Special Senses System
Lacrimal Gland - Atrophy
Narrative
Botts S, Jokinen M, Gaillard ET, Elwell MR, Mann PC. 1999. Salivary, Harderian, and lacrimal glands. In: Pathology of the Mouse: Reference and Atlas (Maronpot RR, Boorman GA, Gaul BW, eds). Cache River Press, Vienna, IL, 49-79.
Abstract: http://www.cacheriverpress.com/books/pathmouse.htmHassan AS, Clouthier SG, Ferrara JL, Stepan A, Mian SI, Ahmad AZ, Elner VM. 2005. Lacrimal gland involvement in graft-versus-host disease: A murine model. Invest Ophthalmol Vis Sci 46:2692-2697.
Abstract: https://pubmed.ncbi.nlm.nih.gov/16043840/Kojima T, Wakamatsu TS, Dogru M, Ogawa Y, Igarishi A, Ibrahim OMA, Inaba T, Shimizu T, Noda S, Obata H, Nakmura S, Wakmatsu A, Shirasawa T, Simazaki J, Negishi K, Tsubota K. 2012. Age-related dysfunction of the lacrimal gland and oxidative stress: Evidence from the Cu,Zn,-superoxide dismutase (Sod1) knockout mice. Am J Pathol 180:1879-1896.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/22440255Lui SH, Prendergast RA, Silverstein AM. 1987. Experimental autoimmune dacryoadenitis. I. Lacrimal disease in the rat. Invest Ophthalmol Vis Sci 28:270–275.
Abstract: https://pubmed.ncbi.nlm.nih.gov/8591907/McCartney-Francis NL, Mizel DE, Frazier-Johnson M, Kulkami AB, McCarthy JB, Wahl SM. 1997. Lacrimal gland inflammation is responsible for ocular pathology in TGF-β1 null mice. Am J Pathol 151:1281-1288.
Abstract: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1858095/National Toxicology Program. 1999. NTP TR-488. Toxicology and Carcinogenesis Studies of 60-HZ Magnetic Fields in F344/N Rats and B6C3F1 Mice (Whole-Body Exposure Studies). NTP, Research Triangle Park, NC.
Abstract: https://ntp.niehs.nih.gov/go/10166Rios JD, Horikawa Y, Chan L-L, Kubin CL, Hodges RR, Dartt DA, Zoukhri D. 2005. Age-dependent alterations in mouse exorbital lacrimal gland structure, innervation and secretory response. Exp Eye Res 80:477-491.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/15781275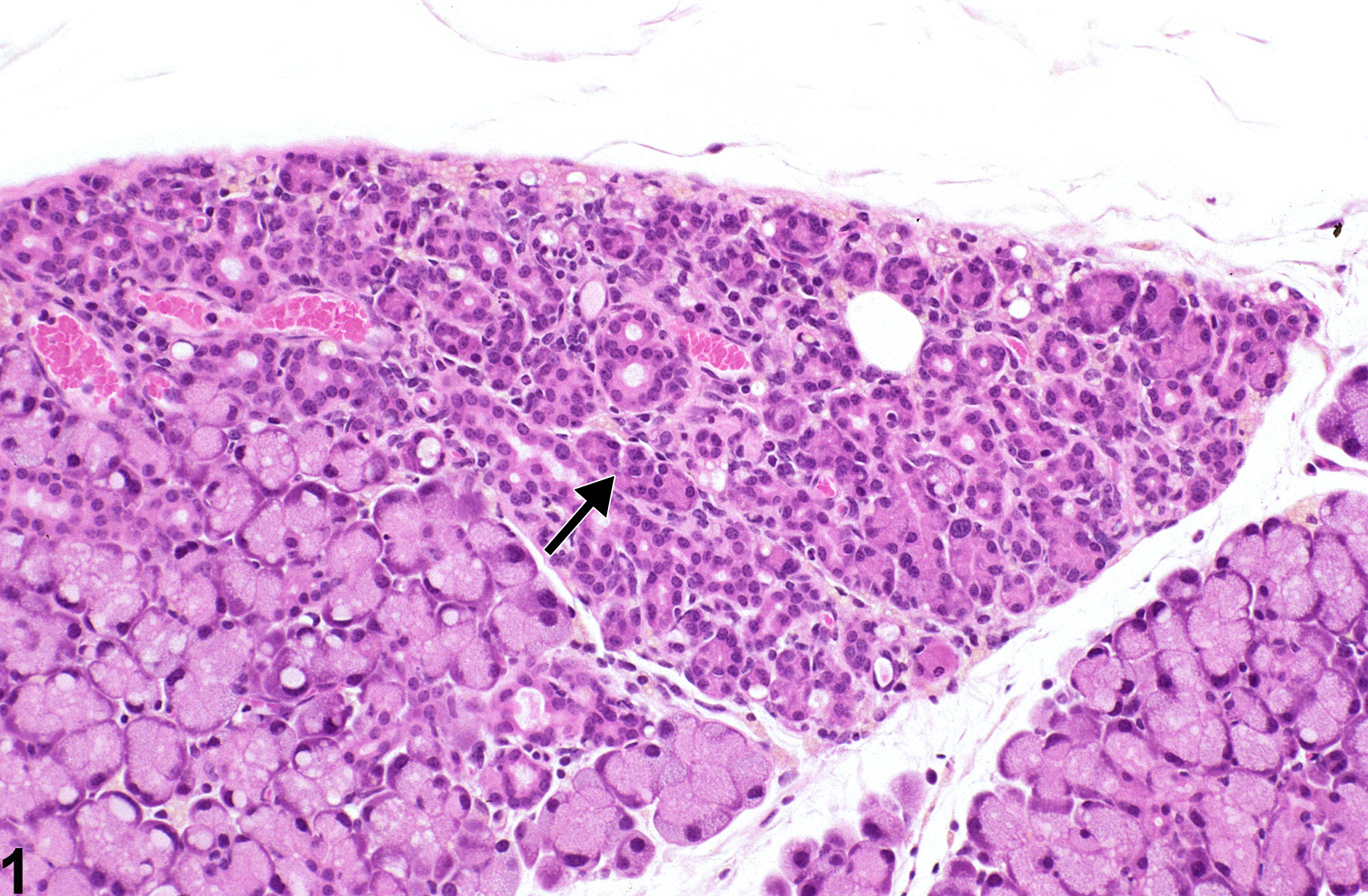
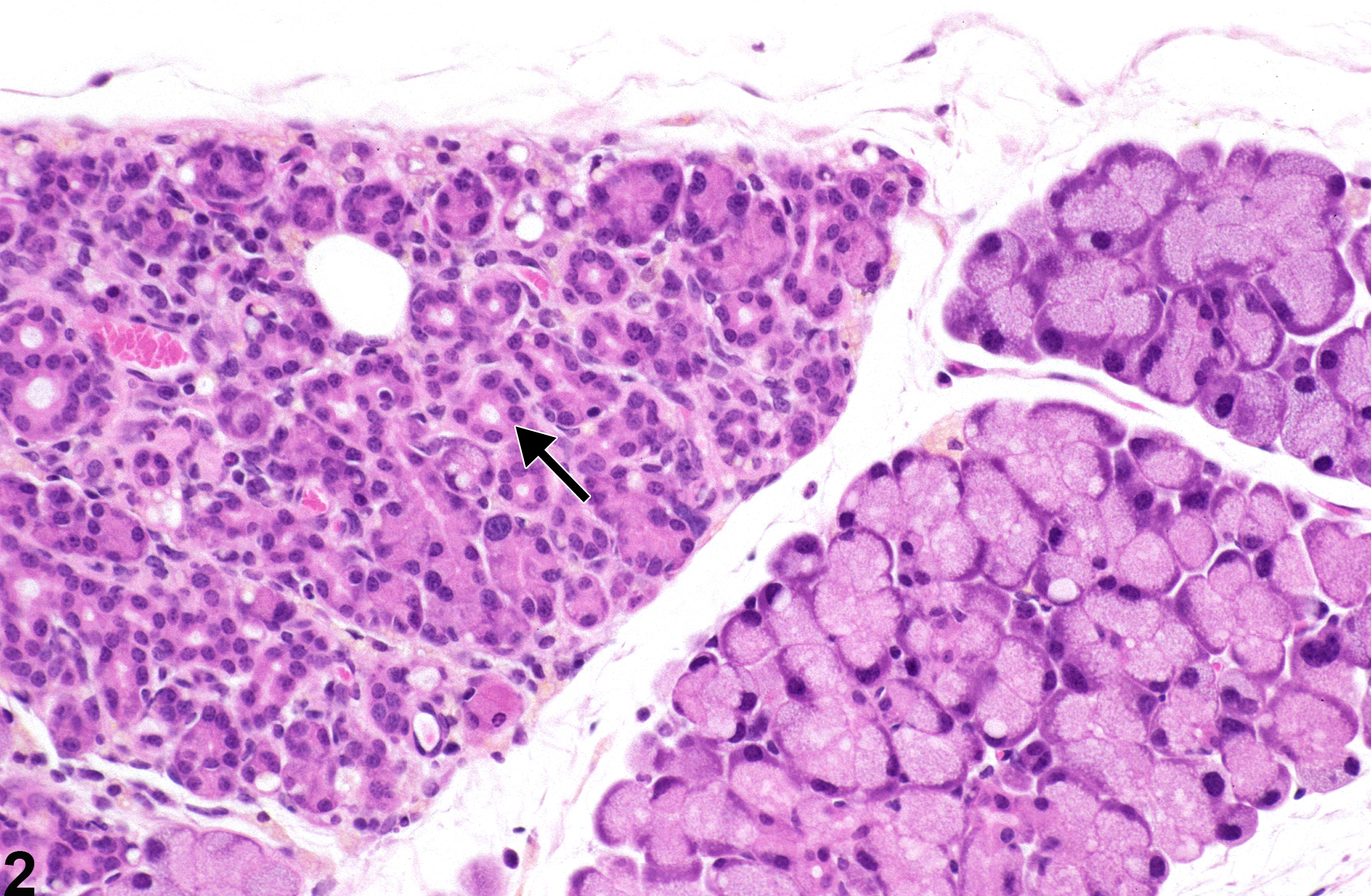
Lacrimal gland - Atrophy in a male B6C3F1 mouse from a chronic study. Atrophy (arrow) is characterized by a focus of shrunken acini lined by small, low cuboidal to flattened cells with increased fibrous stroma.