Special Senses System
Eye, Cornea - Fibrosis
Narrative
Chen M, Matsuda H, Wang L, Watanabe T, Kimura MT, Igarishi J, Wang X, Sakimoto T, Fukuda N, Sawa M, Nagase H. 2010. Pretranscriptional regulation of Tgf-β1 by PI polyamide prevents scarring and accelerates wound healing of the cornea after exposure to alkali. Mol Ther 18:519-527.
Full Text: http://www.nature.com/mt/journal/v18/n3/full/mt2009263a.htmlGaliacy SD, Fournié P, Massoudi D, Ancèle E, Quintyn JC, Erraud A, Raymond-Letron I, Rolling F, Malecaze F. 2011. Matrix metalloproteinase 14 overexpression reduces corneal scarring. Gene Ther 18:462-468.
Abstract: http://www.nature.com/gt/journal/v18/n5/full/gt2010159a.htmlGeiss V, Yoshitomi K. 1991. Eyes. In: Pathology of the Mouse: Reference and Atlas (Maronpot RR, Boorman GA, Gaul BW, eds). Cache River Press, Vienna, IL, 471-489.
Newkirk KM, Chandler HL, Parent AE, Young DC, Colitz CMH, Wilkie DA, Kusewitt DF. 2007. Ultraviolet radiation-induced corneal degeneration in 129 mice. Toxicol Pathol 35:817-824.
Full Text: http://tpx.sagepub.com/content/35/6/817.fullNational Toxicology Program. 1989. NTP TR-342. Toxicology and Carcinogenesis Studies of Dichlorvos (CAS No. 62-73-7) in F344/N Rats and B6C3F1 Mice (Gavage Studies). NTP, Research Triangle Park, NC.
Abstract: https://ntp.niehs.nih.gov/go/10790West-Mays JA. 2006. The keratocyte: Corneal stromal cell with variable repair phenotypes. Int J Biochem Cell Biol 38:1625-1631.
Abstract: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2505273/Wilson SE. 2012. Corneal myofibroblast biology and pathobiology: Generation, persistence, and transparency. Exp Eye Res 99:78-88.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/22542905Yoshitomi K, Boorman GA. 1990. Eye and associated glands. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman GA, Eustis SL, Elwell MR, Montgomery CA, MacKenzie WF, eds). Academic Press, San Diego, CA, 239-260.
Abstract: https://www.ncbi.nlm.nih.gov/nlmcatalog/9002563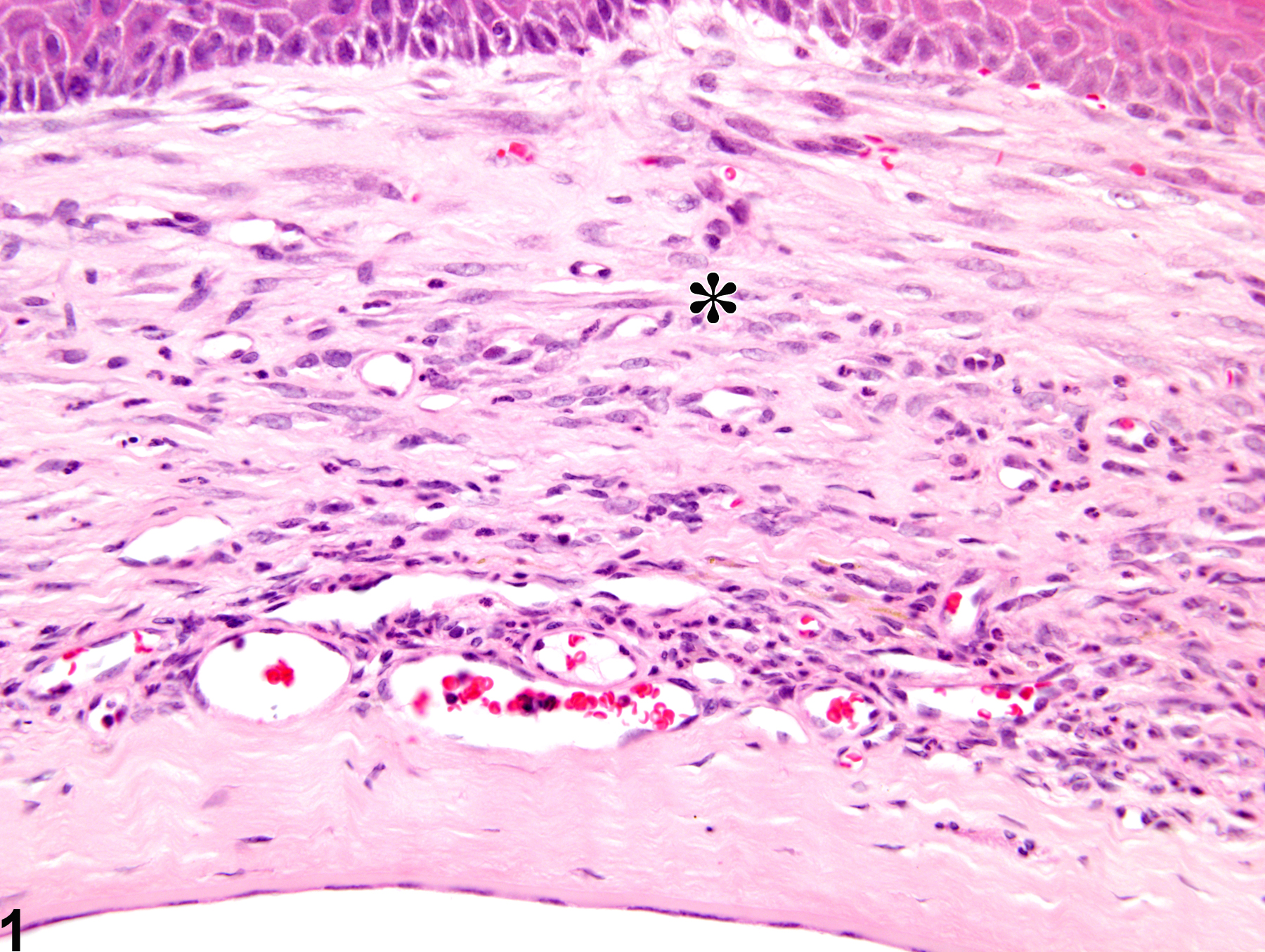
Eye, Cornea - Fibrosis in a male B6C3F1 mouse from a chronic study. The normal orderly collagen lamellar architecture is replaced by coarse, irregular bundles of collagen fibers.


