Respiratory System
Lung - Inflammation
Narrative
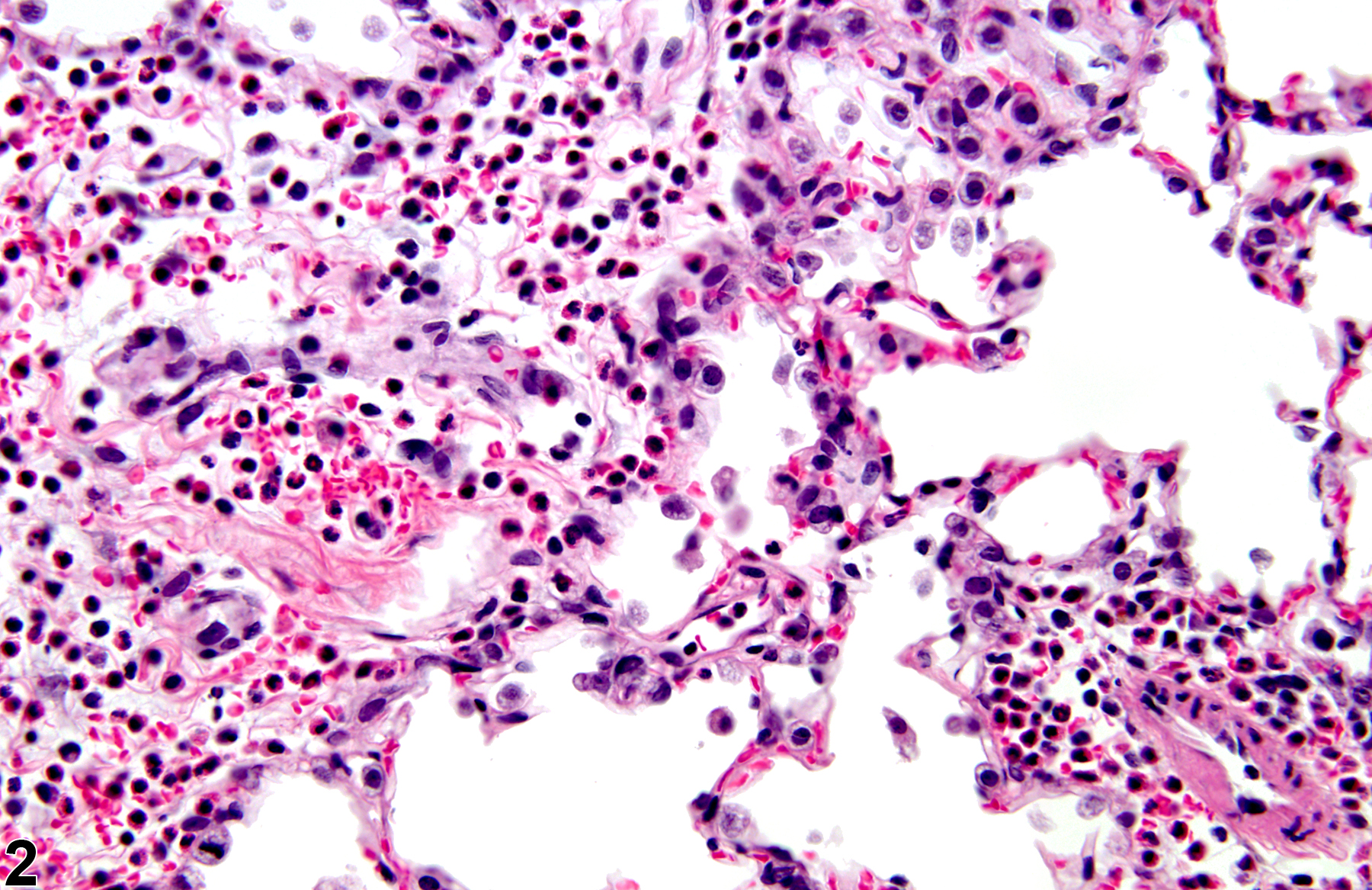
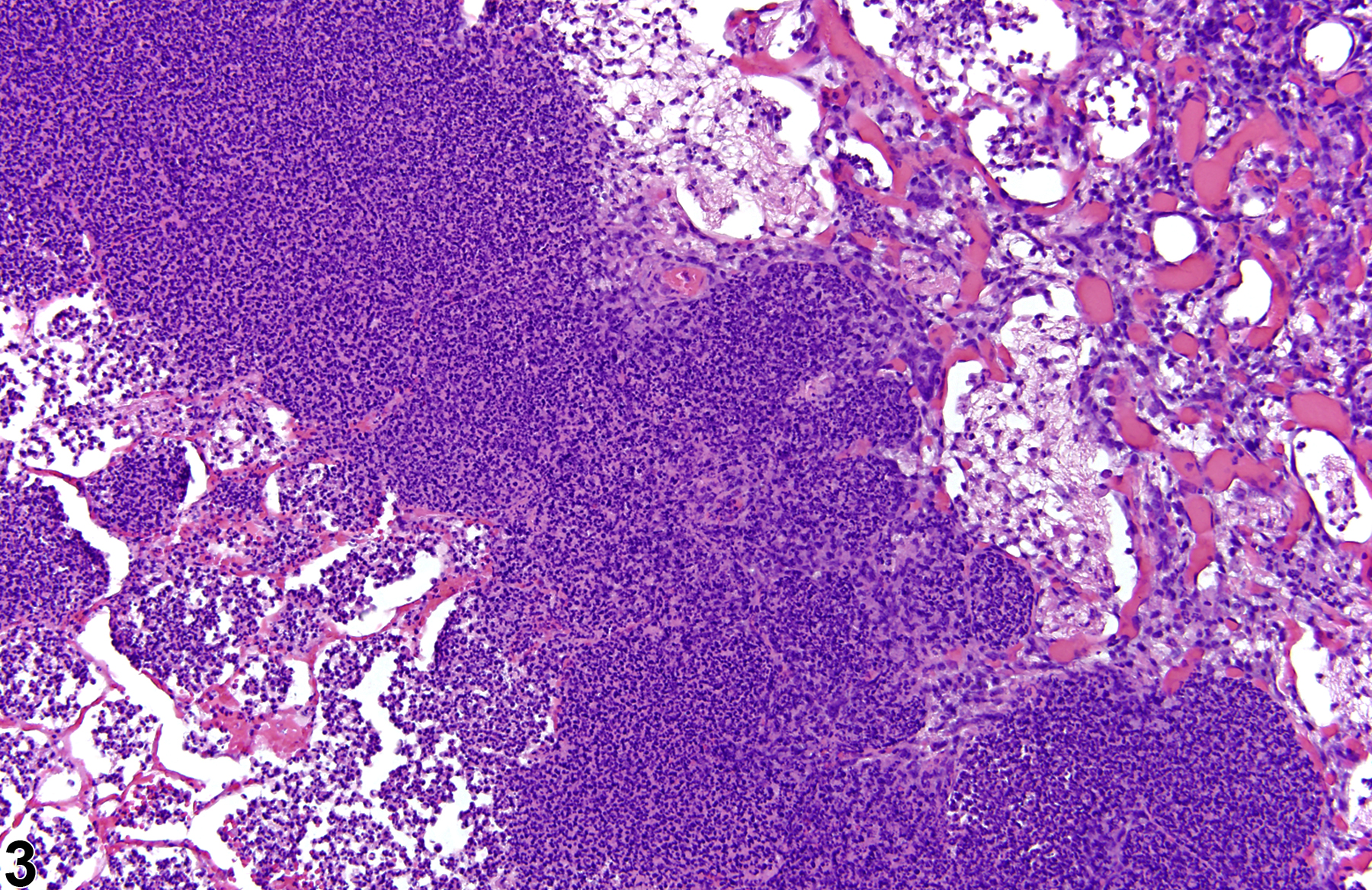
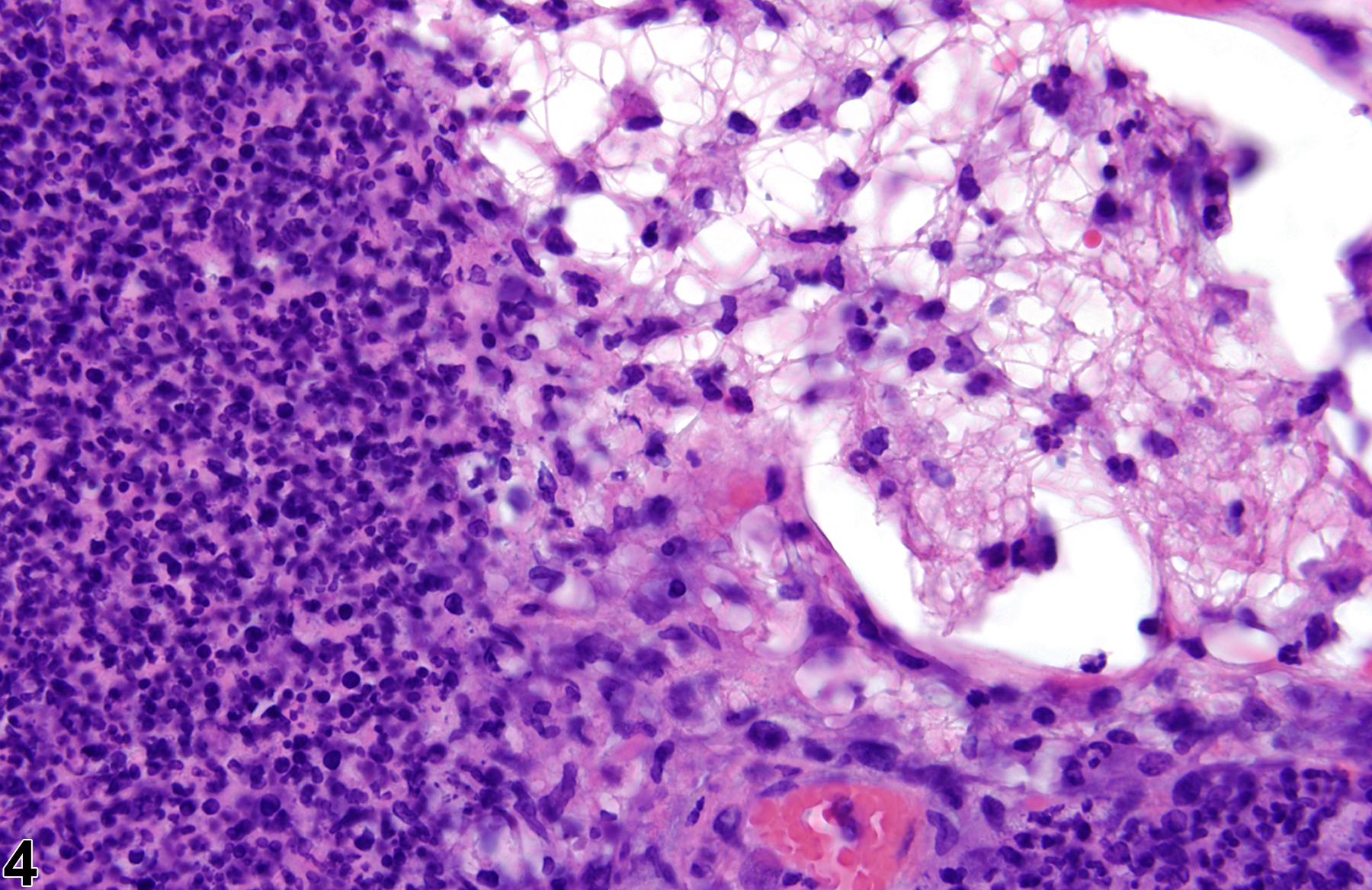
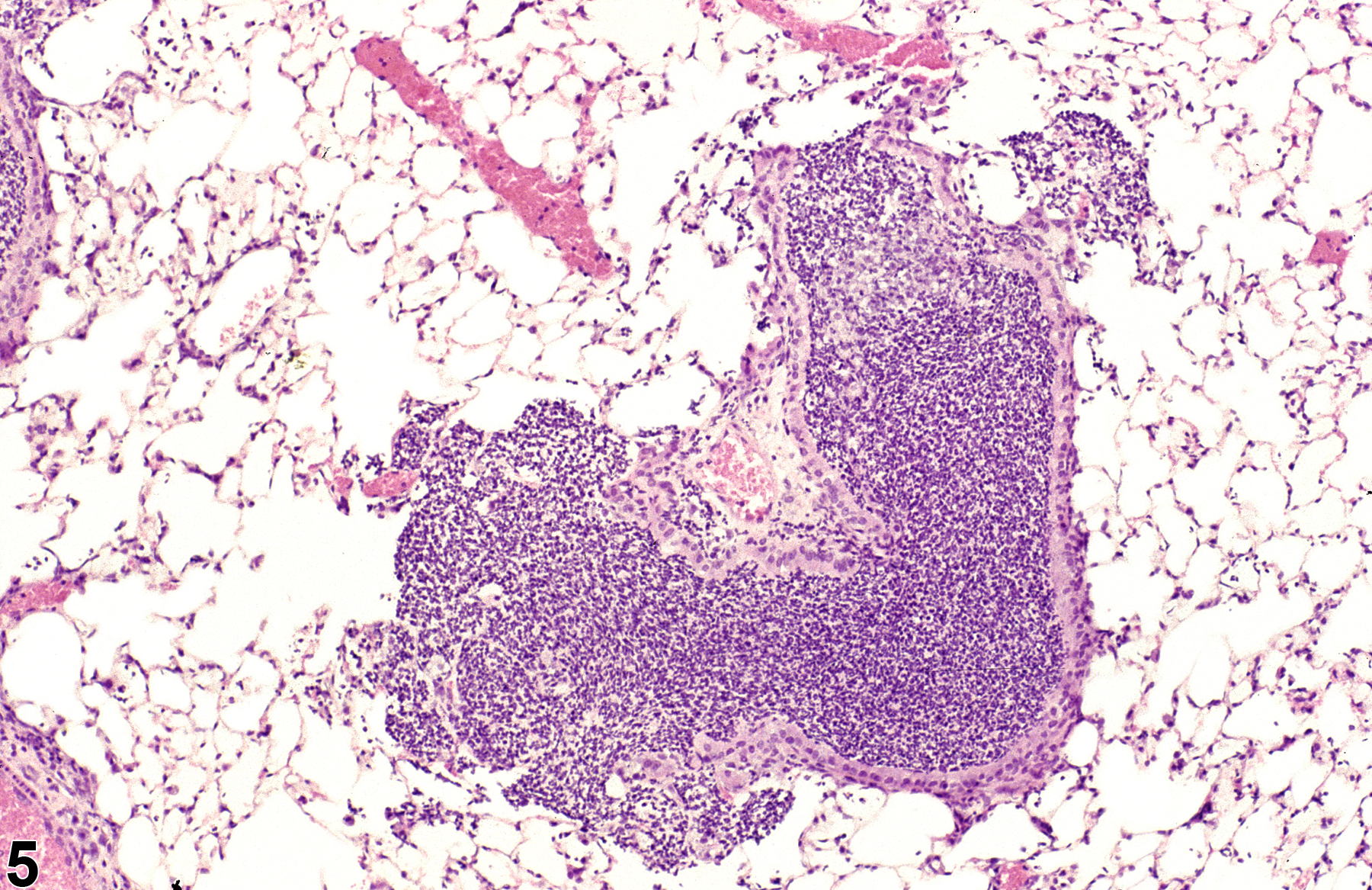
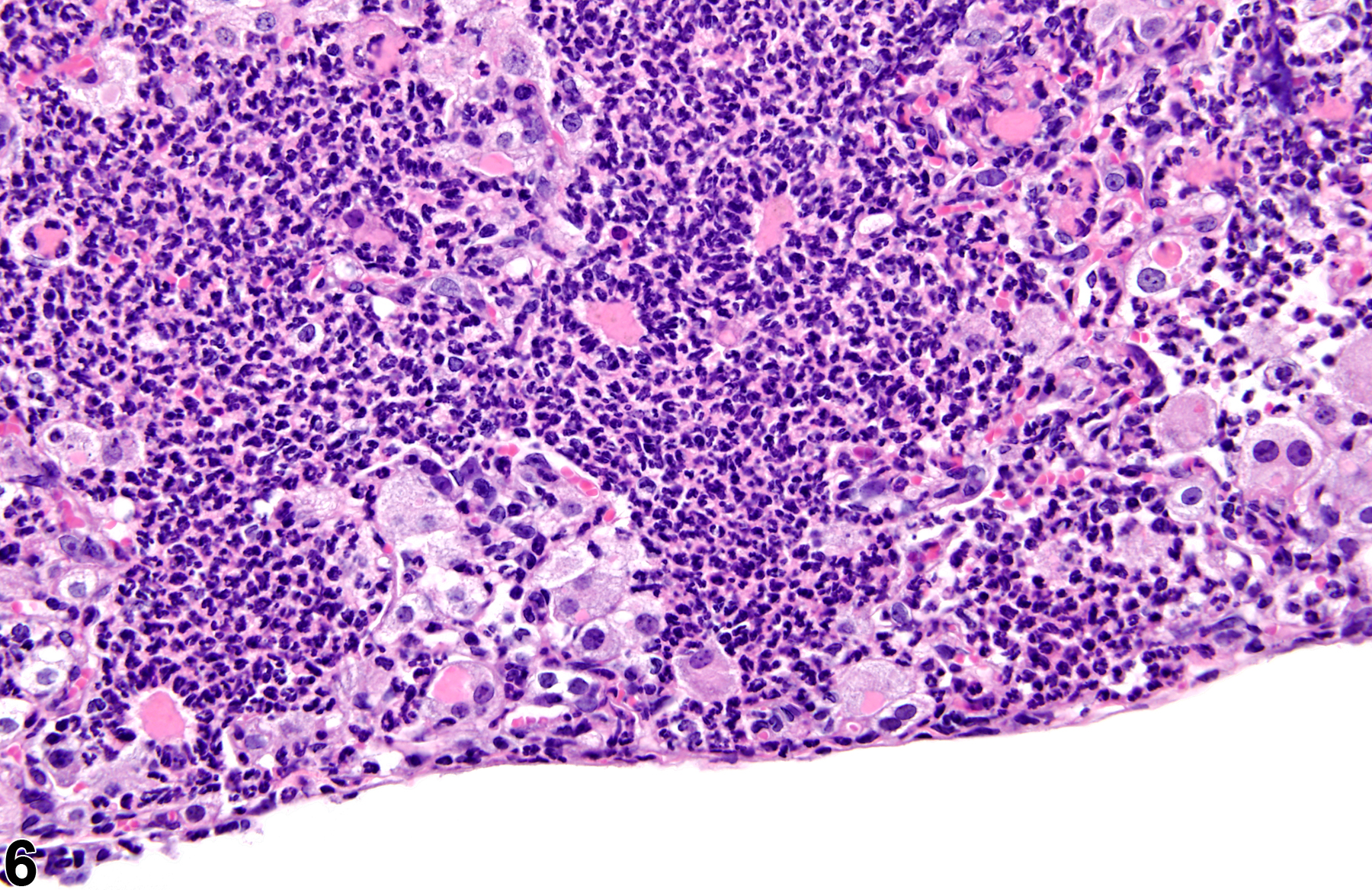
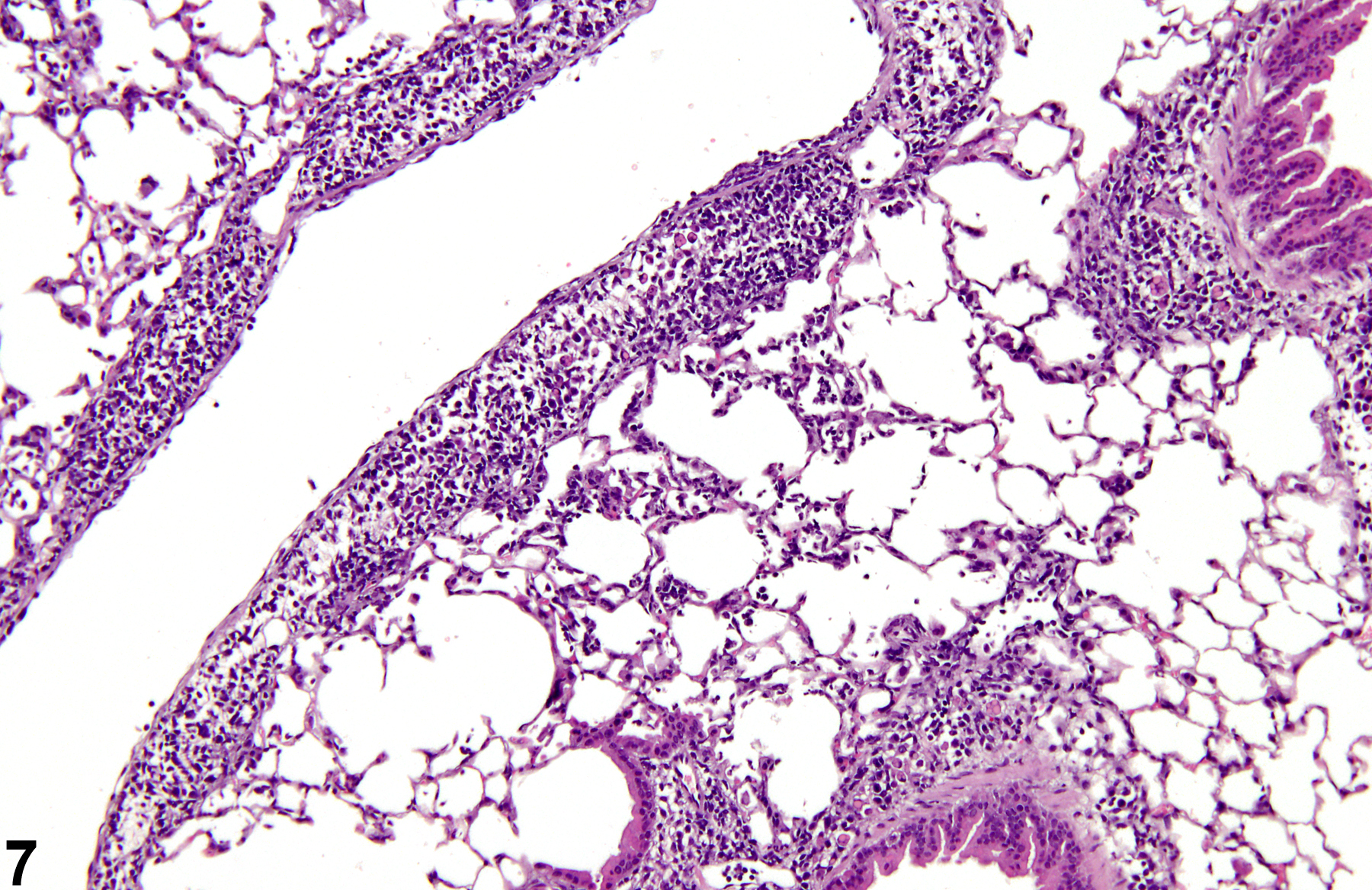
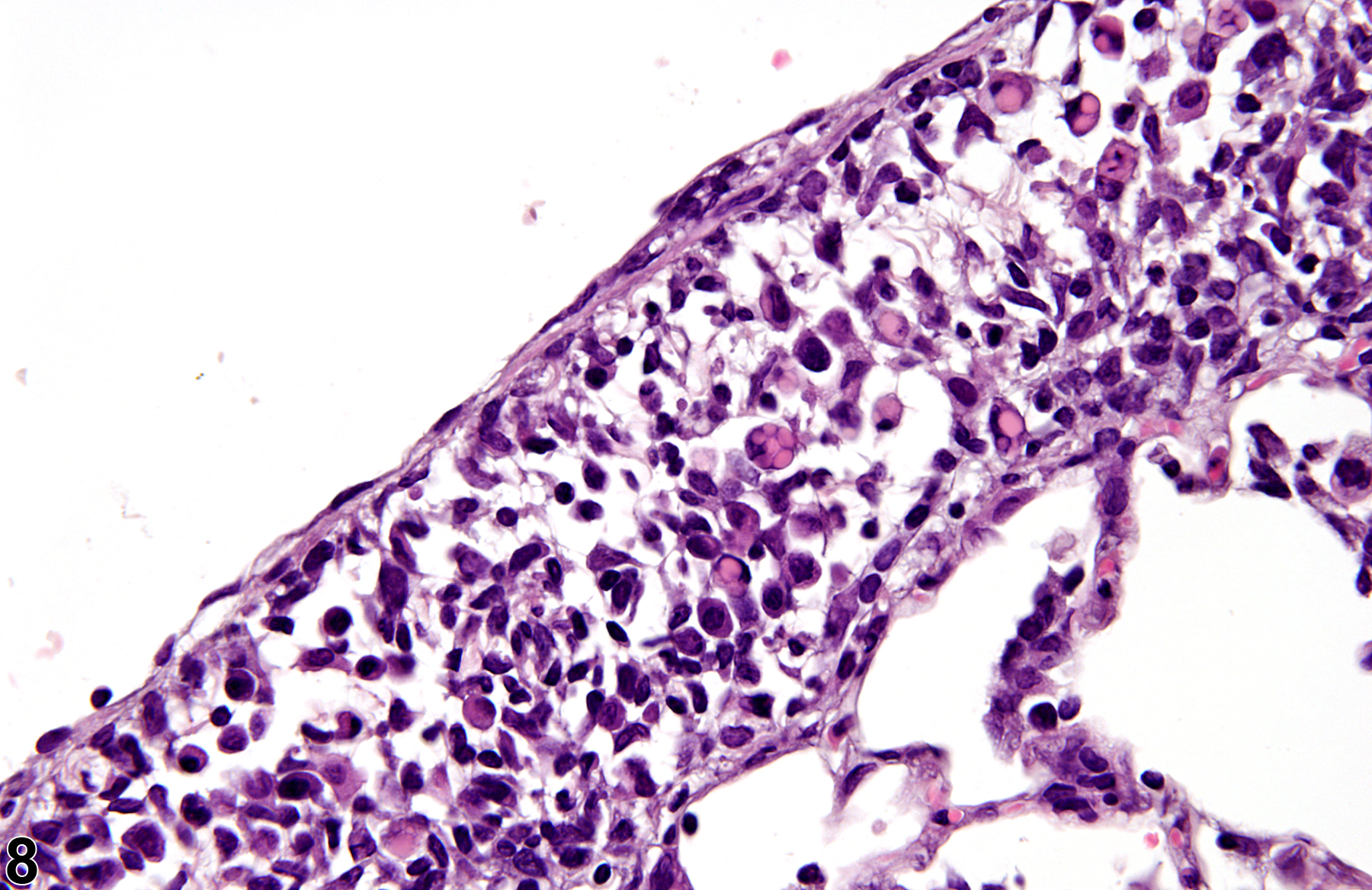
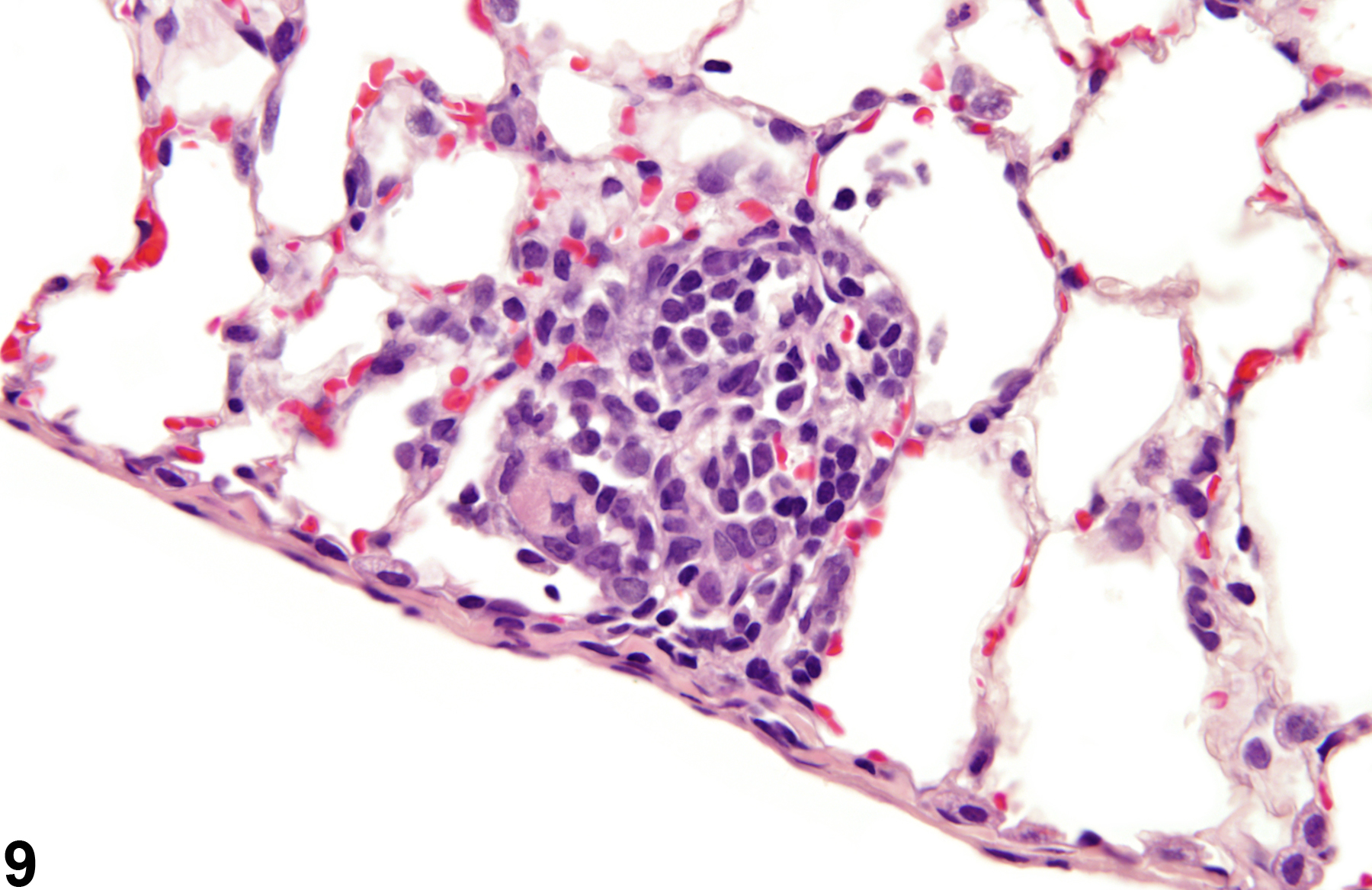
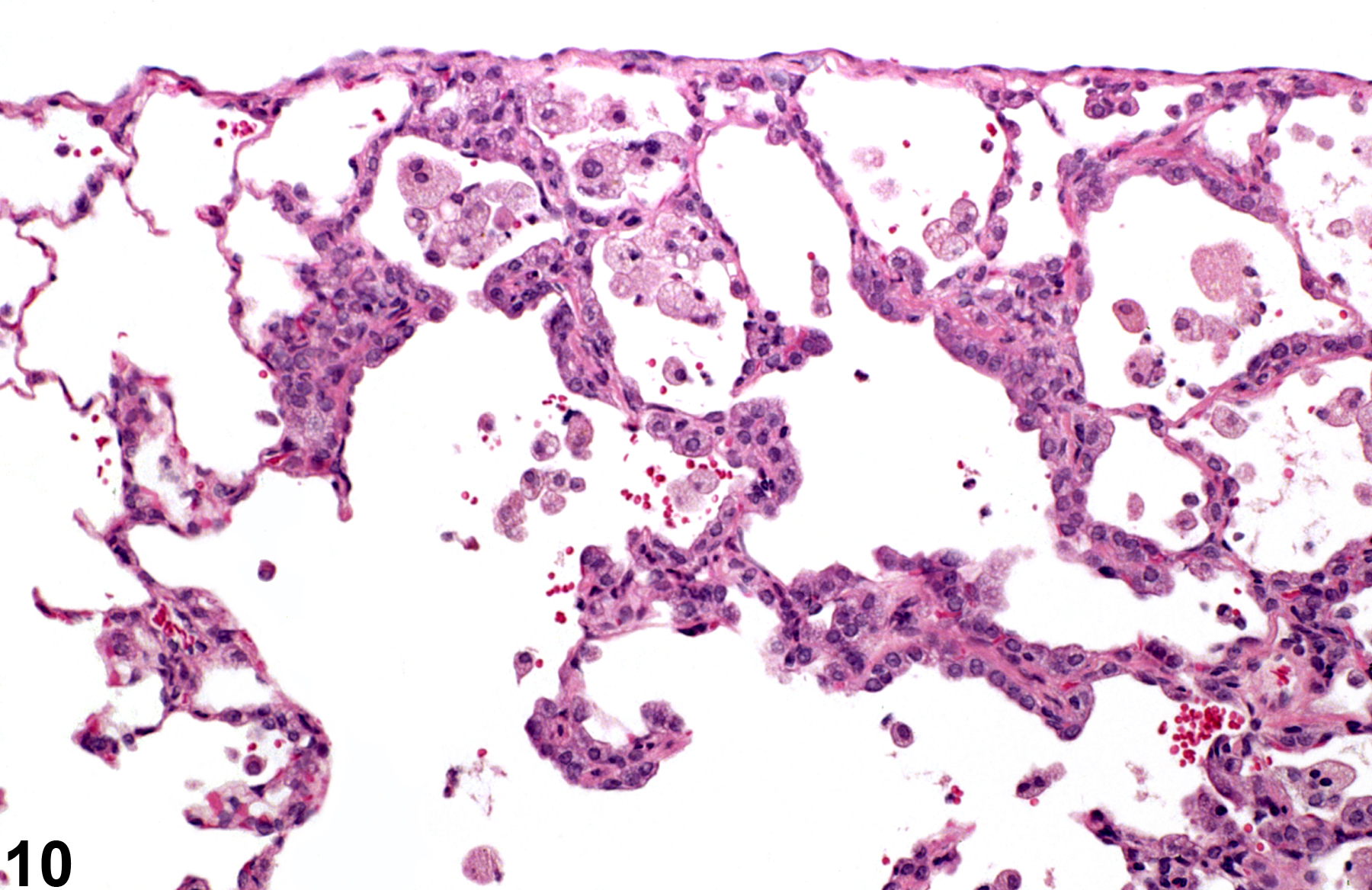
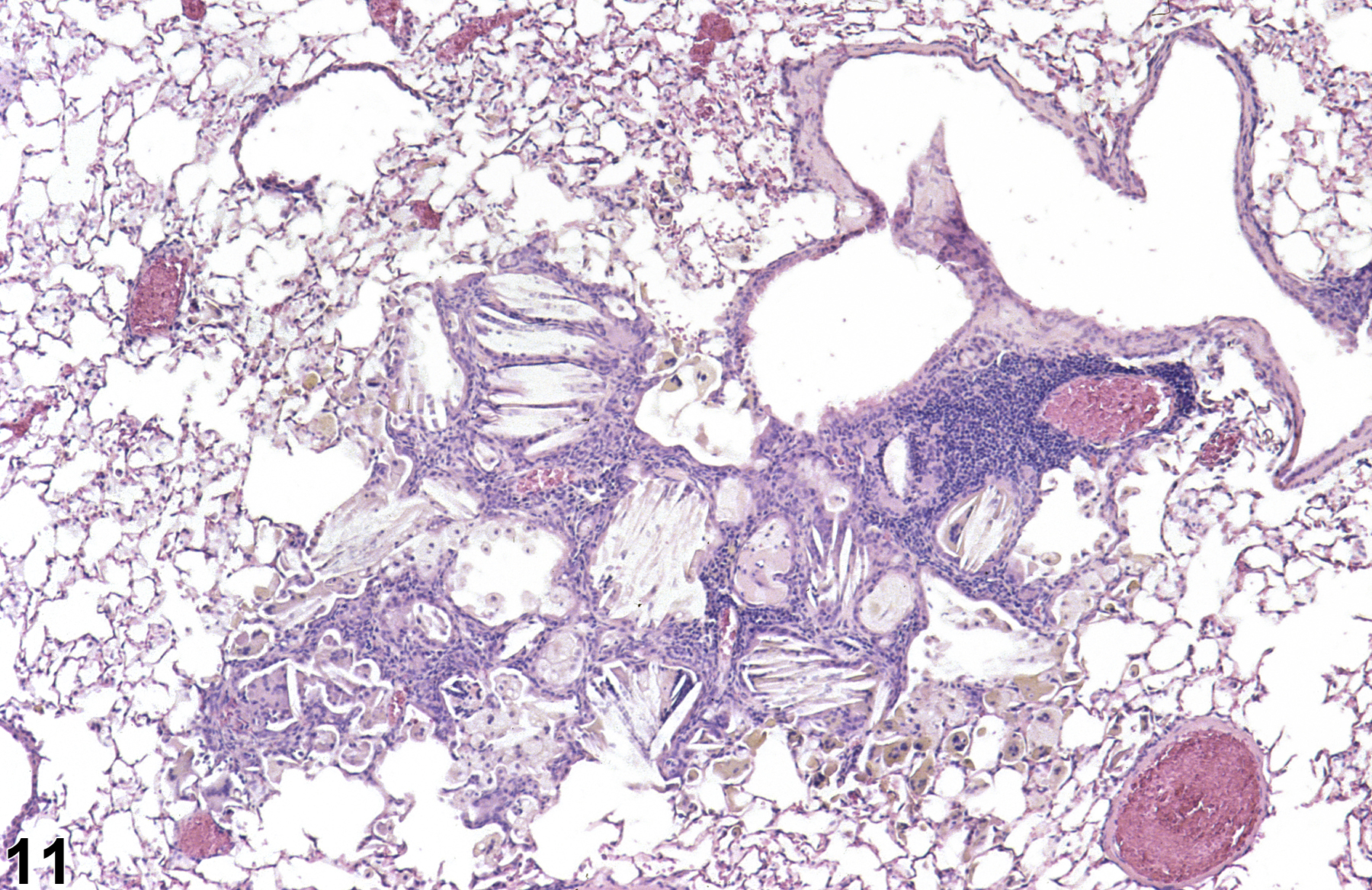
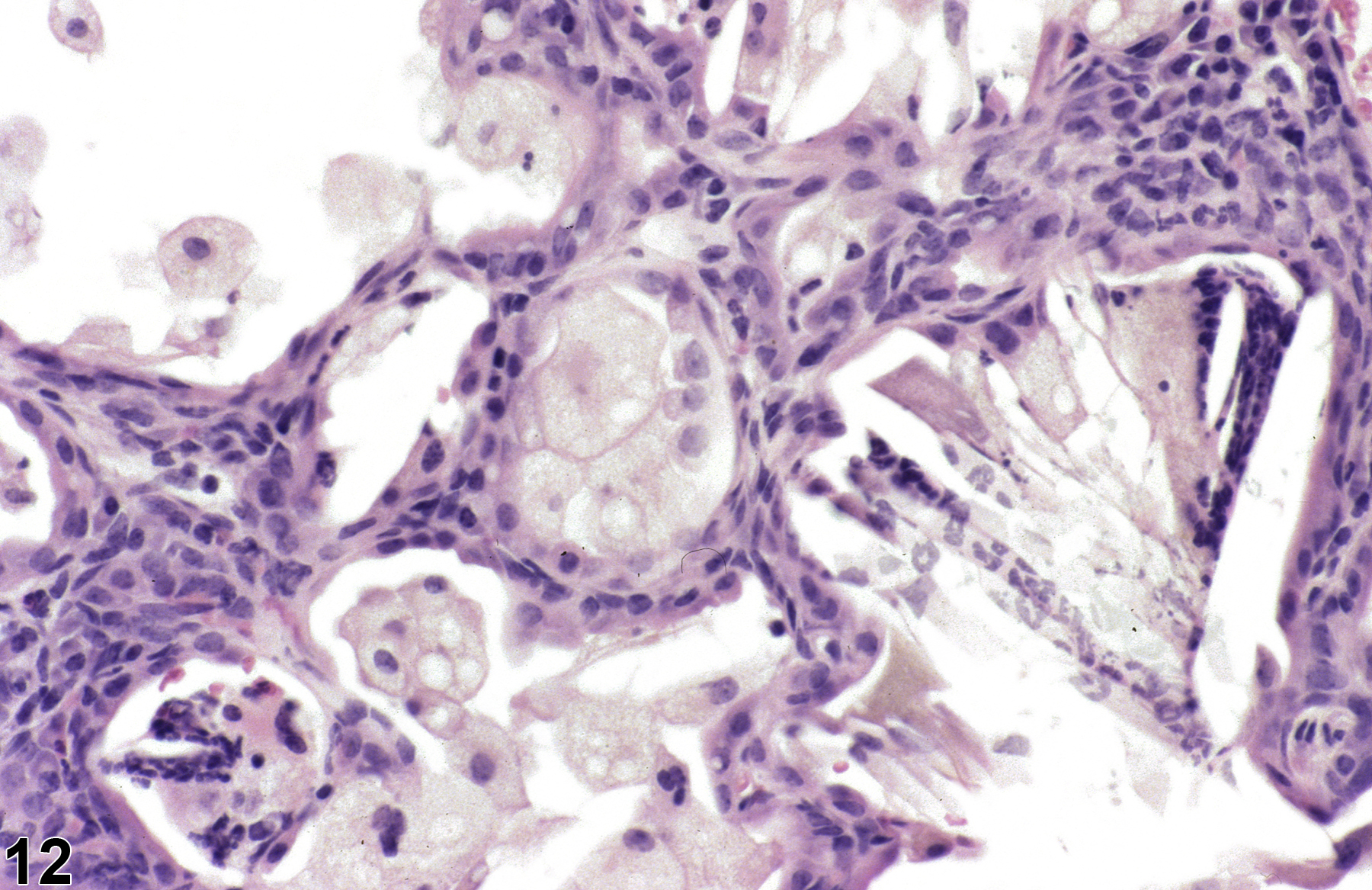
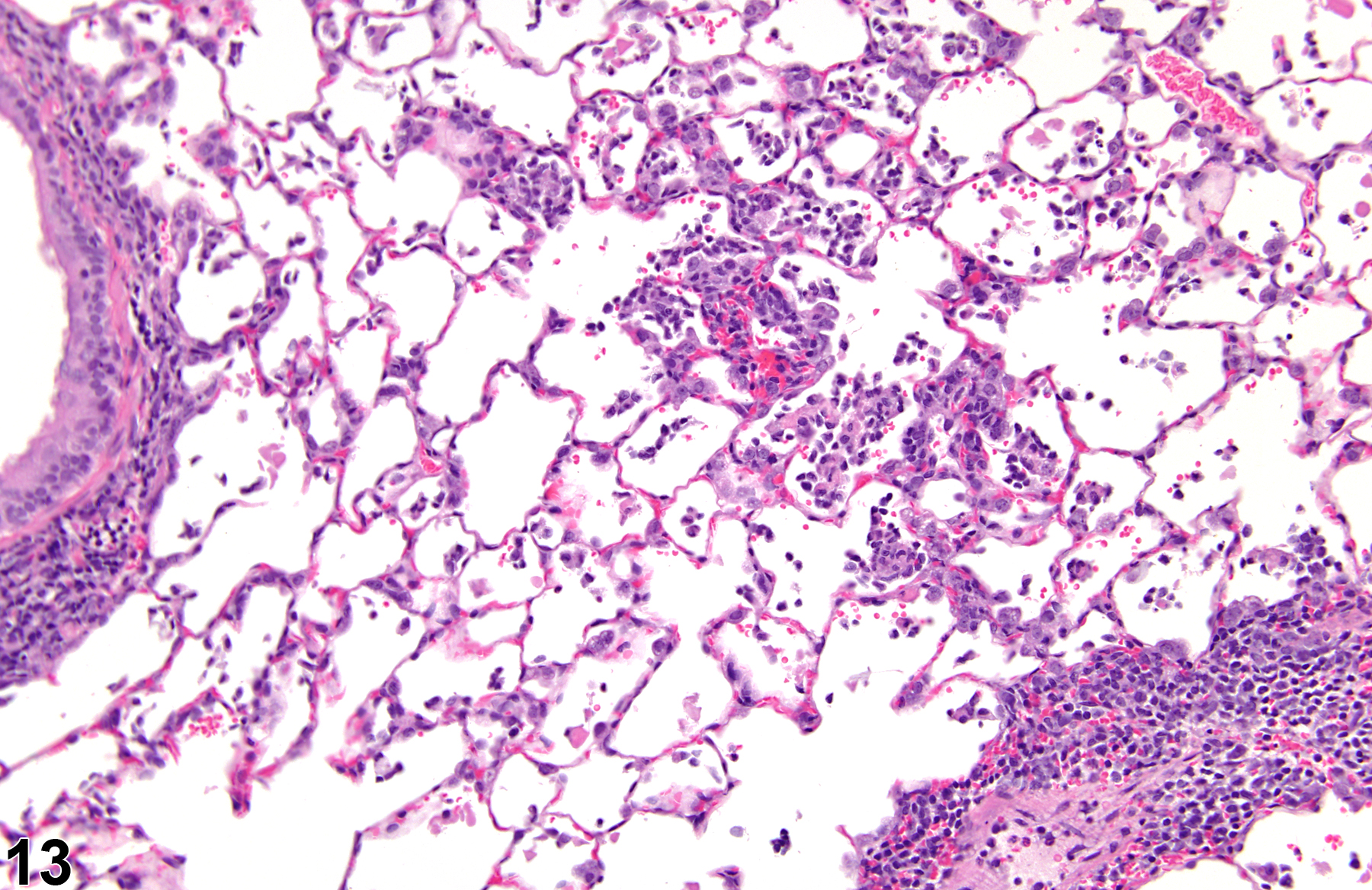
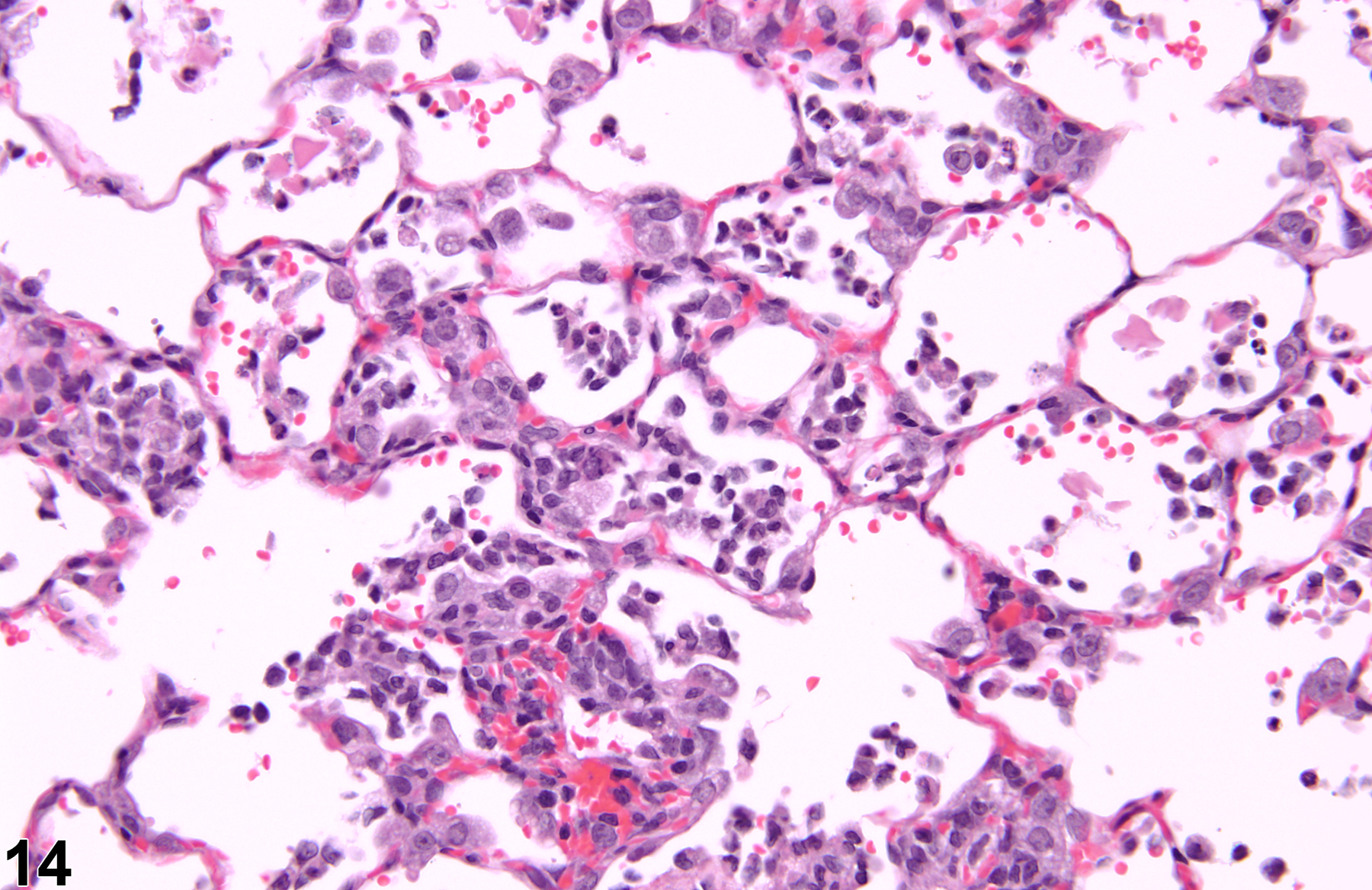
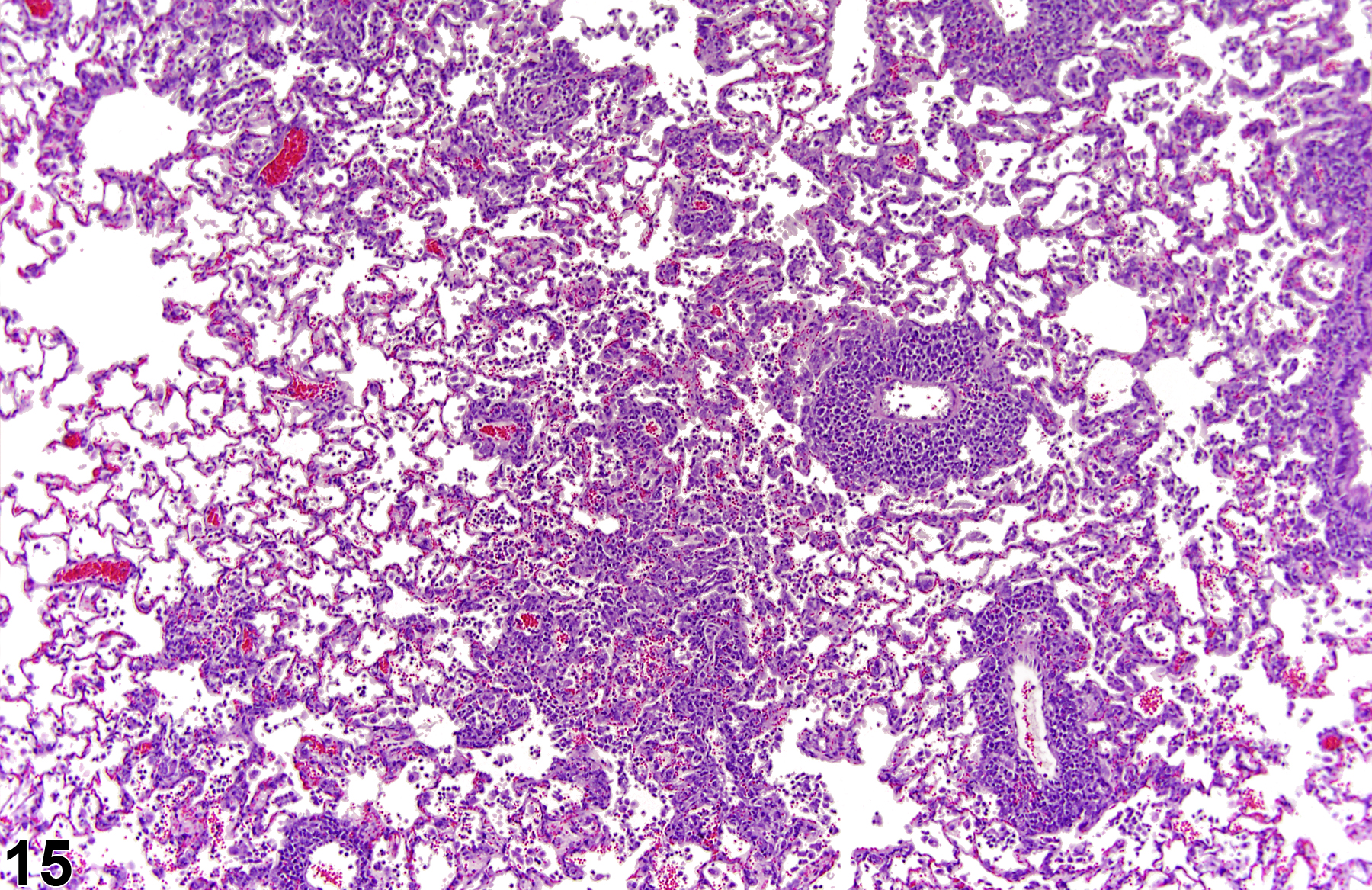
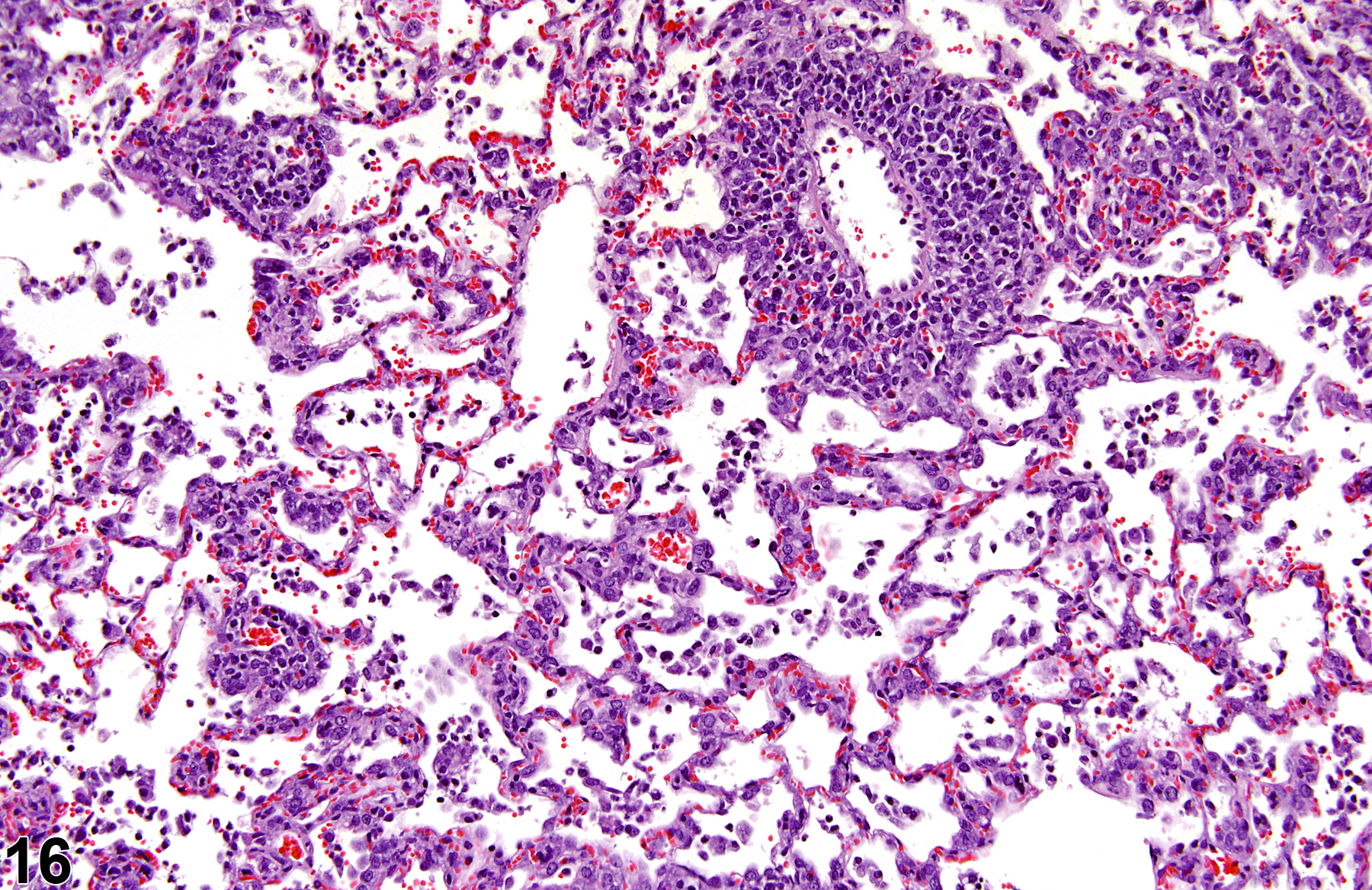
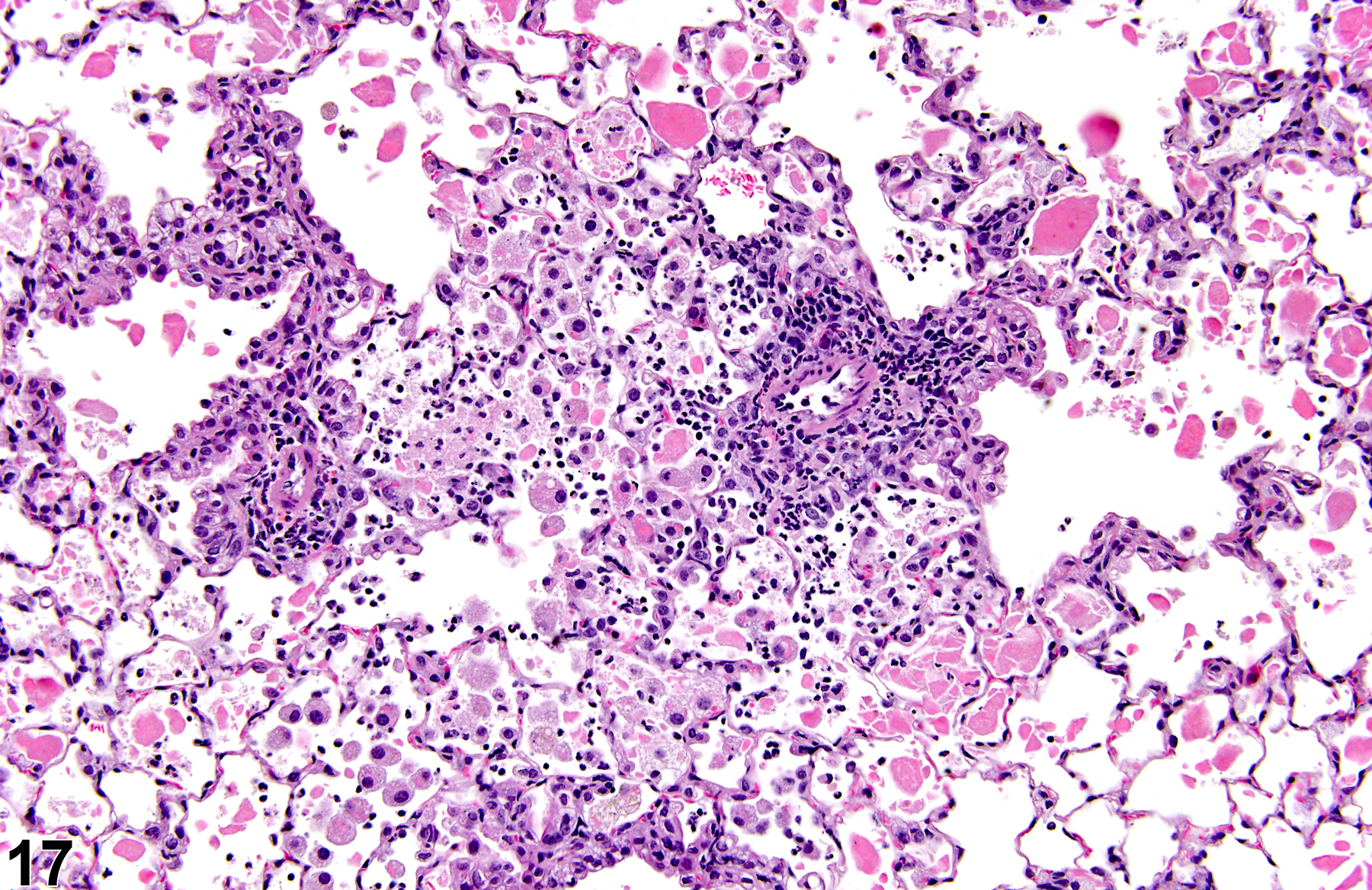
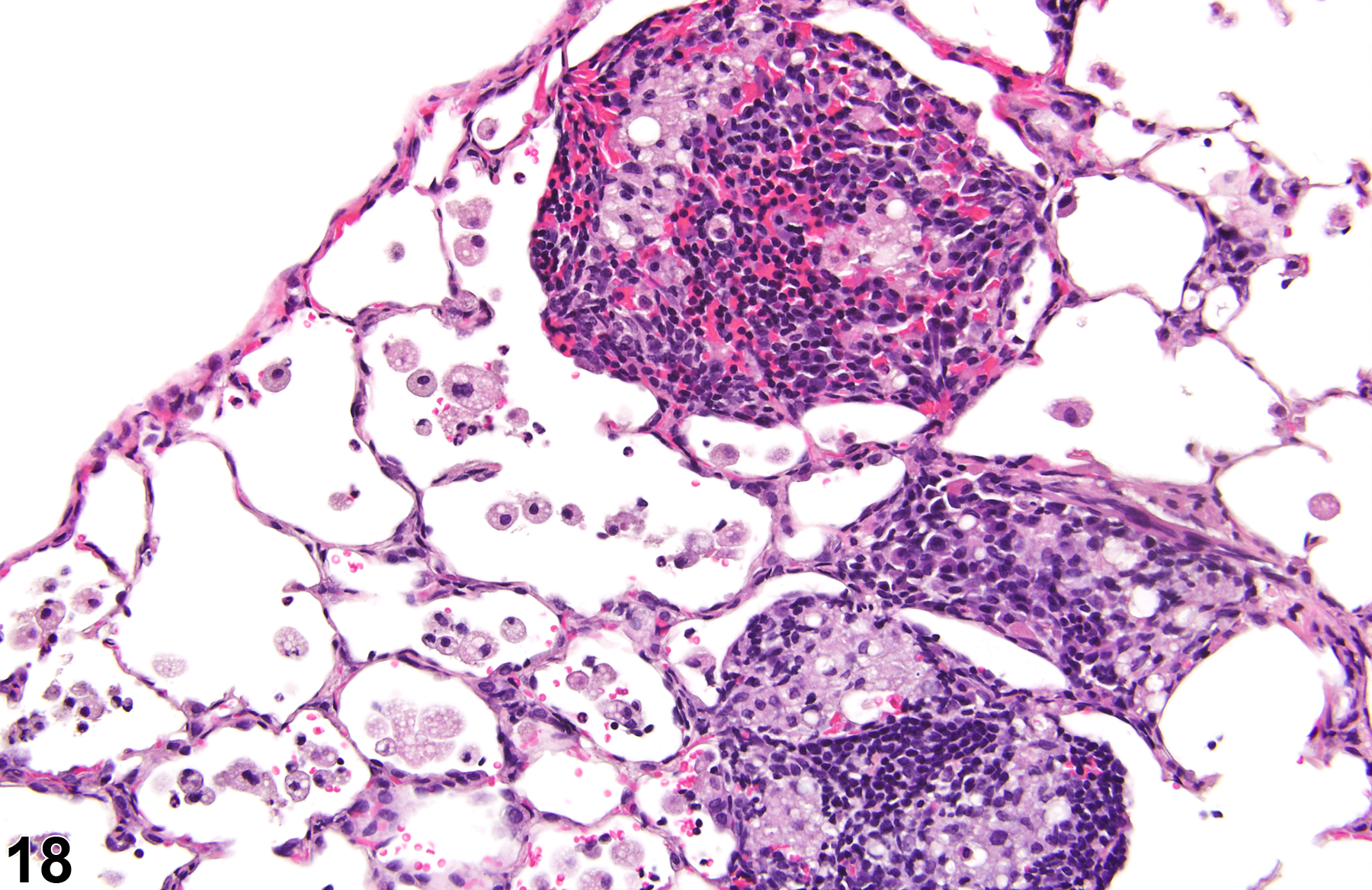
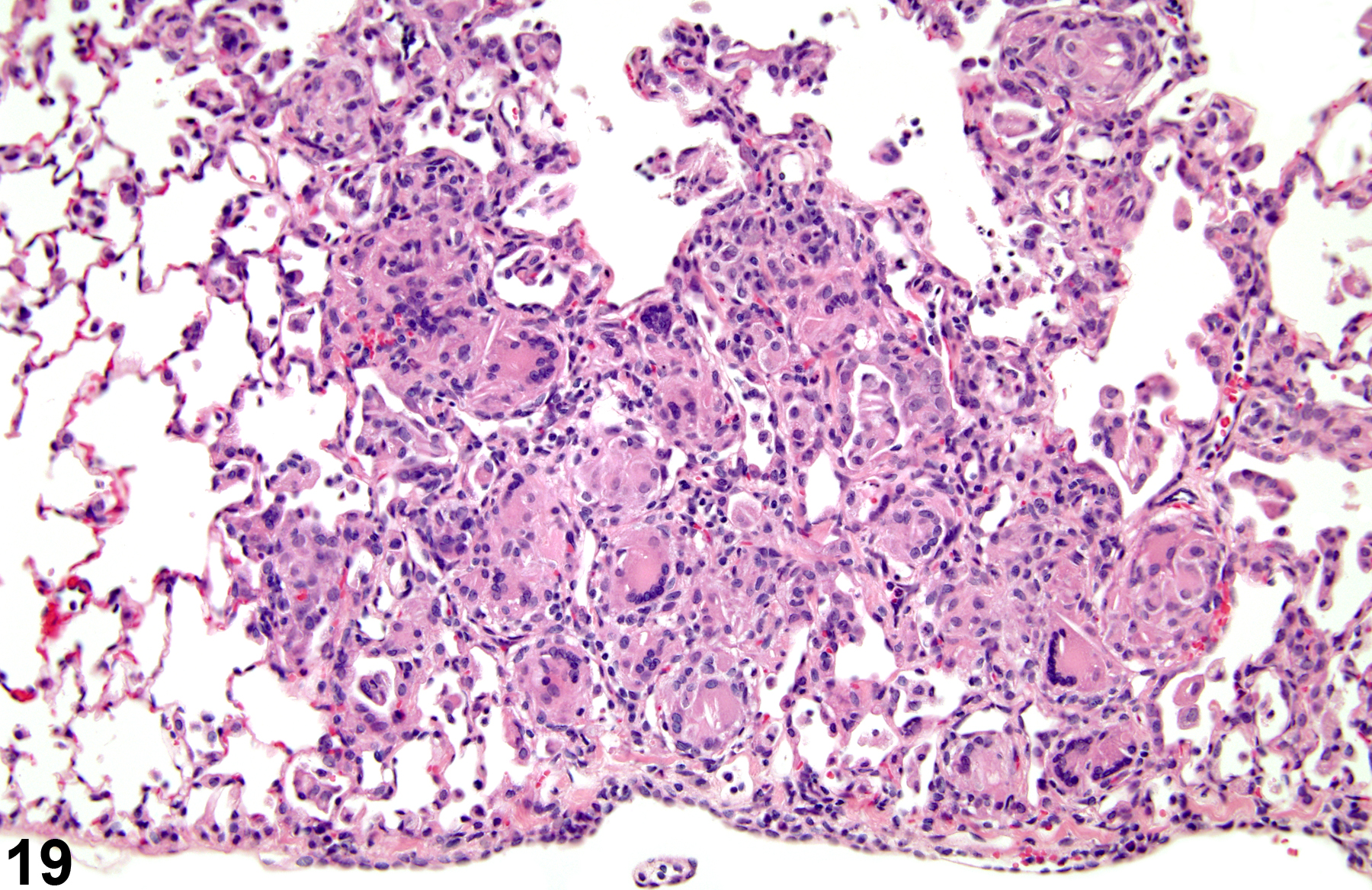
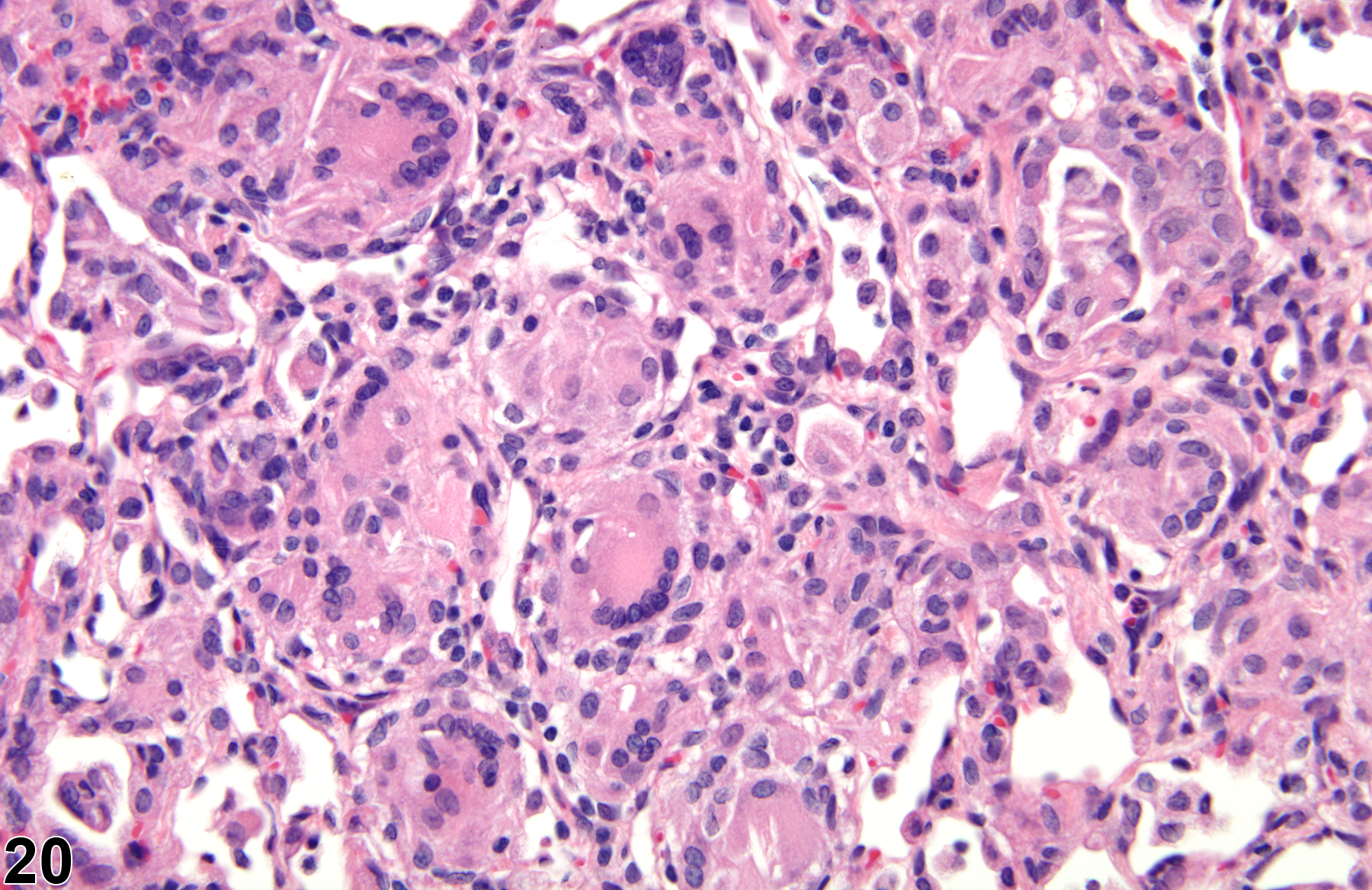
A test agent may stimulate epithelial cells and resident macrophages to secrete cytokines, thus inducing an inflammatory response. Alternatively, a test agent may cause tissue damage, which secondarily results in inflammation. Several compartments within the lung may be inflamed, including the airways (bronchi and bronchioles), the alveoli or alveolar septa (interstitium), the terminal bronchiole/alveolar duct region (acinar region), perivascular areas, and the pleura. Occasionally, focal, minimal inflammation in the lung is seen as a background lesion in mice and rats (Figure 9 and Figure 10), particularly in the subpleural region. Small aggregates of alveolar histiocytes can also be seen (see) as a background lesion and must be differentiated from inflammation. Inflammation can also be caused by a number of infectious agents, but these are rare under current husbandry practices. Systemic bacterial infections affecting the pulmonary interstitium via the bloodstream often produce a suppurative alveolitis, whereas viral infections tend to induce suppurative or mononuclear perivascular inflammation. Inflammation can also be associated with pulmonary neoplasms.
Boorman GA, Eustis SL. 1990. Lung. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman GA, Eustis SL, Elwell MR, Montgomery CA, MacKenzie WF, eds). Academic Press, San Diego, CA, 339-367.
Dixon D, Herbert RA, Sills RC, Boorman GA. 1999. Lungs, pleura, and mediastinum. In: Pathology of the Mouse: Reference and Atlas (Maronpot RR, Boorman GA, Gaul BW, eds). Cache River Press, Vienna, IL, 293-332.
Dungworth DL, Ernst H, Nolte T, Mohr U. 1992. Nonneoplastic lesions in the lungs. In: Pathobiology of the Aging Rat (Mohr U, Dungworth DL, Capen CC, eds). ILSI Press, Washington, DC, 143-160.
Plopper CG, Dungworth DL. 197. Structure, function, cell injury and cell renewal of bronchiolar and alveolar epithelium. In: Lung Carcinomas (McDowell EM, ed). Churchill Livingstone, Edinburgh, 94-128.
Renne, R, Brix A, Harkema J, Herbert R, Kittle B, Lewis D, March T, Nagano K, Pino M, Rittinghausen S, Rosenbruch M, Tellier P, Wohrmann T. 2009. Proliferative and nonproliferative lesions of the rat and mouse respiratory tract. Toxicol Pathol 37(suppl):5S-73S.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/20032296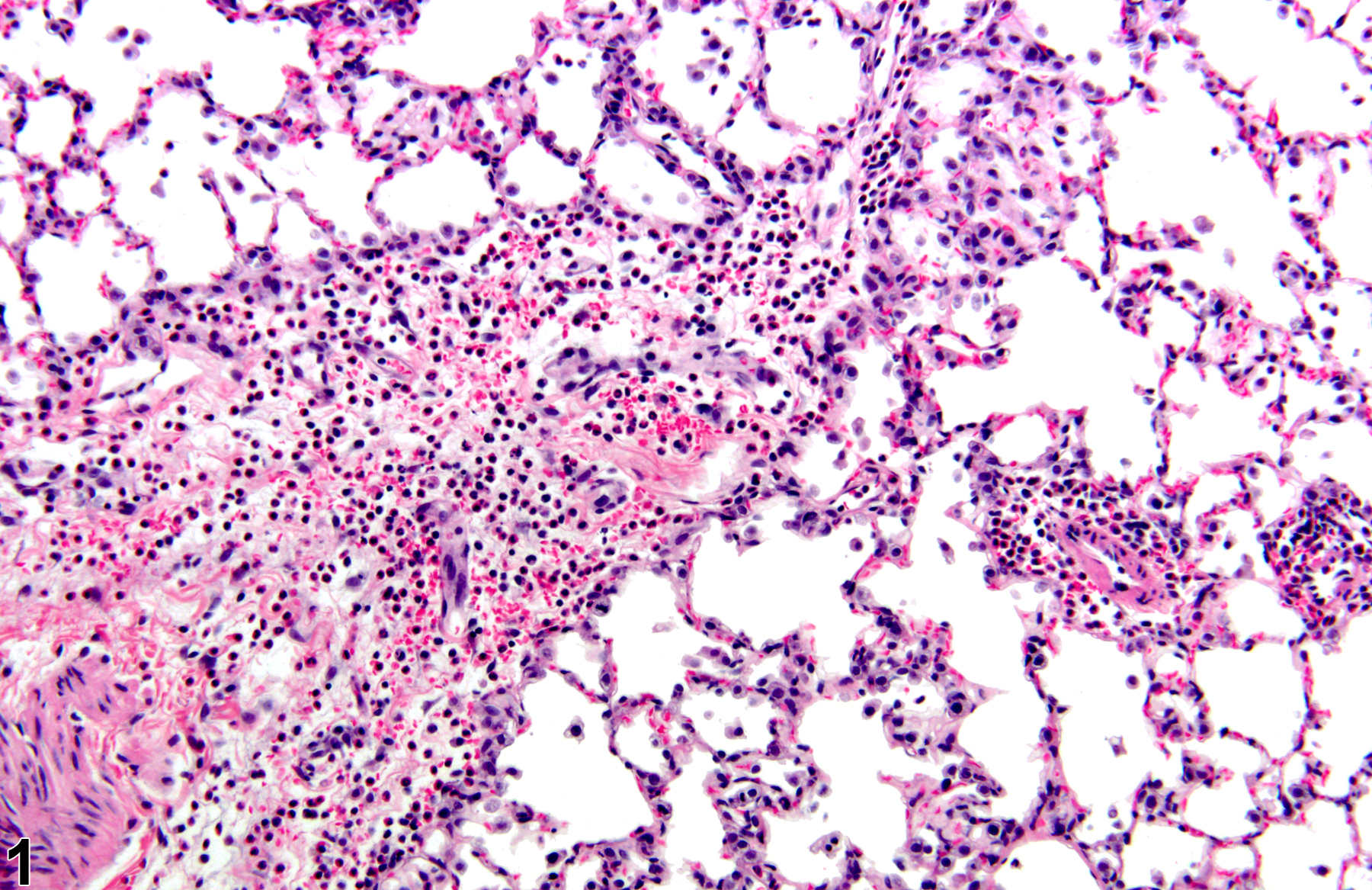
Lung - Inflammation, Acute in a male Wistar Han rat from a subchronic study. The majority of the inflammatory cells are neutrophils; there is also a small amount of hemorrhage.