Urinary System
Renal Tubule - Atypical Tubule Hyperplasia
Narrative
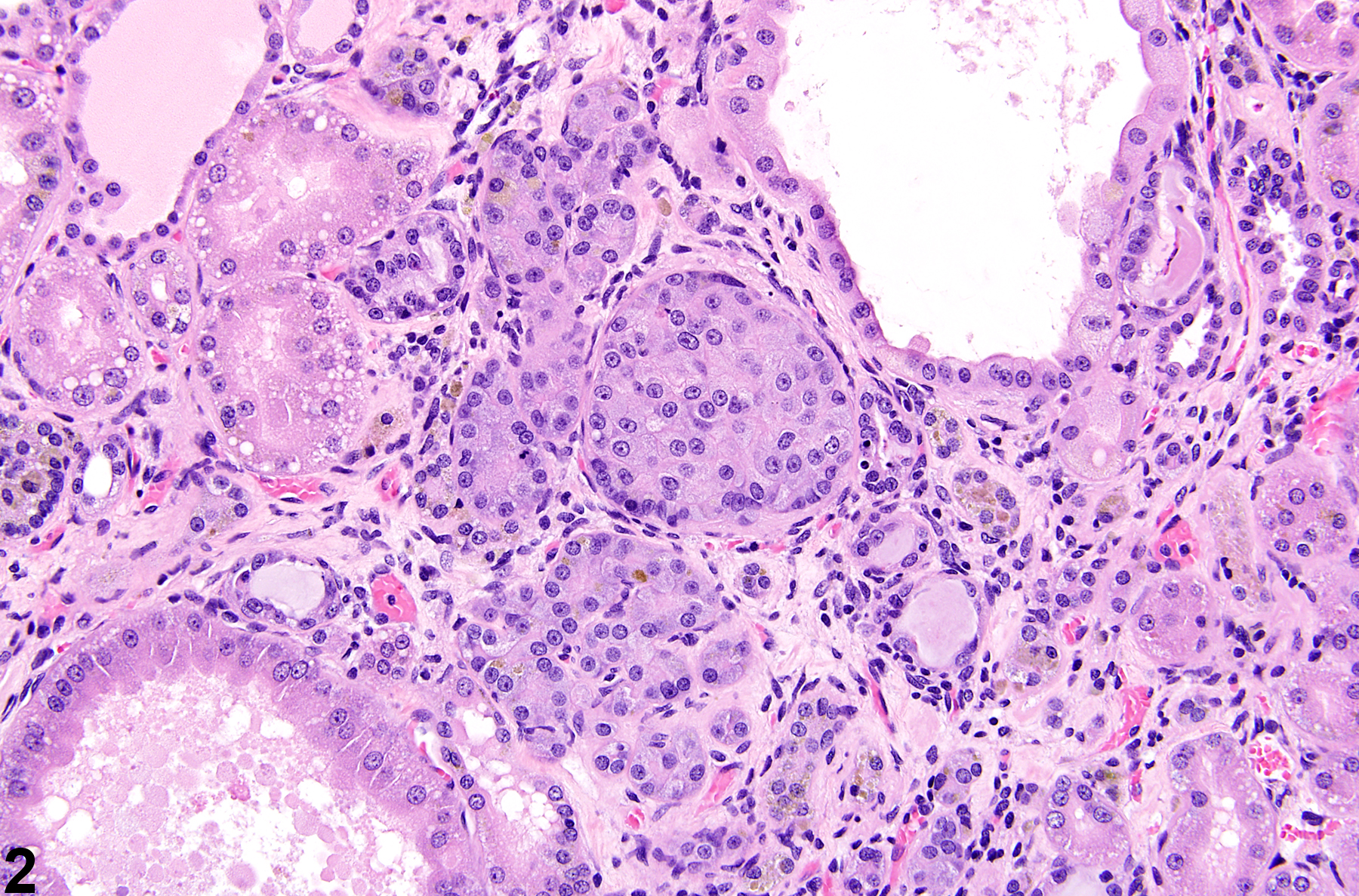
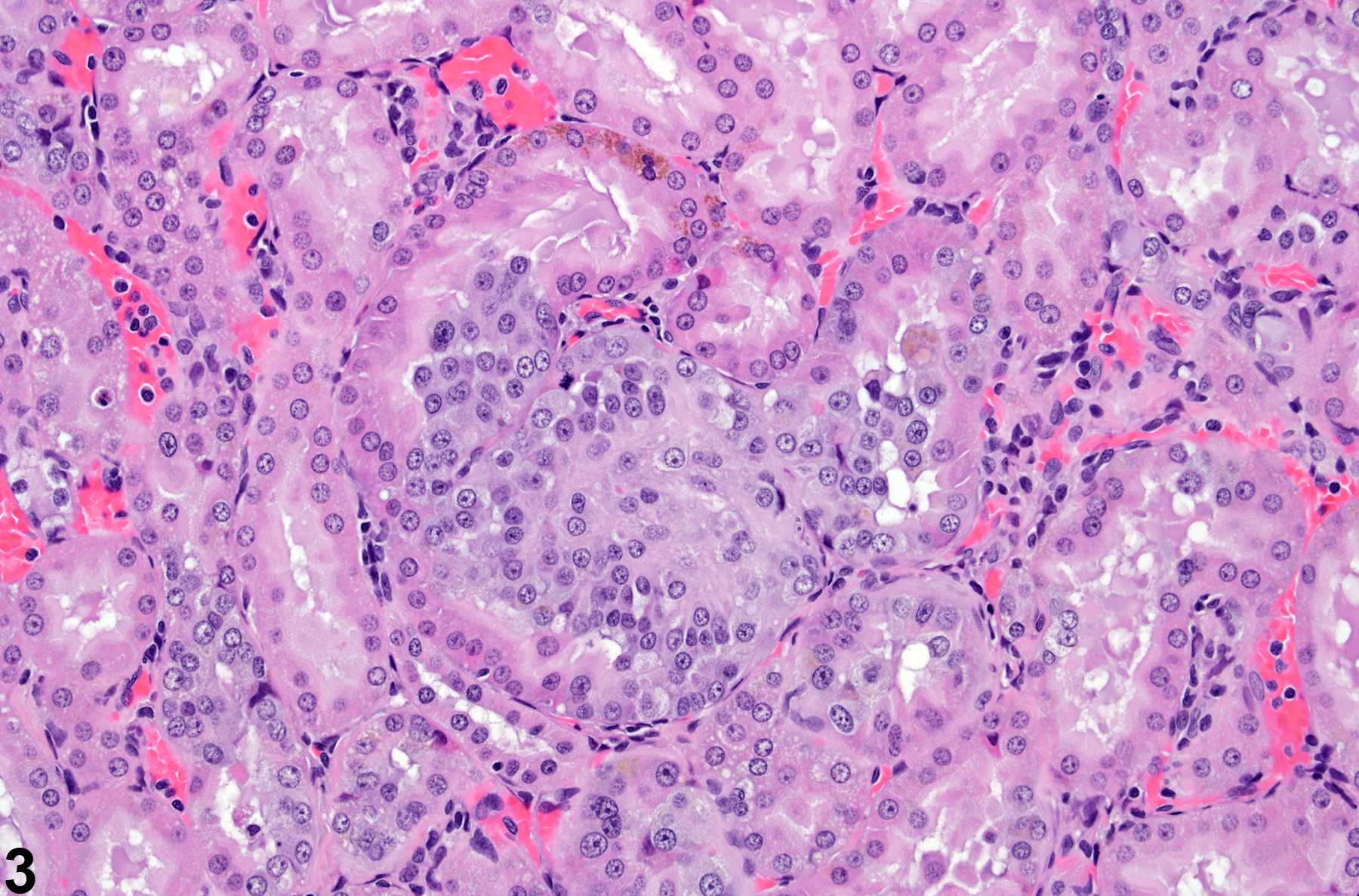
ATH is characterized by an increased number of epithelial cells within the confines of a single tubule, as opposed to an adenoma, in which the proliferating cells are no longer within the confines of a single tubule. The proliferative lining epithelium in ATH is greater than two or three cell layers. Hyperplastic cells appear enlarged with a slightly basophilic “glassy” cytoplasmic sheen. Variable degrees of cytoplasmic and nuclear pleomorphism may be present. Evidence of lesion expansion is identified by fibroblast flattening and margination around the lesion. Neovascularization noted in renal tubule adenomas is not apparent in ATH.
ATH should not be confused with tubule hyperplasia, which is often observed in foci of advanced chronic progressive nephropathy (see ) and characterized as a tubule lined by a single layer of increased numbers of epithelial cells. This form of tubule hyperplasia is rarely induced by chemical administration and is considered to represent a form of regeneration.
Frazier KS, Seely JC, Hard GC, Betton G, Burnett R, Nakatsuji S, Nishikawa A, Durchfeld-Meyer B, Bube A. 2012. Proliferative and non-proliferative lesions in the rat and mouse urinary system. Toxicol Pathol 40:14S-86S.
Abstract: http://www.ncbi.nlm.nih.gov/pubmed/22637735Greaves P. 2012. Histopathology of Preclinical Toxicity Studies, 4th ed. Elsevier, Amsterdam, 569-571.
Abstract: http://www.sciencedirect.com/science/book/9780444538567Hard GC, Seely JC. 2005. Recommendations for the interpretation of renal tubule proliferative lesions occurring in rat kidneys with advanced chronic progressive nephropathy (CPN). Toxicol Pathol 33:641-649.
Abstract: http://www.ncbi.nlm.nih.gov/pubmed/16207638Hard GC, Seely JC. 2006. Histological investigation of diagnostically challenging tubule profiles in advanced chronic progressive nephropathy (CPN) in the Fischer 344 rat. Toxicol Pathol 34:941-948.
Abstract: http://www.ncbi.nlm.nih.gov/pubmed/17178694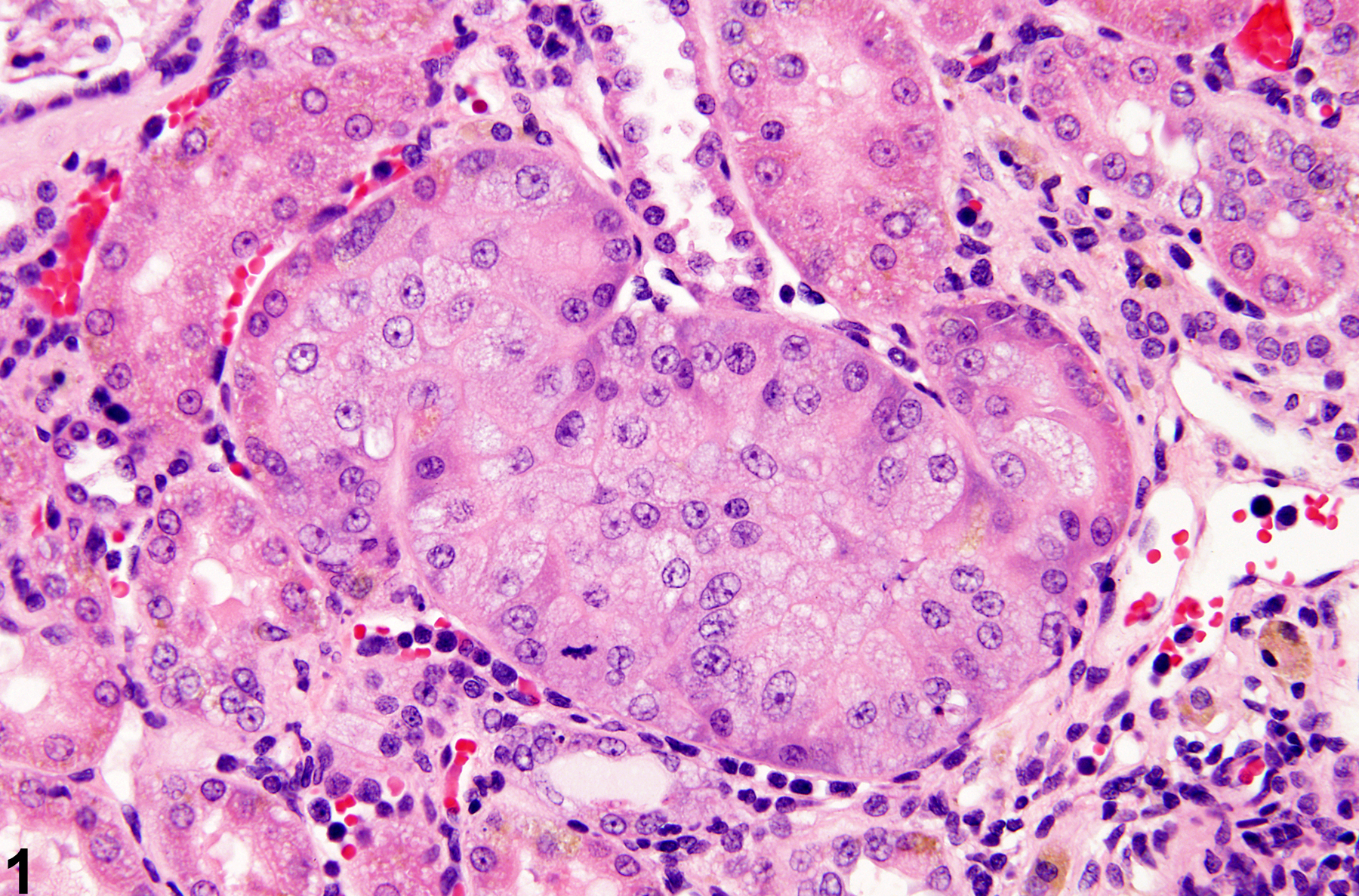
Kidney, Renal tubule - Atypical tubule hyperplasia in a male F344/N rat from a chronic study. Atypical tubule hyperplasia is confined to one tubule and is characterized by an increase in cellularity and cell size, cytoplasmic basophilia, nuclear enlargement, and circumferential expansion.