Alimentary System
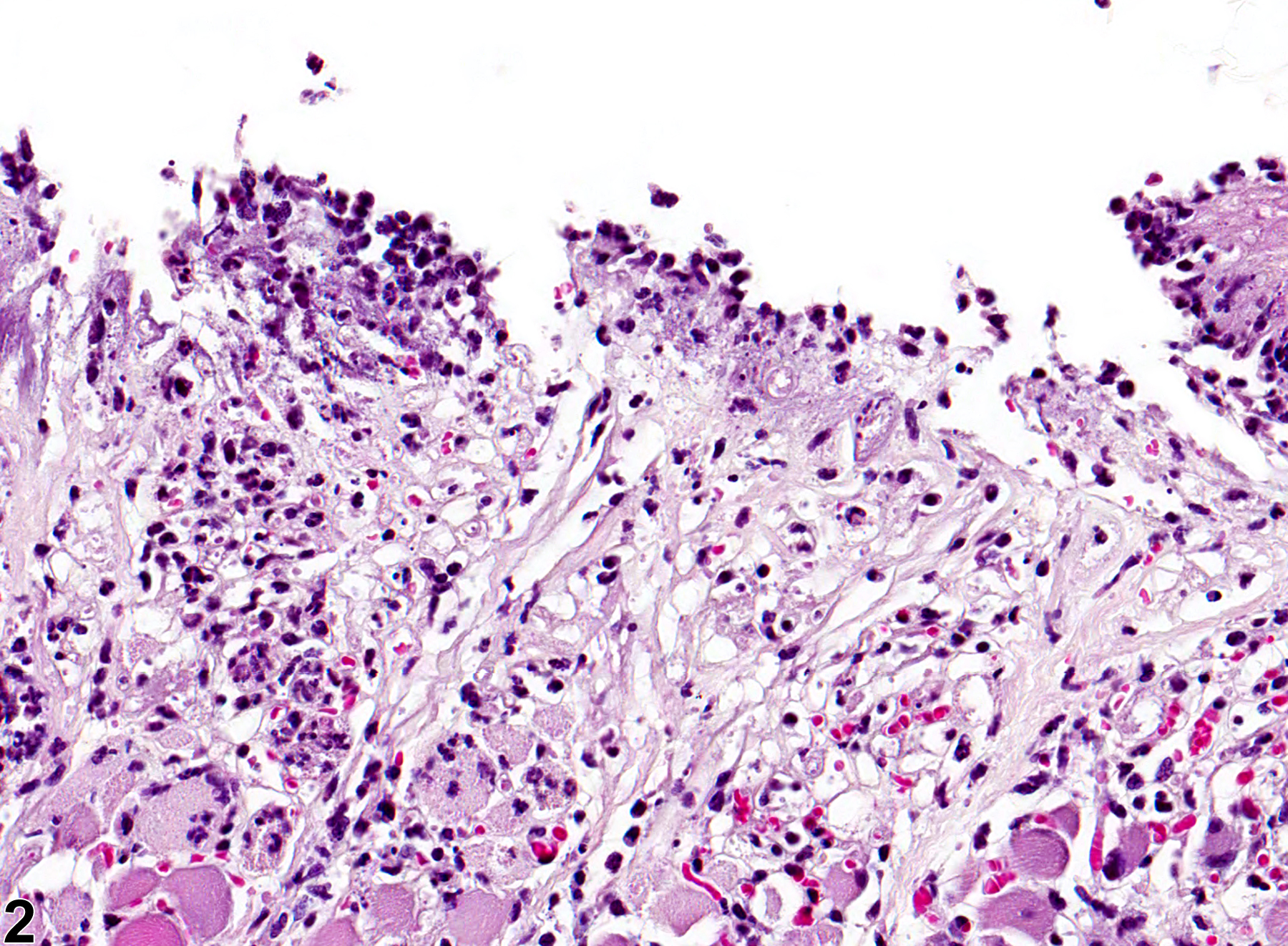
Tongue - Ulcer
Narrative
Bertram TA, Markovits JE, Juliana MM. 1996. Non-proliferative lesions of the alimentary canal in rats GI-1. In: Guides for Toxicologic Pathology. STP/ARP/AFIP, Washington, DC, 1-16.
Full Text: https://www.toxpath.org/docs/SSNDC/GINonproliferativeRat.pdfComereski CR, Peden WM, Davidson TJ, Warner GL, Hirth RS, Frantz JD. 1994. BR96-doxorubicin conjugate (BMS-182248) versus doxorubicin: A comparative toxicity assessment in rats. Toxicol Pathol 22:473-488.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/7899776Leininger JR, Jokinen MP, Dangler CA, Whiteley LO. 1999. Oral cavity, esophagus, and stomach. In: Pathology of the Mouse (Maronpot RR, ed). Cache River Press, St Louis, MO, 29-48.
National Toxicology Program. 2008. NTP TR-546. Toxicology and Carcinogenesis Studies of Sodium Dichromate Dihydrate (CAS No. 7789-12-0) in F344 rats and B6C3F1 Mice (Drinking Water Studies). NTP, Research Triangle Park, NC.
Abstract: https://ntp.niehs.nih.gov/go/29323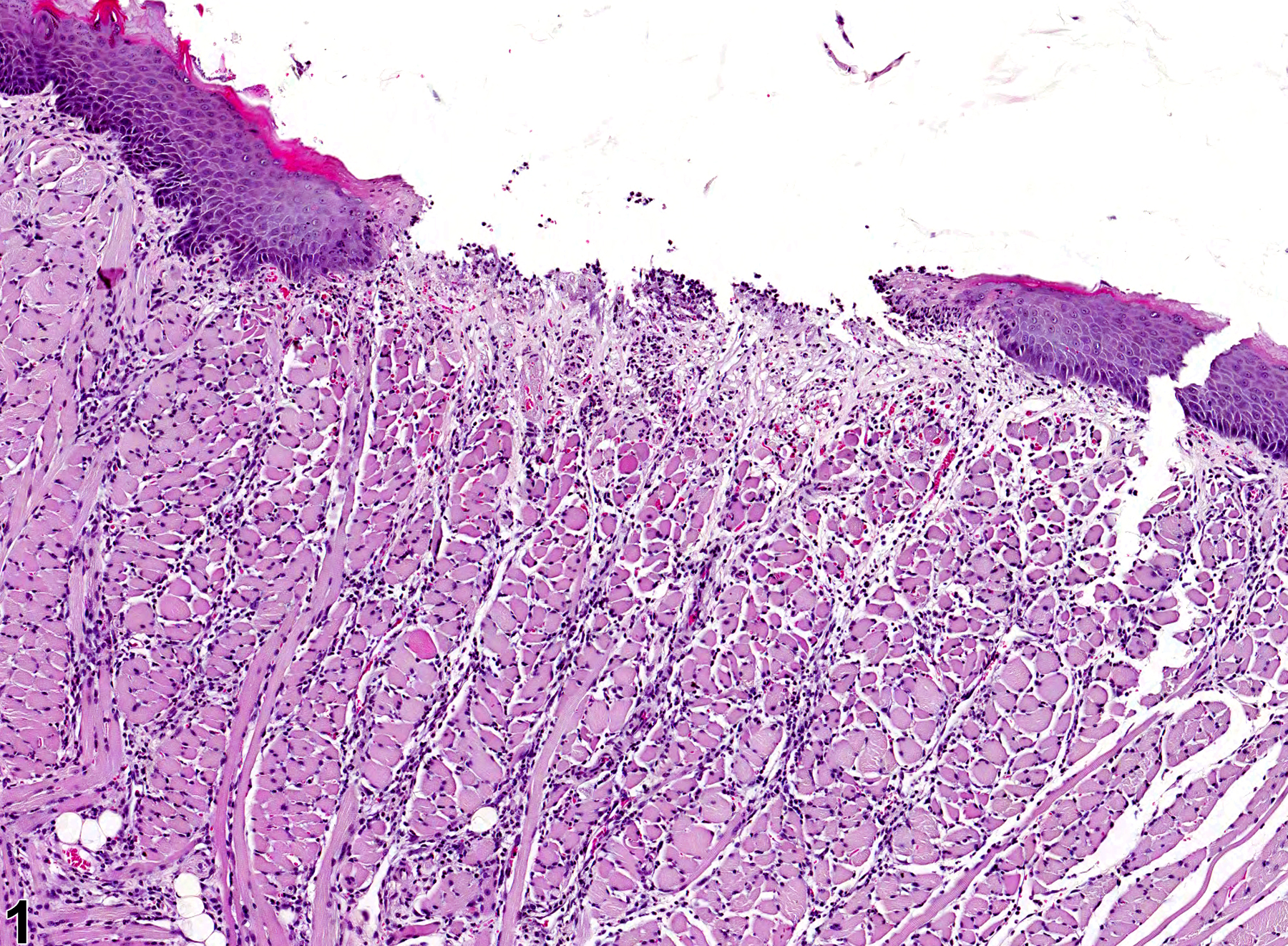
Tongue - Ulcer in a female F344/N rat from a chronic study. A portion of the keratinized squamous epithelium of the tongue has been lost, exposing the underlying lamina propria.