Endocrine System
Pituitary Gland - Hyperplasia
Narrative
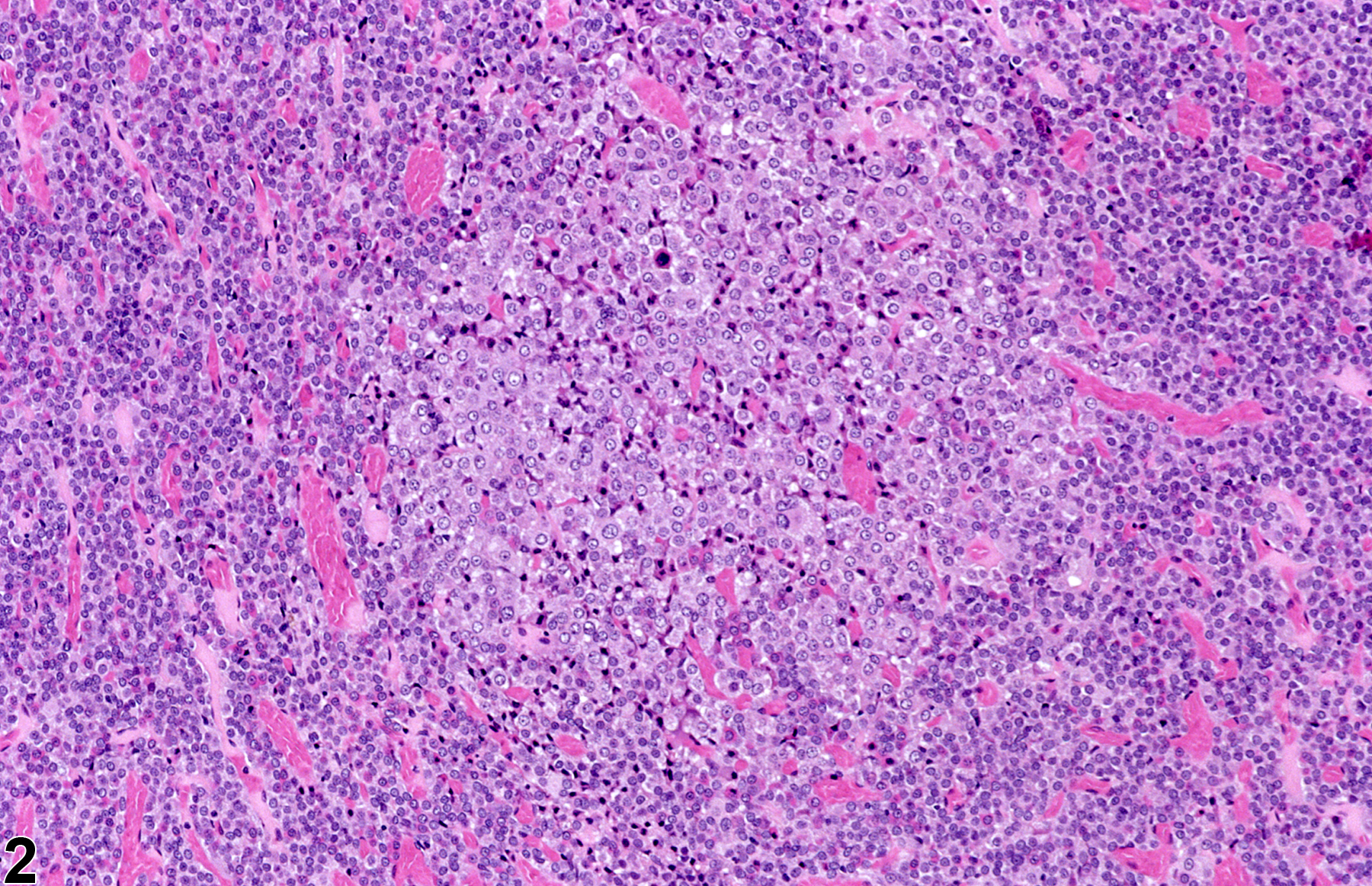
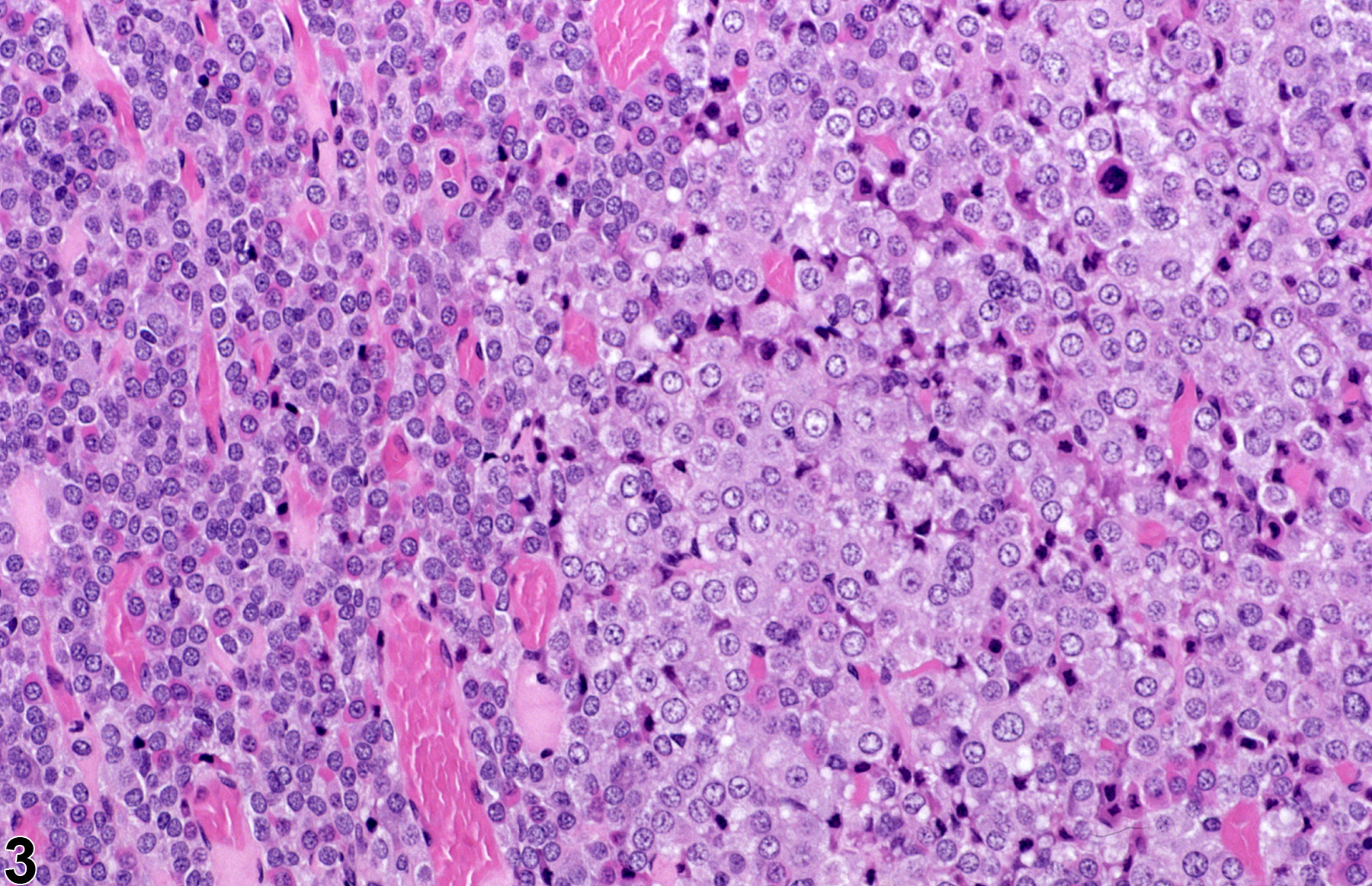
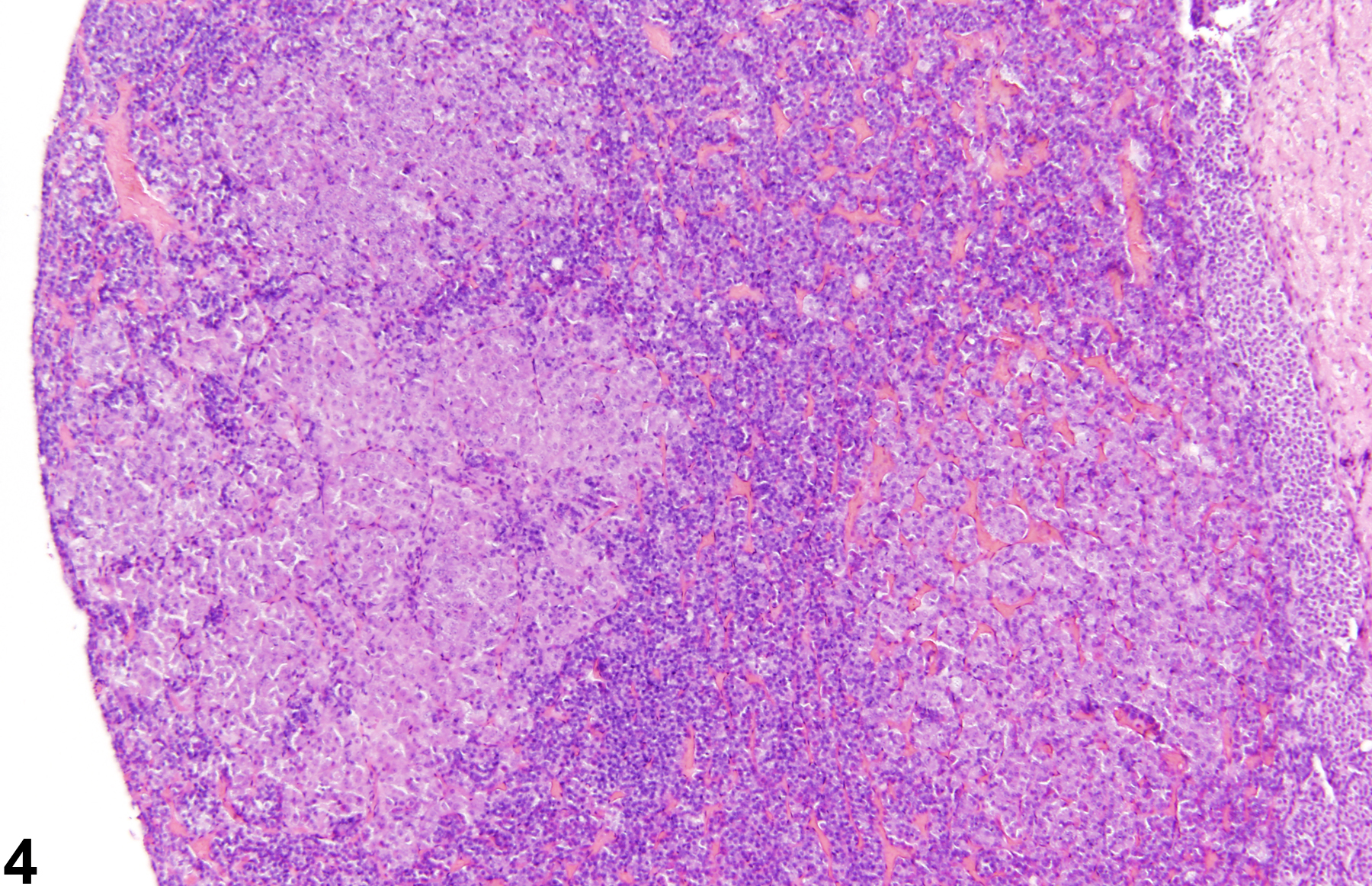
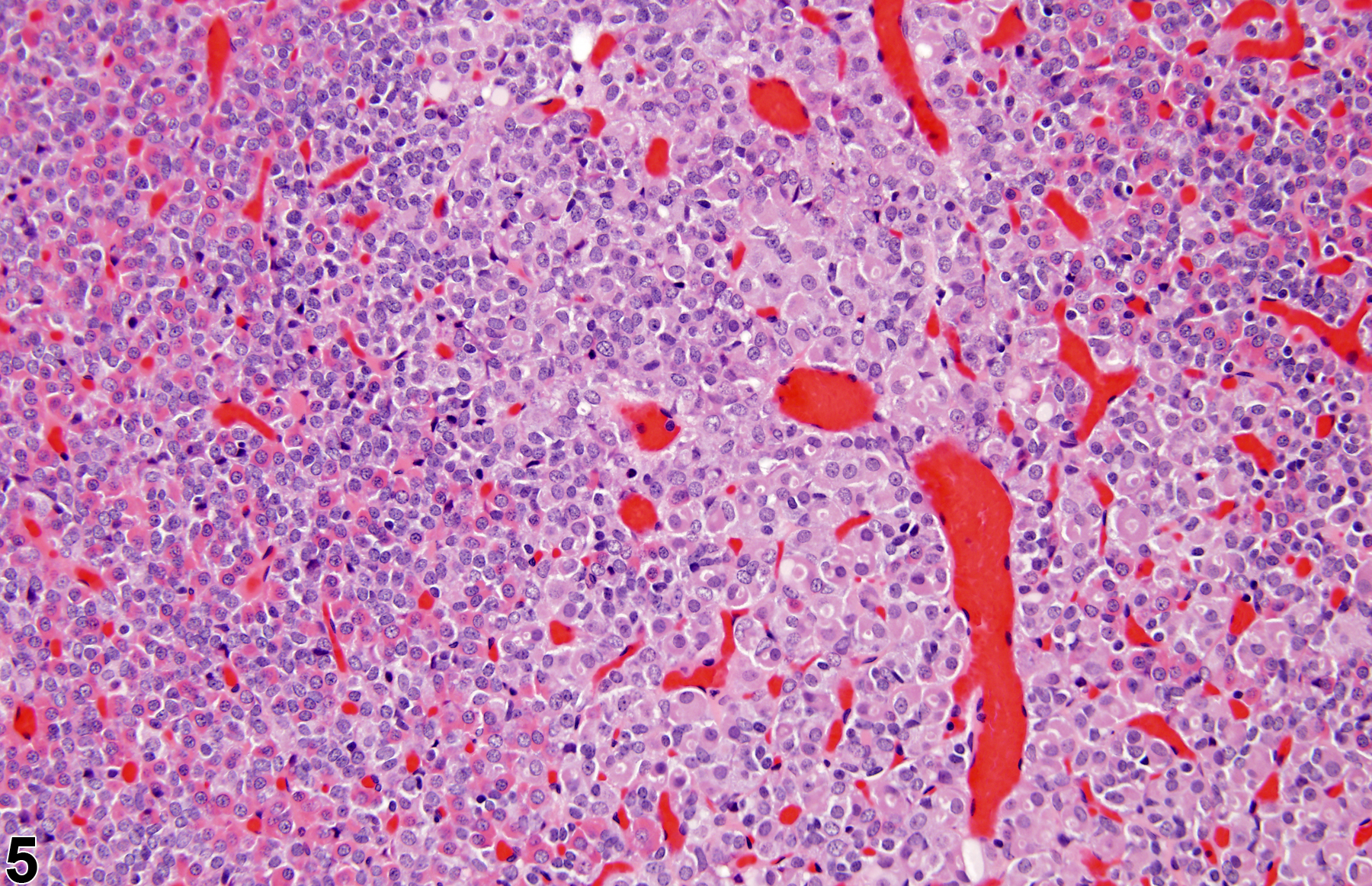
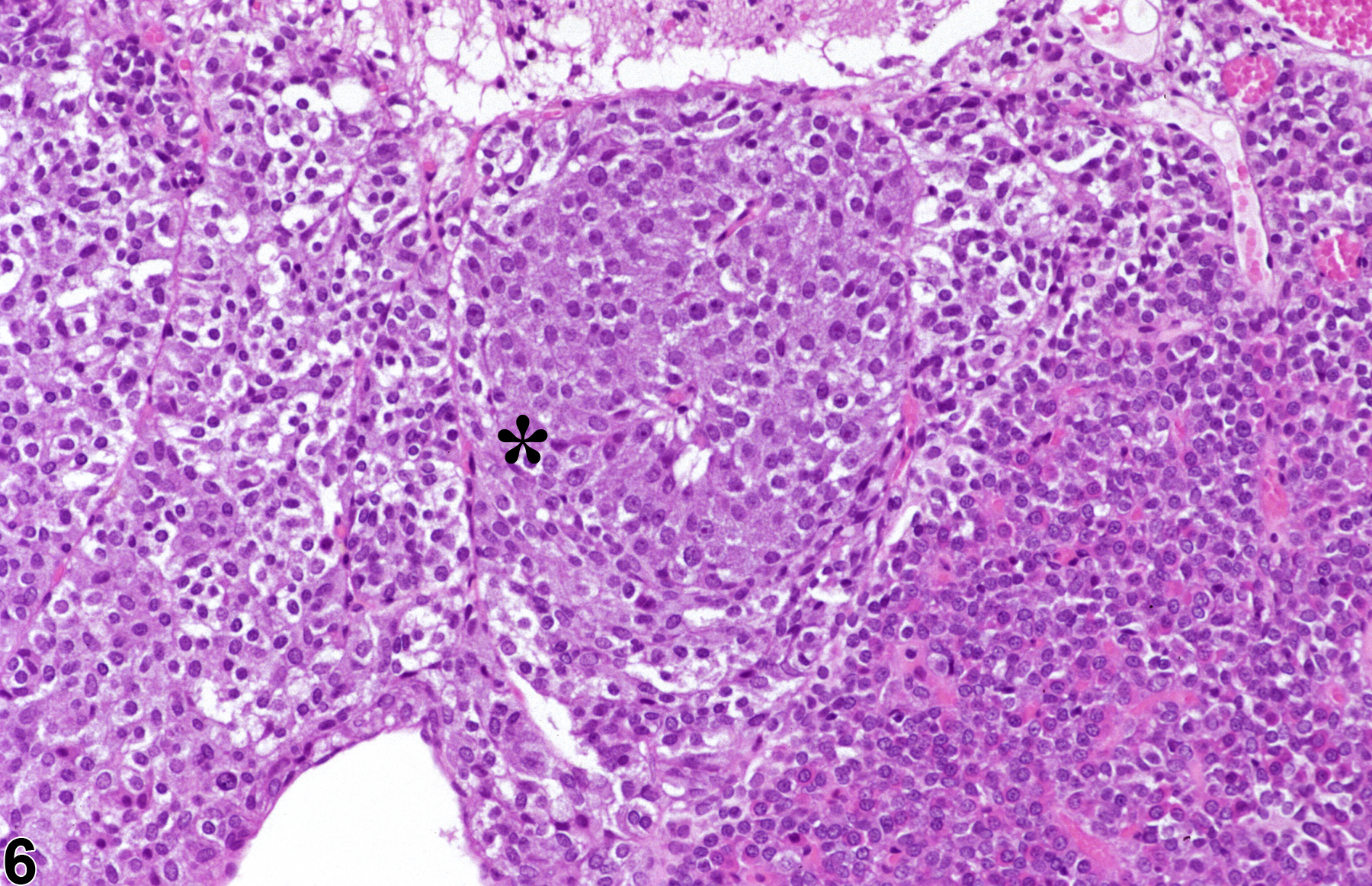
Focal hyperplasia of the pars intermedia (Figure 6 and Figure 7) is less common than hyperplasia of the pars distalis. The hyperplastic cells in the pars intermedia are similar to normal pars intermedia cells, and identification of a focal proliferative lesion may rely on alteration of growth pattern or asymmetrical enlargement of the pars intermedia since there may be no compression of the adjacent parenchyma. Diffuse hyperplasia may also occur and must be distinguished from a tangential section of the pars intermedia. Diffuse hyperplasia is usually of a specific cell type that can be confirmed by immunohistochemistry and typically represents a physiologic response.
There is a morphologic continuum between hyperplasia and pituitary neoplasia, with compression of the adjacent parenchyma being a primary diagnostic feature of neoplasia. Immunohistochemistry for pituitary hormones can be used to determine cell type.
Capen CC. 1983. Functional and pathologic interrelationships of the pituitary gland and hypothalamus. In: Endocrine System (Jones TC, Mohr U, Hunt RD, eds). Springer, New York, 103-120.
Abstract: http://www.springer.com/medicine/pathology/book/978-3-642-96722-1Capen CC, DeLellis RA, Yarrington JT. 1991. Endocrine system. In: Handbook of Toxicologic Pathology (Haschek WM, Rousseaux CG, eds). Academic Press, New York, 697-705.
Abstract: http://www.sciencedirect.com/science/book/9780123302151Carlton WW, Gries CL. 1983. Cysts, pituitary; rat, mouse, and hamster. In: Endocrine System (Jones TC, Mohr U, Hunt RD, eds). Springer, New York, 161-163.
Abstract: http://www.springer.com/medicine/pathology/book/978-3-642-96722-1Greaves P. 2007. Histopathology of Preclinical Toxicity Studies: Interpretation and Relevance in Drug Safety Evaluation, 3rd ed. Academic Press, Amsterdam, 953.
Abstract: http://www.sciencedirect.com/science/book/9780444527714MacKenzie WF, Boorman GA. 1991. Pituitary gland. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman G, Eustis S, Elwell M, Montgomery CA, MacKenzie W, eds). Academic Press, San Diego, 485-500.
Abstract: http://www.ncbi.nlm.nih.gov/nlmcatalog/9002563Mahler J, Elwell M. 1999. The pituitary gland. In: Pathology of the Mouse: Reference and Atlas (Maronpot RR, Boorman GA, Gaul BW, eds). Cache River Press, Vienna, IL, 491-508.
Tucker MJ. 1998. The endocrine system. In: Target Organ Pathology (Turton J, Hoodon J, eds). Taylor and Francis, London, 311-334.
Abstract: http://www.amazon.com/Target-Organ-Pathology-Basic-Text/dp/0748401571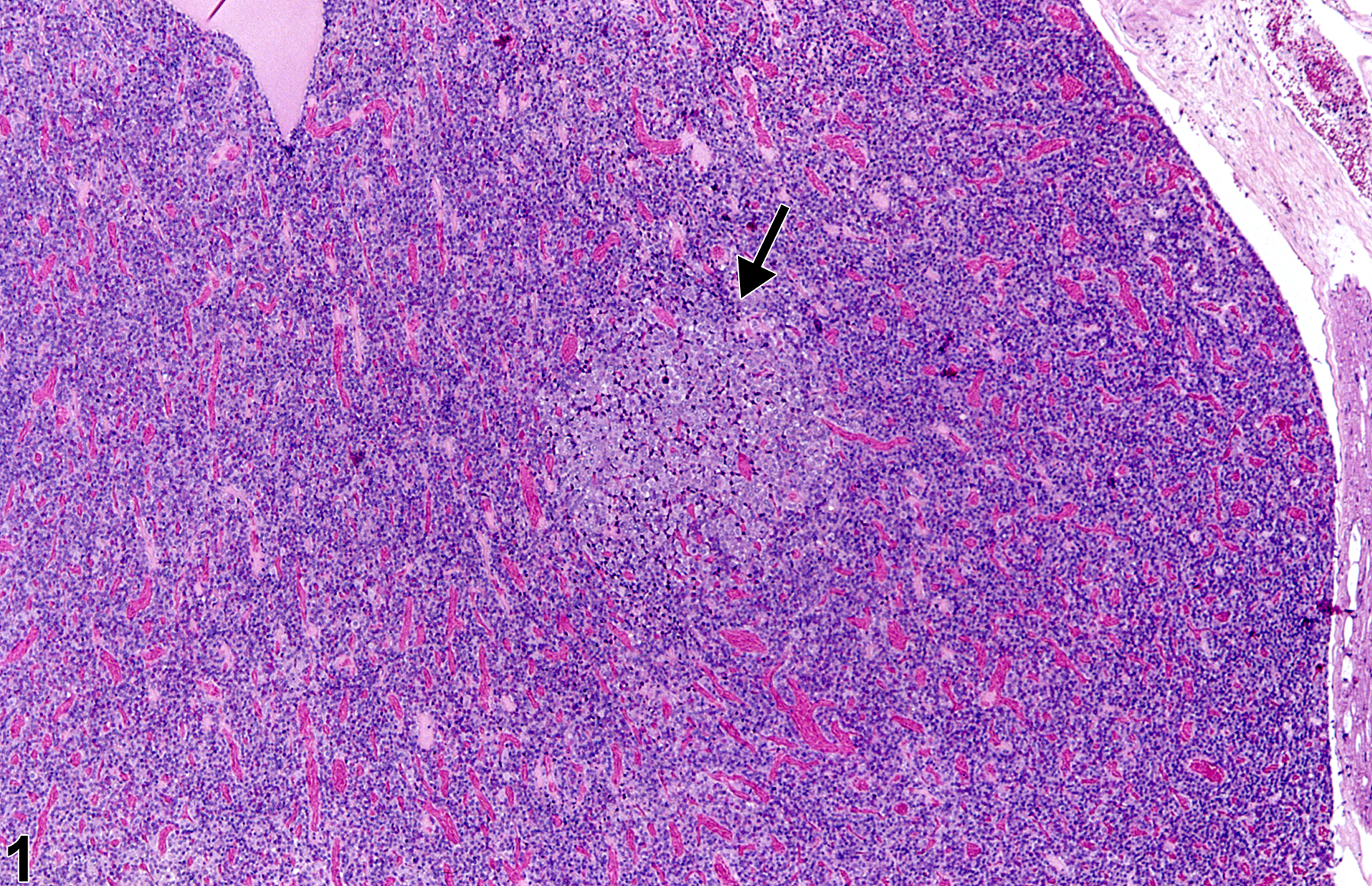
Pituitary Gland, Pars distalis - Hyperplasia in a female Harlan Sprague-Dawley rat from a chronic study. A small focus of hyperplasia (arrow) in the pars distalis is recognized by the paler staining cells.
All Images
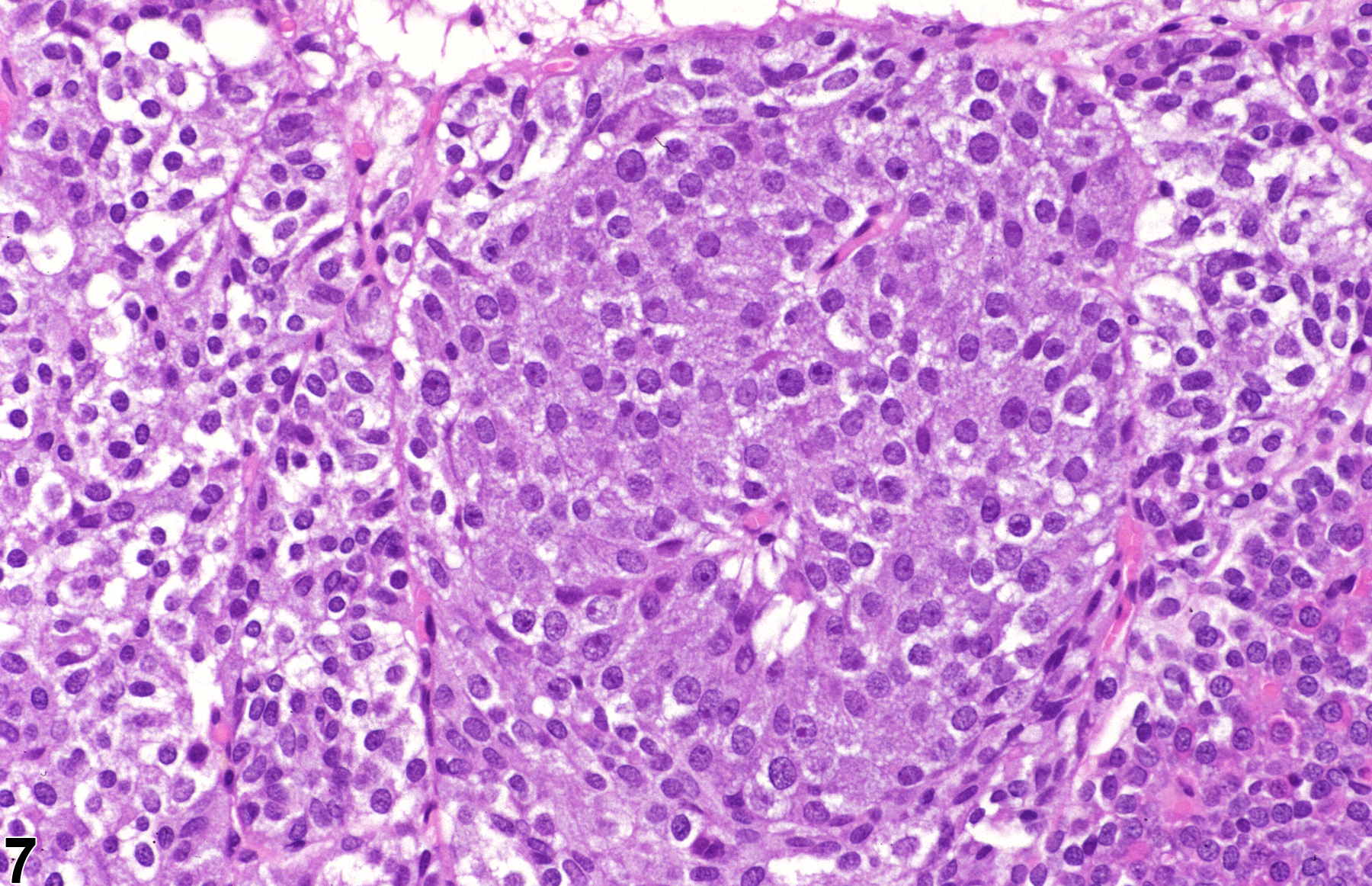
Pituitary Gland, Pars intermedia - Hyperplasia in a male F344/N rat from a chronic study. Higher magnification of Figure 6 shows that the hyperplastic focus in the pars intermedia is characterized by a circumscribed collection of cells with abundant amphophilic cytoplasm without compression of the adjacent normal parenchyma.