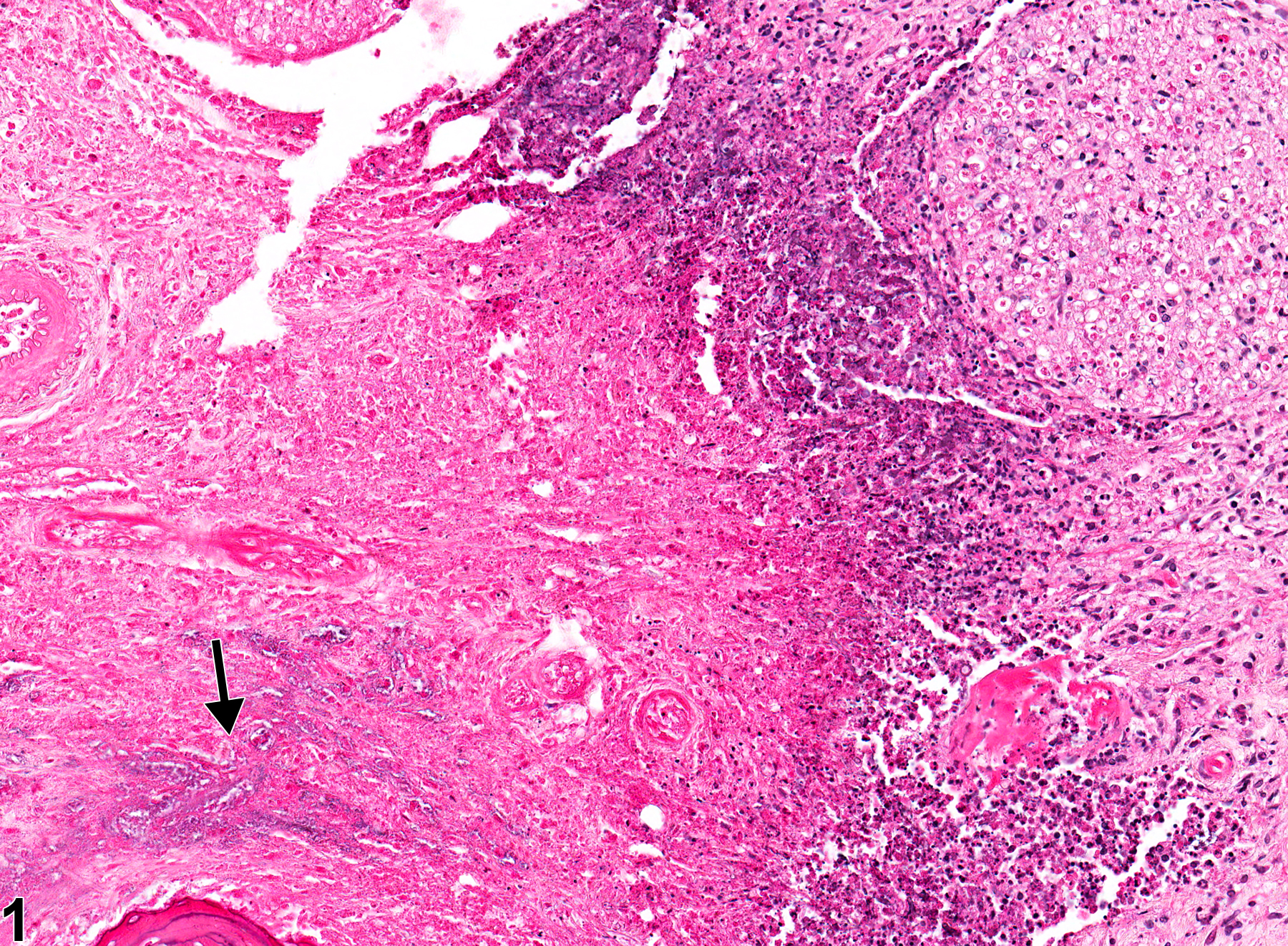
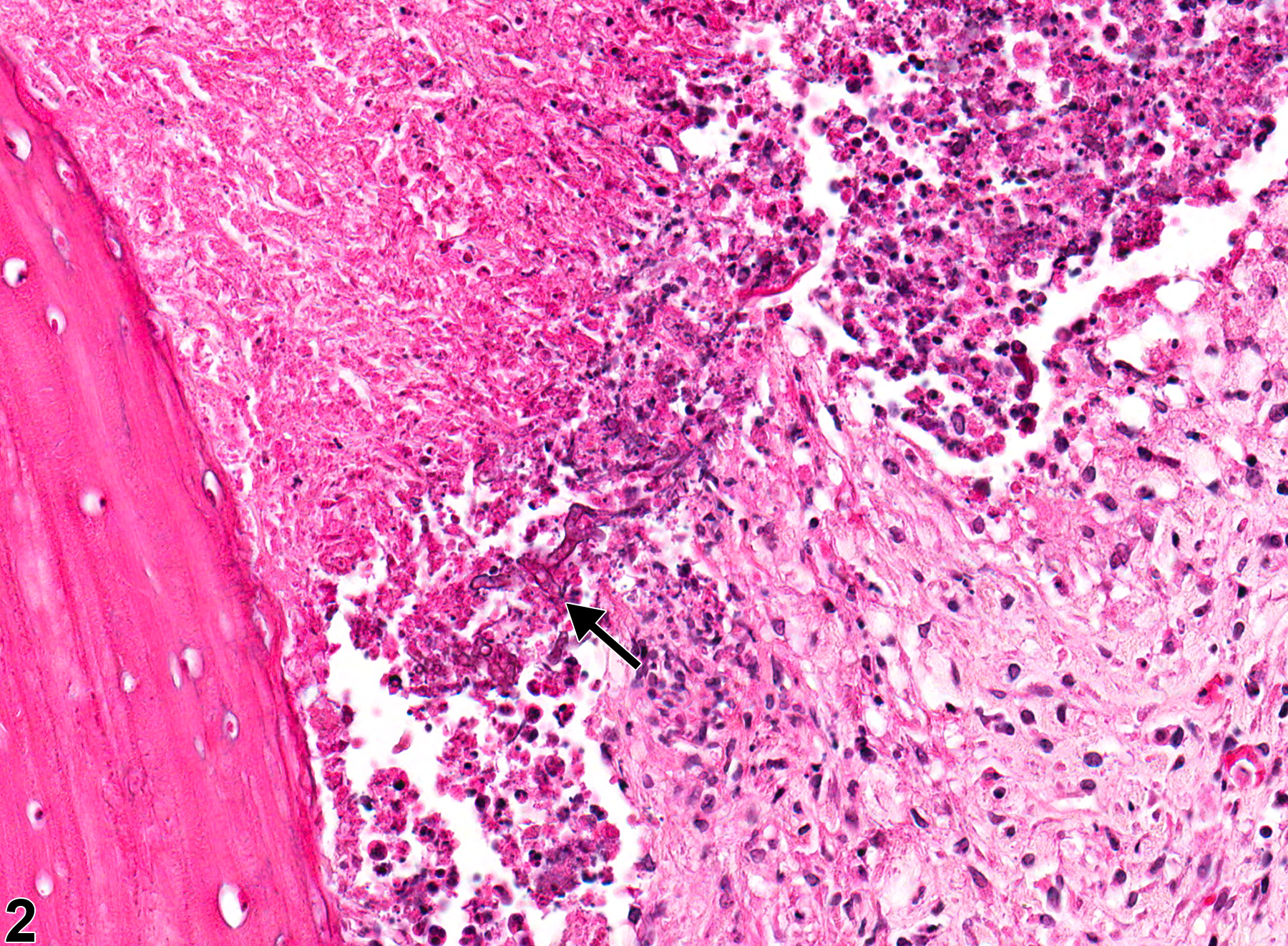
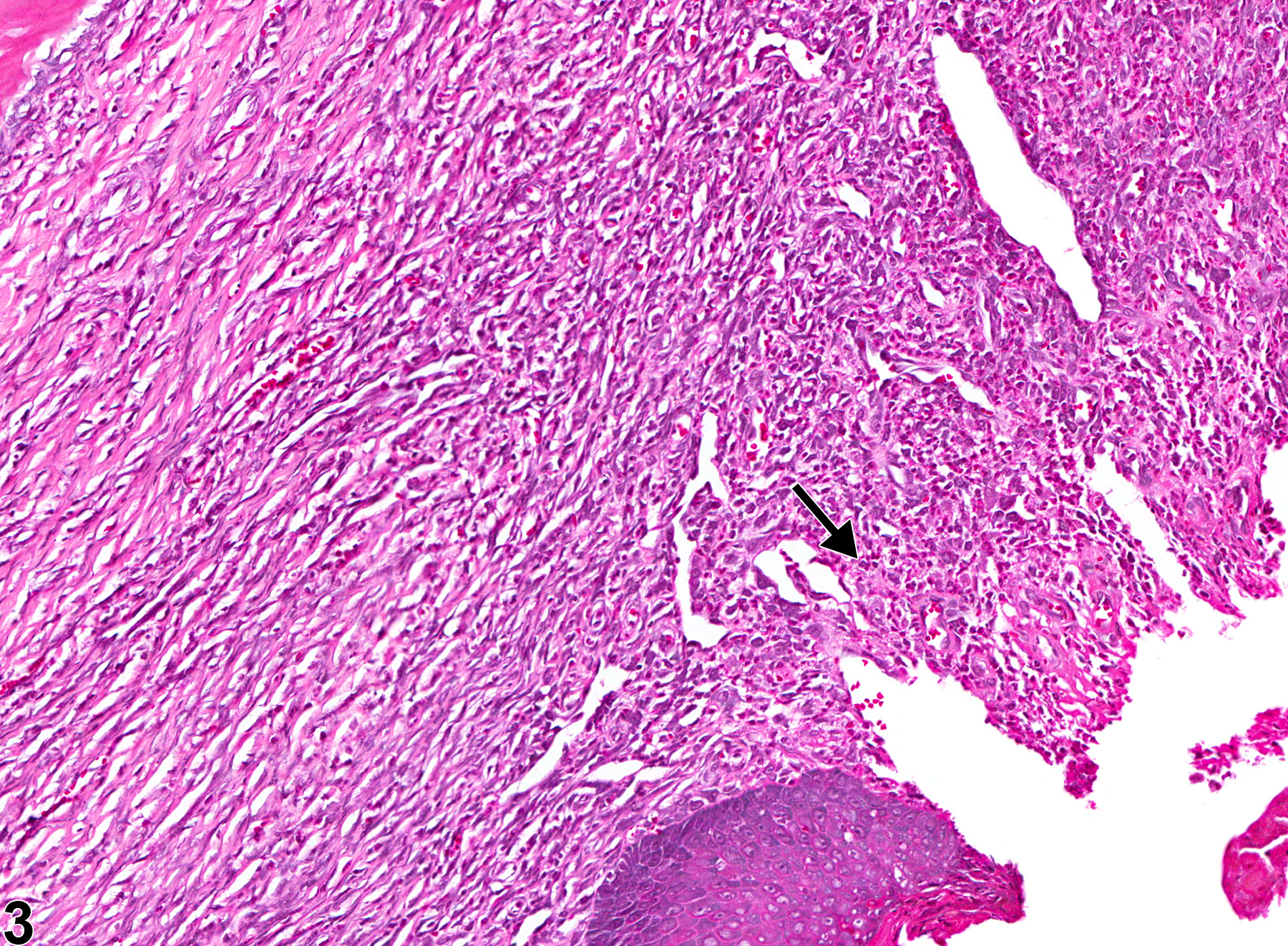
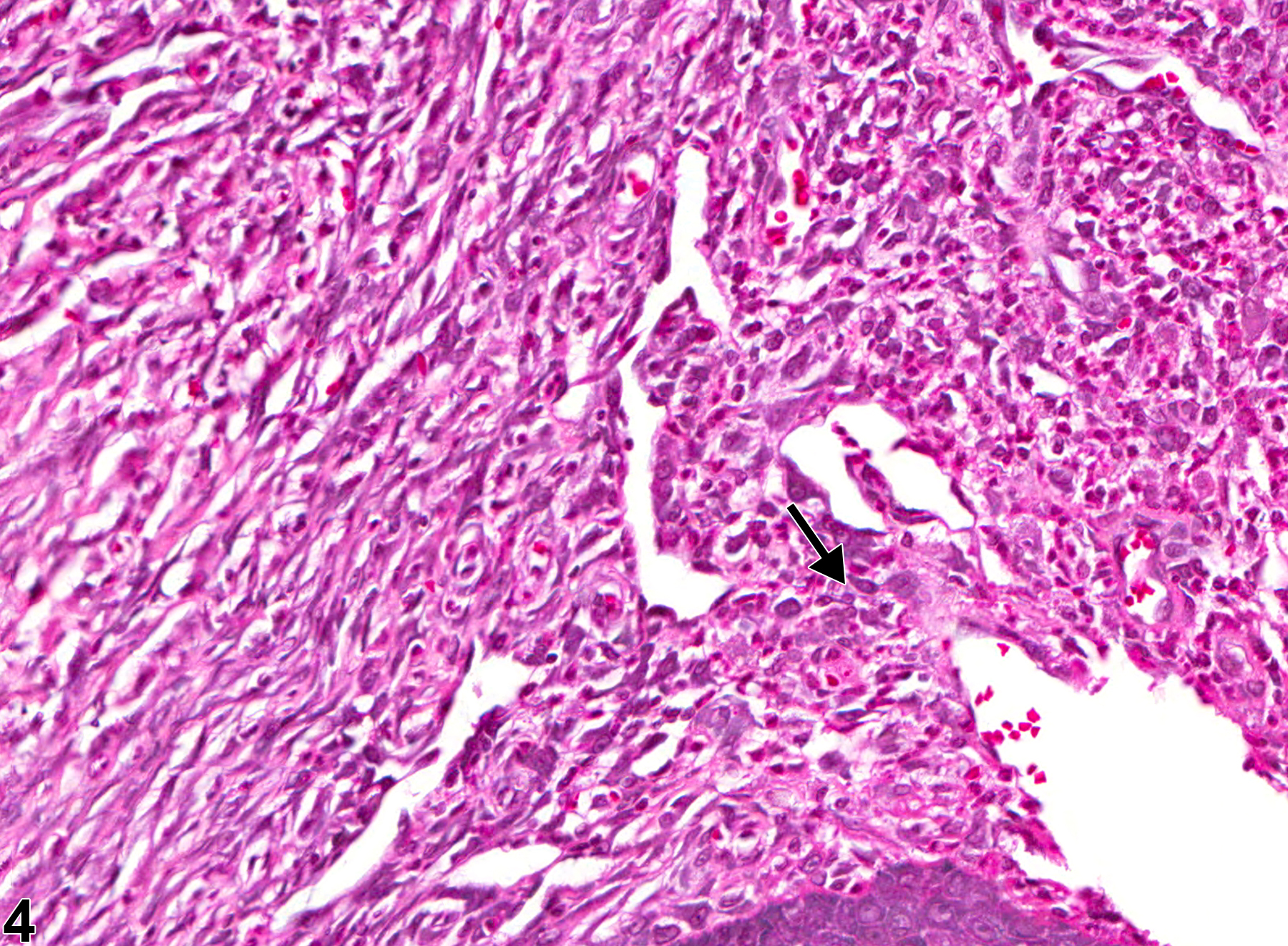
Oral mucosa - Inflammation, Suppurative in a male F344/N rat from a chronic study. There is an area of suppurative inflammation with necrosis and bacterial organisms (arrow).