Integumentary System
Skin - Inflammation
Narrative
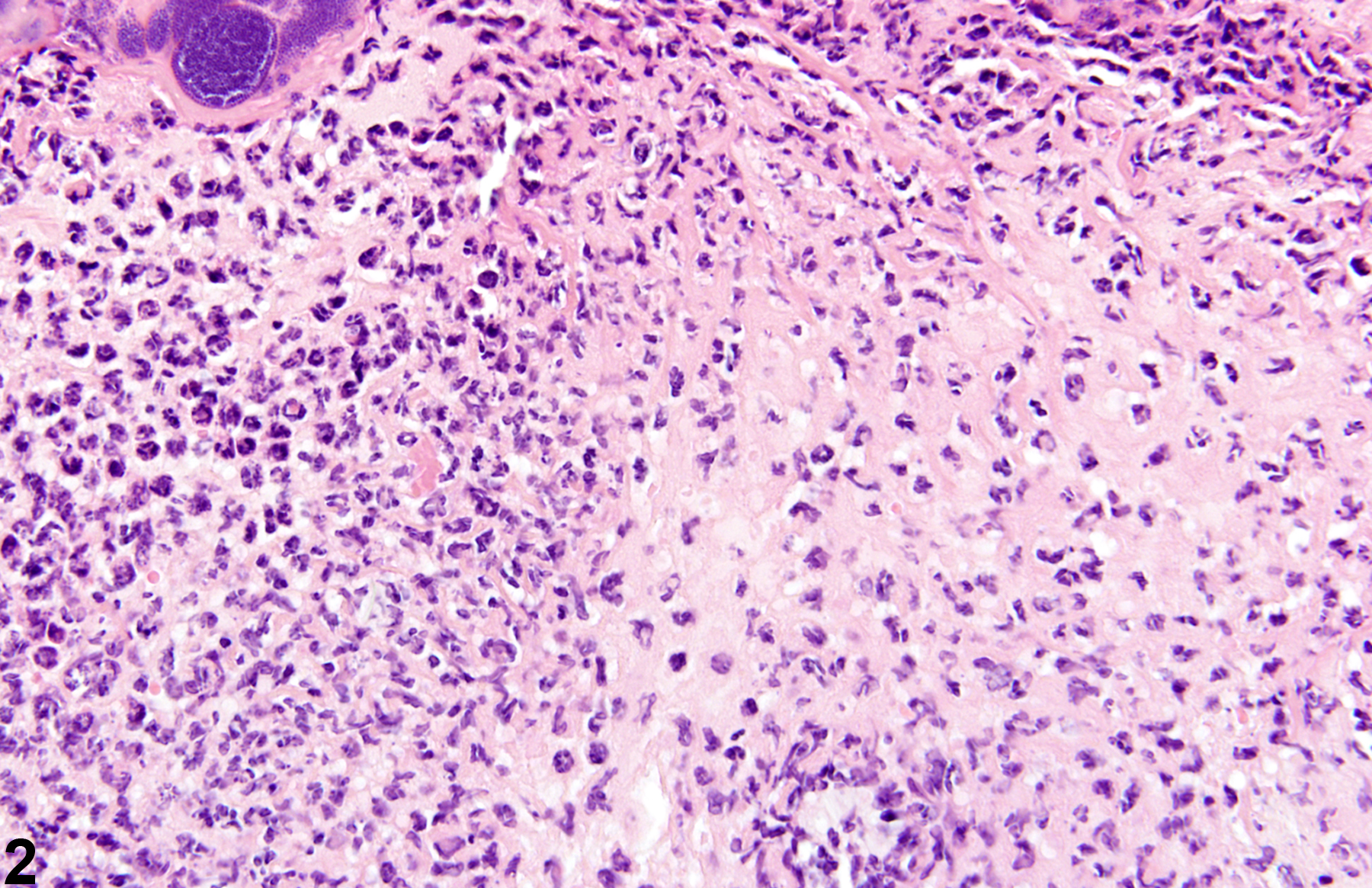
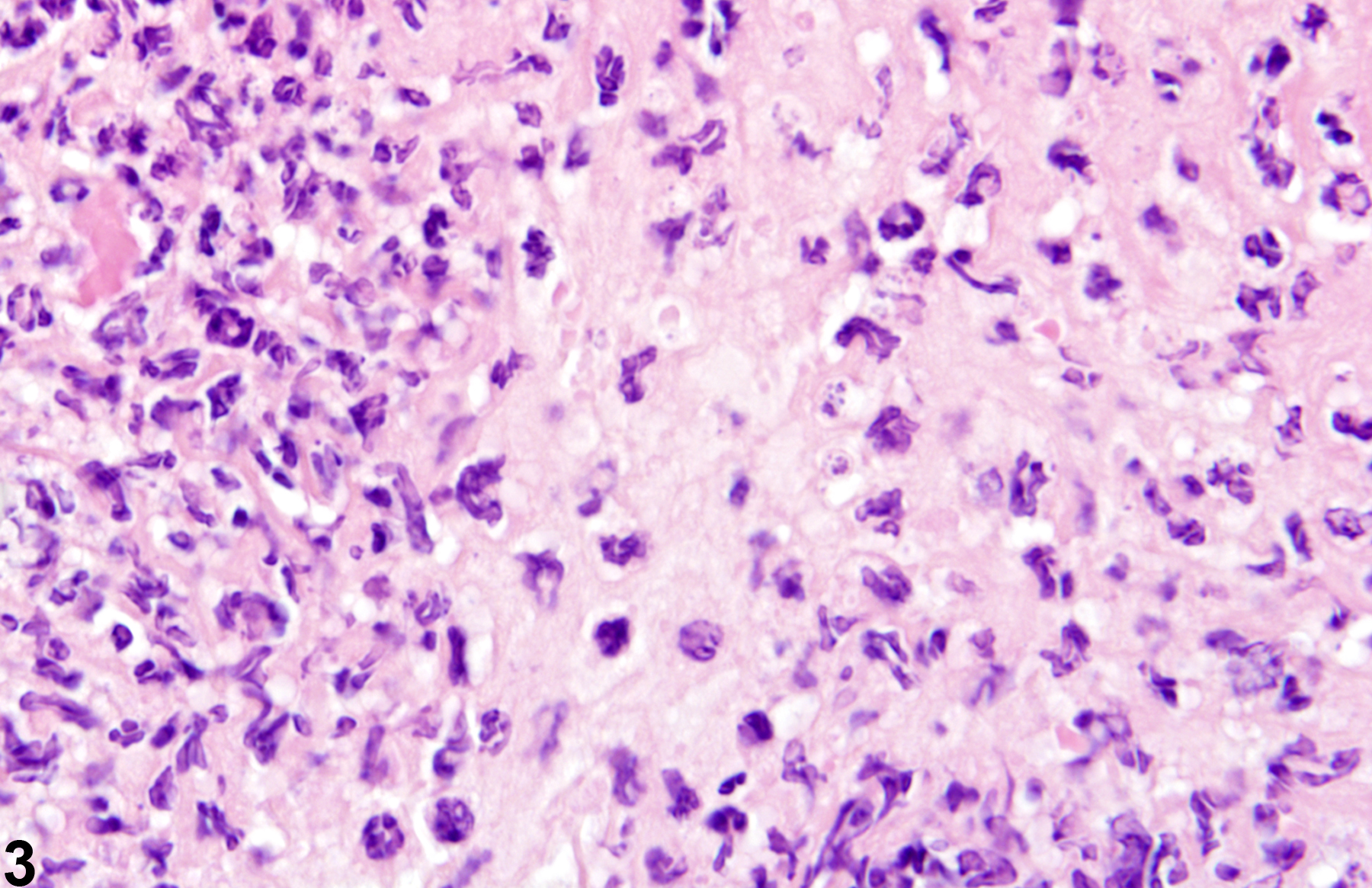
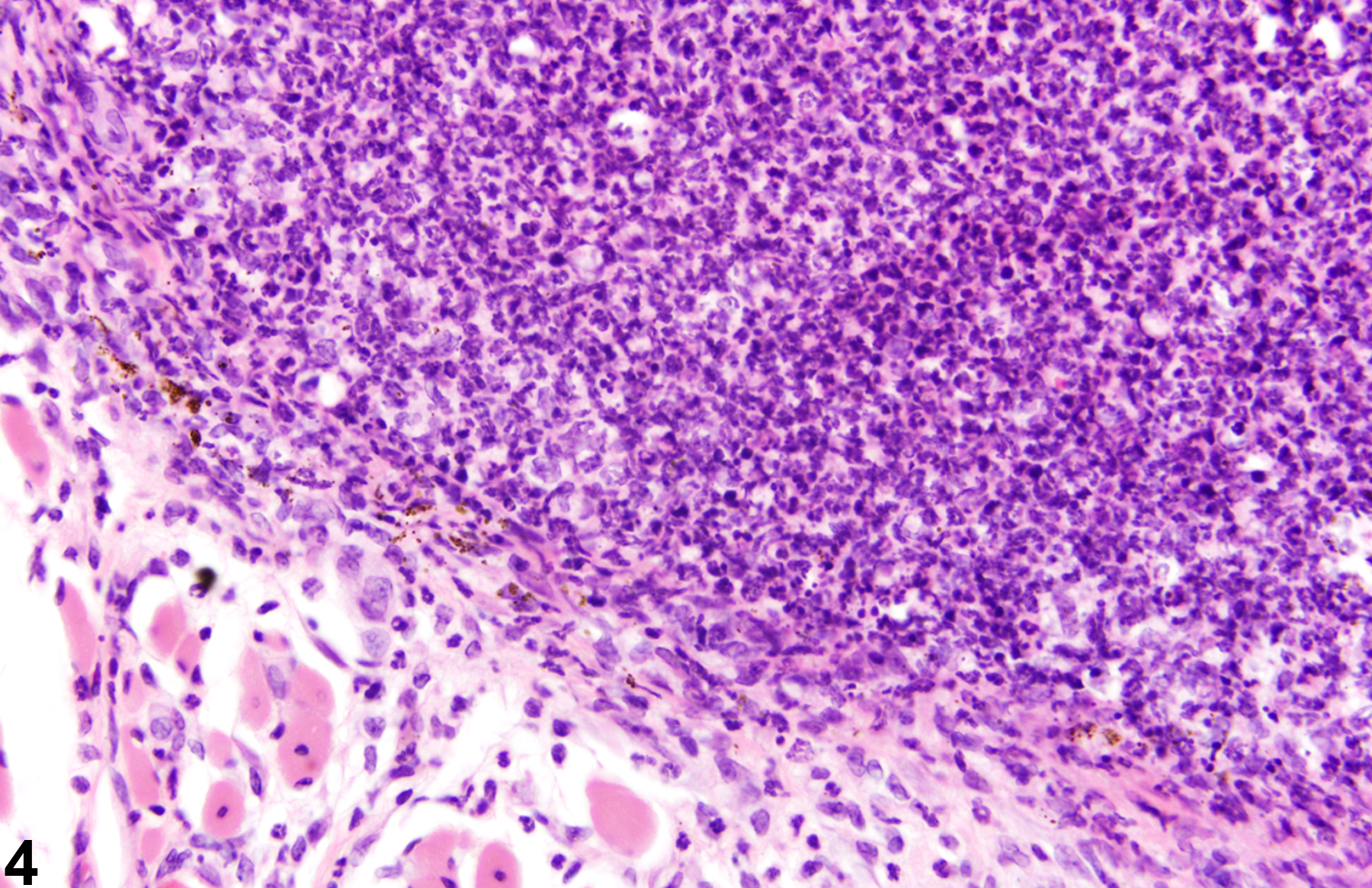
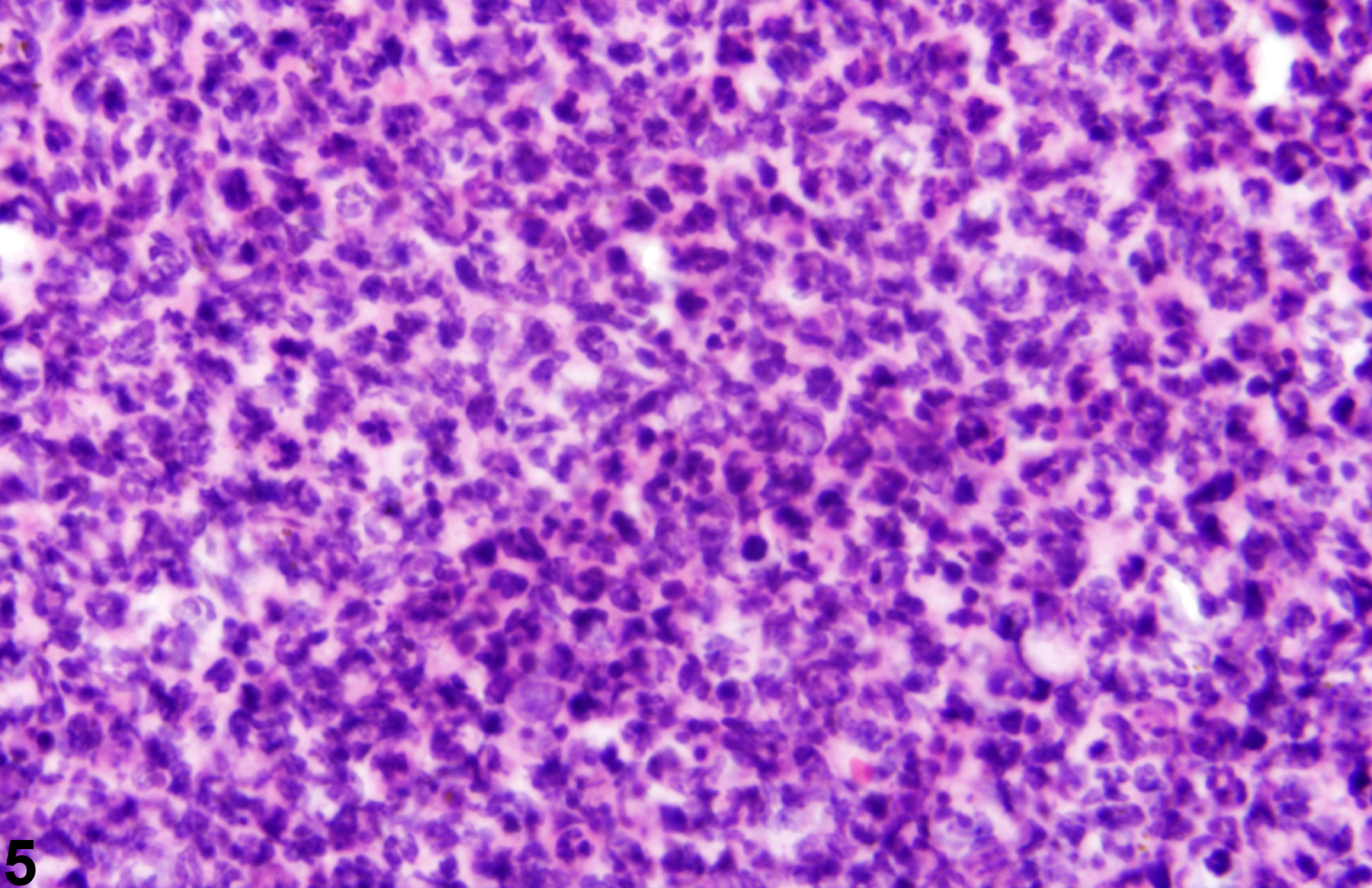
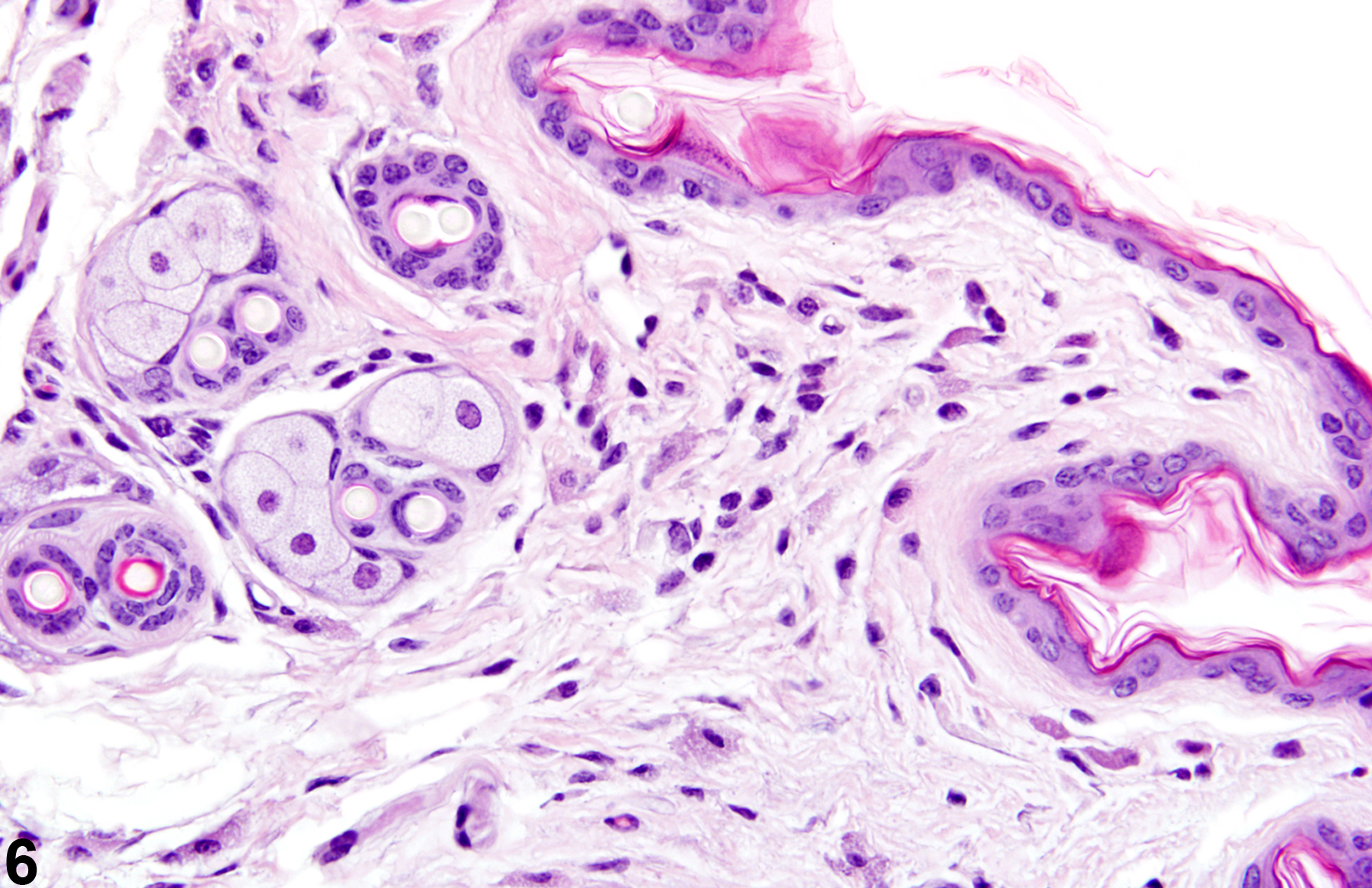
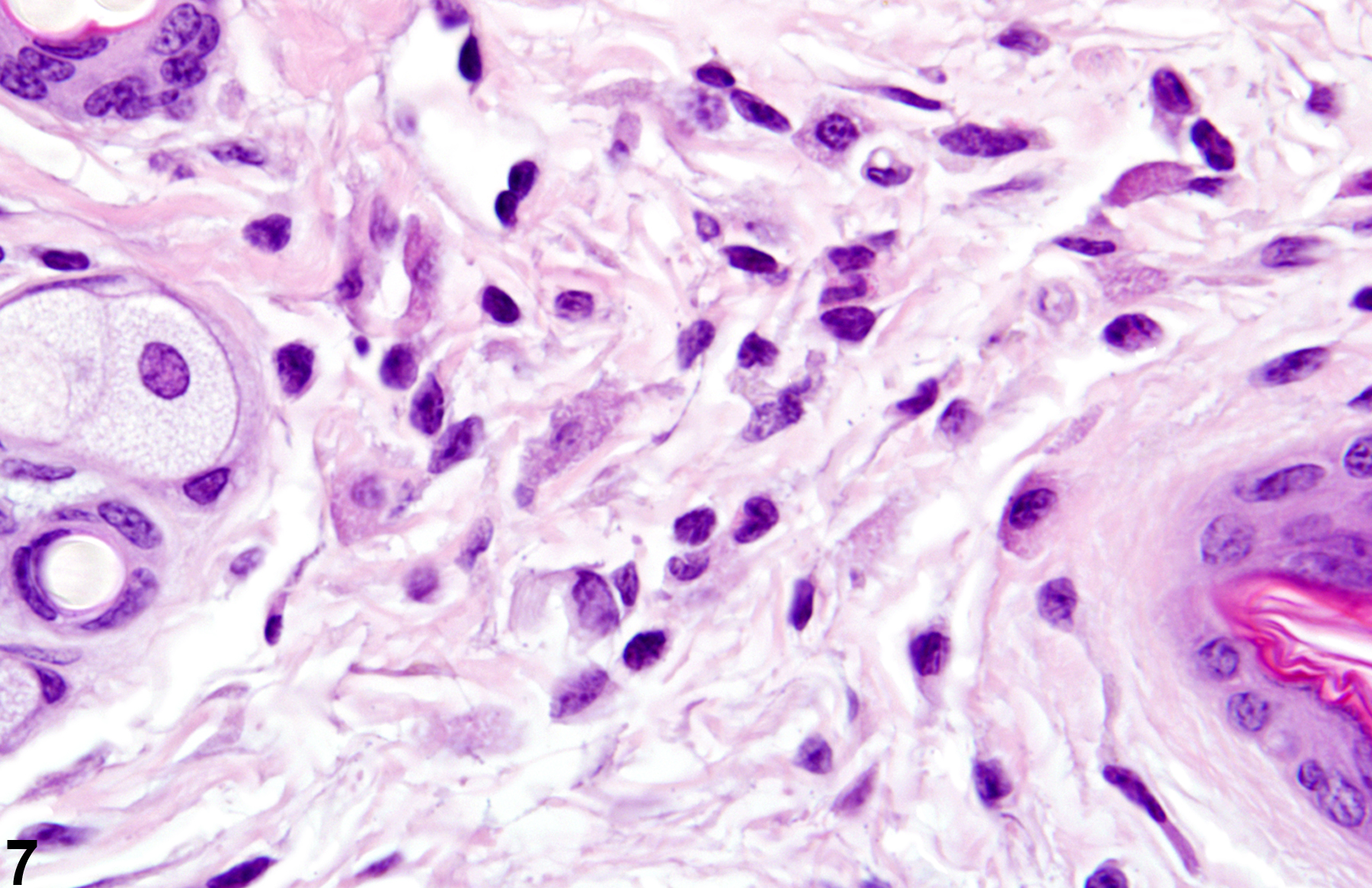
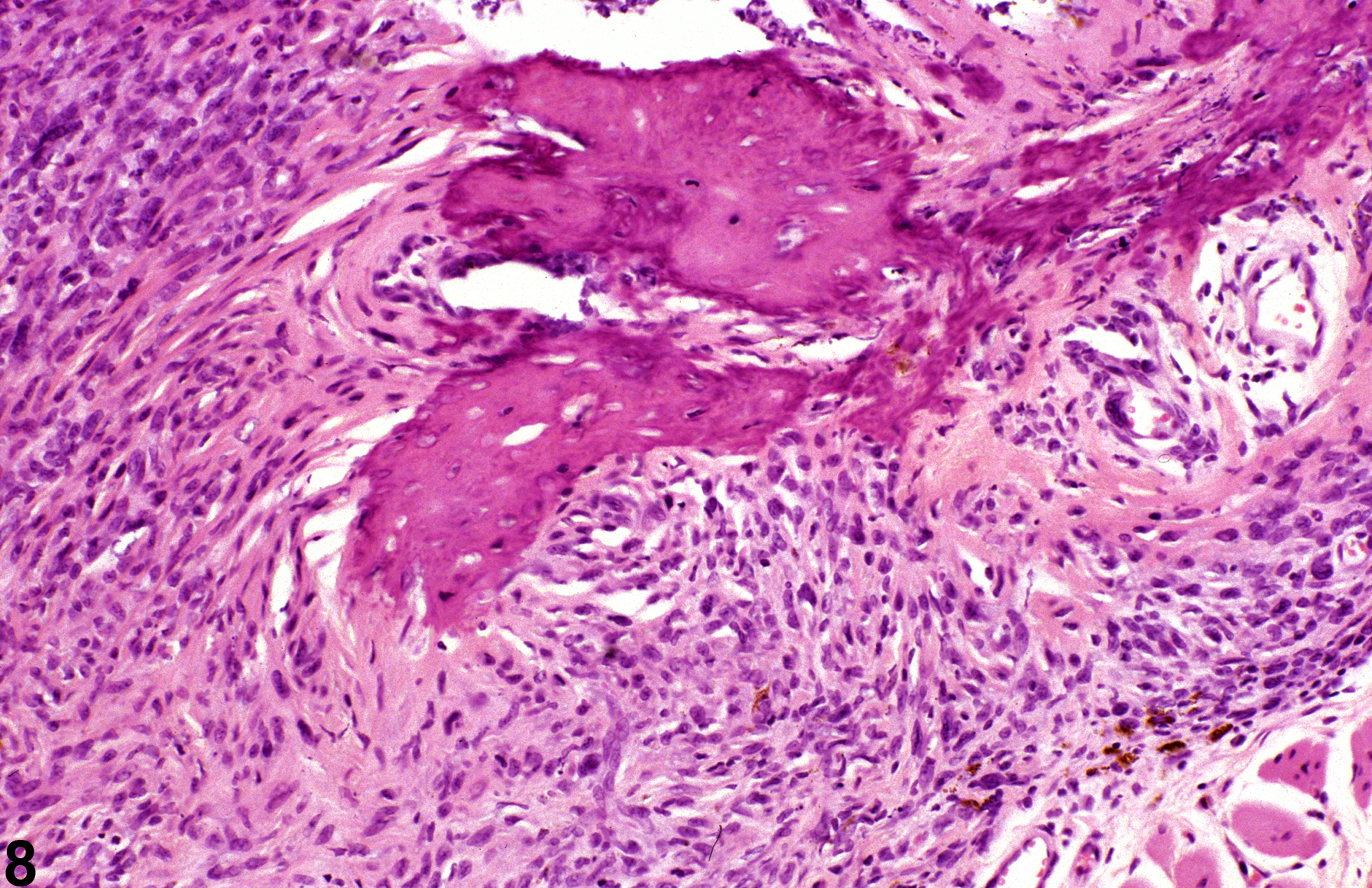
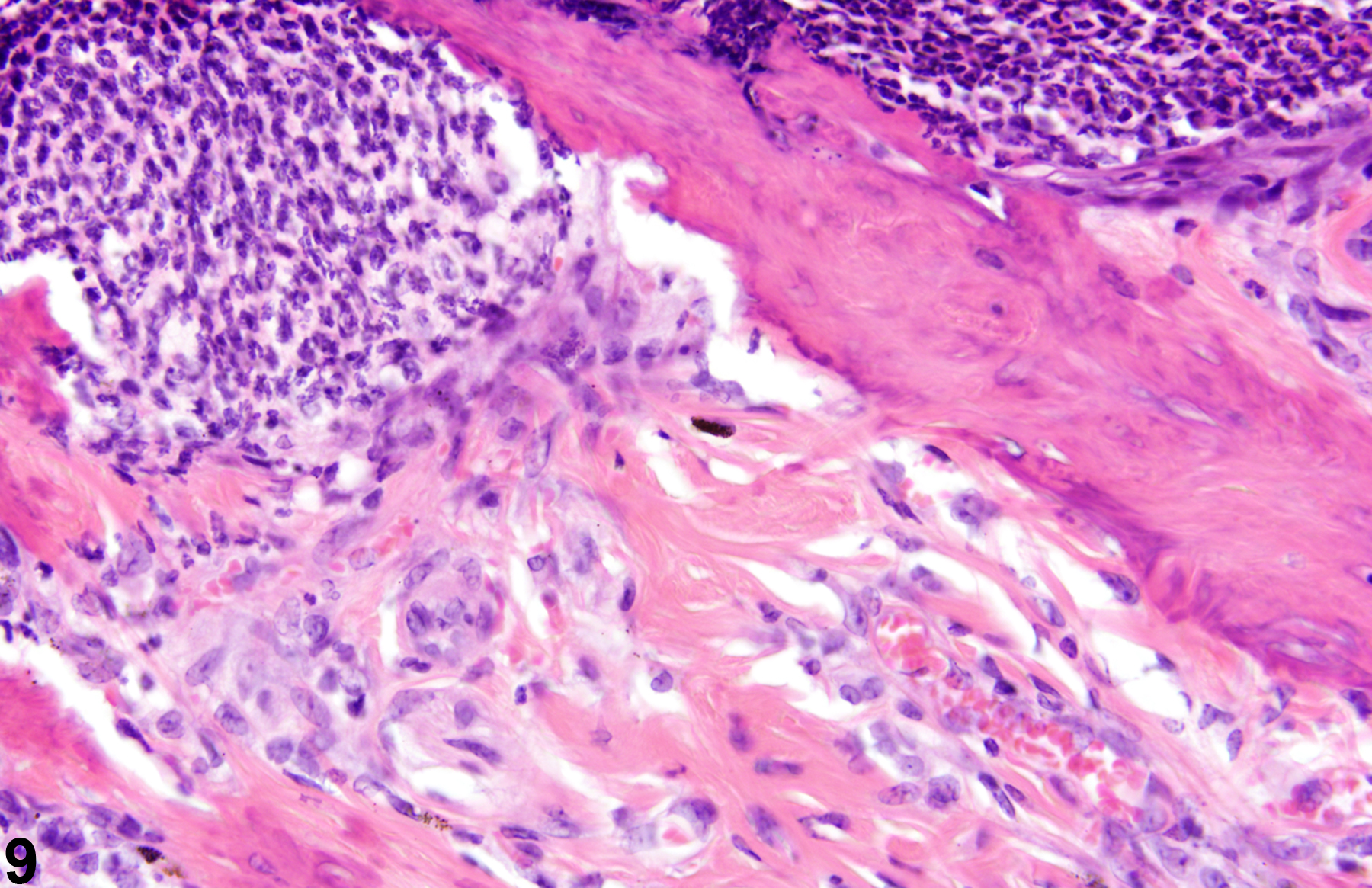
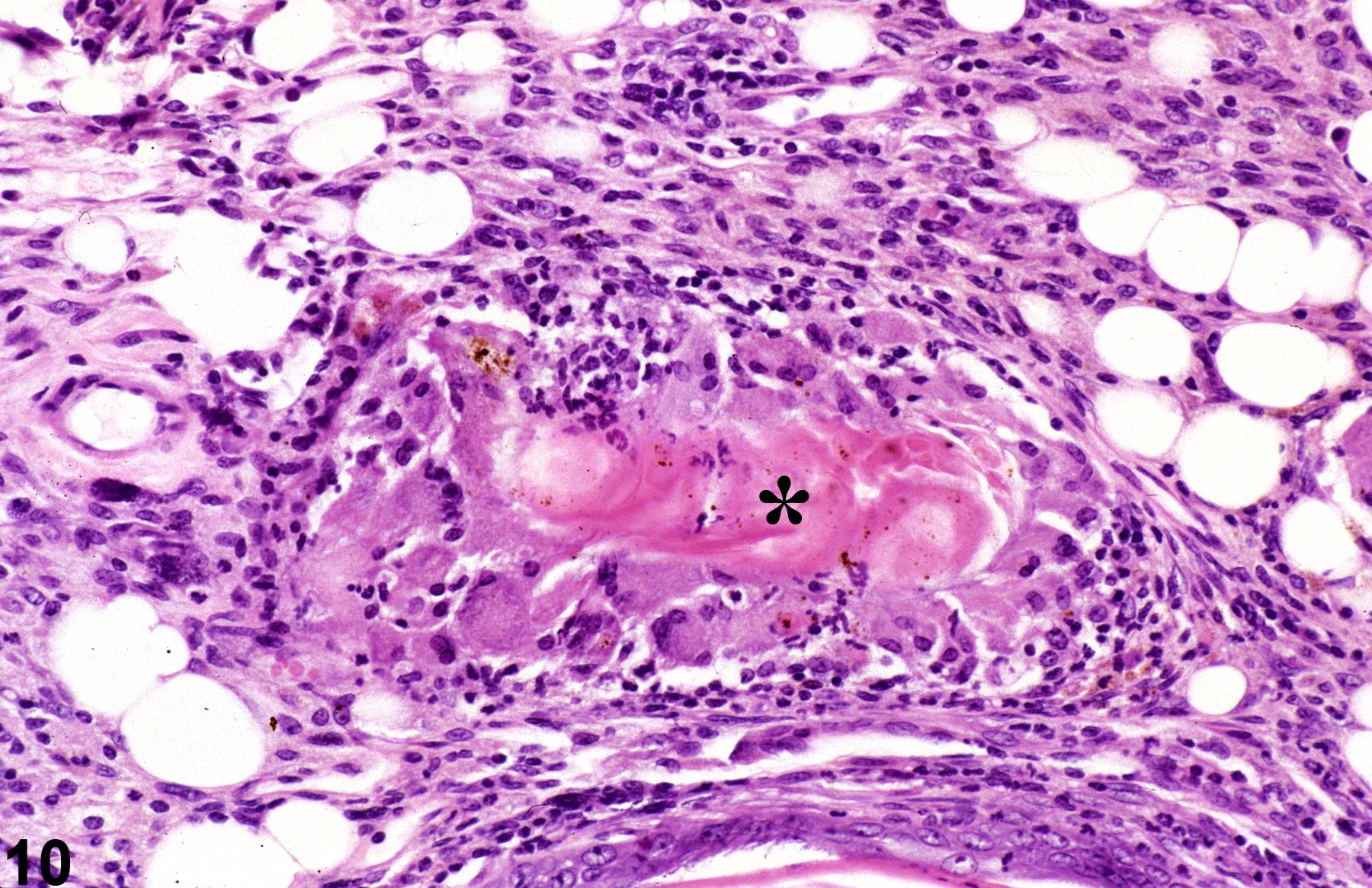
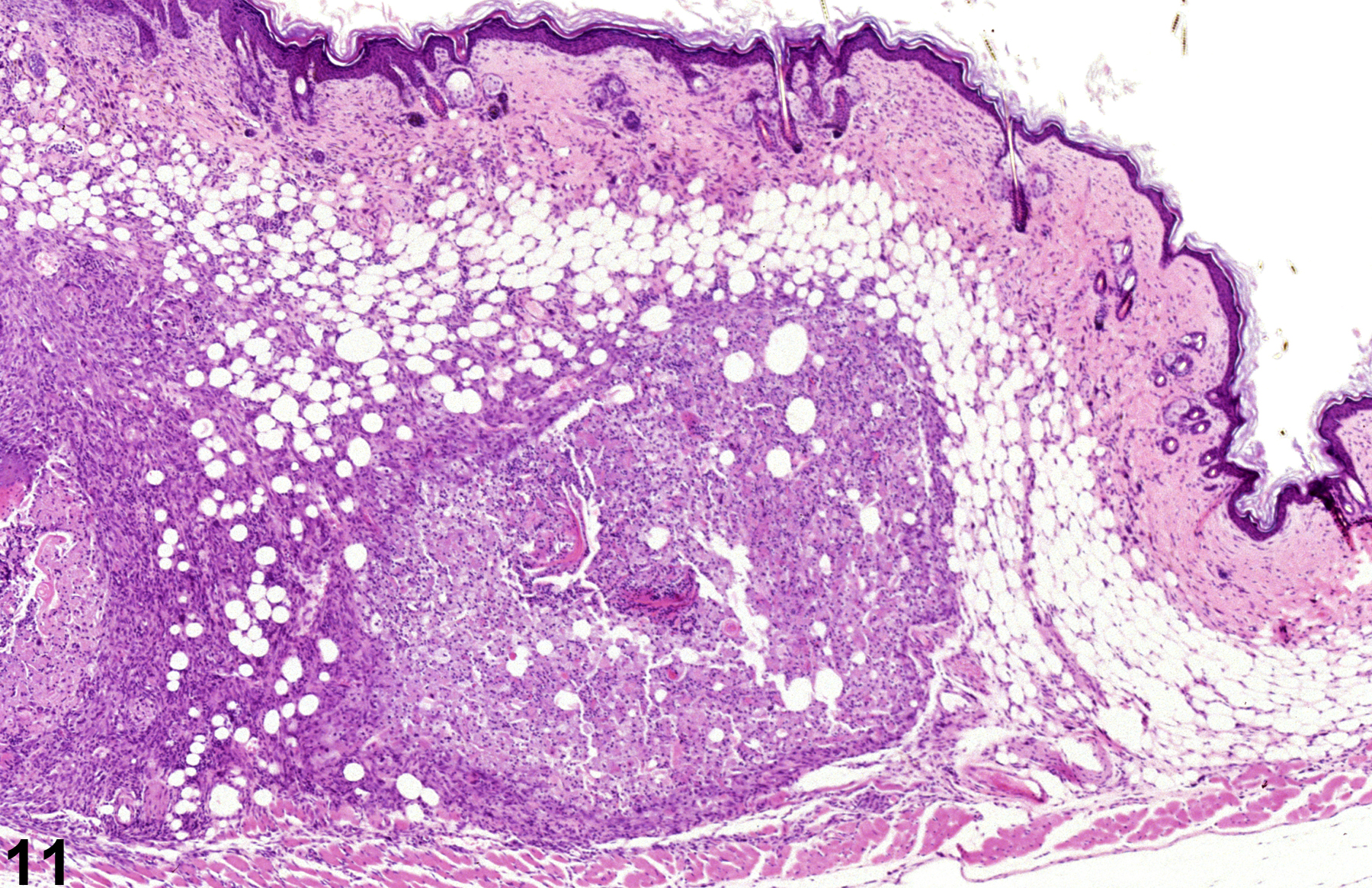
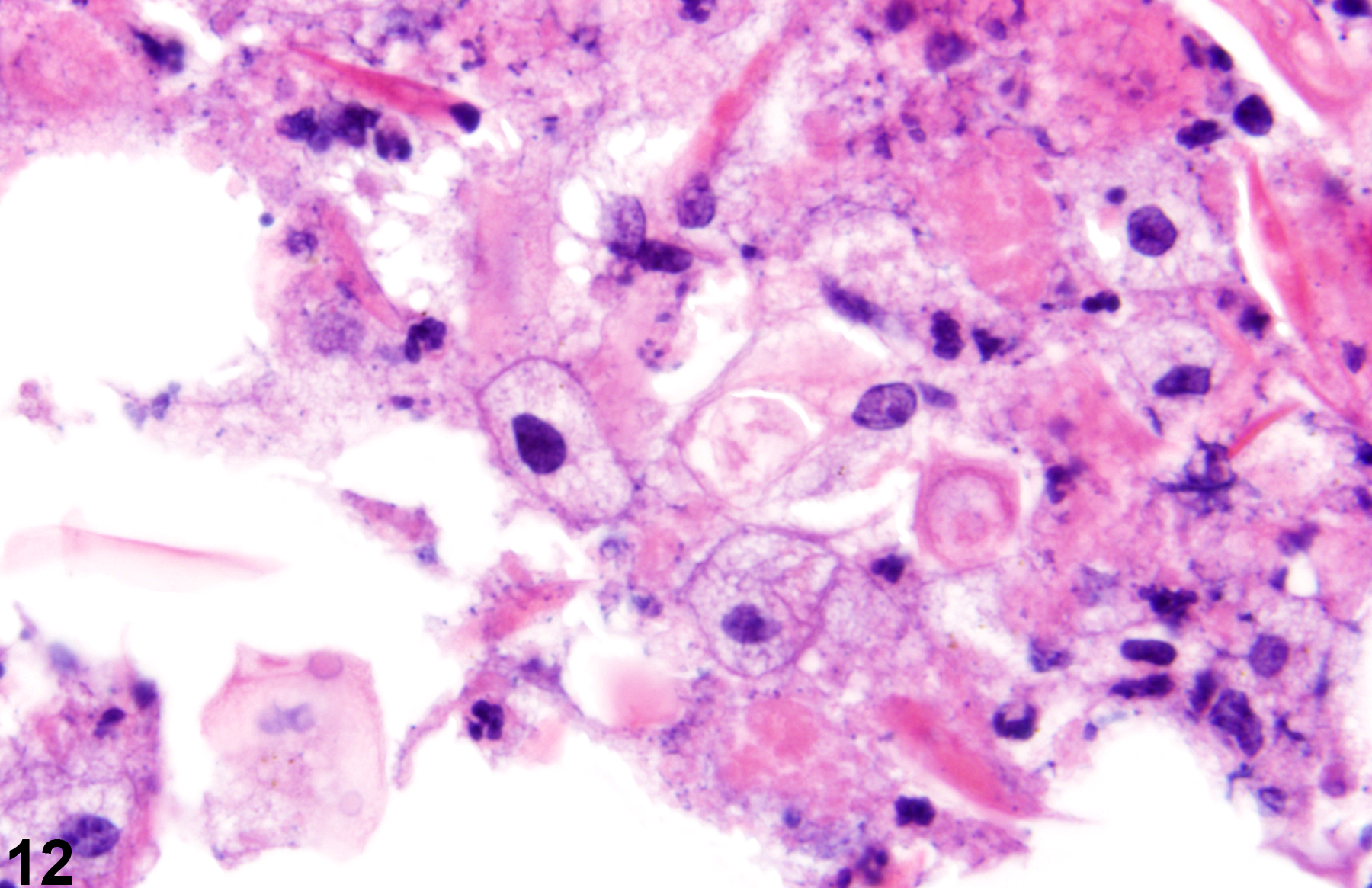
Acute inflammation (Figure 1, Figure 2, and Figure 3) in the skin is characterized by infiltration of neutrophils, which may be accompanied by eosinophils and macrophages as well as occasional mast cells, lymphocytes, and plasma cells. Suppurative inflammation is characterized by discrete pockets of degenerate neutrophils and cellular debris (Figure 4 and Figure 5). Evidence of chronicity, such as fibrosis and lymphoplasmacytic infiltrates, may also surround these pockets. Chronic inflammation (Figure 6 and Figure 7) is characterized by the presence of mononuclear cells (lymphocytes, macrophages, and plasma cells) and may be accompanied by fibrosis or the accumulation of melanin within cells in the dermis. Chronic active inflammation (Figure 8 and Figure 9) is characterized by the coexistence of elements of chronic inflammation (lymphocytes, macrophages, and fibrosis) and superimposed acute inflammation (neutrophilic and/or eosinophilic). Granulomatous inflammation (Figure 10, Figure 11, and Figure 12) is characterized by an accumulation of macrophages and multinucleated giant cells, with variable numbers of lymphocytes, plasma cells, or neutrophils. A typical form of granuloma is one in which natural products of the skin (e.g., keratin, hair shaft, adnexal secretions) are introduced into the connective tissues, usually by trauma. These skin products act as foreign bodies, inciting a “foreign body granuloma,” a characteristic feature of which are multinucleated giant cells and/or epithelioid macrophages.
All forms of inflammation may be accompanied by associated lesions, including edema (though this is more commonly associated with acute inflammation), epithelial hyperplasia, hyperkeratosis, neovascularization, or hemorrhage with or without hemosiderin-containing macrophages.
Elwell MR, Stedman MA, Kovatch RM. 1990. Skin and subcutis. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman GA, Eustis SL, Elwell MR, Montgomery CA, MacKenzie WF, eds). Academic Press, San Diego, 261-277.
Abstract: https://www.ncbi.nlm.nih.gov/nlmcatalog/9002563Klein-Szanto AJP, Conti CJ. 2002. Skin and oral mucosa. In: Handbook of Toxicologic Pathology, 2nd ed (Haschek WM, Rousseaux CG, Wallig MA, eds). Academic Press, San Diego, 2:85-116.
Abstract: http://www.sciencedirect.com/science/book/9780123302151Peckham JC, Heider K. 1999. Skin and subcutis. In: Pathology of the Mouse: Reference and Atlas (Maronpot RR, Boorman GA, Gaul BW, eds). Cache River Press, Vienna, IL, 555-612.
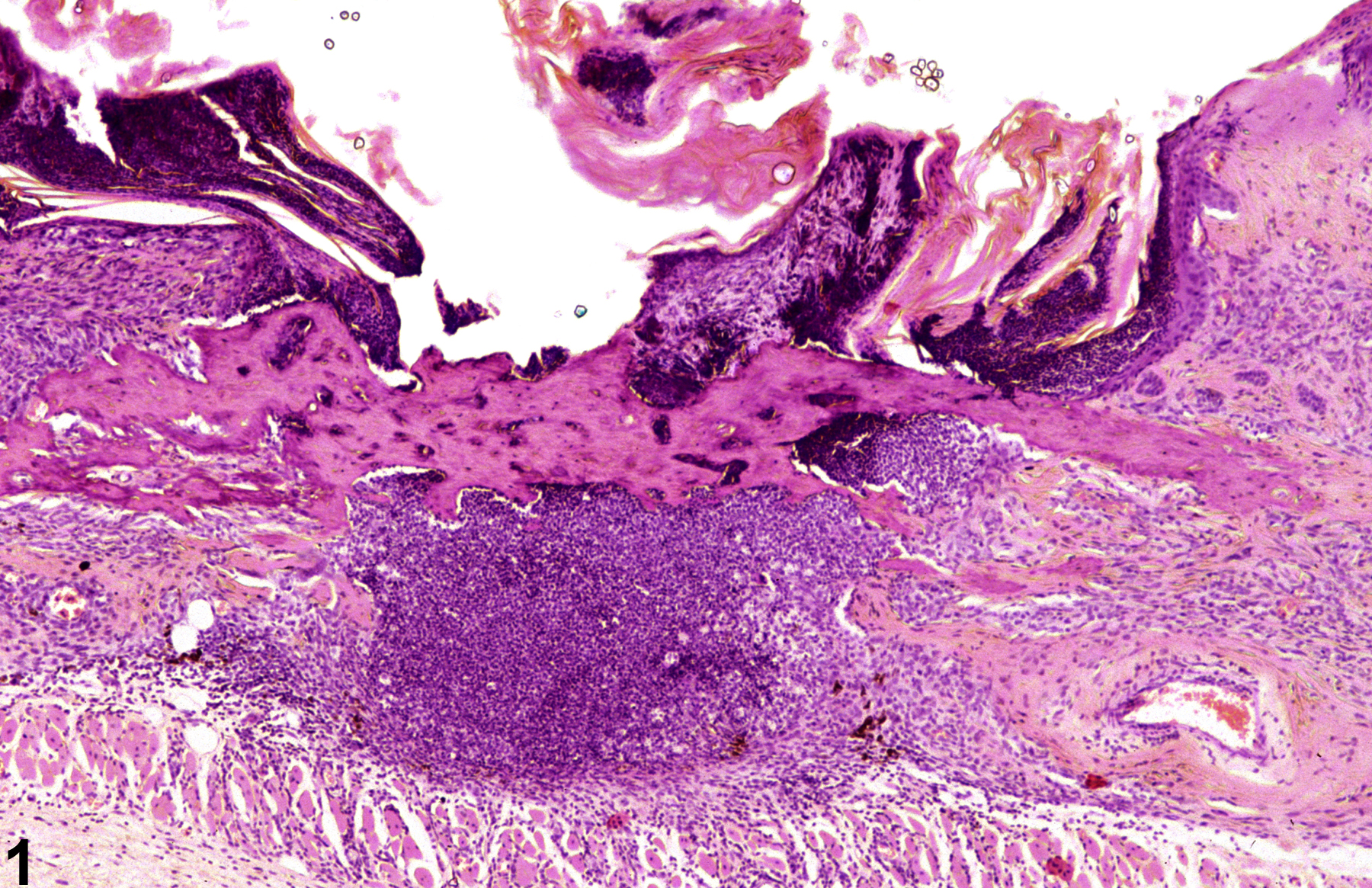
Acute inflammation-dense infiltrations of neutrophils and osseous metaplasia in a male B6C3F1 mouse from a chronic study.