Musculoskeletal System
Bone, Joint - Degeneration
Narrative
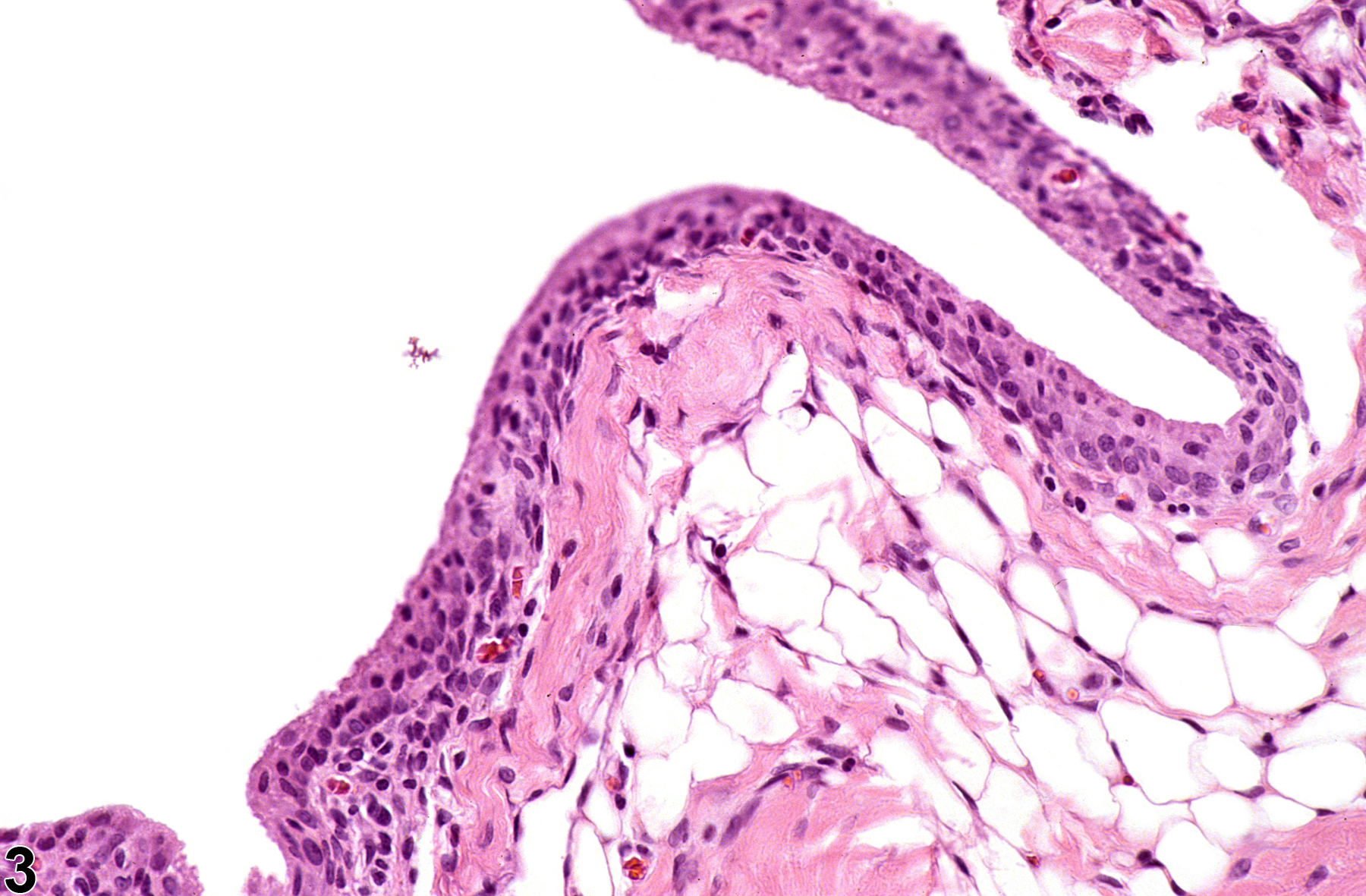
Degenerative joint disease occurs in nearly all strains of rats and mice as a component of the aging process. In the B6C3F1 mouse, the disease occurs more commonly in males than females and has an incidence in the stifle joint of up to 2% for males and 4% for females. The disease is known to preferentially affect the stifle and elbow joints in the mouse but also occurs in the distal thoracic vertebrae and joints of the sternum. In the F344 rat, spontaneous lesions have been reported as early as 13 months. Although a normal age-related change, the disease is multifactorial and influenced by diet, strain, sex hormones, and weight, in addition to exposure to various toxicants, which can cause alterations in the cartilaginous matrix. Chondromucinous/cystic degeneration (aseptic necrosis) of articular cartilage or growth plates in the rat should not be confused with degenerative joint disease. This is a common spontaneous lesion in aged rats that may lead to spontaneous fractures of bony trabeculae of the physis and epiphysis but does not cause degenerative lesions of the articular cartilage.
Leininger JR, Riley MGI. 1990. Bones, joints, and synovia. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman G, Eustis SL, Elwell MR, Montgomery CA, MacKenzie WF, eds). Academic Press, San Diego, 209-226.
Long PH, Leininger JR. 1999. Bones, joints, and synovia. In: Pathology of the Mouse (Maronpot R, Boorman G, Gaul BW, eds). Cache River Press, St Louis, 645-678.
Schunke M, Tillmann B, Bruck M, Muller-Ruchholtz W. 1988. Morphologic characteristics of developing osteoarthritic lesions in the knee cartilage of STR/IN mice. Arthritis Rheum 31:898-905.
Abstract: http://www.ncbi.nlm.nih.gov/pubmed/3395383Sheldon WG, Bucci TJ, Turturro A. 1996. Thoracic apophyseal osteoarthiritis in feed-restricted and ad libitum-fed B6C3F1 mice. In: Pathobiology of the Aging Mouse, Vol 2 (Mohr U, Dungworth DL, Capen CC, Carlton WW, Sundberg JP, Ward JM, eds). ILSI Press, Washington, DC, 445-453.
Silberberg M, Silberberg R. 1970. Age-linked modification of the effect of estrogen on joints and cortical bone of female mice. Gerontologica 16:201-211.
Sokoloff L. 1956. Natural history of degenerative joint disease in small laboratory animals. 1. Pathologic anatomy of degenerative joint disease in mice. AMA Arch Pathol 62:118-128.
Stanescu R, Knyszynski A, Muriel M, Stanescu V. 1993. Early lesions of the articular surface in a strain of mice with very high incidence of spontaneous osteoarthritic-like lesions. J Rheumatol 20:102-110.
Abstract: http://www.ncbi.nlm.nih.gov/pubmed/8441138Yamamoto H, Iwase N, Kohno M. 1999. Histopathological characterization of spontaneously developing osteoarthropathy in the BCBC/Y mouse established newly from B6C3F1 mice. Exp Toxicol Pathol 51:15-20
Abstract: http://www.ncbi.nlm.nih.gov/pubmed/10048708Yamamoto K, Shishido T, Masaoka T, Imakiire A. 2005. Morphological studies on the ageing and osteoarthritis of the articular cartilage in C57 black mice. J Orthop Surg (Hong Kong) 13:8-18.
Abstract: http://www.ncbi.nlm.nih.gov/pubmed/15872395Yamasaki K. 1993. Morphological studies on the bone and cartilage of laboratory animals. Exp Anim 42:11-21.
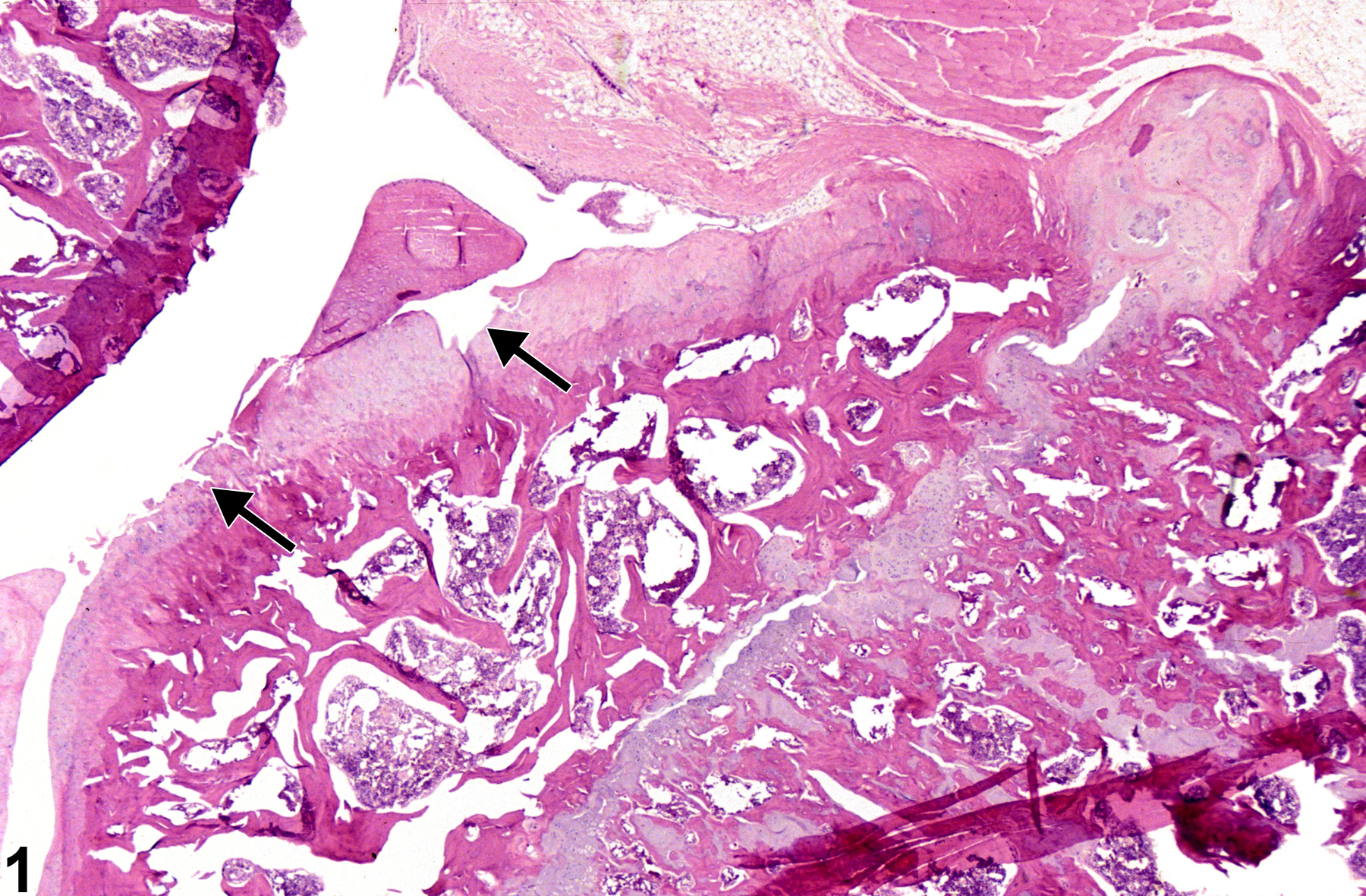
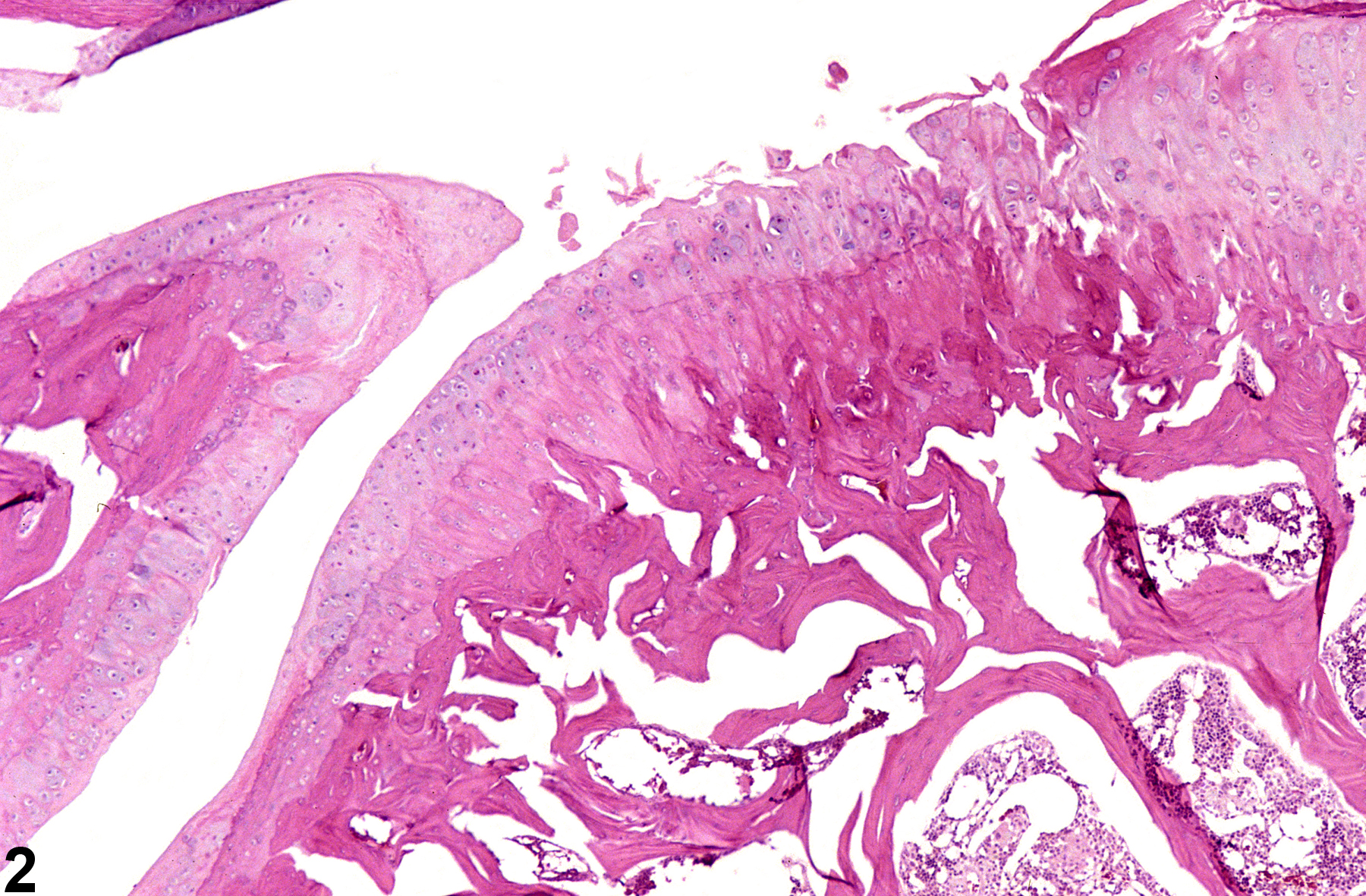
Bone, Joint - Degeneration in a female F344/N rat from a chronic study. The articular surface of the femorotibial joint is roughened and contains clefts (arrow).