Nervous System
Brain - Hydrocephalus
Narrative
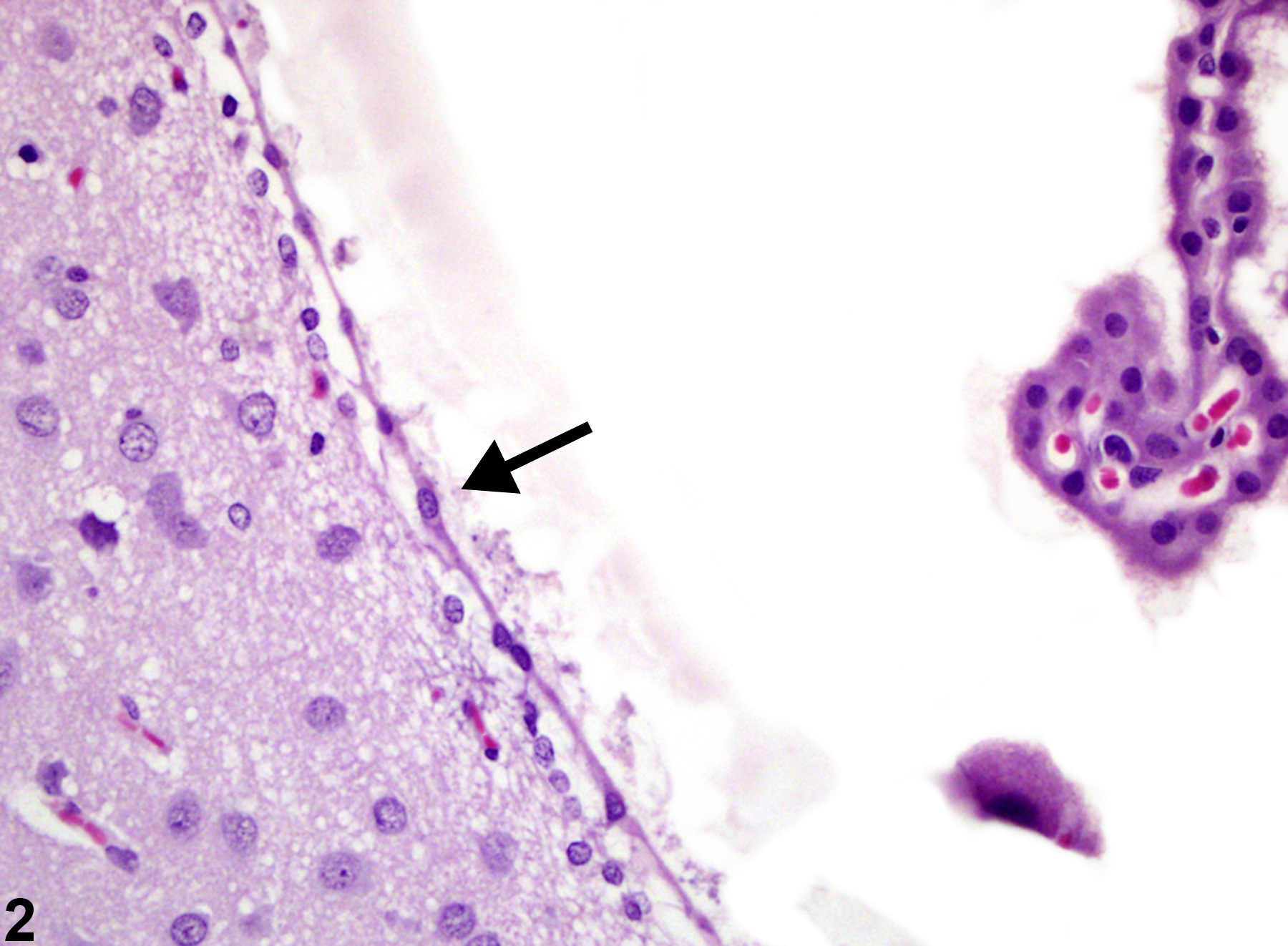
Ependymal cells have been generally considered by pathologists to be poorly responsive to insults, simply undergoing degeneration and necrosis. However, in investigations of controlled spinal injury of rats, ependymal cells and closely associated subjacent cells appear to be quite responsive, at least to trauma. Nestin and GAP-43, immunohistochemical indicators of immature neural stem cells, and glial fibrillary acid protein were detected posttrauma in in vivo cells identified as ependymal, suggesting dedifferentiation of ependymal cells to neural stem cells and glia and their potential role in spinal injury repair.
Takahashi M, Arai Y, Kurosawa H, Sueyoshi N, Shirai S. 2003. Ependymal cell reactions in spinal cord segments after compression injury in adult rat. J Neuropathol Exp Neurol 62:185-194.
Abstract: http://www.ncbi.nlm.nih.gov/pubmed/12578228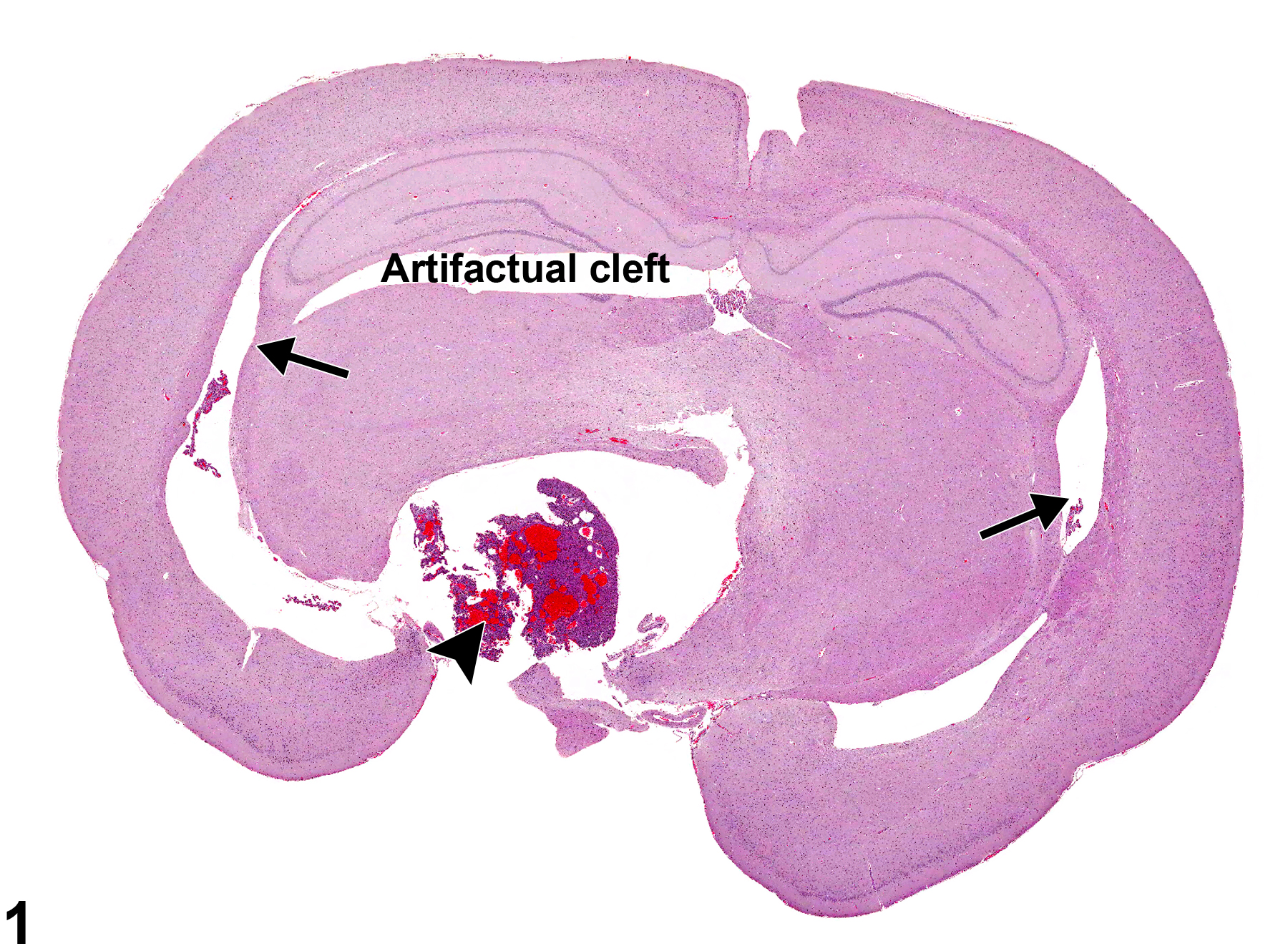
An example of bilateral noncommunicating, obstructive hydrocephalus of the lateral ventricles (arrows) in a male F344/N rat from a chronic study. It is secondary to a pituitary neoplasm (arrowhead) compressing and distorting the diencephalon while obstructing the ventral aspect of the third ventricle.
All Images

An example of bilateral noncommunicating, obstructive hydrocephalus of the lateral ventricles (arrows) in a male F344/N rat from a chronic study. It is secondary to a pituitary neoplasm (arrowhead) compressing and distorting the diencephalon while obstructing the ventral aspect of the third ventricle.