Respiratory System
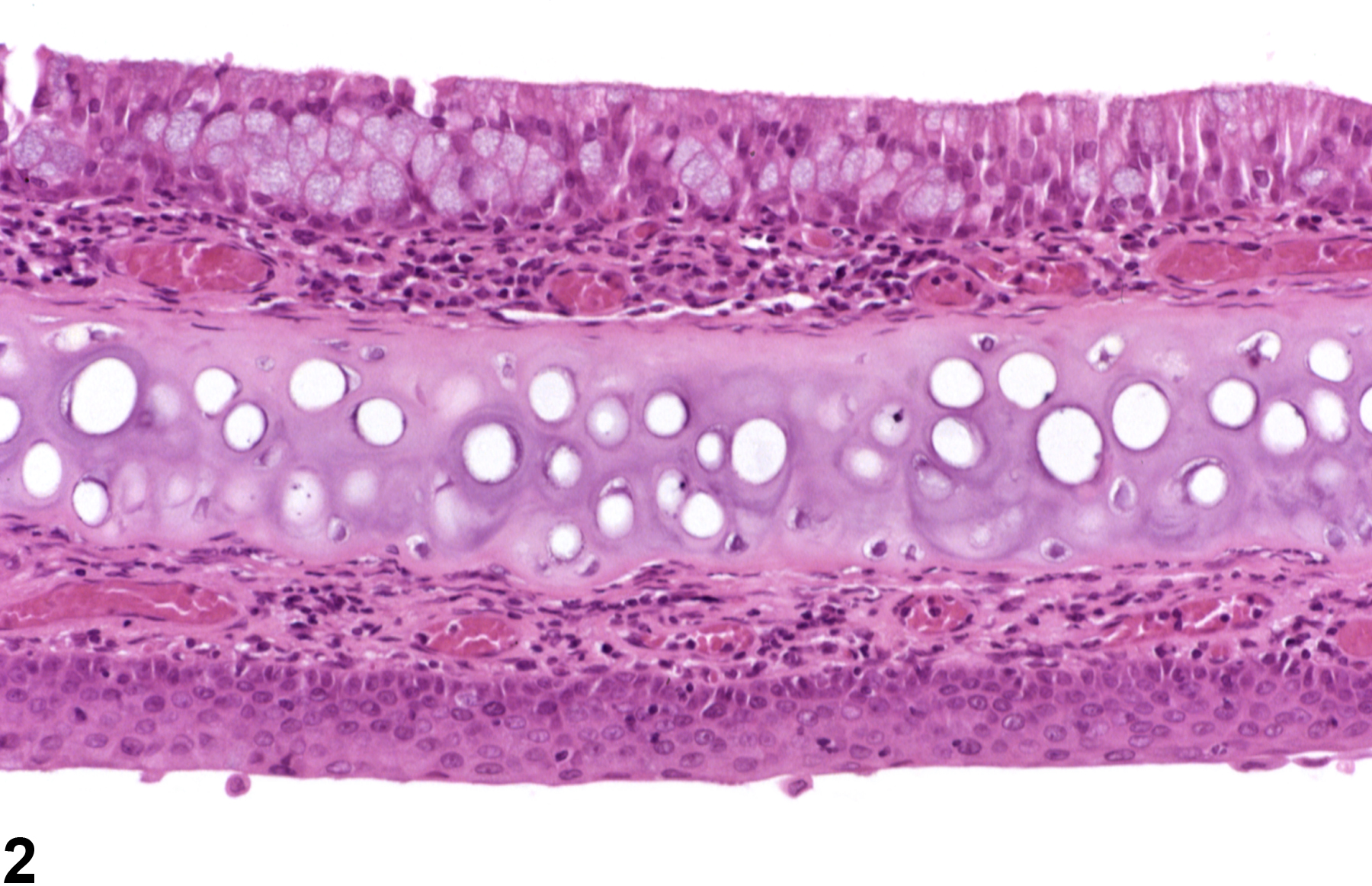
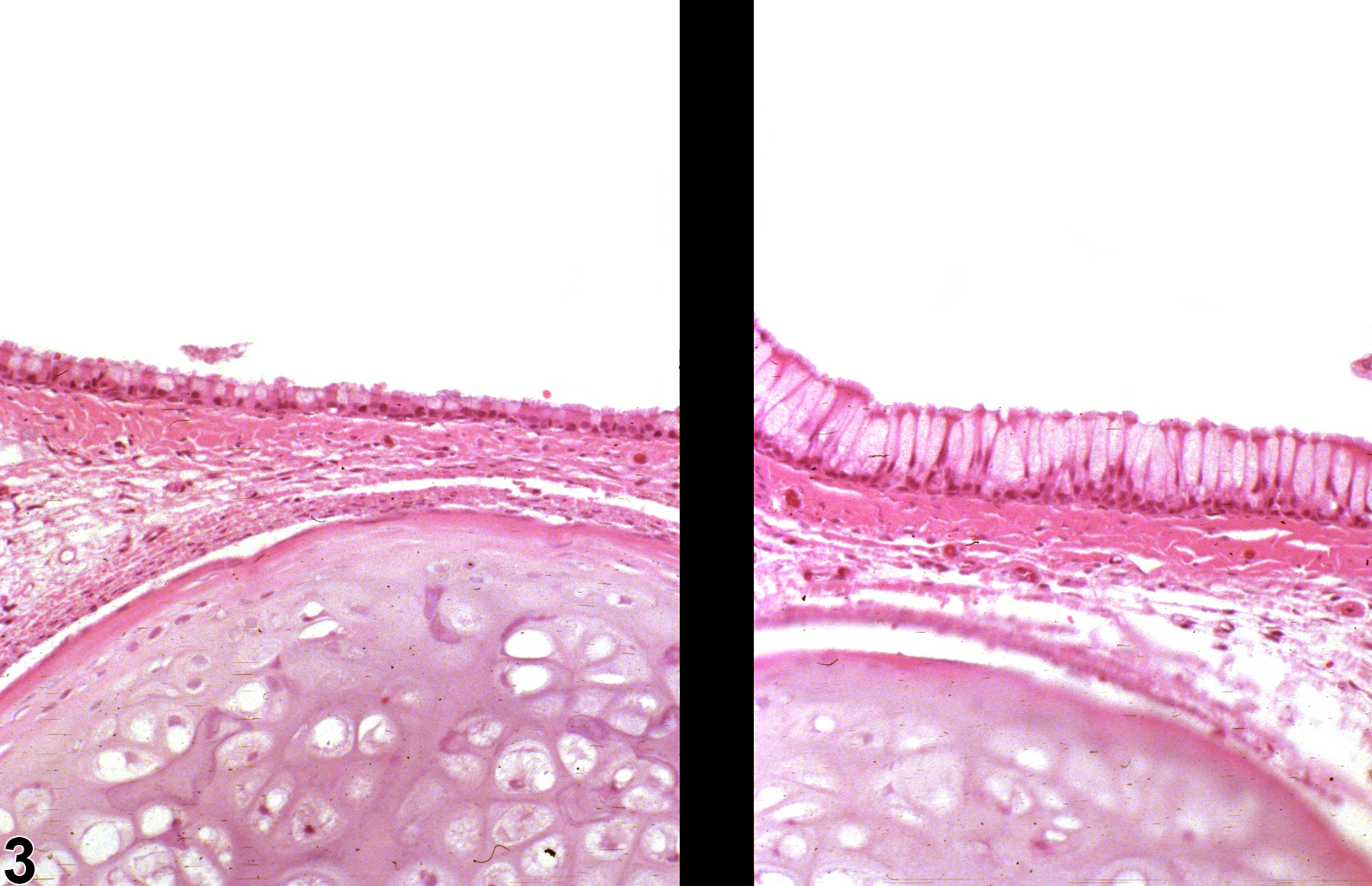
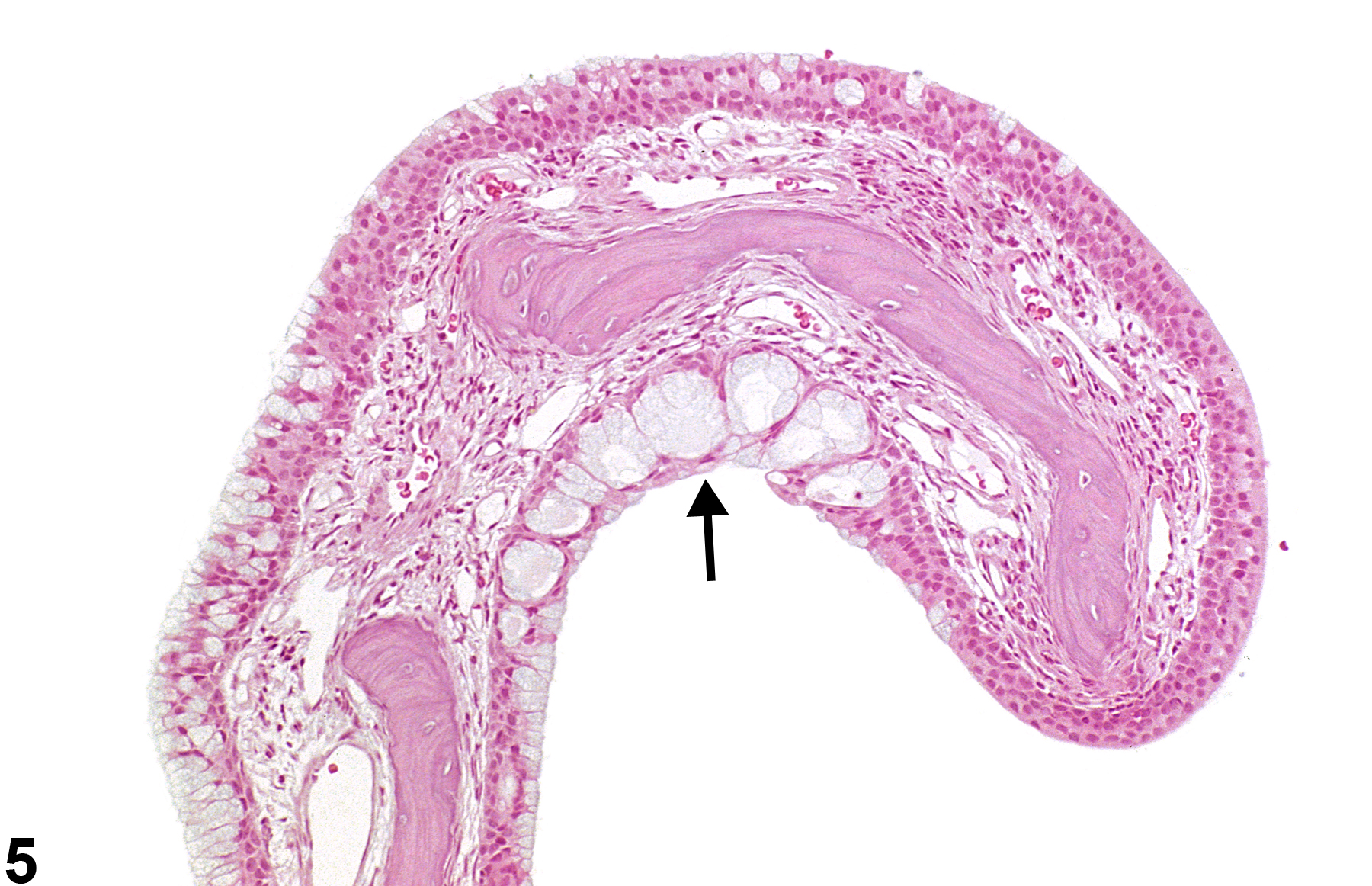
Nose - Hyperplasia, Goblet Cell
Narrative
Boorman GA, Morgan KT, Uraih LC. 1990. Nose, larynx, and trachea. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman GA, Eustis SL, Elwell MR, eds). Academic Press, San Diego, 315-337.
Harkema JR, Hotchkiss JA, Henderson RF. 1989. Effects of 0.12 and 0.80 ppm ozone on rat nasal and nasopharyngeal epithelial mucosubstances: Quantitative histochemistry. Toxicol Pathol 17:525-535.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/2814228Harkema JR, Morgan KT, Gross EA, Catalano PJ, Griffith WC. 1994. Consequences of Prolonged Inhalation of Ozone on F344/N Rats: Collaborative Studies. Part VII: Effects on the Nasal Mucociliary Apparatus. Research Report No. 65. Health Effects Institute, Cambridge, MA.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/7888110Herbert RA, Leninger JR. 1999. Nose, larynx, and trachea. In: Pathology of the Mouse: Reference and Atlas (Maronpot RR, ed). Cache River Press, Vienna, IL, 259-292.
Monticello TM, Morgan KT, Uraih LC. 1990. Nonneoplastic nasal lesions in rats and mice. Environ Health Perspect 85:249-274.
Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1568333/National Toxicology Program. 1997. NTP TR-461. Toxicology and Carcinogenesis Studies of Nitromethane (CAS No. 75-52-5) in F344/N Rats and B6C3F1 Mice (Inhalation Studies). NTP, Research Triangle Park, NC.
Abstract: https://ntp.niehs.nih.gov/go/6066National Toxicology Program. 1999. NTP TR-490. Toxicology and Carcinogenesis Studies of Glutaraldehyde (CAS No. 111-30-8) in F344/N Rats and B6C3F1 Mice (Inhalation Studies). NTP, Research Triangle Park, NC.
Abstract: https://ntp.niehs.nih.gov/go/10170Renne R, Brix A, Harkema J, Kittel B, Lewis D, March T, Nagano K, Pino M, Rittinghausen S, Rosenbruch M, Tellier P, Wohrmann T. 2009. Proliferative and nonproliferative lesions of the rat and mouse respiratory tract. Toxicol Pathol 37(7 suppl):5S-73S.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/20032296Wagner JG, Hotchkiss JA, Harkema JR. 2001. Effects of ozone and endotoxin coexposure on rat airway epithelium: Potentiation of toxicant-induced alterations. Environ Health Perspect 109:591-598.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/11544169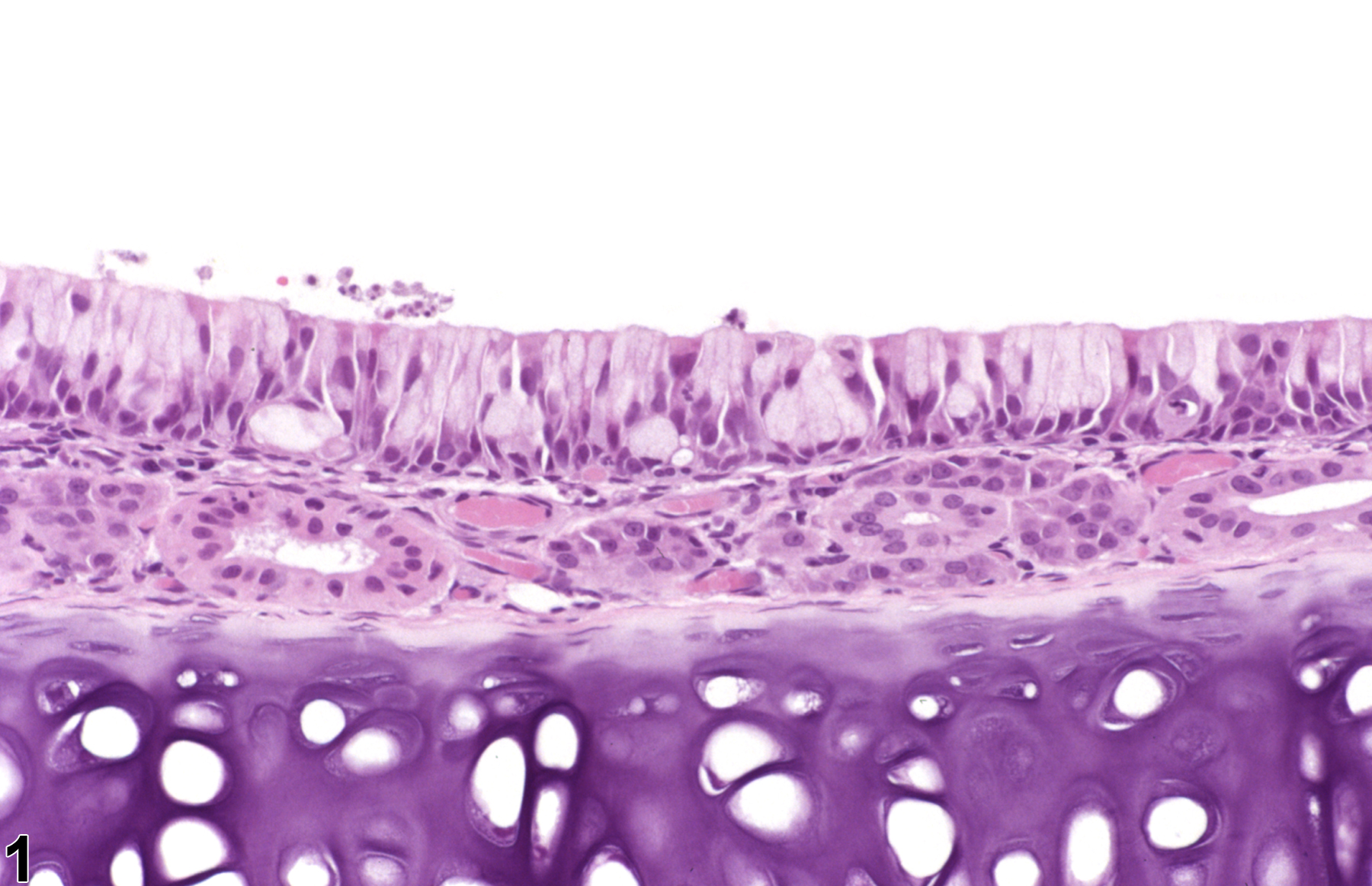
Nose, Respiratory epithelium - Hyperplasia, Goblet cell in a male F344/N rat from a chronic study. Goblet cells are increased in number in the epithelium lining the nasal septum.