Endocrine System
Parathyroid Gland - Hyperplasia, Diffuse
Narrative
Capen CC, Rosol TJ. 1989. Recent advances in the structure and function of the parathyroid gland in animals and the effects of xenobiotics. Toxicol Pathol 17:333-345.
Abstract: http://www.ncbi.nlm.nih.gov/pubmed/2675284Capen CC, DeLellis RA, Yarrington JT. 2002. Endocrine system. In: Handbook of Toxicologic Pathology, Vol 2 (Haschek WM, Rousseaux CG, Wallig MA, eds). Academic Press, New York, 681-783.
Abstract: http://www.sciencedirect.com/science/book/9780123302151Rosol TJ, Capen CC. 1989. Tumors of the parathyroid gland and circulating parathyroid hormone-related protein associated with persistent hypercalcemia. Toxicol Pathol 17:346-356.
Full Text: http://tpx.sagepub.com/content/17/2/346.full.pdfSeely JC, Hildebrandt PK.. 1990. Parathyroid gland. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman GA, Eustis SL, Elwell MR, Montgomery CA, MacKenzie WF, eds). Academic Press, San Diego, 537-543.
Abstract: http://www.ncbi.nlm.nih.gov/nlmcatalog/9002563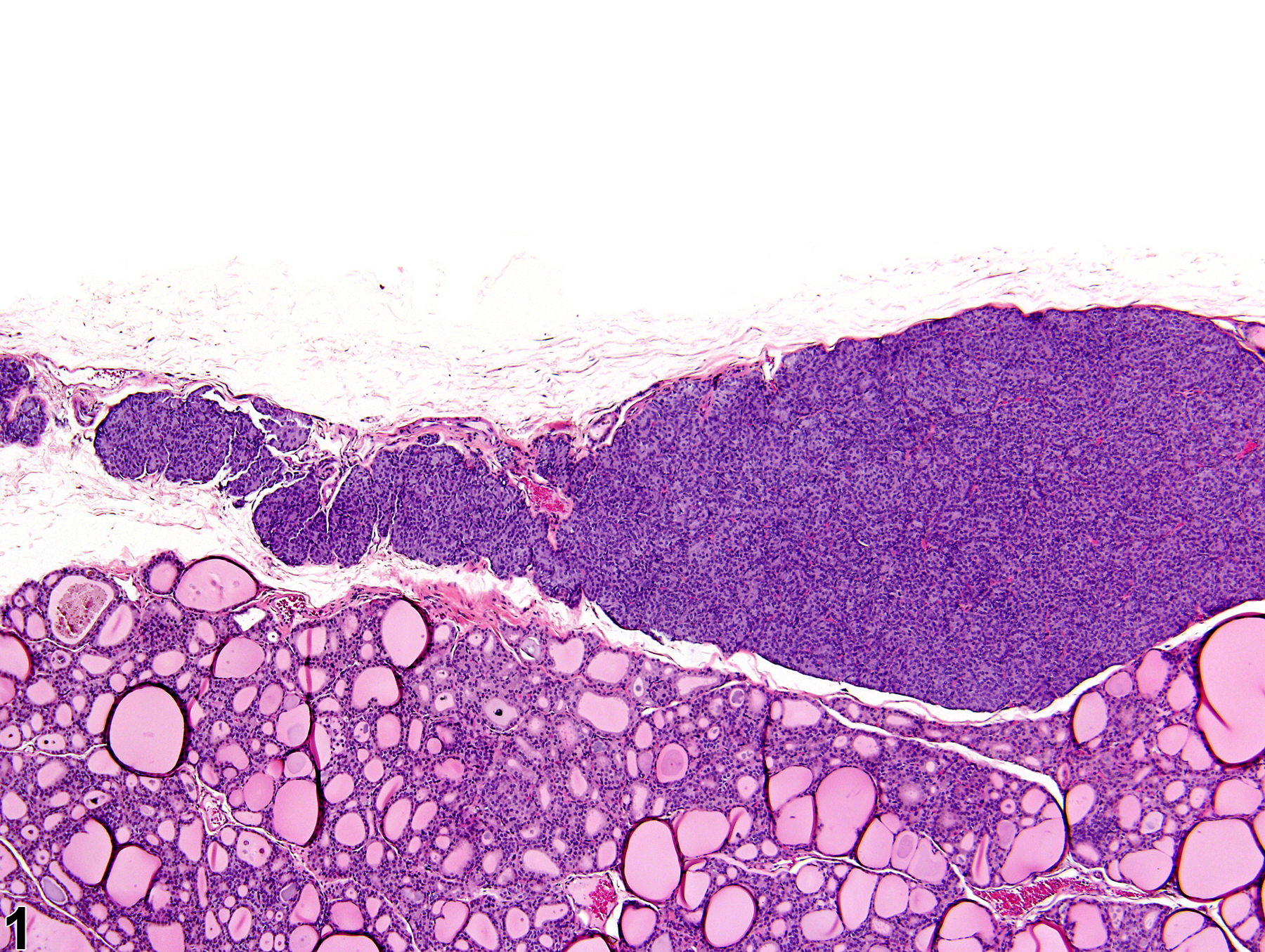
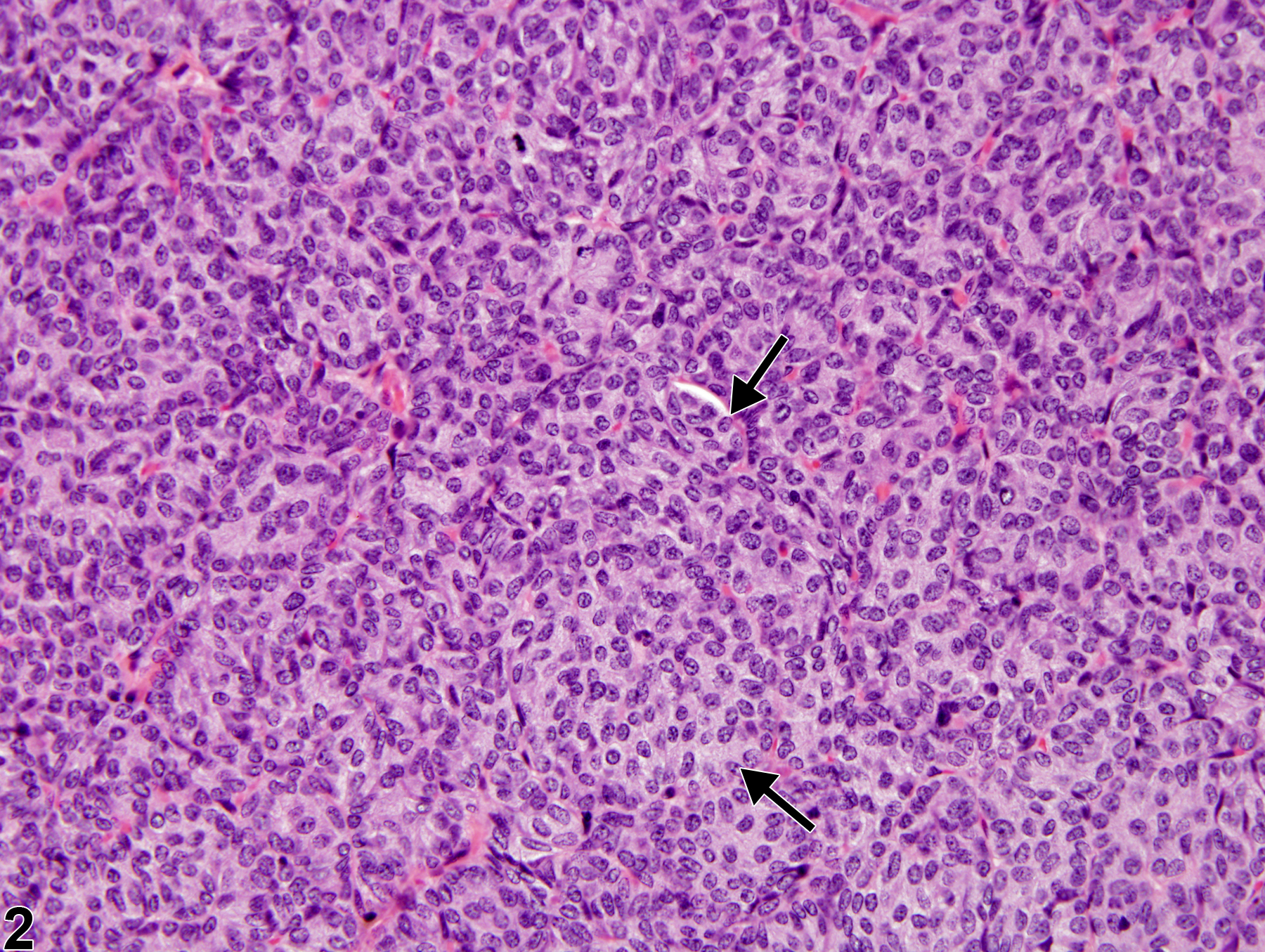
Parathyroid gland - Hyperplasia, Diffuse in a male F344/N rat from a chronic study. The parathyroid gland is increased in volume.