Respiratory System
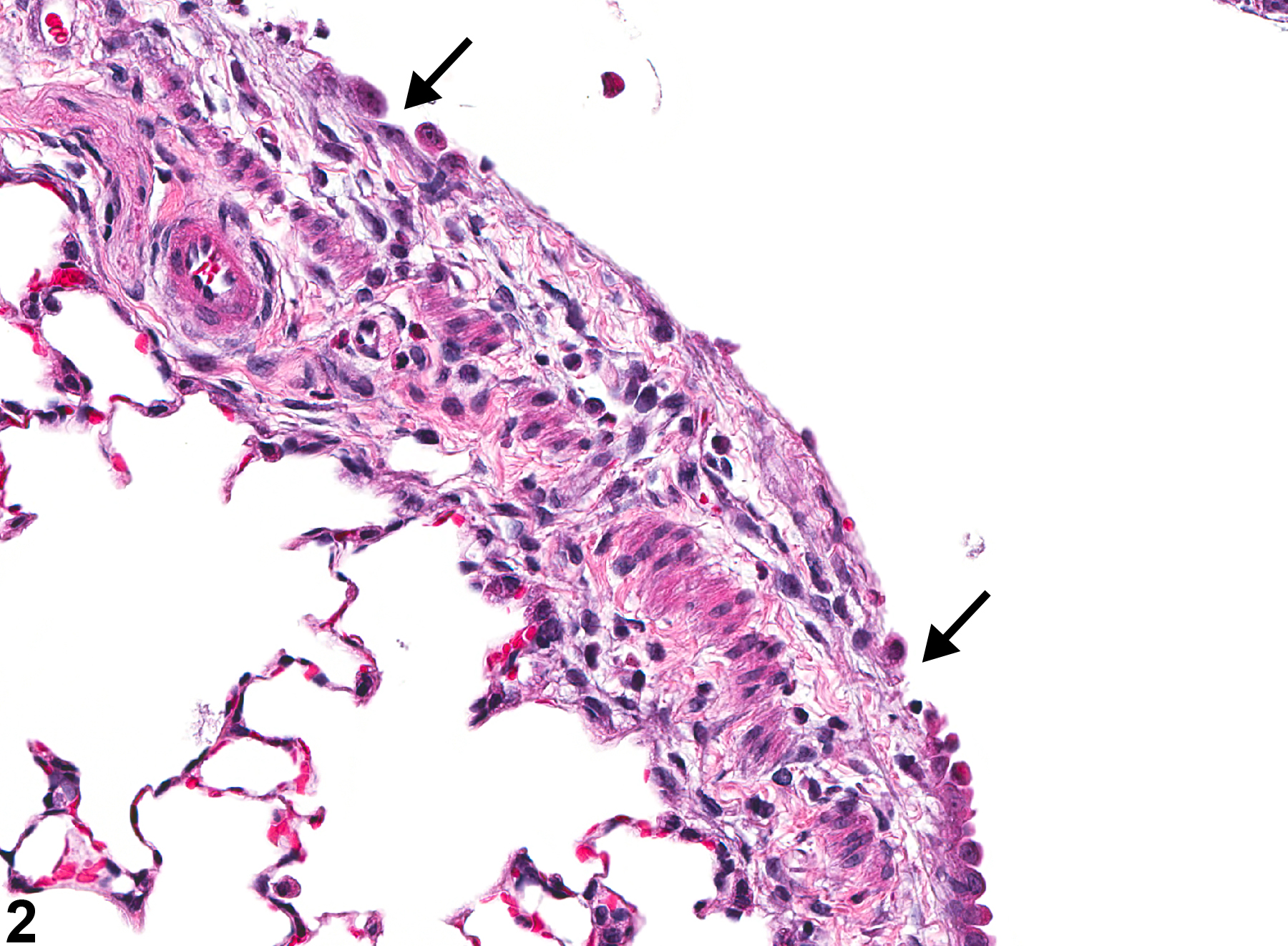
Lung - Ulceration
Narrative
Boorman GA, Eustis SL. 1990. Lung. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman GA, Eustis SL, Elwell MR, Montgomery CA, MacKenzie WF, eds). Academic Press, San Diego, CA, 339-367.
Bucher JR, Boorman GA, Gupta BN, Uraih LC, Hall LB, Stefanski SA. 1987. Two-hour methyl isocyanate inhalation exposure and 91-day recovery: A preliminary description of pathologic changes in F344 rats. Environ Health Perspect 72:71-75.
Abstract: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1474667/Dixon D, Herbert RA, Sills RC, Boorman GA. 1999. Lungs, pleura, and mediastinum. In: Pathology of the Mouse: Reference and Atlas (Maronpot RR, Boorman GA, Gaul BW, eds). Cache River Press, Vienna, IL, 293-332.
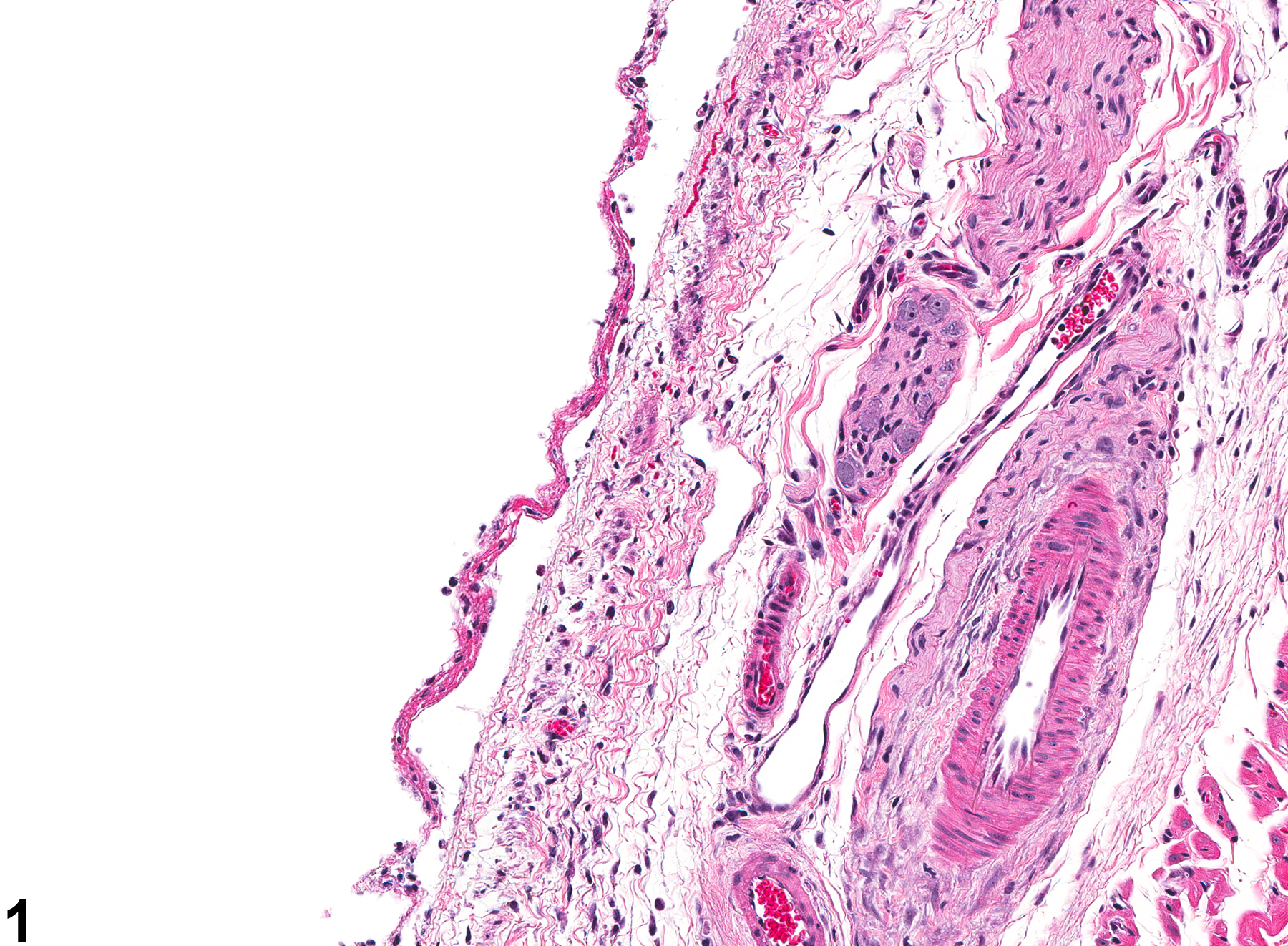
Lung, Bronchus - Ulceration in a male Wistar Han rat from an acute study. A ribbon of necrotic tissue is adjacent to the bronchial surface, which has lost its epithelial cells.