Special Senses System
Eye, Retina - Detachment
Narrative
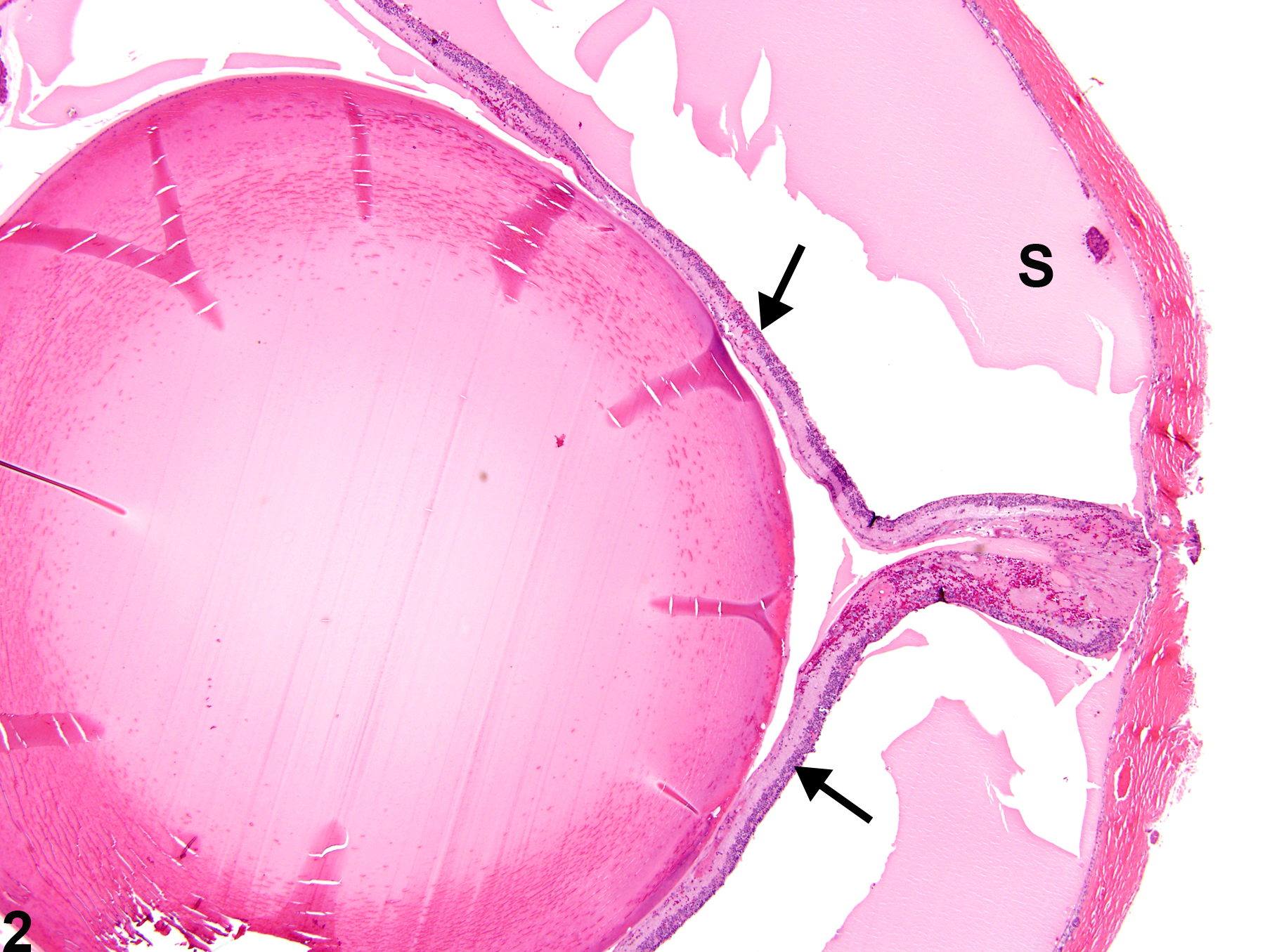
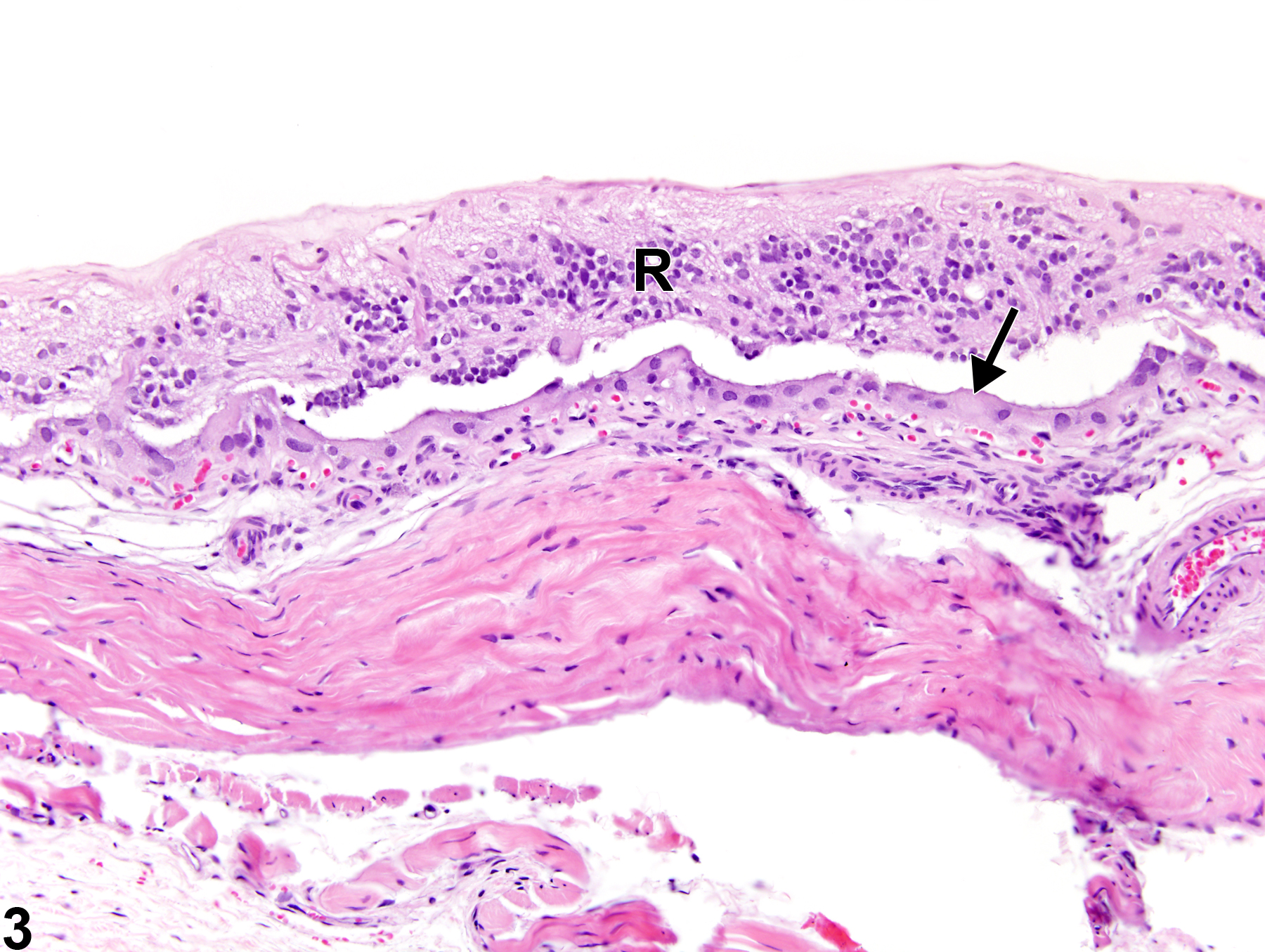
Complete retinal detachment can result in a classic cone or funnel shape that in microscopic cross section has a Y- or V-like configuration (Figure 1 and Figure 2). Large amounts of subretinal fluid may displace the detached and degenerate retina from the posterior fundus. The detached retina may be degenerate, and the RPE may exhibit hypertrophy and hyperplasia (Figure 2).
Geiss V, Yoshitomi K. 1991. Eyes. In: Pathology of the Mouse: Reference and Atlas (Maronpot RR, Boorman GA, Gaul BW, eds). Cache River Press, Vienna, IL, 471-489.
Greaves P. 2007. Nervous system and special sense organs. In: Histopathology of Preclinical Toxicity Studies: Interpretation and Relevance in Drug Safety Evaluation, 3rd ed. Academic Press, San Diego, CA, 861-933.
Abstract: http://www.sciencedirect.com/science/book/9780444527714Kakehashi A, Saito Y, Mori K, Sugi N, Ono R, Yamagami H, Shinohara M, Tamemoto H, Ishikawa SE, Kawakami M, Kanazawa Y. 2006. Characteristics of diabetic retinopathy in SDT rats. Diabetes Metab Res Rev 22:455-461.
Full Text: http://onlinelibrary.wiley.com/doi/10.1002/dmrr.638/fullKuno H, Usui T, Eydelloth RS, Wolf ED. 1991. Spontaneous ophthalmic lesions in young Sprague-Dawley rats. J Vet Med Sci 53:607-614.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/10845604National Toxicology Program. 1997. NTP TR-450. Toxicology and Carcinogenesis Studies of Tetrafluoroethylene (CAS No. 116-14-3) in F344 Rats and B6C3F1 Mice (Inhalation Studies). NTP, Research Triangle Park, NC.
Abstract: https://ntp.niehs.nih.gov/go/6044Ramos M, Reilly CM, Bolon B. 2011. Toxicological pathology of the retina and optic nerve. In: Fundamental Neuropathology for Pathologists and Toxicologists (Bolon B, Butt MT, eds). Wiley, Hoboken, NJ, 385-412.
Abstract: http://onlinelibrary.wiley.com/doi/10.1002/9780470939956.ch24/summarySmith RS, Hawes NL, Chang B, Nishina PM. 2002. Retina. In: Systematic Evaluation of the Mouse Eye: Anatomy, Pathology, and Biomethods (Smith RS, John SWM, Nishina PM, Sundberg JP, eds). CRC Press, Boca Raton, FL, 195-225.
Takase H, Yu C-R, Ham D-I, Chan C-C, Chen J, Vistica BP, Warousek EF, Durum SK, Egwuagu CE, Gery I. 2006. Inflammatory processes triggered by TCR engagement or by local cytokine expression: Differences in profiles of gene expression and infiltrating cell populations. J Leukocyte Biol 80:538-545.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/16793919Taradach C, Greaves P, Rubin LF. 1984. Spontaneous eye lesions in laboratory animals: Incidence in relation to age. Crit Rev Toxicol 12:121-147.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/6368130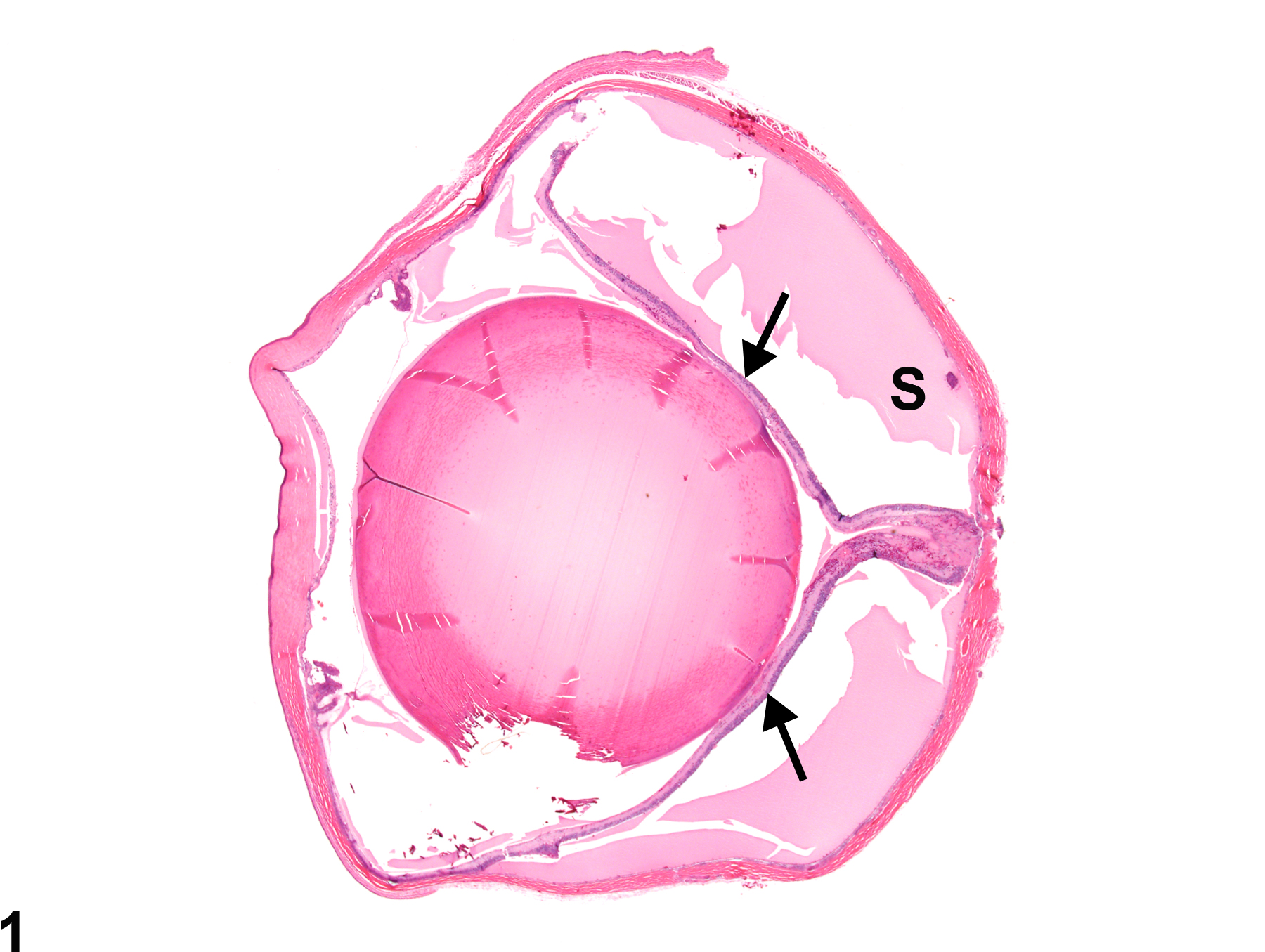
Eye, Retina - Detachment in a female F344/N rat from a chronic study. The retina is detached from the posterior fundus, remaining attached only at the optic disc and the ora ciliaris retinae, resulting in the classic "Y-shaped" configuration, and there is proteinaceous fluid in the subretinal space (S).
All Images

Eye, Retina - Detachment in a female F344/N rat from a chronic study. The retina is detached from the posterior fundus, remaining attached only at the optic disc and the ora ciliaris retinae, resulting in the classic "Y-shaped" configuration, and there is proteinaceous fluid in the subretinal space (S).