Cardiovascular System
Blood Vessel - Arteriosclerosis
Narrative
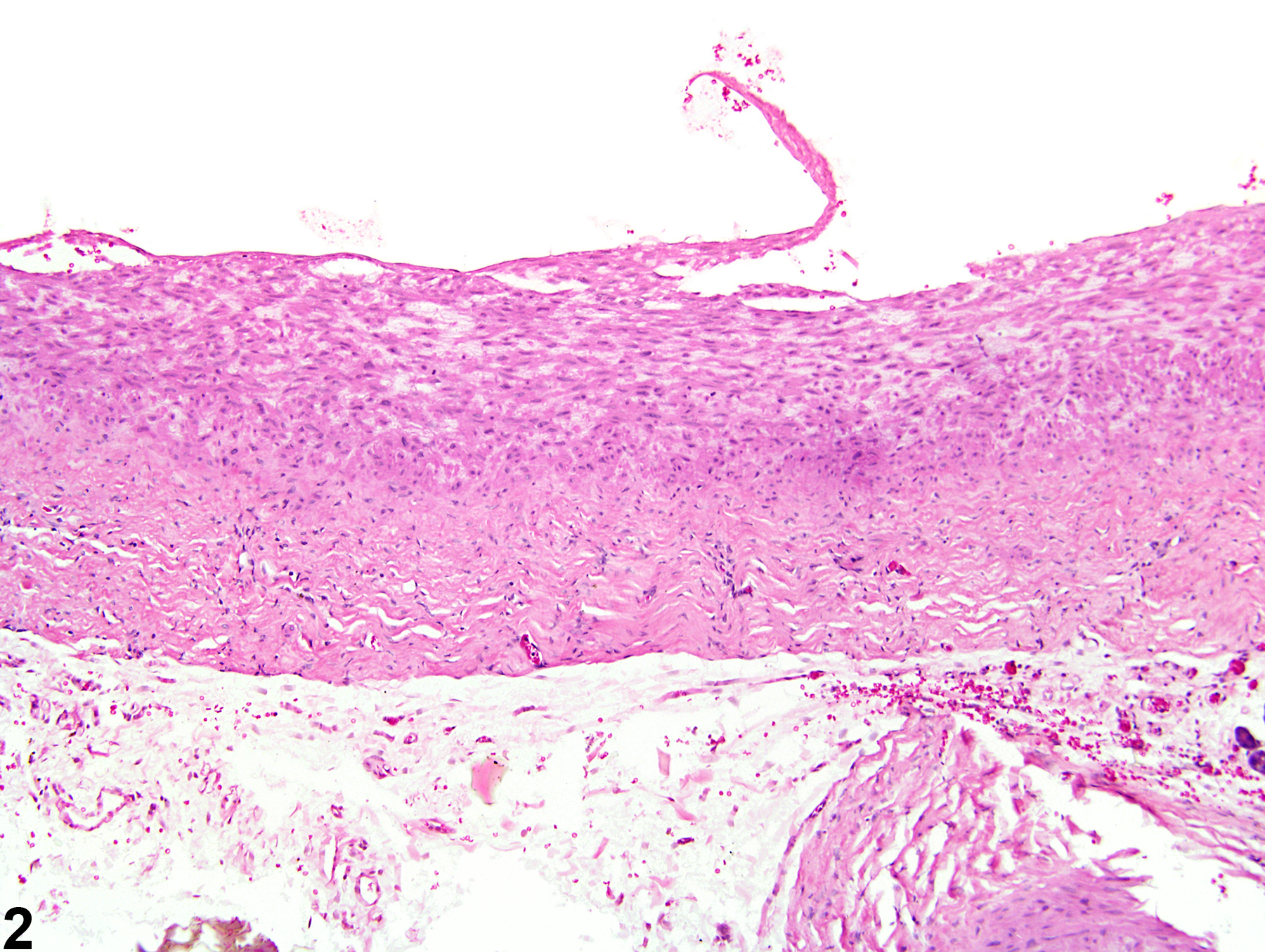
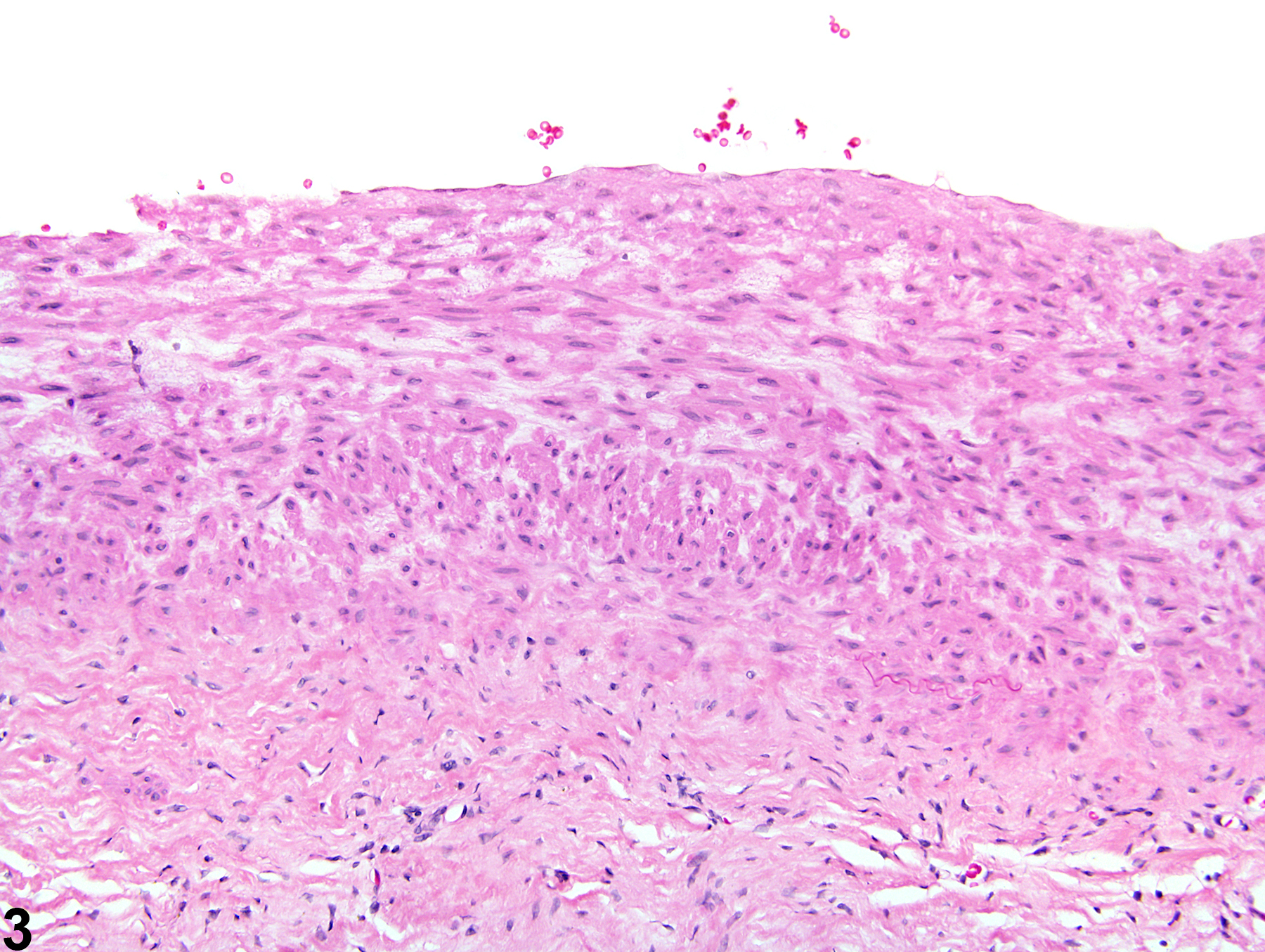
Arteriosclerosis is defined as a proliferative and/or degenerative (hyaline) change to the tunica media and tunica intima of arteries that results in loss of elasticity ("hardening") and is often associated with luminal narrowing. Grossly, there is a slight thickening and wrinkling of the tunica intima that appear as white, oval to linear plaques on the intimal surface. These gross lesions can be stained specifically and counted. Histologically, arteriosclerosis is characterized by degeneration and splitting of the internal elastic lamina in the tunica media with accumulation of mucopolysaccharide substance. Myointimal proliferation follows, and the lesion may progress to contain areas of mineralization or cartilaginous metaplasia or may lead to aneurysm formation.
While arteriosclerosis is not considered inflammatory, inflammation may be a predisposing factor. Endothelial damage is thought to be the primary initiating event leading to plaque formation. Vascular thickening and luminal narrowing that occur with arteriosclerosis can eventually lead to ischemic change. Lesions with significant narrowing of the lumen may contribute to distal ischemia and subsequent thrombus formation, as arterial branching points are preferred sites of lesion development.
Arteriosclerosis of the aorta and the iliac, renal, carotid, and cerebral arteries frequently occurs in breeders of several strains of rats, including Sprague-Dawley, Holtzman, Mead-Johnson, Long-Evans, Wistar, and Lewis. The extent and severity of the lesions correlate positively with breeding frequency, and lesions are generally more severe in females than in males.
Arteriosclerosis should be differentiated from atherosclerosis. Atherosclerosis is a form of arteriosclerosis that contains a lipid component. Atherosclerosis often results in more narrowing of the vascular lumen due to plaque formation containing lipid and macrophages.
Arteriosclerosis should be diagnosed and graded in the organs in which it is observed, with the type of blood vessel affected (artery or vein) included as a site modifier. If the type of blood vessel cannot be determined, the site modifier "blood vessel" may be used. Lesions in protocolrequired great vessels, such as aorta, should be recorded with the blood vessel as the site (e.g., Aorta - Arteriosclerosis). Severity grades should be applied and should encompass the lesion and the extent, including the number of vessels displaying the change in that particular organ. Severity grading should not be based on systemic disease but should be assessed in the individual organ affected.
Lewis BK, Wexler BC. 1975. Serum insulin changes in arteriosclerotic breeder female rats versus non-arteriosclerotic virgin rats. Horm Res 6(4):247-257.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/773805Maxie MG, Robinson WF. 2007. Cardiovascular system. In: Jubb, Kennedy and Palmer's Pathology of Domestic Animals, Vol 3, 5th ed (Maxie MG, ed). Saunders Elsevier, Edinburgh, 56-60.
Xu Q. 2004. Mouse models of arteriosclerosis: From arterial injuries to vascular grafts. Am J Pathol 165(1):1-10.
Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2216680/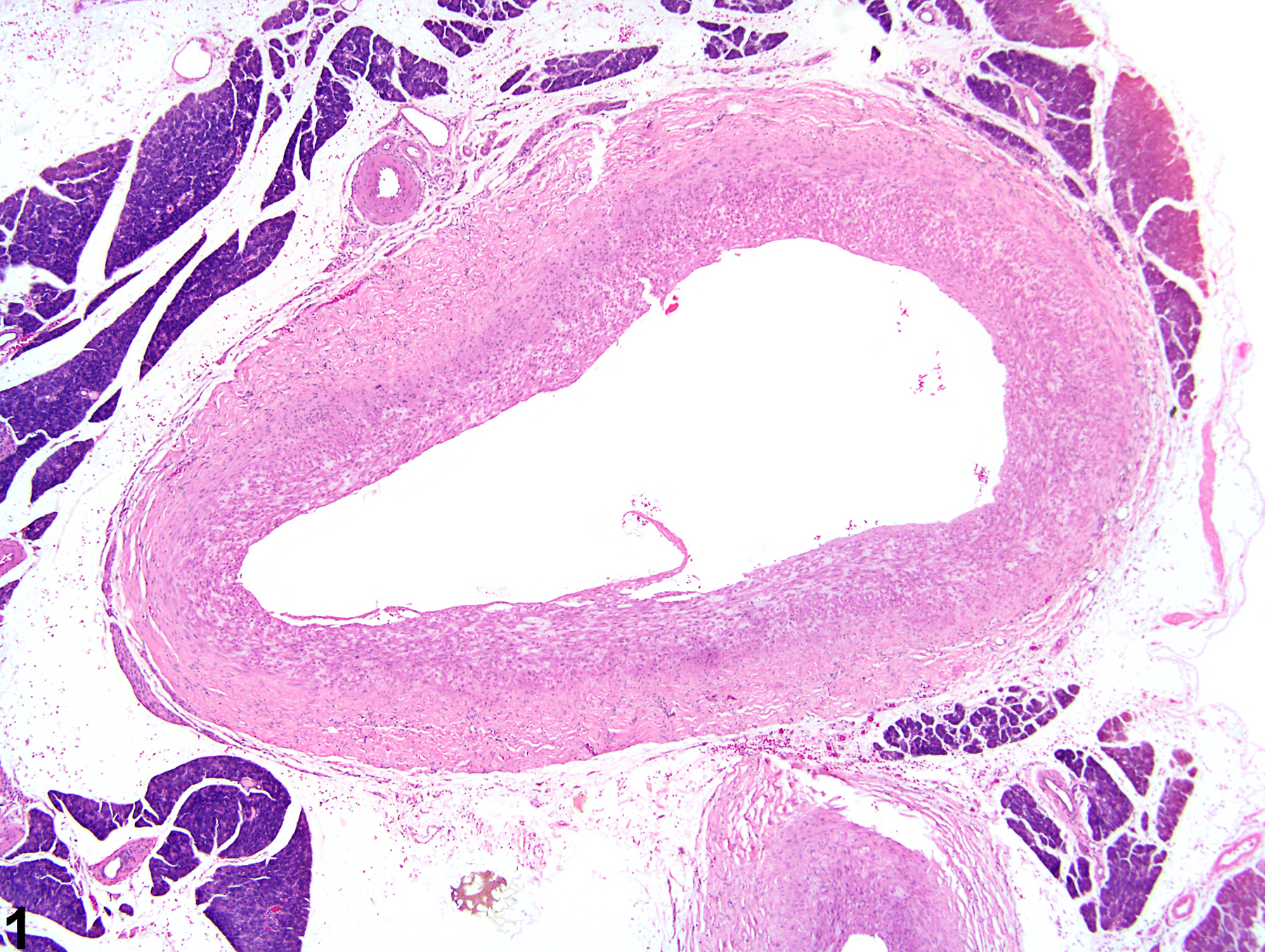
Mesentery, Artery - Arteriosclerosis in a male F344/N rat from a chronic study. The tunica media of a large mesenteric muscular artery is thickened.