Urinary System
Kidney - Inflammation
Narrative
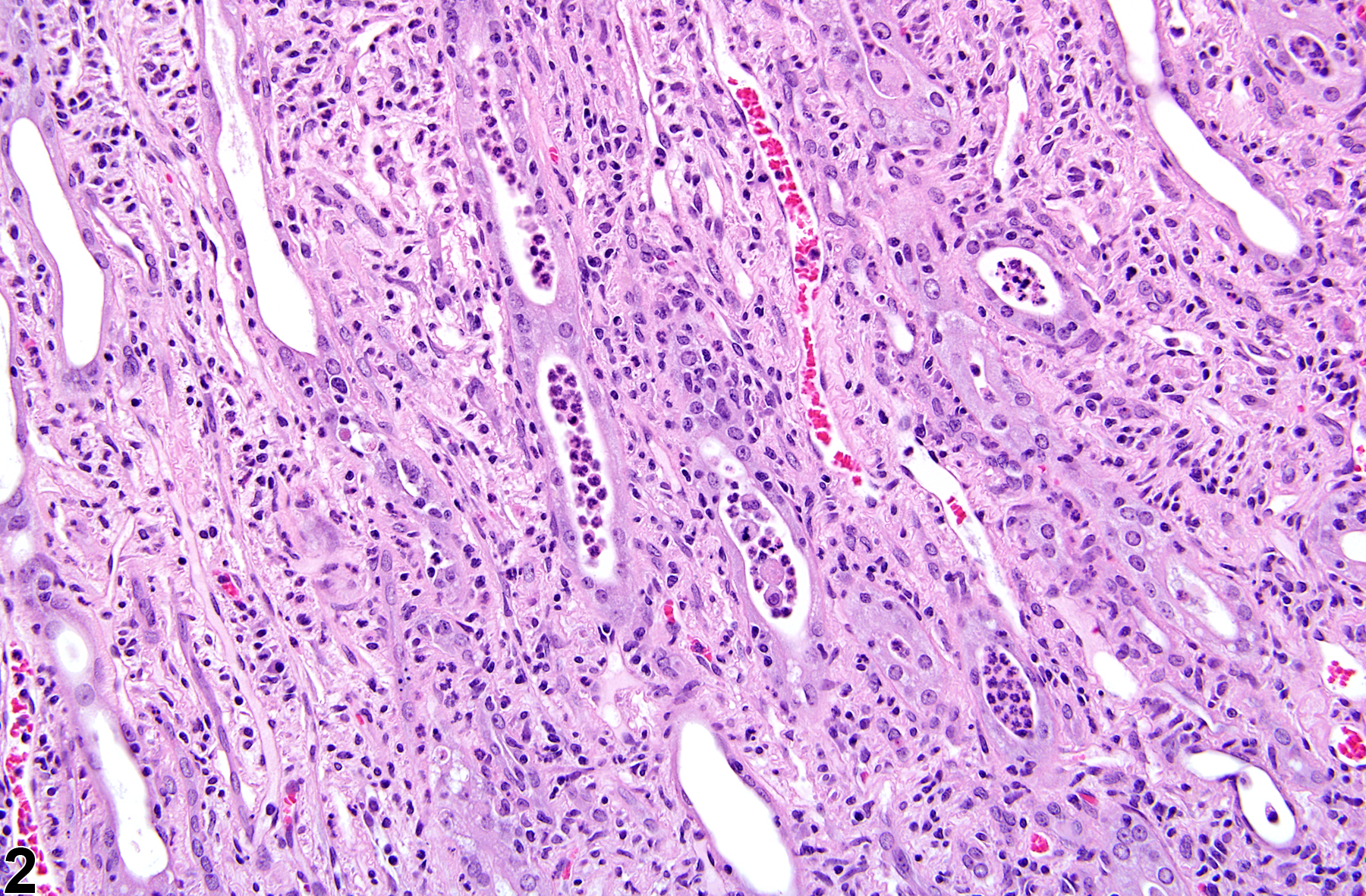
Renal tubule inflammation (tubulitis) (Figure 1 and Figure 2) may be associated with a number of causes that may include the deposition of crystals, extension from the lower urinary tract (pyelonephritis), infectious processes, chronic progressive nephropathy, previous infarction, or direct chemical administration. Tubule inflammation is characterized by the presence of inflammatory cells within the tubule lumen, epithelium, or both.
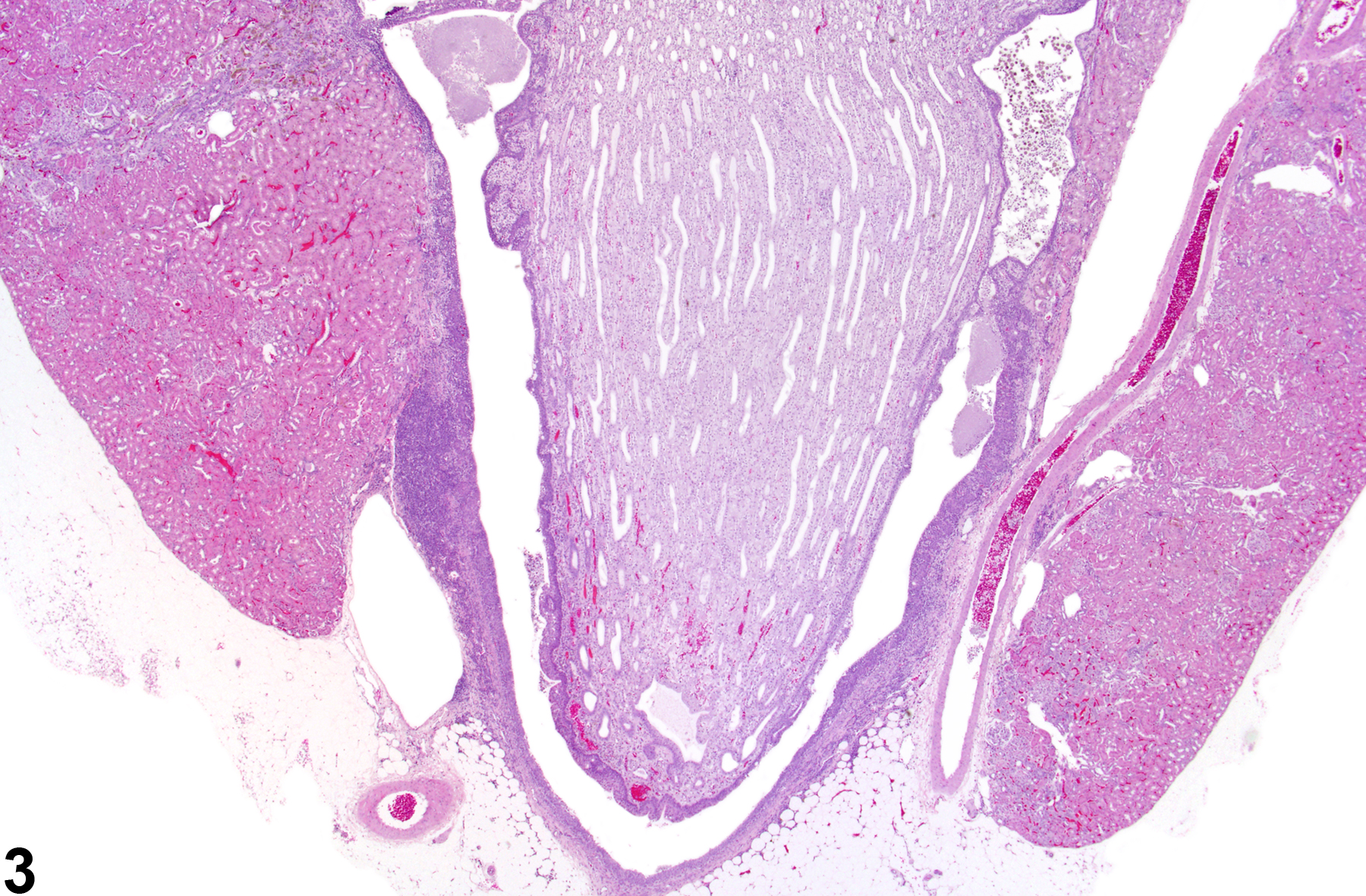
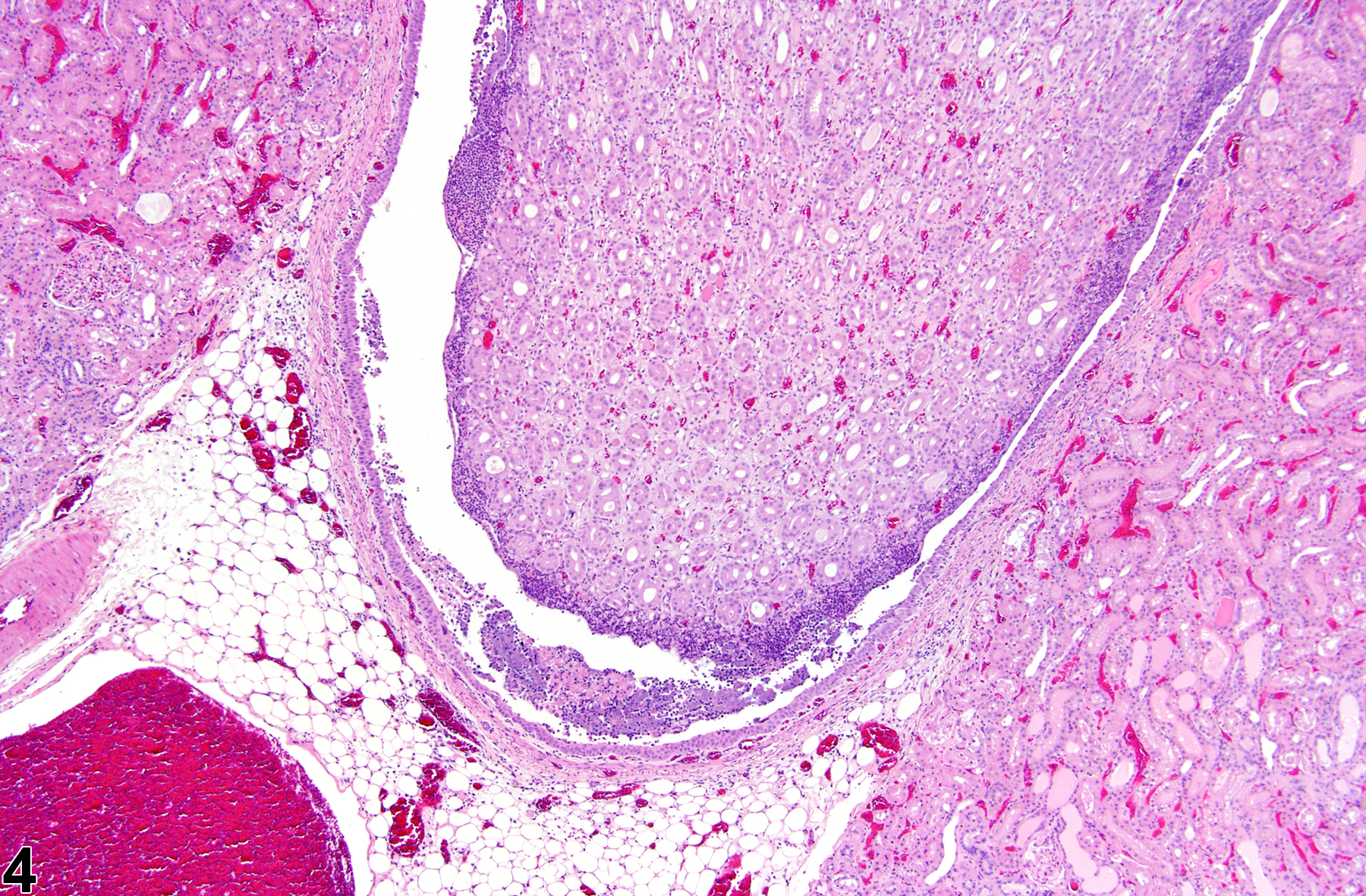
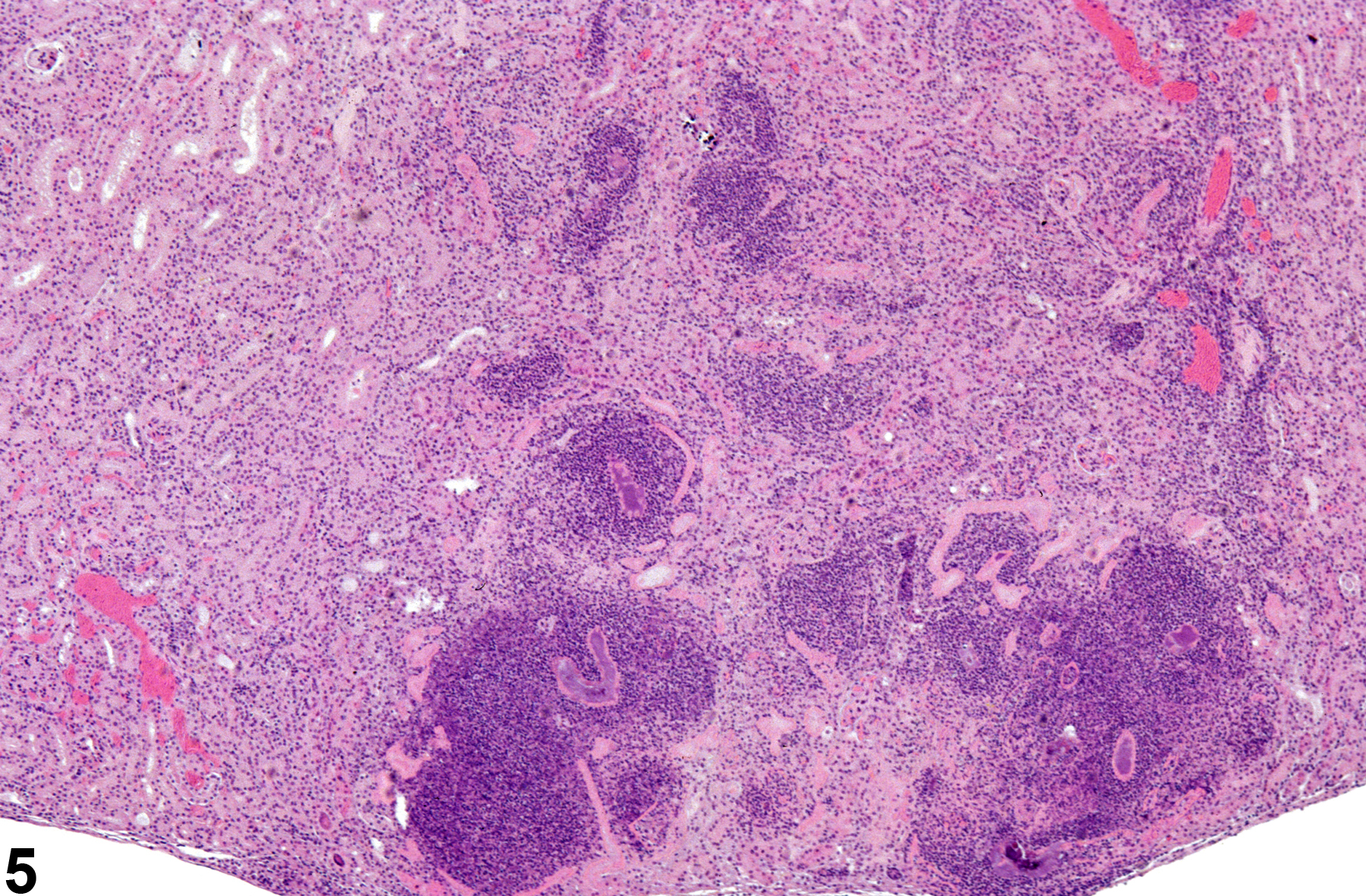
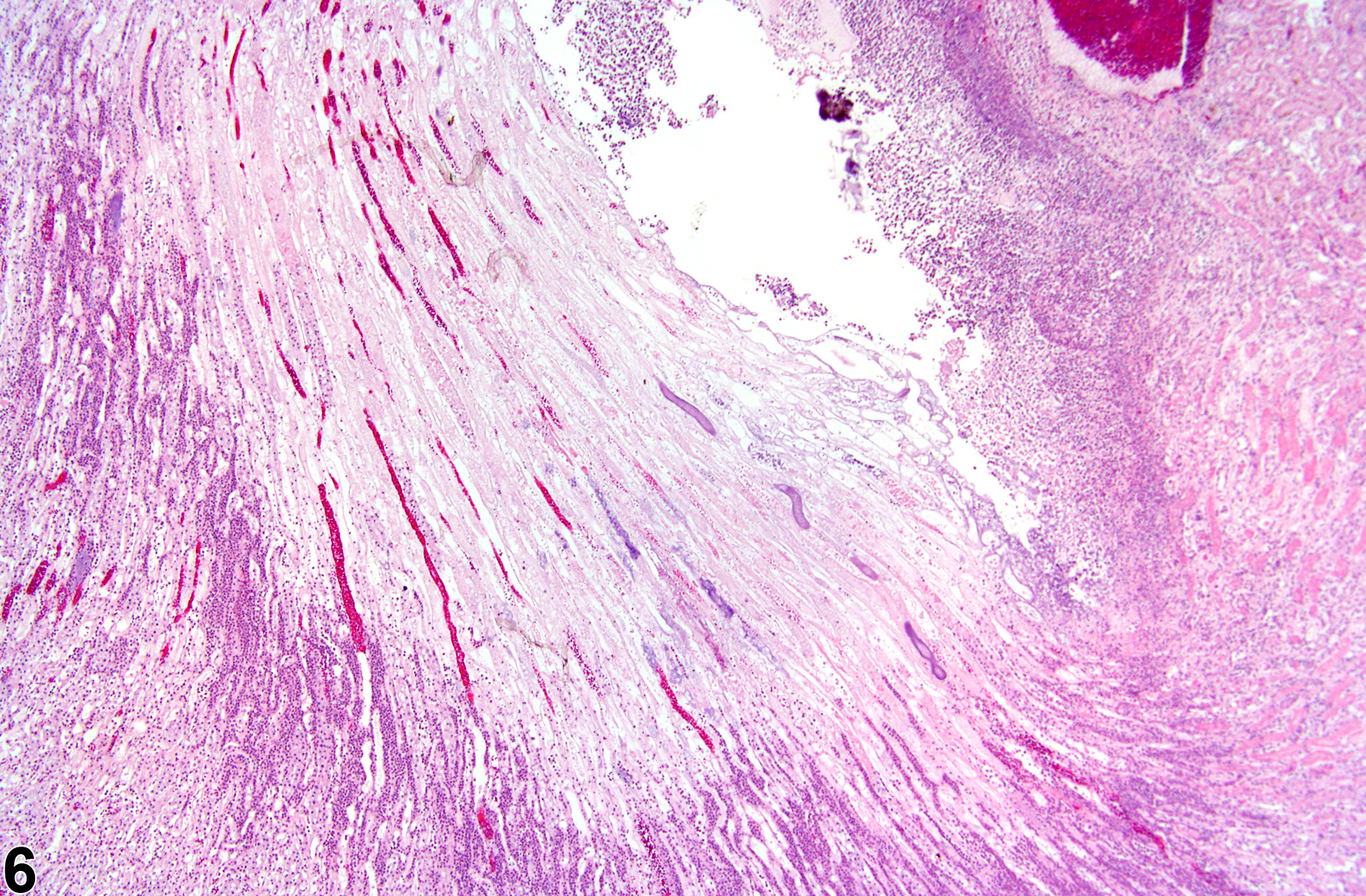
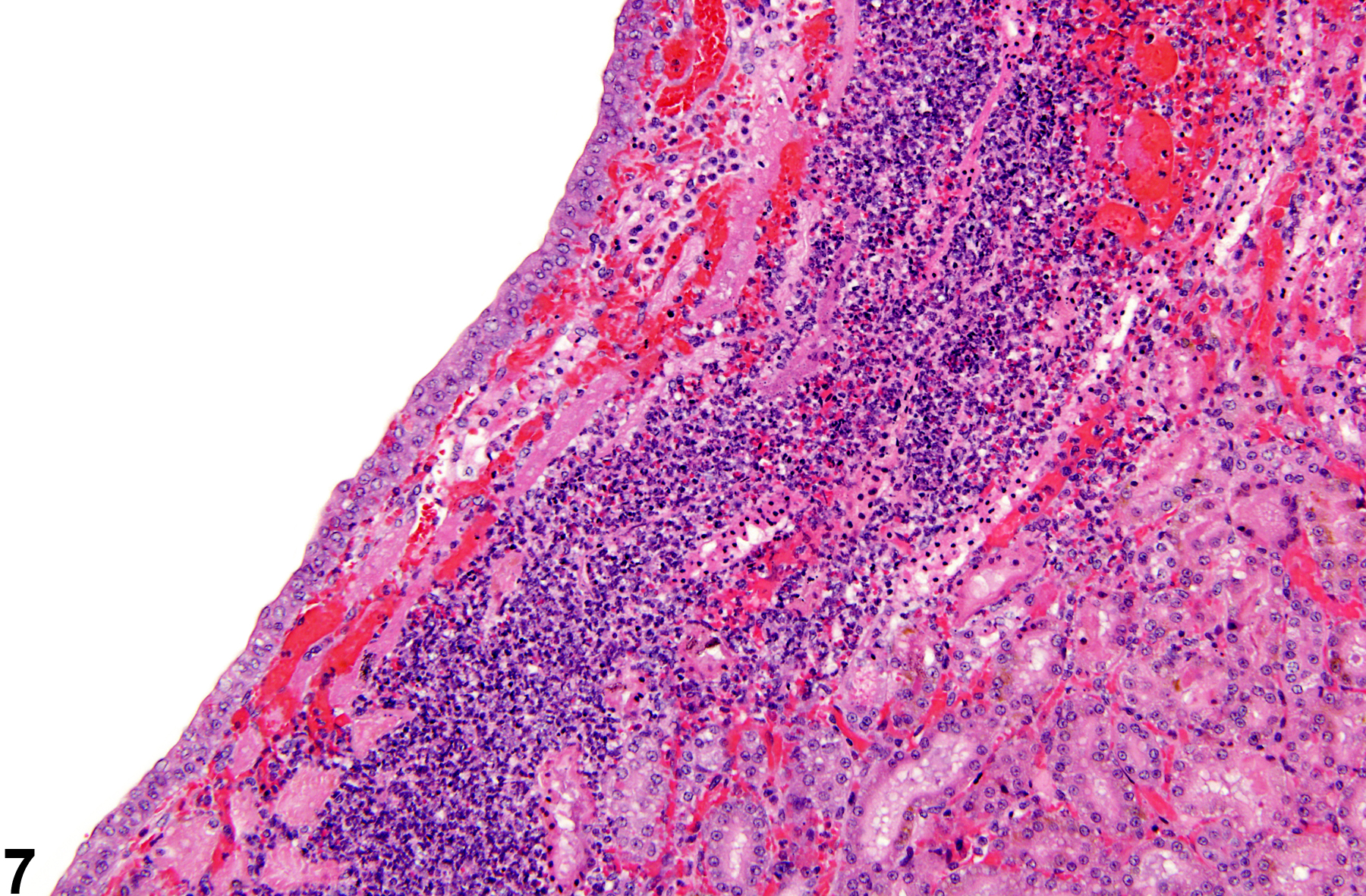
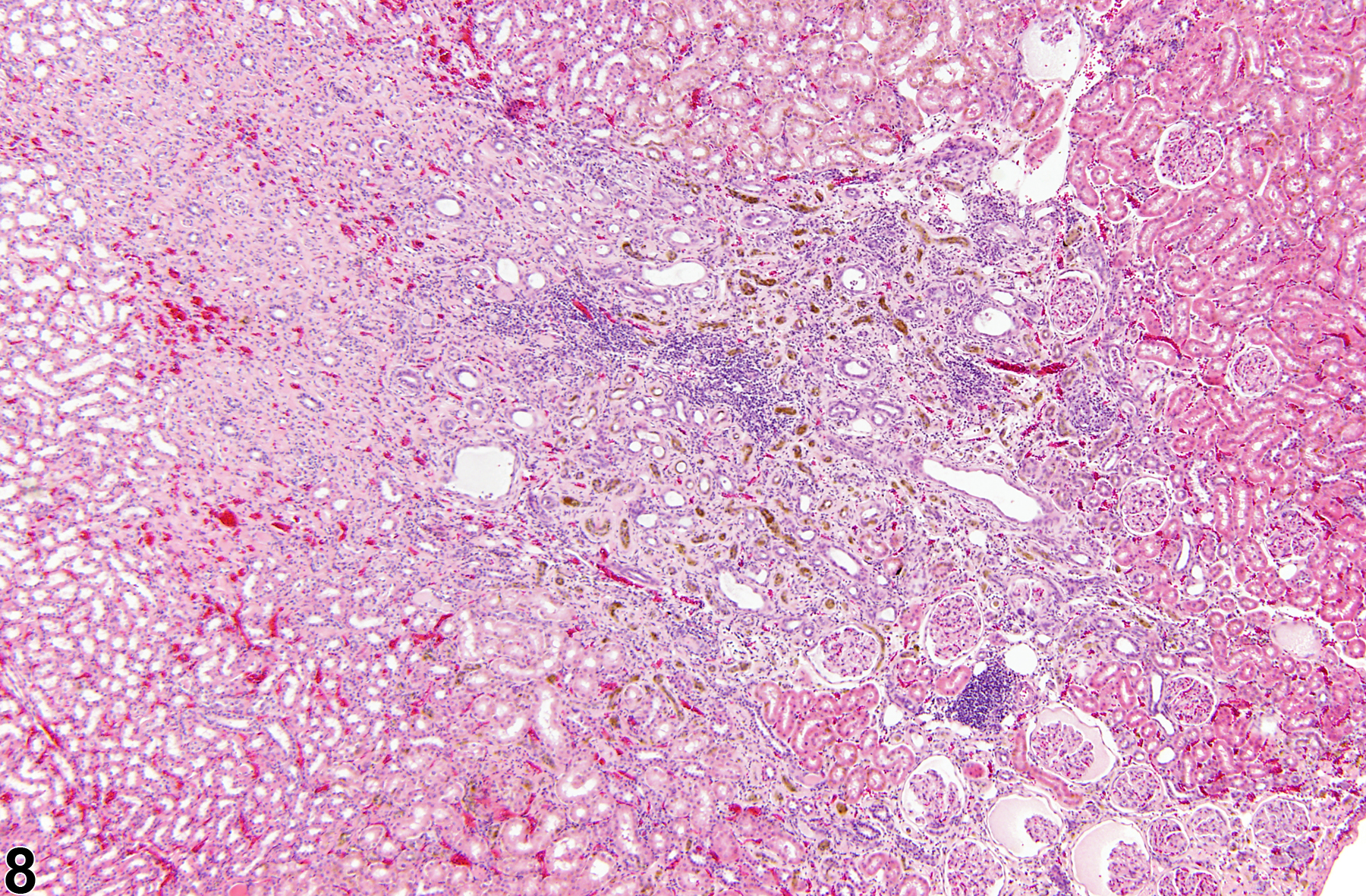
Inflammation can also be localized to the renal pelvis (Figure 3, Figure 4, Figure 5, and Figure 6) or the interstitium (Figure 7 and Figure 8). Renal pelvis inflammation usually arises from conditions related to localized infections, which ascend from the lower urinary tract and extend into the renal papilla, medulla, and cortex. However, renal pelvis inflammation without lower urinary tract involvement may also be seen. There may be a number of causes for inflammation. Renal pelvis inflammation typically is acute or suppurative, with more chronic lesions noted in peripelvic tissues. Another diagnostic term occasionally used by pathologists to describe a similar condition is "pyelonephritis," which emphasizes renal involvement along with pelvis inflammation. Microabscesses may be noted in marked cases, due to either an ascending infection or a coinciding septicemic infection. Renal papillary ulceration and/or necrosis may occur as a result of renal pelvis inflammation. Reactive urothelial and/or papillary epithelial hyperplasia are often noted in more chronic cases. Interstitial inflammation, a cellular reaction to tissue injury from a variety of causes, may be observed frequently in the kidney of rodents. Chronic interstitial inflammation is often seen as a component of chronic progressive nephropathy (see ).
Cattell V, Jennette JC. 1998. Mechanisms of acute inflammatory and immunologic renal injury. In: Heptistall’s Pathology of the Kidney (Jennette JC, Olson JL, Schwartz MM, Silva FG, eds). Lippincott-Raven, Philadelphia, 85-136.
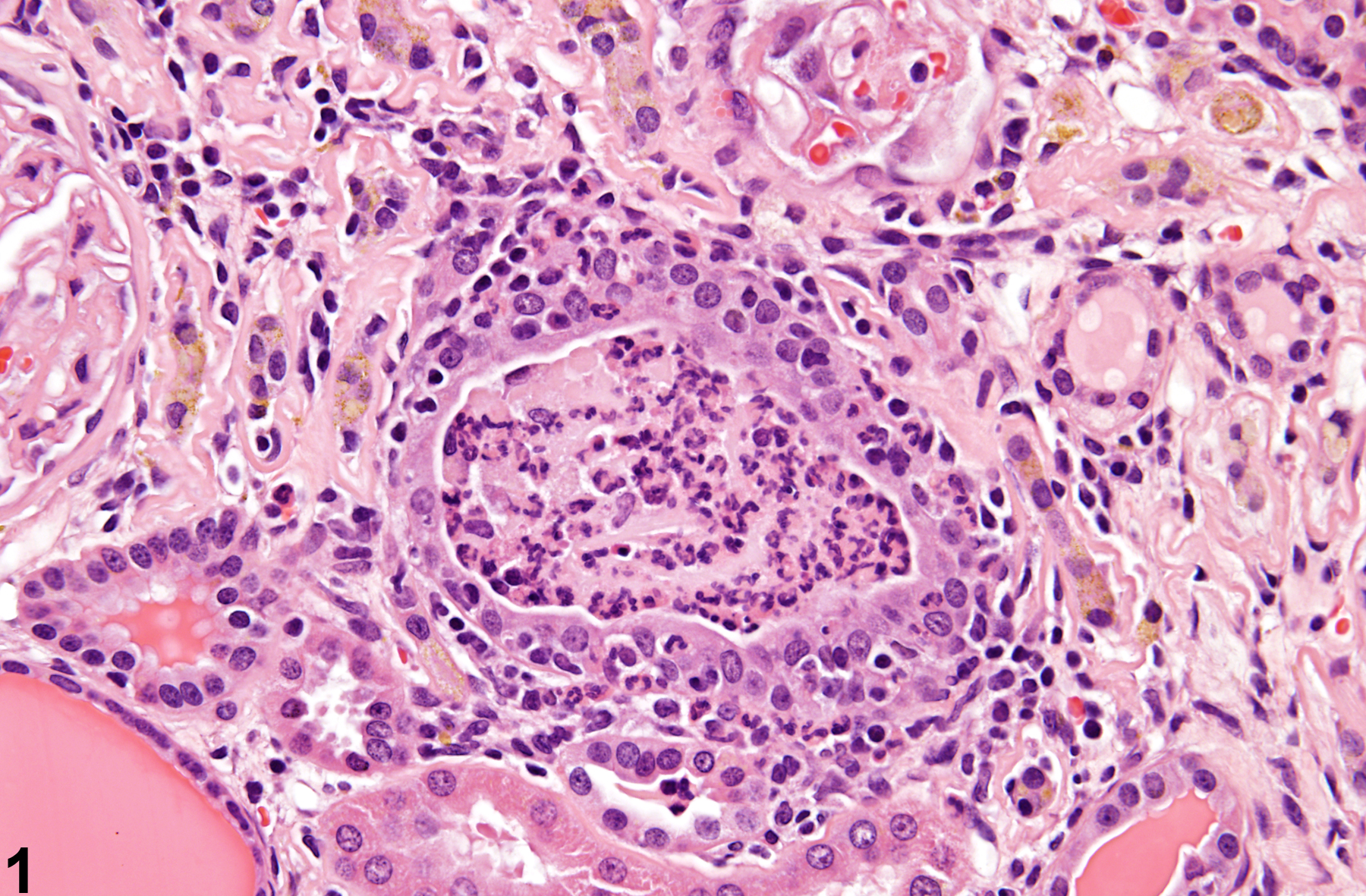
Kidney, Renal tubule - Inflammation, Acute in a male F344/N rat from a chronic study. Acute inflammatory cells are present in the renal tubule.