Hematopoietic System
Bone Marrow - Inflammation
Narrative
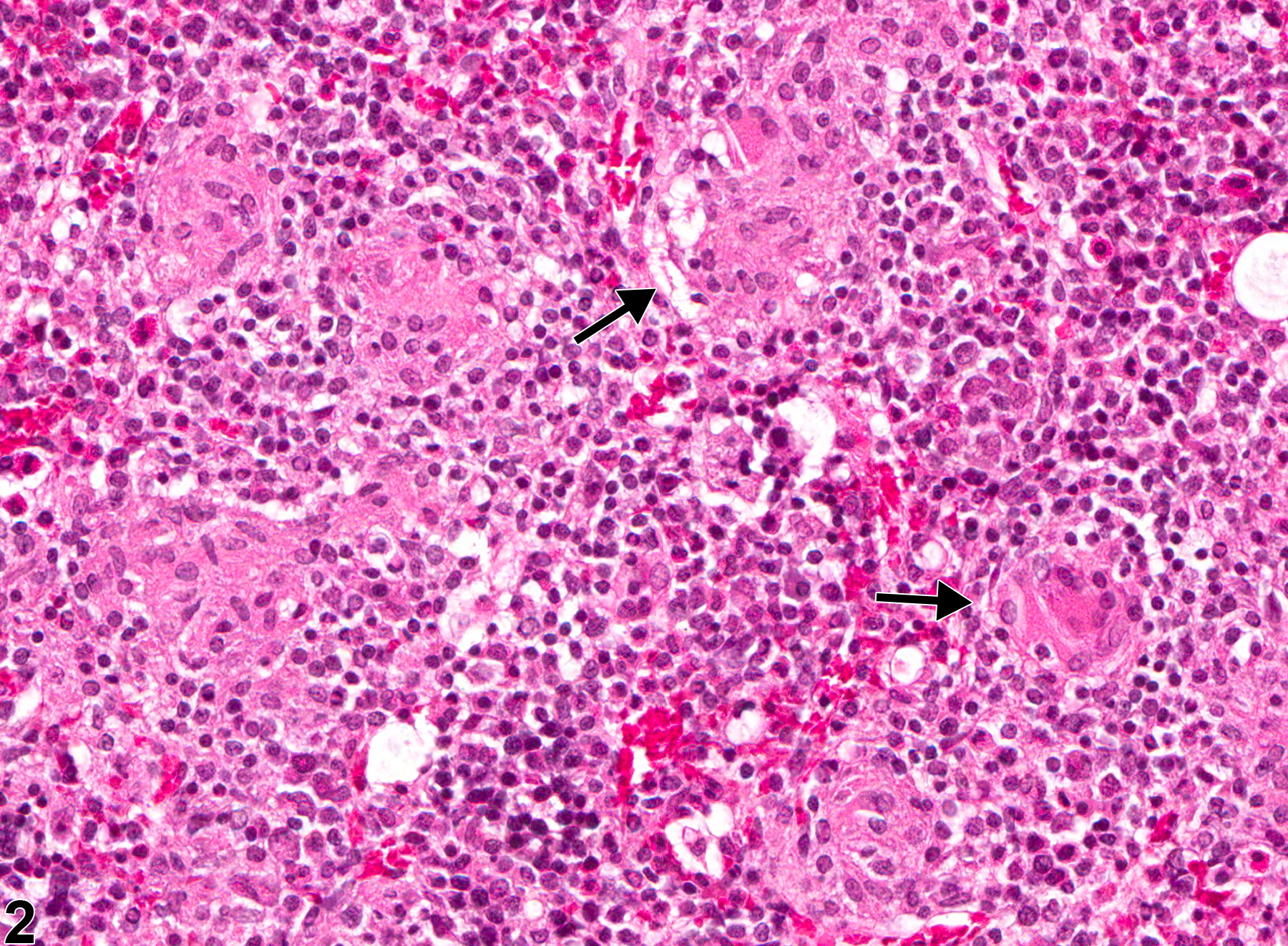
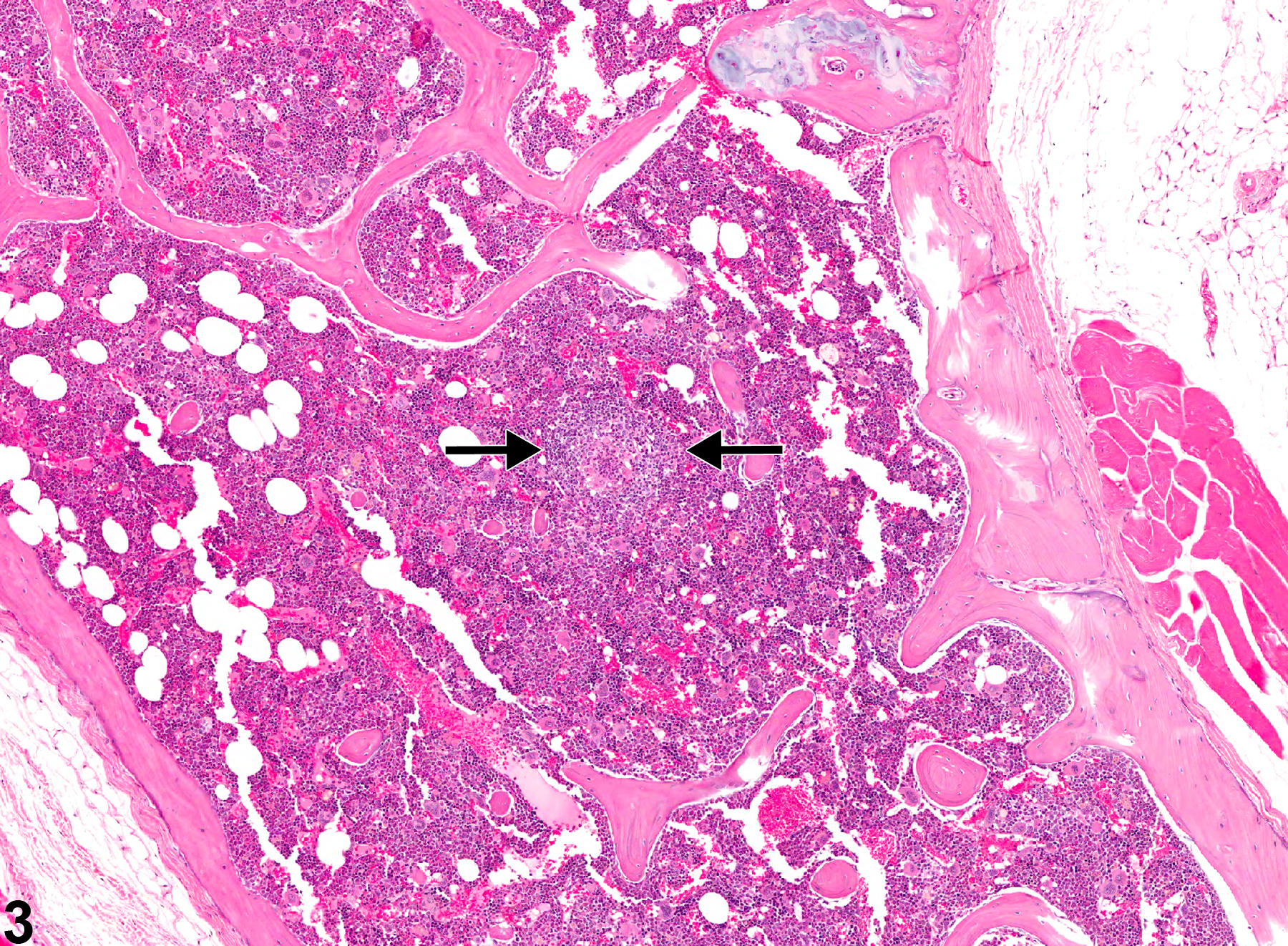
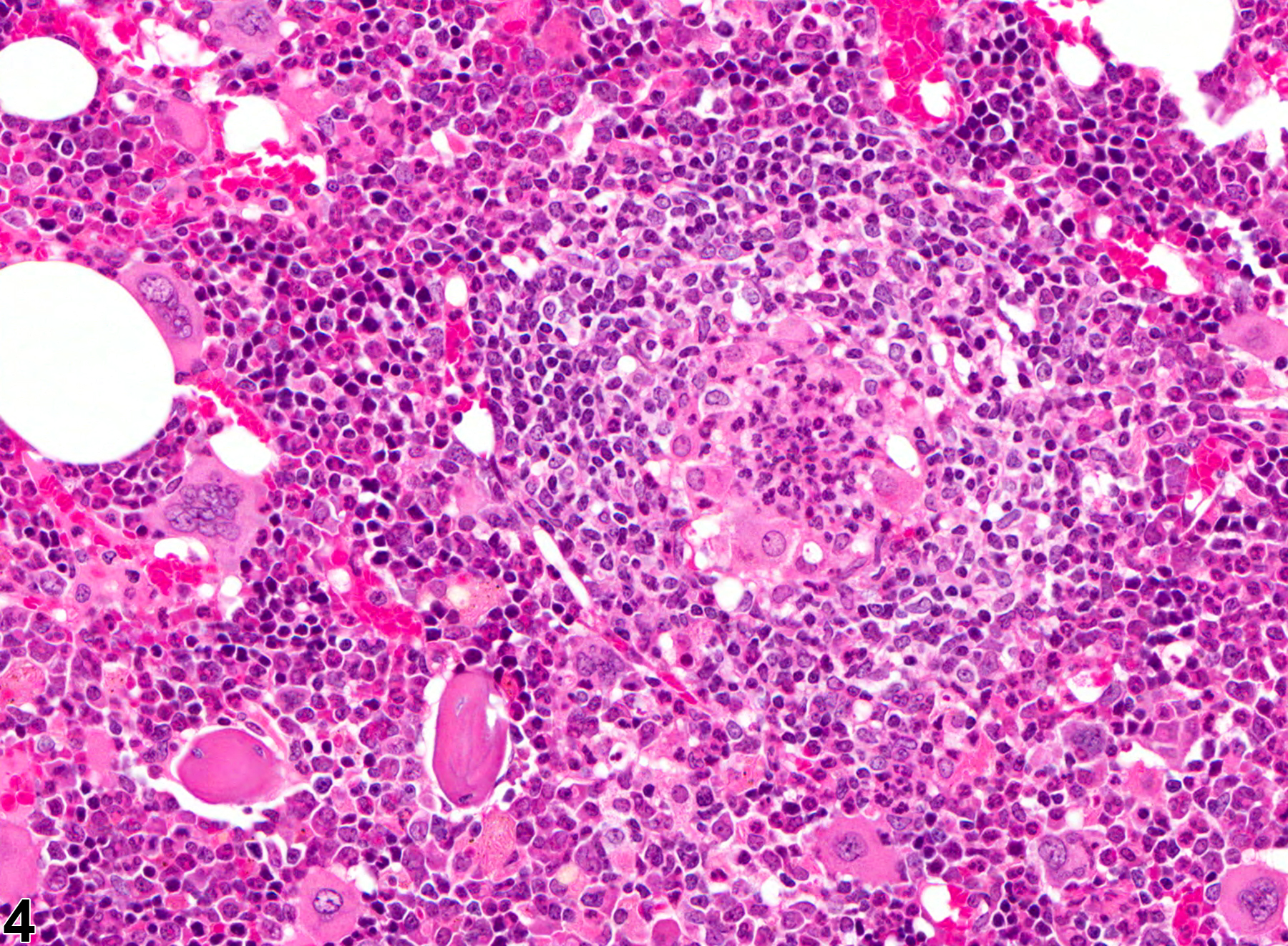
Occasionally, granulomatous inflammation is associated with lipid vacuoles that are usually smaller than the vacuoles of marrow adipocytes and are seen within macrophages and extracellularly. These lesions appear to be similar to the so-called lipid granulomas that have been described in human and canine bone marrow. Granulomatous inflammation may be associated with compound administration or infectious agents but is sometimes a nonspecific finding.
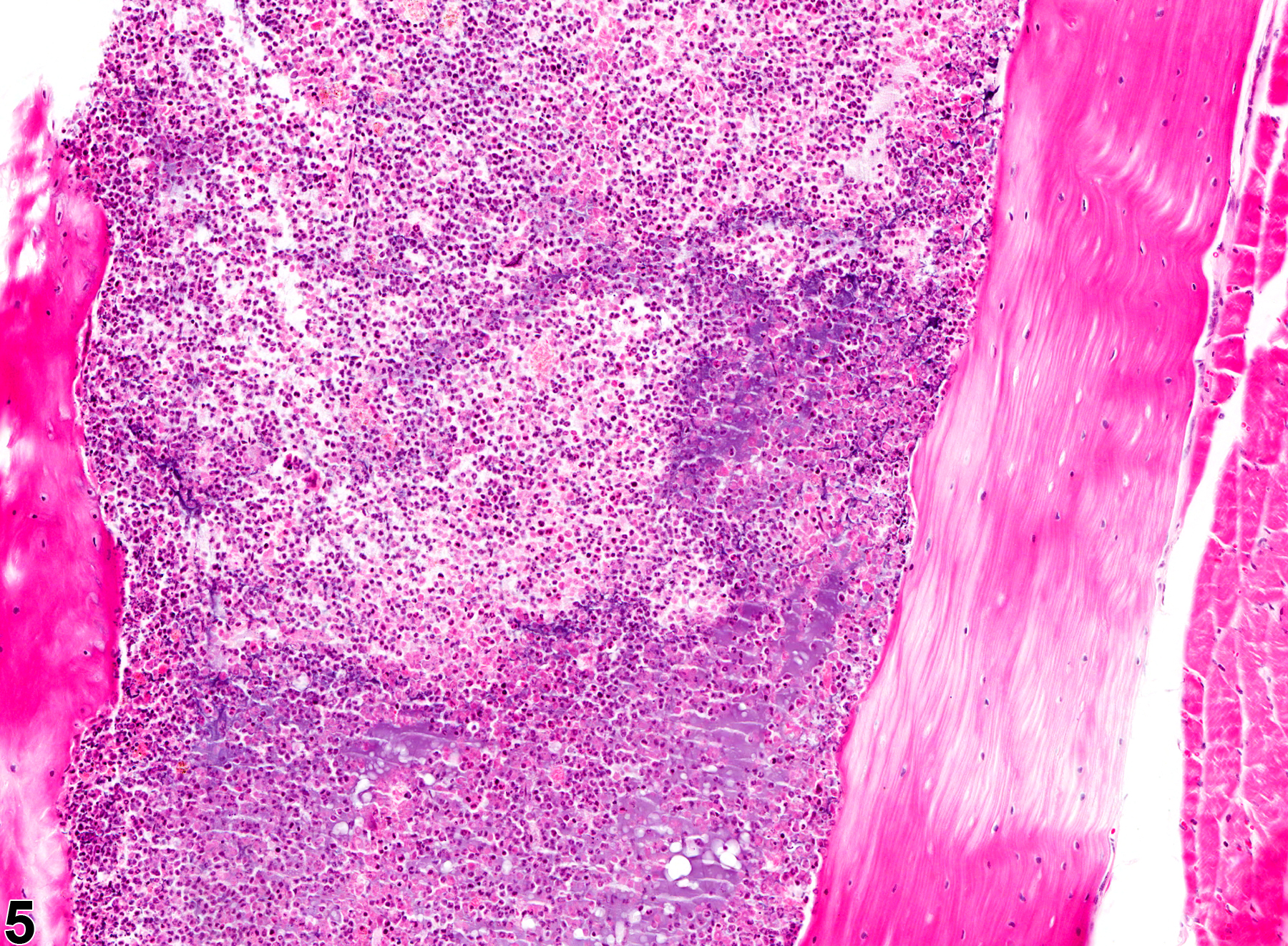
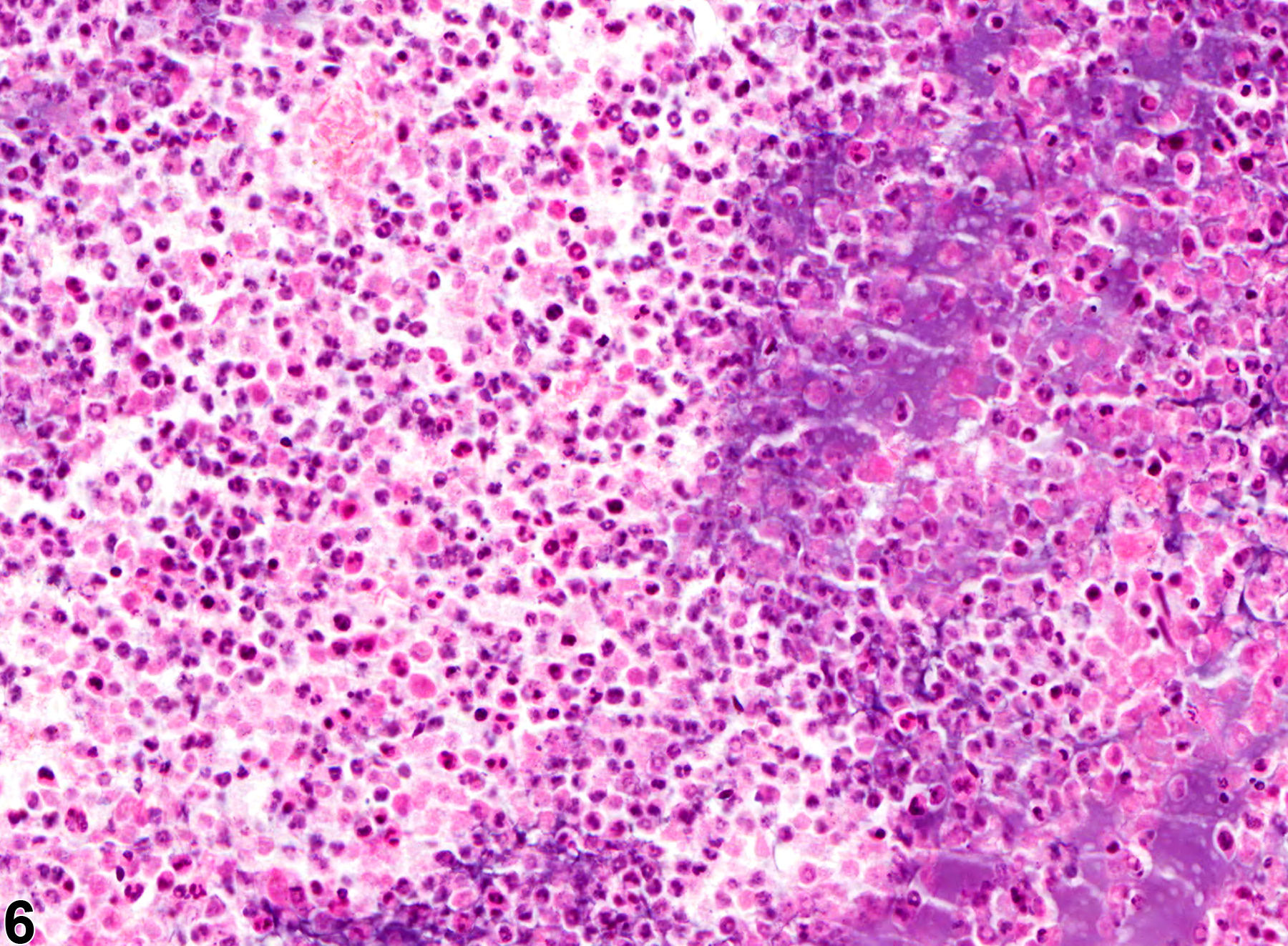
Suppurative inflammation, as occurs with bacterial sepsis, is rarely observed in the bone marrow of rodents involved in toxicologic studies. It consists of aggregates of nondegenerate and degenerate neutrophils (Figure 5 and Figure 6). Cell debris from the resident hematopoietic cells and the infiltrating leukocytes, as well as proteinaceous fluid, fibrin, and fewer lymphocytes, plasma cells, and macrophages, may also be present within the aggregates. Additional findings may include dilated sinusoids, interstitial edema, and/or hemorrhage.
In NTP studies, there are three other standard categories of inflammation: acute, chronic, and chronic-active. Briefly, in acute inflammation, the predominant infiltrating cell is the neutrophil, though fewer macrophages and lymphocytes may also be present. Lymphocytes predominate in chronic inflammation; lymphocytes also predominate in chronic-active inflammation, but there are also a significant number of neutrophils—both lesions may contain macrophages. These three other categories of inflammation are uncommon or are difficult to appreciate in the bone marrow because neutrophils are a resident population and lymphocytes are not easily identified—appearing very similar to erythroid precursors.
Bain BJ, Clark DM, Lampert IA, Wilkins BS. 2001. Bone Marrow Pathology, 3rd ed. Blackwell, Ames, IA, 90-140.
Abstract: http://onlinelibrary.wiley.com/book/10.1002/9780470757130MacKenzie WF, Eustis SL. 1990. Bone marrow. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman GA, Eustis SL, Elwell MR, Montgomery CA, Mackenzie WF, eds). Academic Press, San Diego, 315-337.
Abstract: http://www.ncbi.nlm.nih.gov/nlmcatalog/9002563Rosenthal NS. 2011 Bone marrow findings in inflammatory, infectious and metabolic disorders. In: Hematopathology (Jaffe ES, Harris NL, Vardiman JW, Campo E, Arber DA, eds). Elsevier Saunders, St Louis, 194-207.
Abstract: http://www.us.elsevierhealth.com/Medicine/Pathology/book/9780721600406/Hematopa…Travlos GS. 2006. Histopathology of the bone marrow. Toxicol Pathol 34:566-598.
Abstract: http://tpx.sagepub.com/content/34/5/566.abstractWeiss DJ. 2010. Chronic inflammation and secondary myelofibrosis. In: Schalm’s Veterinary Hematology, 5th ed (Weiss DJ, Wardrop KJ, eds). Wiley-Blackwell, Ames, IA, 112-117.
Abstract: http://vet.sagepub.com/content/40/2/223.1Weiss DJ. 2010. Myelonecrosis and acute inflammation. In: Schalm’s Veterinary Hematology, 5th ed (Weiss DJ, Wardrop KJ, eds). Wiley-Blackwell, Ames, IA, 106-111.
Abstract: http://vet.sagepub.com/content/40/2/223.1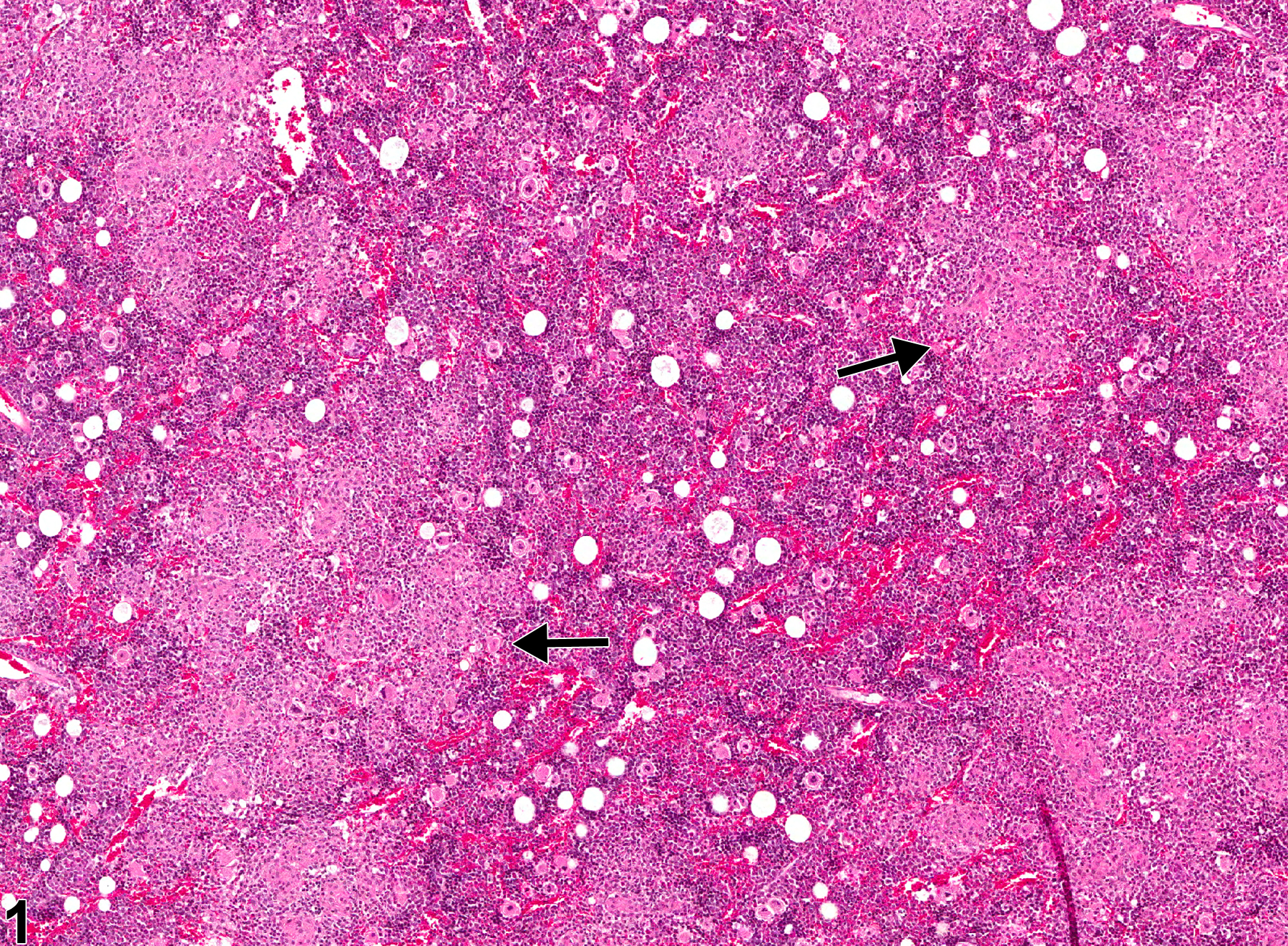
Bone marrow in a male F344/N rat from a chronic study. This low-power view shows relatively pale eosinophilic areas of granulomatous inflammation consisting of aggregates of macrophages (arrows).