Special Senses System
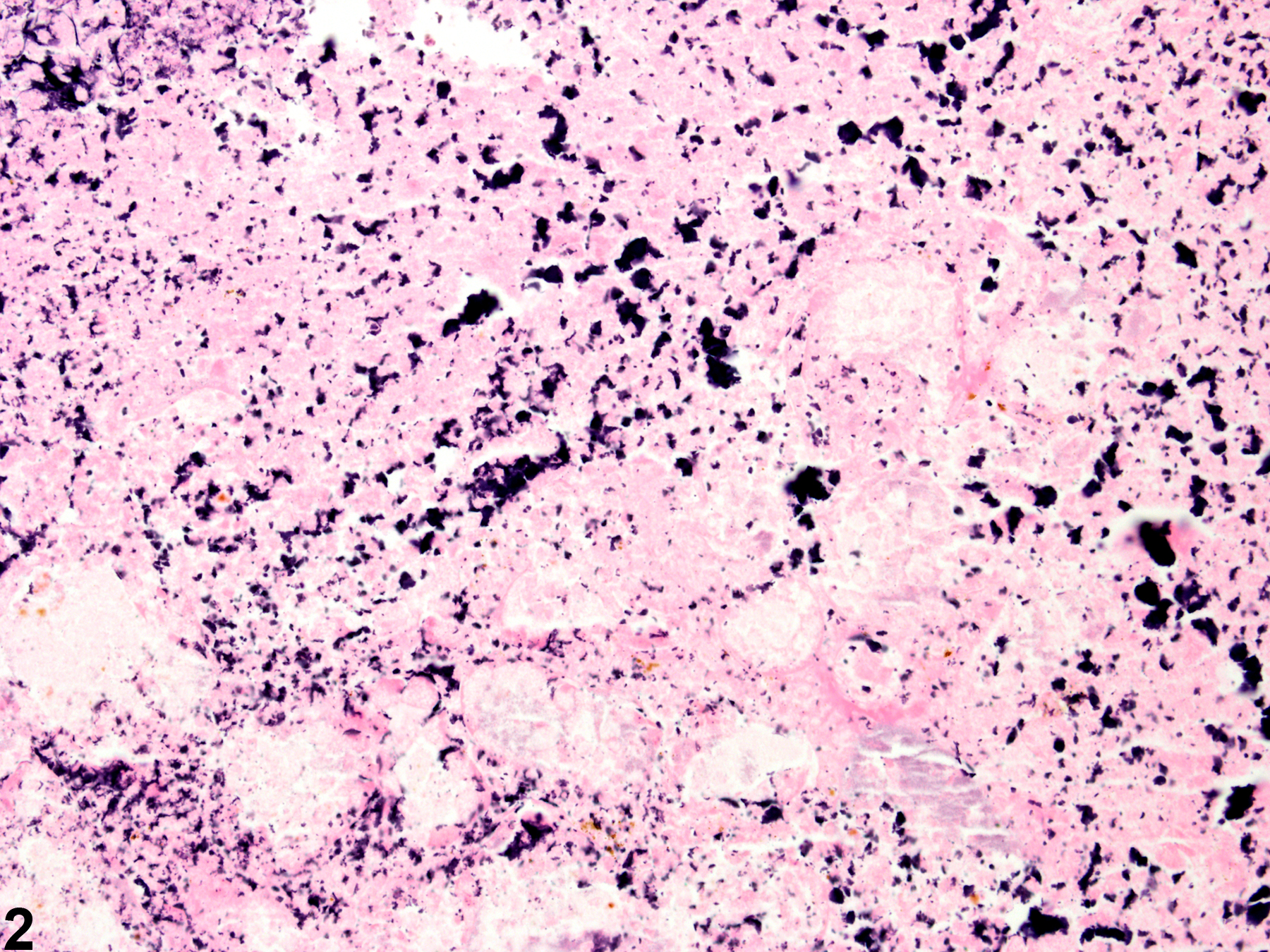
Harderian Gland - Necrosis
Narrative
Botts S, Jokinen M, Gaillard ET, Elwell MR, Mann PC. 1999. Salivary, Harderian, and lacrimal glands. In: Pathology of the Mouse: Reference and Atlas (Maronpot RR, Boorman GA, Gaul BW, eds). Cache River Press, Vienna, IL, 49-79.
Carlson BM, Rainin EA. 1985. Rat extraocular muscle regeneration: Repair of local anesthetic-induced damage. Arch Ophthalmol 103:1373-1377.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/4038130Carthew P, Slinger RP. 1982. Diagnosis of sialodacryoadenitis virus infection of rats in a virulent enzootic outbreak. Lab Anim 15:339-342.
Abstract: http://lan.sagepub.com/content/15/4/339.shortNational Toxicology Program. 1992. NTP TR-388. Toxicology and Carcinogenesis Studies of Ethylene Thiourea (CAS: 96-45-7) in F344 Rats and B6C3F1 Mice (Feed Studies). NTP, Research Triangle Park, NC.
Abstract: https://ntp.niehs.nih.gov/go/12227O’Steen WK, Kraeer SL, Shear CR. 1978. Extraocular muscle and Harderian gland degeneration and regeneration after exposure of rats to continuous fluorescent illumination. Invest Ophthalmol Vis Sci 17:847-856.
Abstract: https://pubmed.ncbi.nlm.nih.gov/700964/Strum JM, Shear CR. 1982. Constant light exposure induces damage and squamous metaplasia in Harderian glands of albino mice. Tissue Cell 14:149-161.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/7089962Yoshitomi K, Boorman GA. 1990. Eye and associated glands. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman GA, Eustis SL, Elwell MR, Montgomery CA, MacKenzie WF, eds). Academic Press, San Diego, CA, 239-260.
Abstract: https://www.ncbi.nlm.nih.gov/nlmcatalog/9002563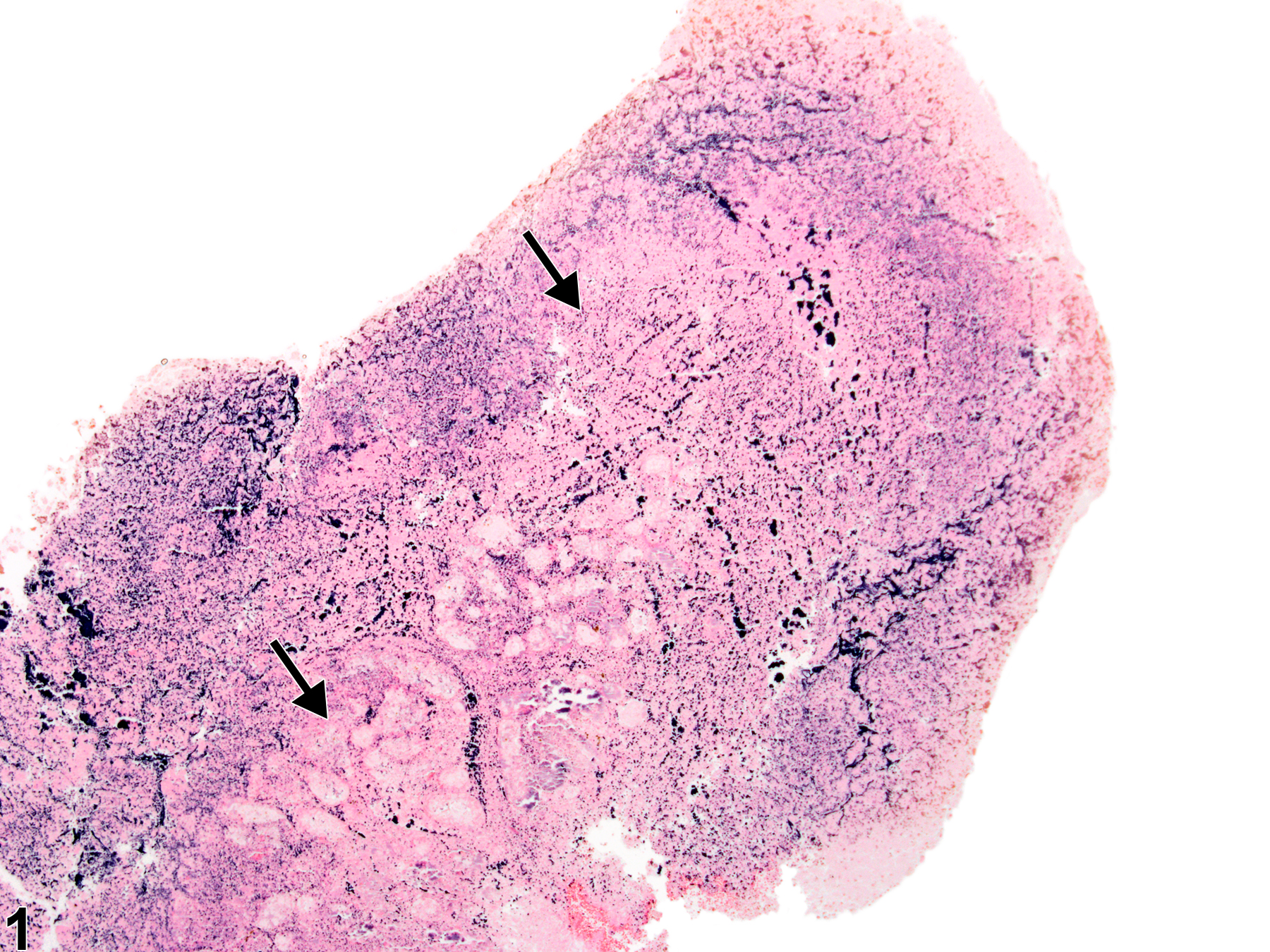
Harderian gland - Necrosis in a male B6C3F1 mouse from a chronic study. Large areas are effaced and replaced by necrotic cell debris (arrows).