Special Senses System
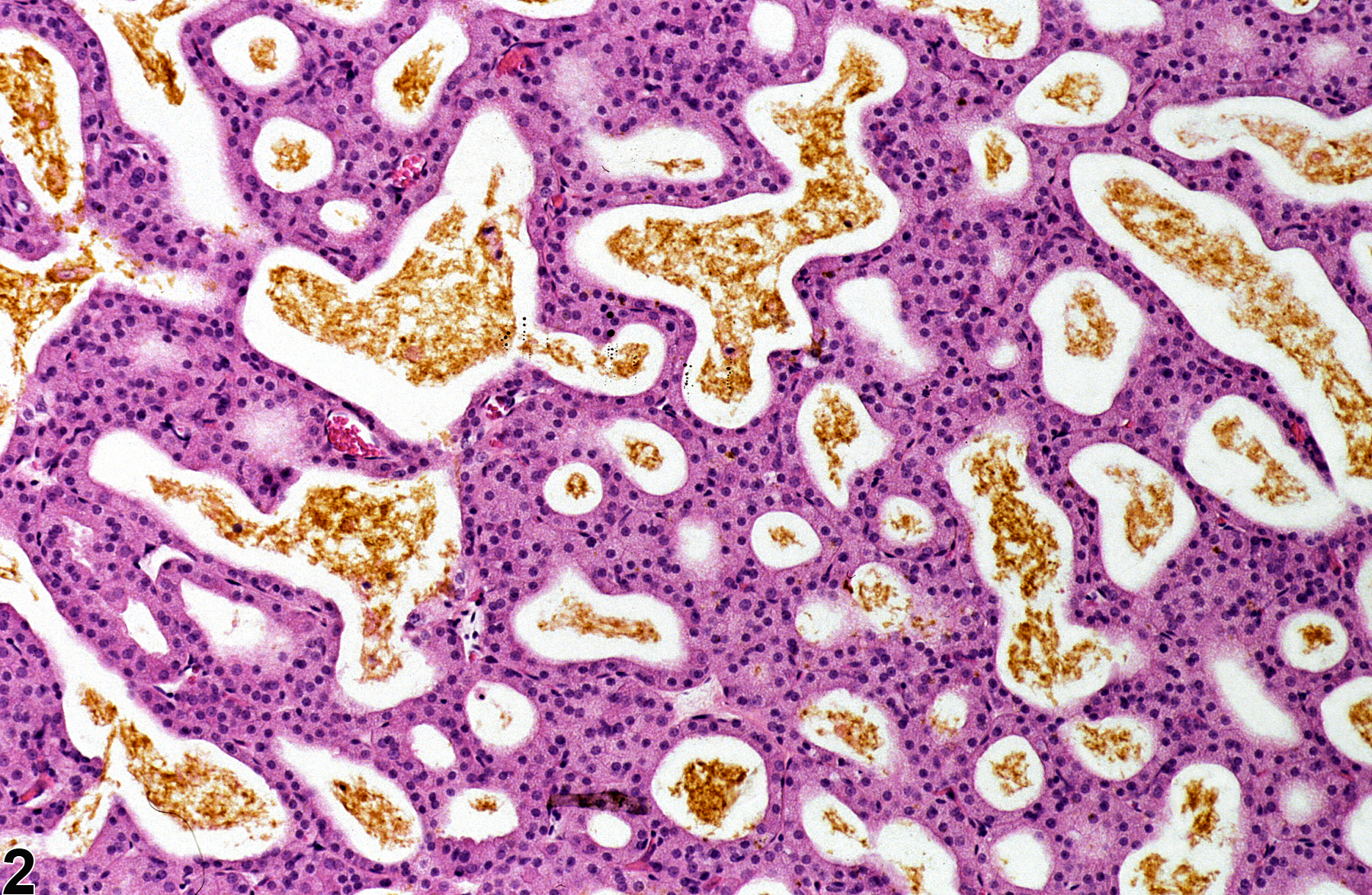
Harderian Gland - Pigment
Narrative
Beaumont SD. 2002. Ocular disorders of pet mice and rats. Vet Clin Exot Anim 5:311-324.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/12170635Botts S, Jokinen M, Gaillard ET, Elwell MR, Mann PC. 1999. Salivary, Harderian, and lacrimal glands. In: Pathology of the Mouse: Reference and Atlas (Maronpot RR, Boorman GA, Gaul BW, eds). Cache River Press, Vienna, IL, 49-79.
Brownscheidle CM, Niewenhuis RJ. 1978. Ultrastructure of the Harderian gland in male albino rats. Anat Rec 190:735-754.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/637321Chieffi G, Chieffi Baccani G, Di Matteo L, D’Istria M, Minucci S, Varriale B. 1996. Cell biology of the Harderian gland. Int Rev Cytol 168:1-180.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/8843648Djeridane Y. 1994. The Harderian gland and its excretory duct in the Wistar rat. A histological and ultrastructural study. J Anat 184:553-566.
Abstract: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1259964/Greaves P. 2007. Nervous system and special sense organs. In: Histopathology of Preclinical Toxicity Studies: Interpretation and Relevance in Drug Safety Evaluation, 3rd ed. Academic Press, San Diego, CA, 861-933.
Abstract: http://www.sciencedirect.com/science/book/9780444527714Iwai H, Tagawa Y, Hayasaka I, Hayasaka I, Yanai T, Masegi T. 2000. Effects of atropine sulfate on rat Harderian glands: Correlation between morphological changes and porphyrin levels. J Toxicol Sci 25:151-159.
Abstract: http://europepmc.org/abstract/MED/10987121Krinke GJ, Schaetti PR, Krinke A. 1996. Nonneoplastic and neoplastic changes in the Harderian and lacrimal glands. In: Pathobiology of the Aging Mouse, Vol 2 (Mohr U, Dungworth DL, Capen CC, Carlton WW, Sundberg JP, Ward JM, eds). International Life Sciences Institute Press, Washington, DC, 139-152.
Payne AP. 1994. The Harderian gland: A tercentennial review. J Anat 185:1-49.
Abstract: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1166813/Percy DH, Wojcinski ZW, Schunk MK. 1989. Sequential changes in the Harderian and exorbital lacrimal glands in Wistar rats infected with sialodacryoadenitis virus. Vet Pathol 26:238–245.
Full Text: http://vet.sagepub.com/content/26/3/238.full.pdfSakai T. 1981. The mammalian Harderian gland: Morphology, biochemistry, function, and phylogeny. Arch Histol Jpn 44:299-333.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/7030263Seely JC. 1987. The Harderian gland. Lab Anim 16:33-39.
Watanabe M. 1980. An autoradiographic, biochemical, and morphological study of the Harderian gland of the mouse. J Morphol 163:349-365.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/6990006Williams DL. 2002. Ocular disease in rats: A review. Vet Ophthalmol 5:183-192.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/12236869Yoshitomi K, Boorman GA. 1990. Eye and associated glands. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman GA, Eustis SL, Elwell MR, Montgomery CA, MacKenzie WF, eds). Academic Press, San Diego, CA, 239-260.
Abstract: https://www.ncbi.nlm.nih.gov/nlmcatalog/9002563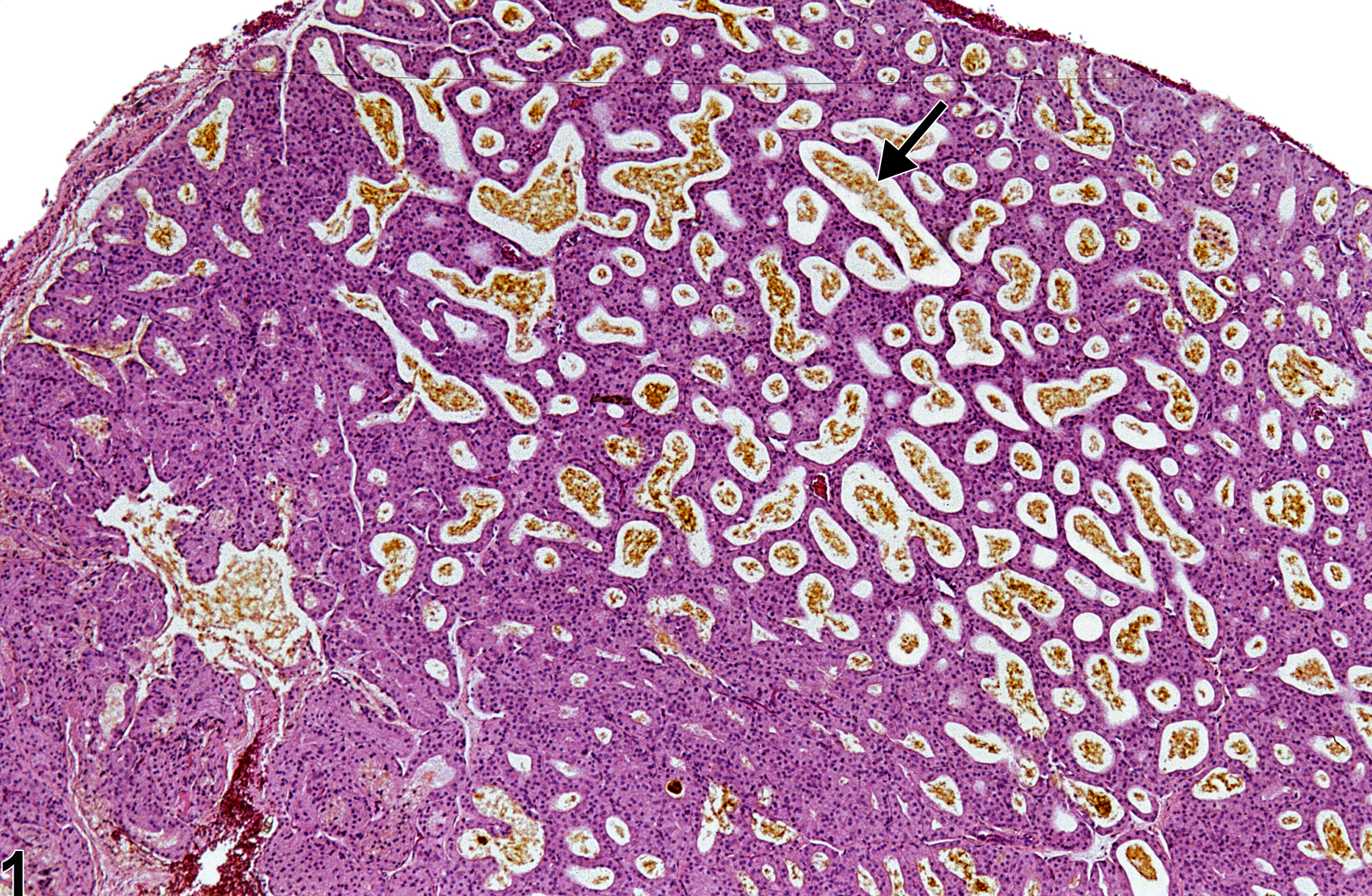
Harderian gland - Pigment in a female F344/N rat from a subchronic study. There are golden to dark brown amorphous clumps or laminated concretions of pigment (likely porphyrin) in the acinar lumens (arrow).