Immune System
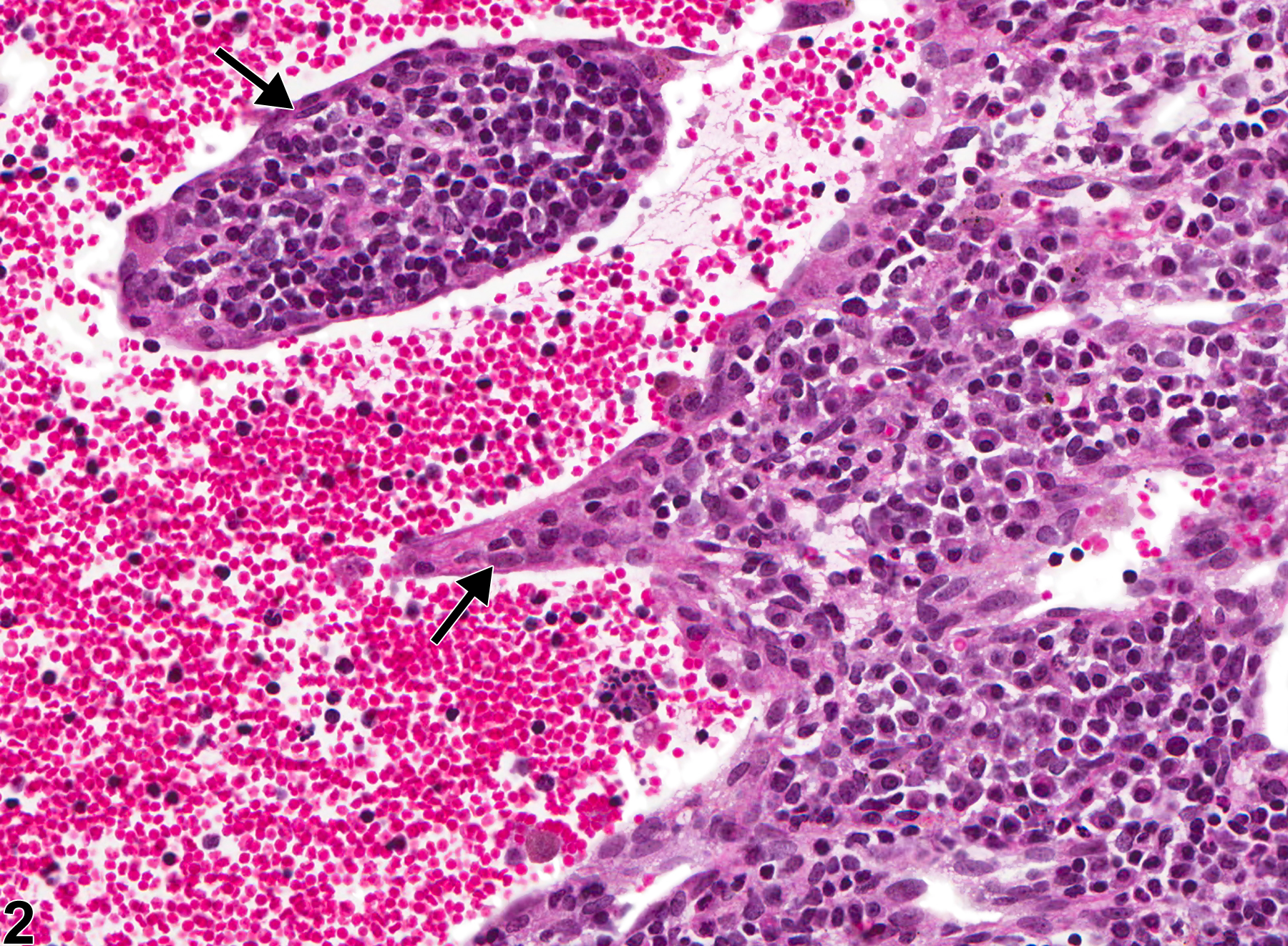
Lymph Node - Angiectasis
Narrative
Elmore SA. 2006. Histopathology of the lymph nodes. Toxicol Pathol 34:425-454.
Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1892634/Frith CH, Ward JM, Chandra M, Losco PE. 2000. Non-proliferative lesions of the hematopoietic system in rats. In: Guides for Toxicologic Pathology.TP/ARP/AFIP, Washington, DC.
Full Text: https://www.toxpath.org/docs/SSNDC/HematopoieticNonprolifRat.pdfNational Toxicology Program. 2007. NTP TR-538. Toxicology and Carcinogenesis Studies of Methyl Isobutyl Ketone (CAS No. 108-10-1) in F344/N Rats and B6C3F1 Mice (Inhalation Studies). NTP, Research Triangle Park, NC.
Abstract: https://ntp.niehs.nih.gov/go/17630Ward JM, Mann PC, Morishima H, Frith CH. 1999. Thymus, spleen, and lymph nodes. In: Pathology of the Mouse (Maronpot RR, ed). Cache River Press, Vienna, IL, 333-360.
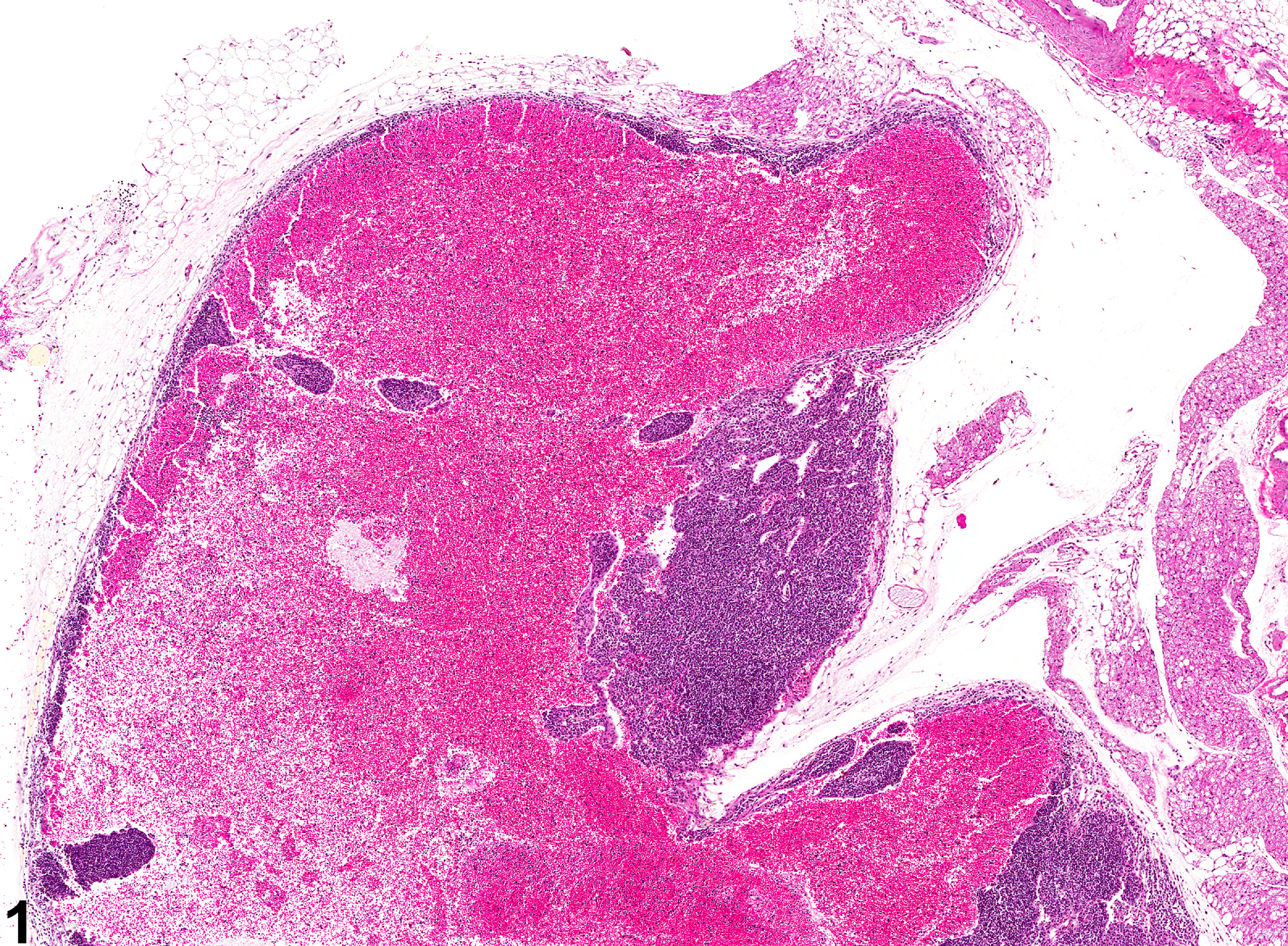
Lymph node - Angiectasis in a female B6C3F1/N mouse from a chronic study. The lymph node architecture is distorted by a markedly distended vessel.