Musculoskeletal System
Bone - Fibrous Osteodystrophy
Narrative
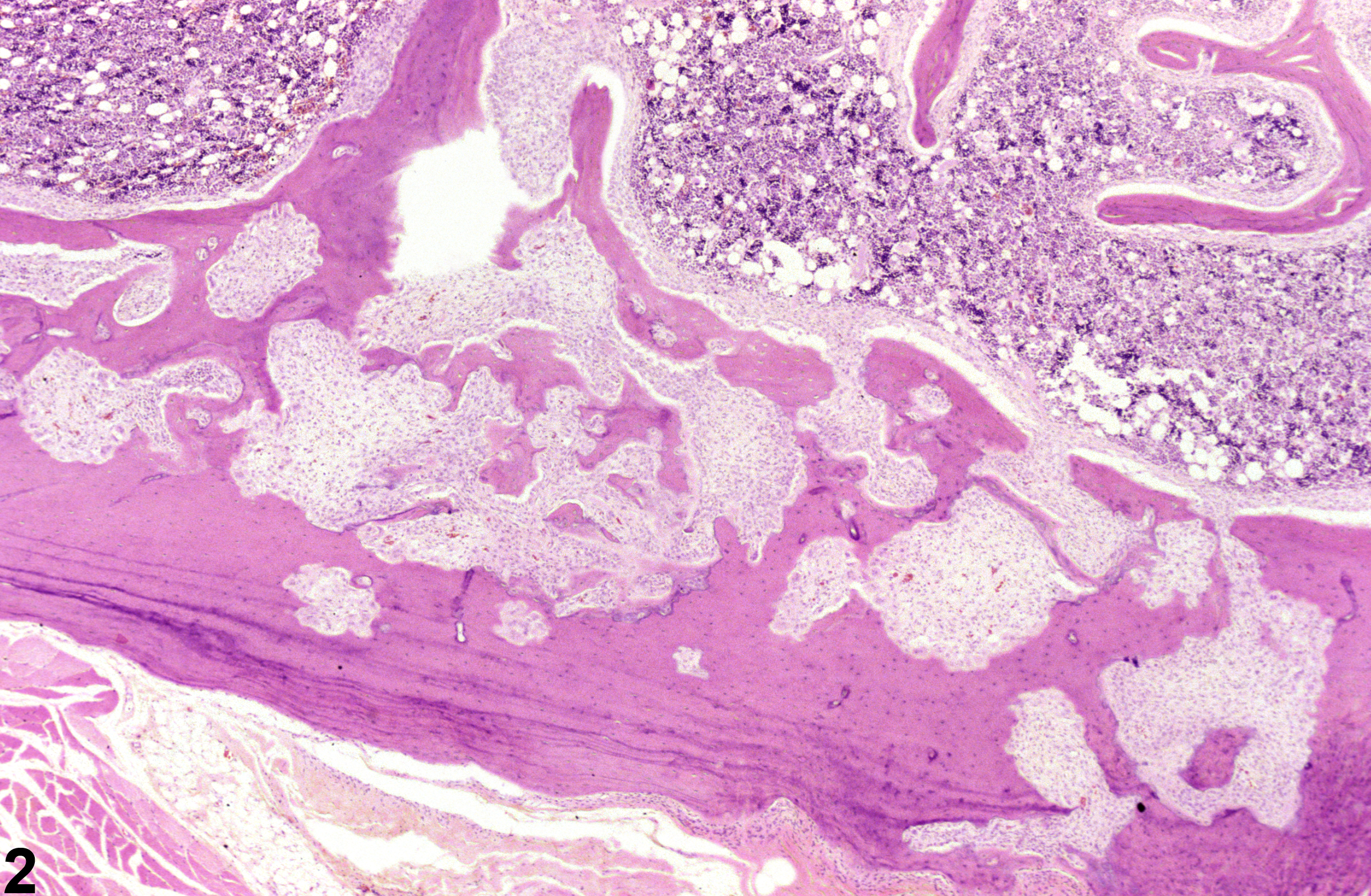
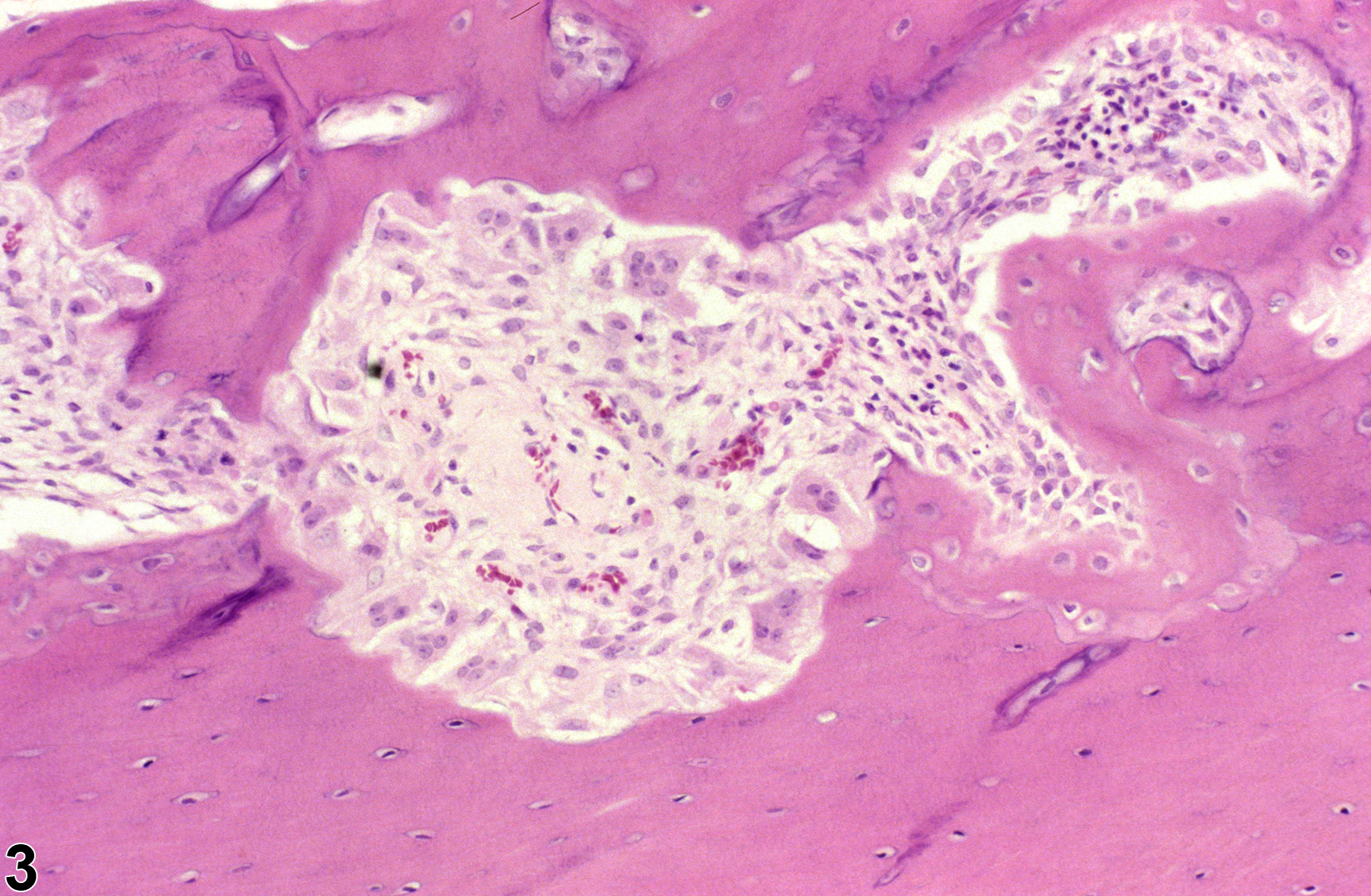
Fibrous osteodystrophy (FOD) (Figure 1, Figure 2, and Figure 3) (previously referred to as osteodysplasia, fibrous dysplasia, and osteofibrosis) is characterized by osteoclastic resorption of cancellous or cortical bone, with replacement by loose to mature fibrous connective tissue. This lesion is the result of a metabolic bone disease that occurs in conjunction with hyperparathyroidism, whether due to a functional parathyroid tumor (primary) or chronic renal disease (secondary). Primary chief cell tumors are very uncommon and usually nonfunctional in rodents, and most often, FOD occurs as a result of secondary hyperparathyroidism in conjunction with chronic progressive nephropathy. Exacerbation of chronic progressive nephropathy may result from treatment by various chemicals, leading to secondary hyperparathyroidism, FOD, and metastatic calcification of various organs, including the heart, aorta, and other soft tissues. Early FOD lesions are characterized by a moth-eaten appearance of the affected bone, with increased osteoclast numbers and "scalloping" of mature bone (Figure 3), eventually progressing to replacement by fibrous connective tissue and immature osteoid (Figure 1 and Figure 2).
The incidence of FOD is low in B6C3F1 mice (1% in females, 0% in males) due to the low incidence of chronic renal failure in this strain.
Capen CC, DeLellis RA, Yarrington JT. 2002. Endocrine system. In: Handbook of Toxicologic Pathology, Vol 2 (Haschek WM, Rousseaux C, Wallig MA, eds). Academic Press, San Diego, 719-771.
Courtney CL, Kim SN, Walsh KM, Watkins JR, Dominick MA. 1991. Proliferative bone lesions in rats given anticancer compounds. Toxicol Pathol 19:184-188.
Abstract: http://www.ncbi.nlm.nih.gov/pubmed/1837612Leininger JR, Riley MGI. 1990. Bones, joints, and synovia. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman G, Eustis SL, Elwell MR, Montgomery CA, MacKenzie WF, eds). Academic Press, San Diego, 209-226.
Long PH, Leininger JR. 1999. Bones, joints, and synovia. In: Pathology of the Mouse (Maronpot R, Boorman G, Gaul BW, eds). Cache River Press, St Louis, 645-678.
Rosol TJ, Capen CC. 1989. Tumors of the parathyroid gland and circulating parathyroid hormone-related protein associated with persistent hypercalcemia. Toxicol Pathol 17:346-356.
Abstract: http://www.ncbi.nlm.nih.gov/pubmed/2675285Travlos G. 2006. Histopathology of bone marrow. Toxicol Pathol 34:566-598.
Abstract: http://www.ncbi.nlm.nih.gov/pubmed/17067944Yamasaki K. 1993. Morphological studies on the bone and cartilage of laboratory animals. Exp Anim 42:11-21.
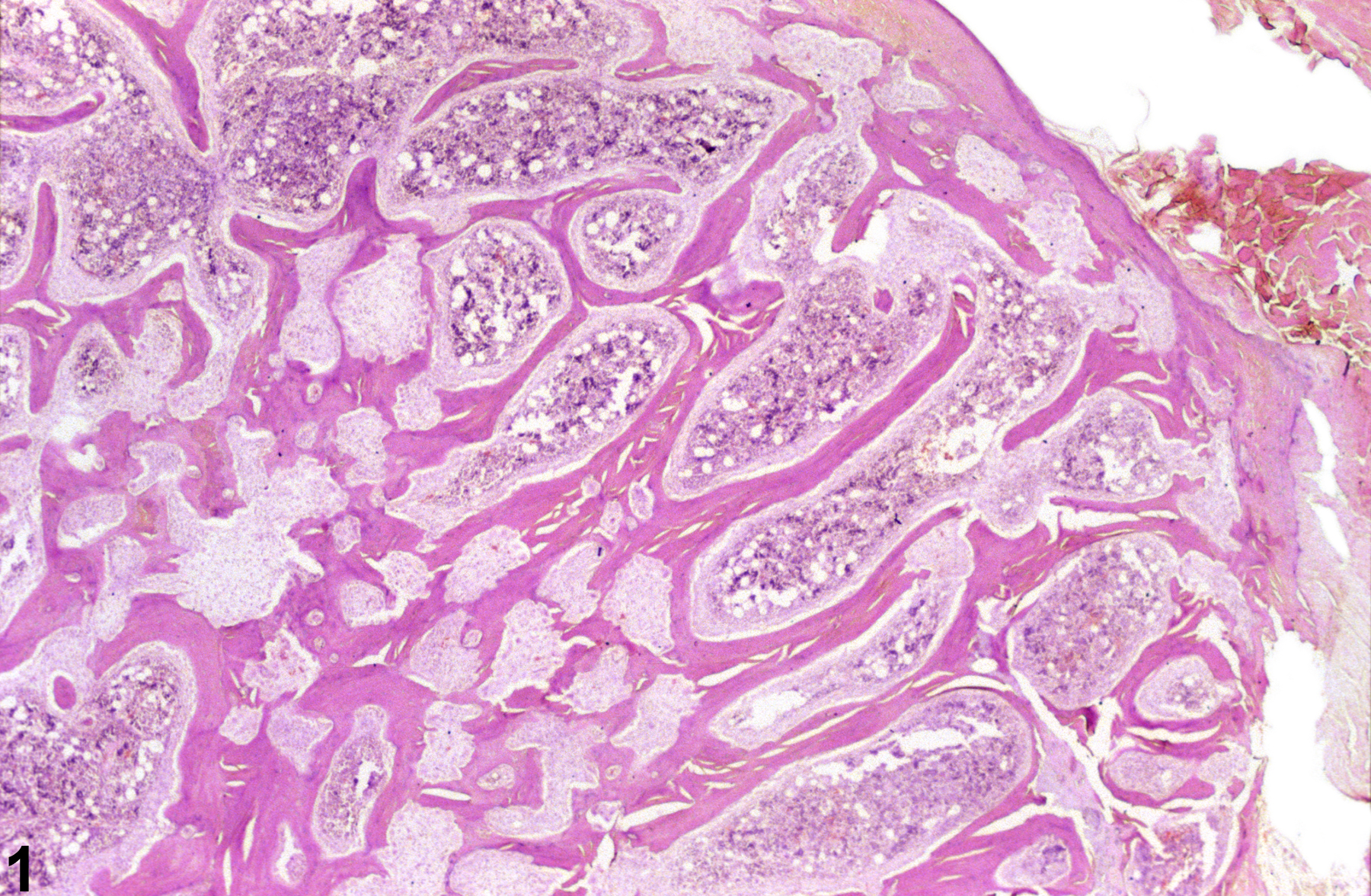
Bone - Fibrous osteodystrophy in a male F344/N rat from a chronic study. There is replacement of bone by fibrous connective tissue.