Respiratory System
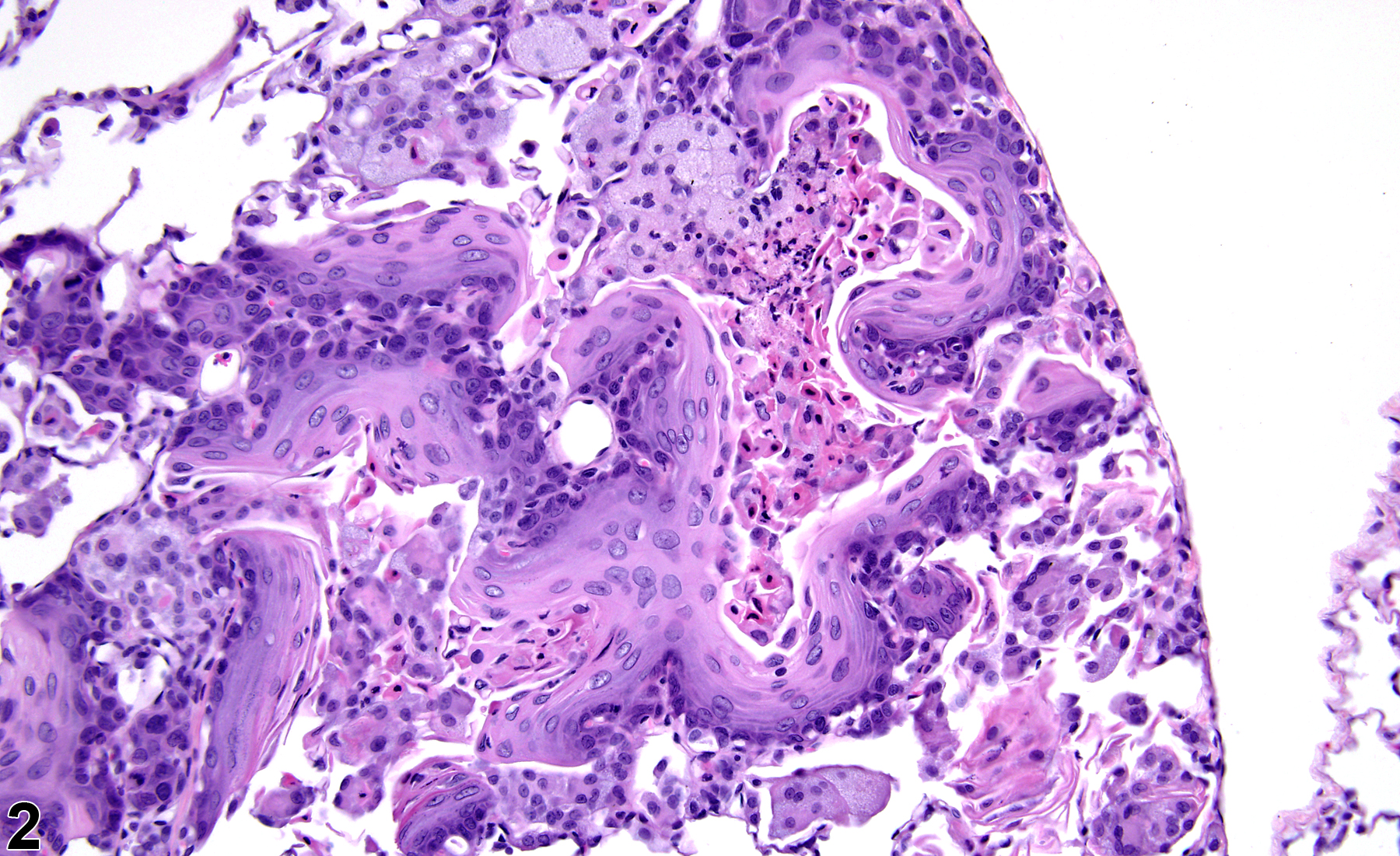
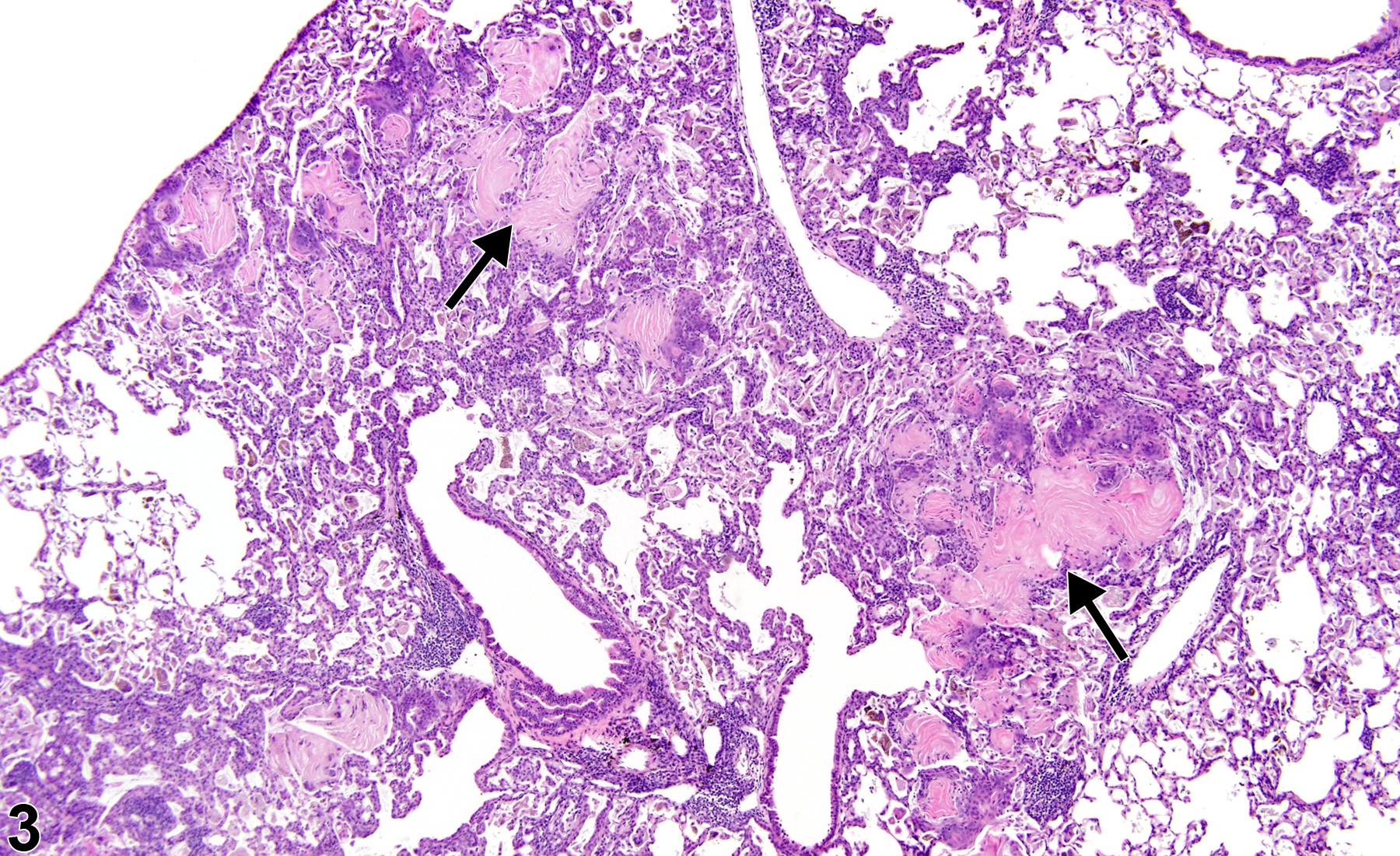
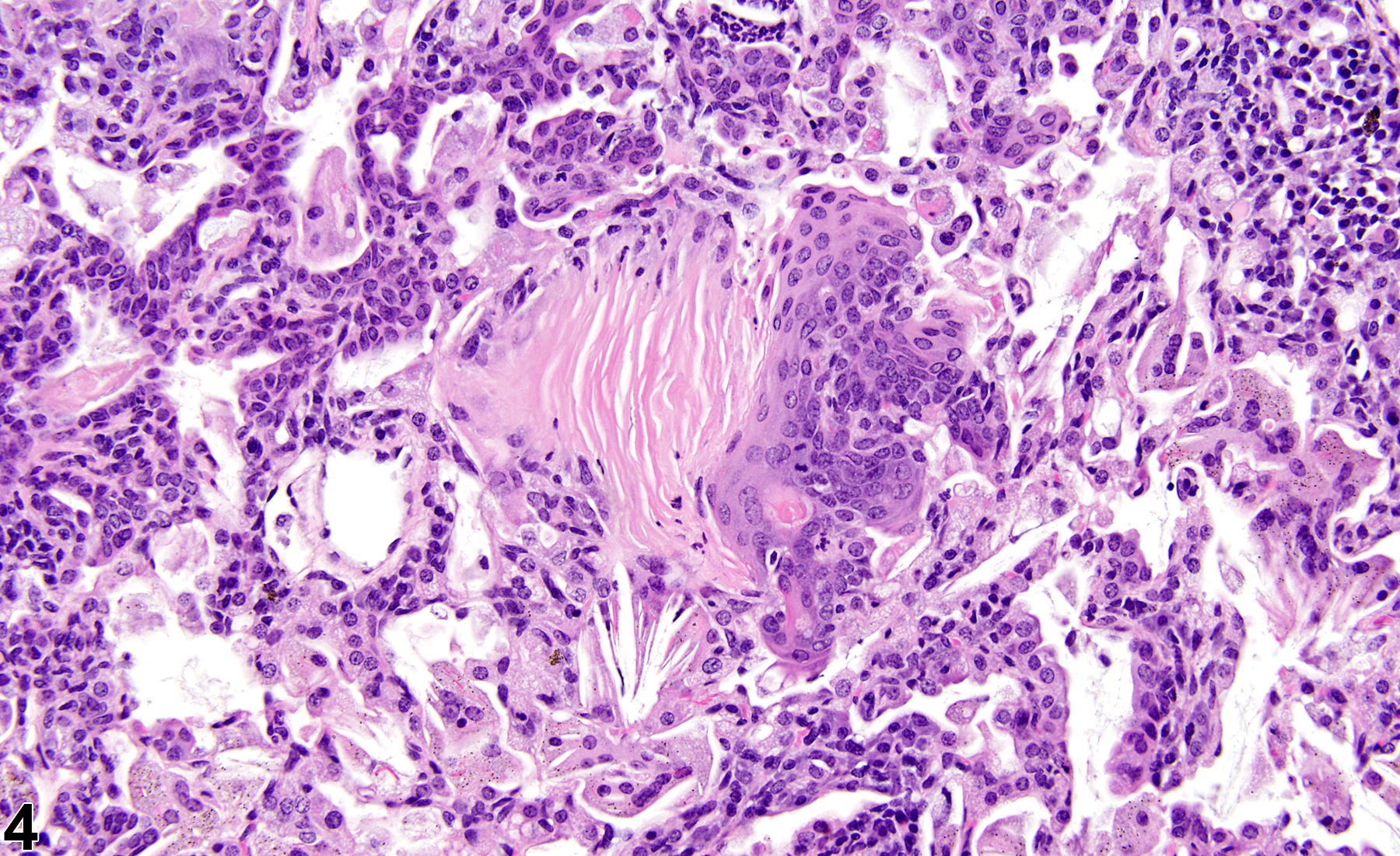
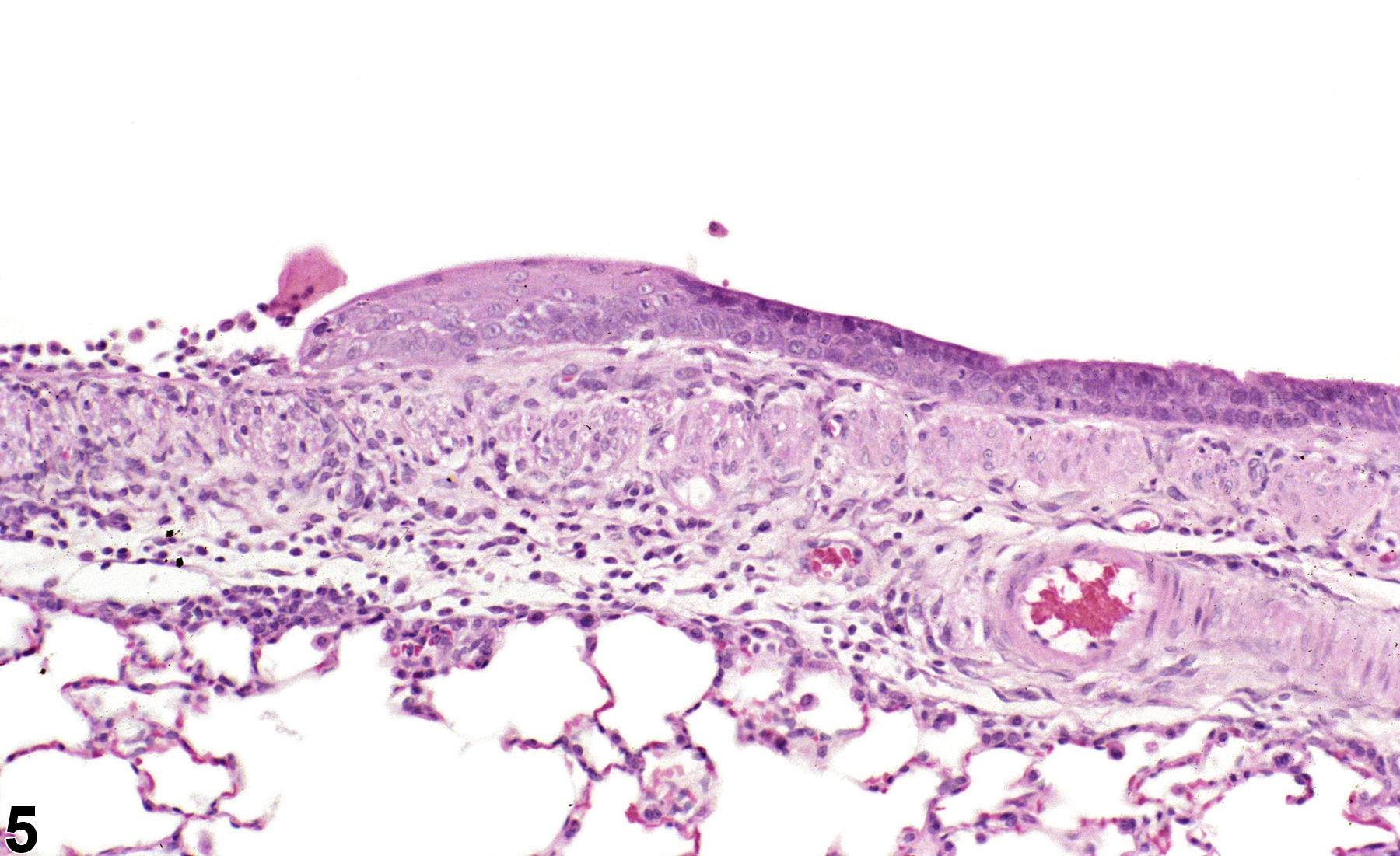
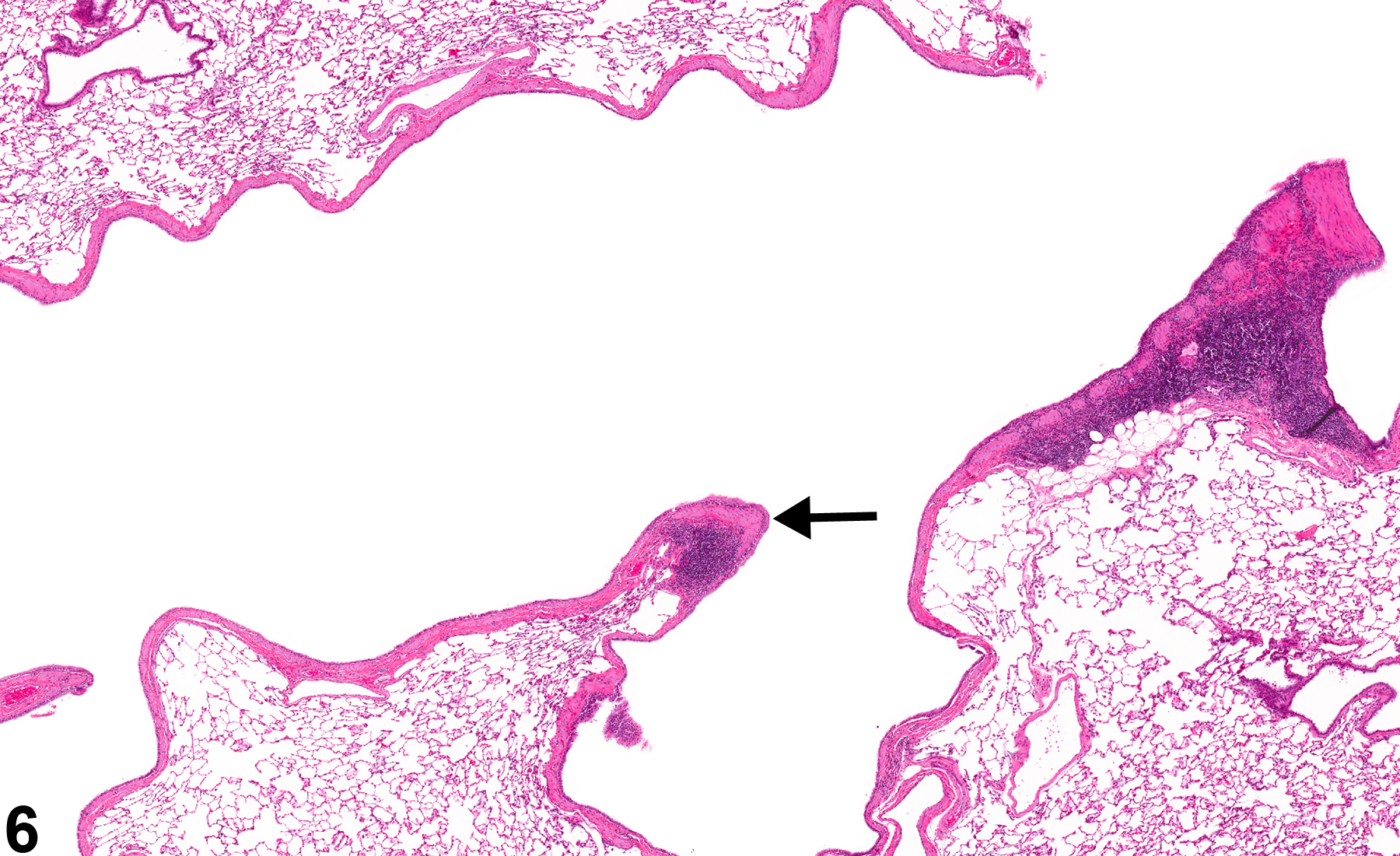
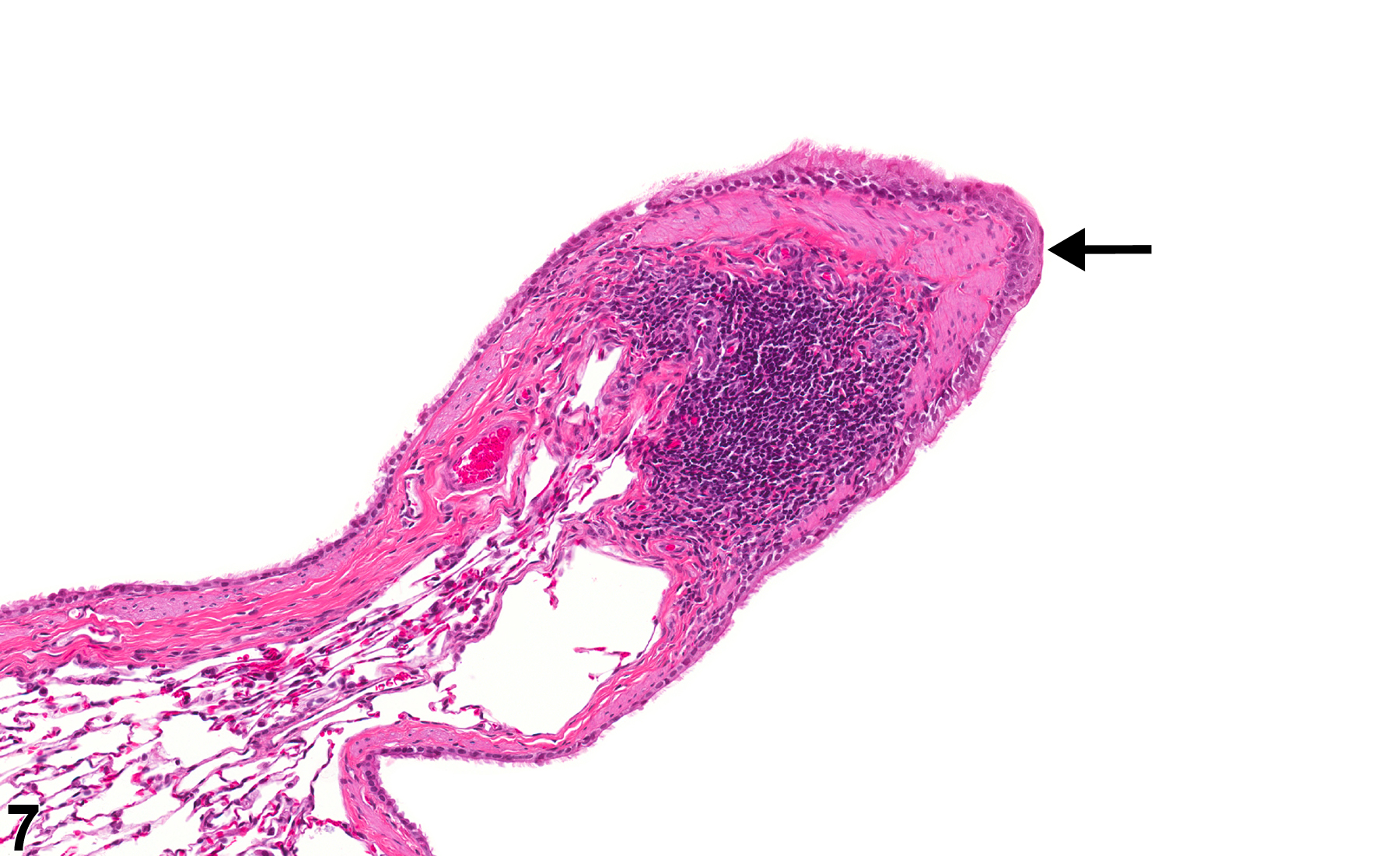
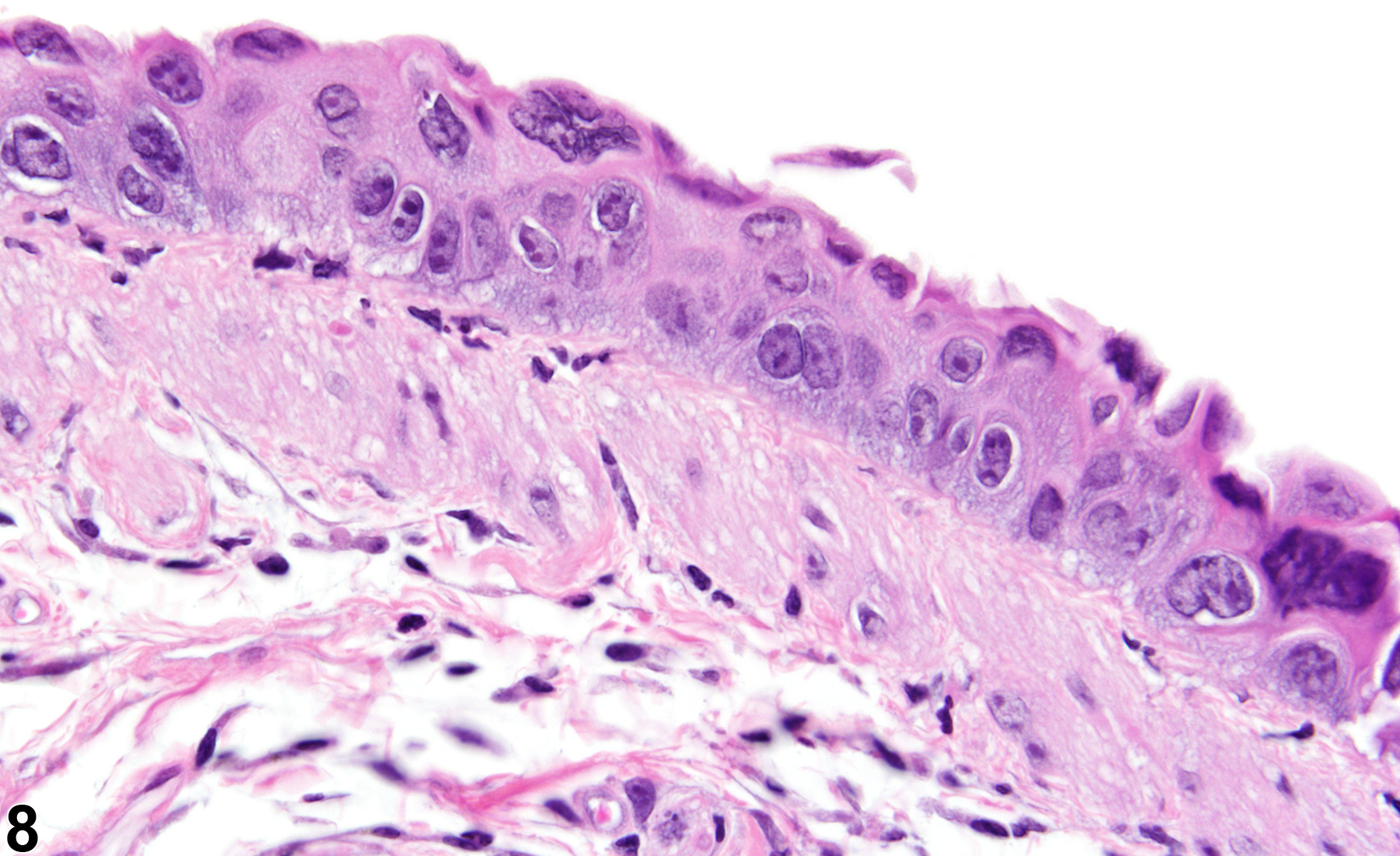
Lung - Metaplasia, Squamous
Narrative
Boorman GA, Eustis SL. 1990. Lung. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman GA, Eustis SL, Elwell MR, Montgomery CA, MacKenzie WF, eds). Academic Press, San Diego, CA, 339-367.
Renne, R, Brix A, Harkema J, Herbert R, Kittle B, Lewis D, March T, Nagano K, Pino M, Rittinghausen S, Rosenbruch M, Tellier P, Wohrmann T. 2009. Proliferative and nonproliferative lesions of the rat and mouse respiratory tract. Toxicol Pathol 37(suppl):5S-73S.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/20032296Sells DM, Brix AE, Nyska A, Jokinen MP, Orzech DP, Walker NJ. 2007. Respiratory tract lesions in noninhalation studies. Toxicol Pathol 35:170-177.
Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3433271/Walker NJ, Yoshizawa K, Miller RA, Brix AE, Sells DM, Jokinen MP, Wyde ME, Easterling M, Nyska A. 2007. Pulmonary lesions in female Harlan Sprague-Dawley rats following two-year oral treatment with dioxin-like compounds. Toxicol Pathol 35:880-889.
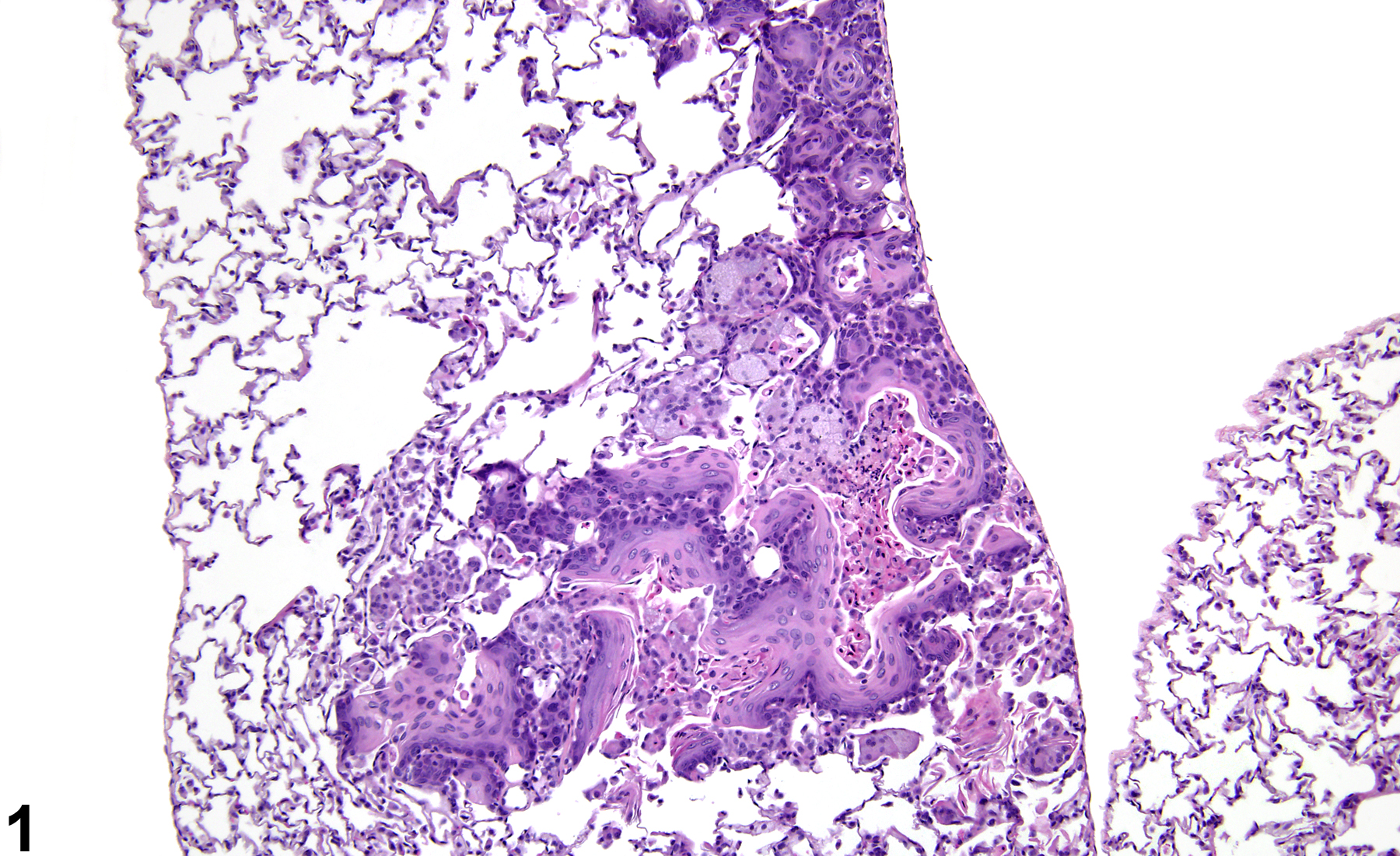
Lung, Alveolus - Metaplasia, Squamous in a female Harlan Sprague-Dawley rat from a subchronic study. The normal alveolar epithelium has been replaced by squamous epithelium.