Reproductive System, Male
Testis
Narrative
General
The male reproductive system tissues include testes, epididymides, the various accessory sex glands, and the penis. These tissues exhibit direct and indirect (usually hormonal) pleotrophic pathologic responses, often with a change in one reproductive tissue accompanied by changes in other reproductive tissues. The majority of the male reproductive tissues are paired, allowing identification of unilateral versus bilateral responses. Artifacts are rare and typically reflect the use of less than ideal fixatives for testes (modified Davidson’s fixative is preferred) or physical damage, including drying out of tissues, during the weighing process prior to fixation.
Evaluation of male reproductive system tissues should be correlated with wet tissue weights when possible. Substantial changes in weight, particularly for testes and for the combined seminal vesicle and coagulating gland weights, will typically have a morphologic counterpart that should be documented. Prostate weights, particularly specific prostate lobe weights, are dependent upon the consistency of gross dissection and are variable. Identification of morphologic changes in the whole prostate or in specific lobes that correlate with tissue weight changes can be challenging. During evaluation of paired tissues, documentation of unilateral versus bilateral changes may help in identifying a systemic response. As a general guideline for paired tissues, if both are involved the diagnosis should be qualified as bilateral and the severity grade based on the more severely affected tissue.
In evaluating the male reproductive system, if potential treatment-related increases in changes occur, they should be described in the pathology narrative and correlated with other potential lesions in reproductive and endocrine tissues. Secondary changes such as metaplasia, degeneration, or apoptosis that accompany a primary lesion are usually not diagnosed unless warranted by virtue of their severity.
A final general concern relates to a variety of spontaneous background changes in testes, epididymides, and accessory sex glands, many of which can be exacerbated by treatment. The amount, tinctorial properties, and physical features of prostatic acinar secretions, for example, change significantly as rodents age or become less sexually active. Consequently, a consistent severity-grading scheme should be used in documenting commonly occurring lesions in male reproductive tissues if treatment-related exacerbation of common background changes is suspected.
Evaluation of the Testes
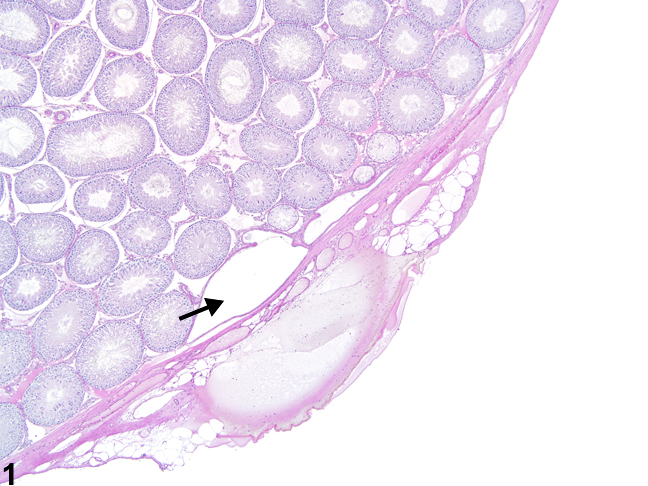
Figure 1. Testis, rete testis - normal. The rete testis is located at the hilus of the testis and appears as a dilated structure (arrow) beneath the testicular tunic in a male Sprague-Dawley rat from a multigeneration reproduction study. HPAS stain.
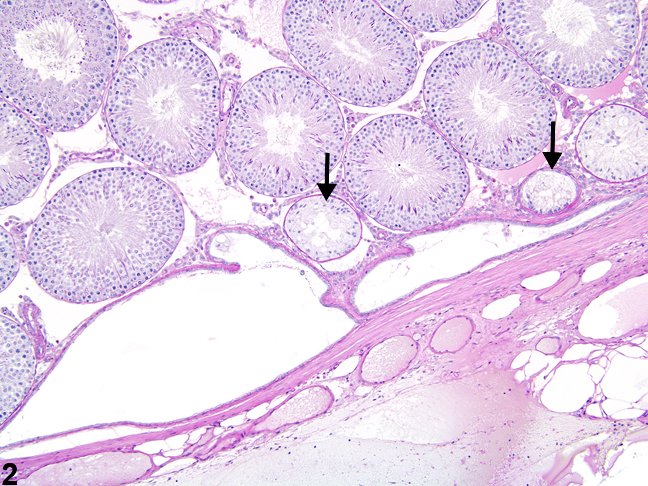
Figure 2. Testis, rete testis - normal. This higher magnification of Figure 1 shows the rete testis lined by low cuboidal epithelium in a male Sprague-Dawley rat from a multigeneration reproduction study. Adjacent seminiferous tubules may be lined only by Sertoli cells and should not be mistaken for focal seminiferous tubule atrophy (arrows). HPAS stain.
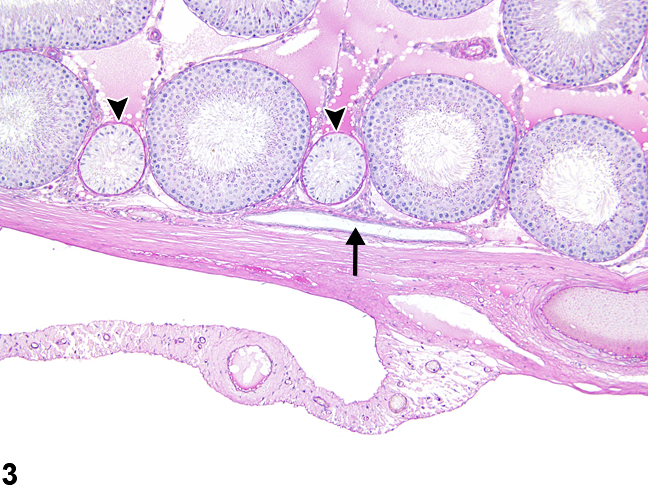
Figure 3. Rete testis - normal. The rete testis in this section is narrow and elongated (arrow) in a male Sprague-Dawley rat from a multigeneration reproduction study. Two adjacent seminiferous tubules (arrowheads) contain only Sertoli cells and should not be mistaken for focal seminiferous tubule atrophy. HPAS stain.
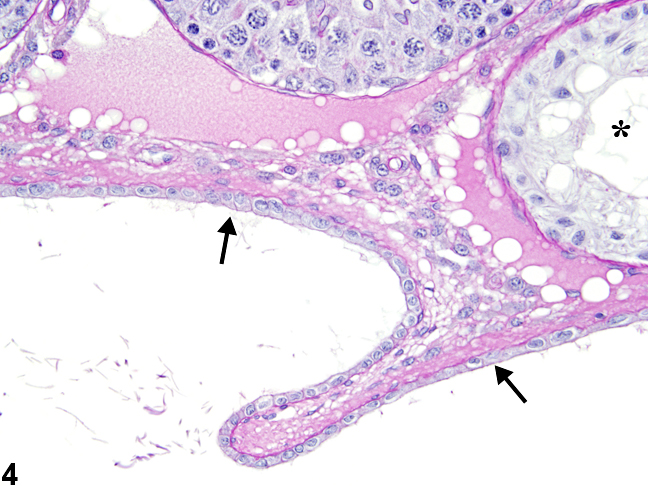
Figure 4. Testis, rete testis - normal. This high magnification shows the low cuboidal epithelium lining (arrows) of the rete testis from a male Sprague-Dawley rat in a multigeneration reproduction study. An adjacent seminiferous tubule, containing only Sertoli cells (asterisk), should not be mistaken for seminiferous tubule atrophy. HPAS stain.
In the absence of obvious changes such as cytoplasmic vacuolation, necrosis, apoptosis, and atrophy, stage-aware histopathologic assessment of the testes is recommended in general toxicity studies. This is a qualitative assessment intended to identify when germ cells in seminiferous tubules are missing or inappropriately present. Stage-aware histopathology does not involve counting the number of tubules in each stage but should include a high-magnification examination of 50-100 tubules representing early and late stages of the spermatogenic cycle. Abnormalities are recognized by missing cell populations, retained spermatids, and/or loss of an orderly pattern of cells in seminiferous tubules. Noting the presence and placement of both round and elongating spermatids in early stages of spermatogenesis (stages I-VIII in rat and mouse) and a single layer of elongated spermatids in late stages of seminiferous tubules (stages IX-XIV in rat and IX-XII in mouse) may be helpful in stage-aware histopathologic evaluation of rat testes. Of course, spermatocytes should be present in all stages of seminiferous tubules. Normal features for stage-aware histopathologic assessment of testes are summarized as follows:
| Stages I-VIII (rat and mouse) | Stages IX-XIV (rat) and IX-XII (mouse) |
|---|---|
| Round spermatids | Elongating spermatids |
| Elongated spermatids | Pachytene spermatocytes |
| Pachytene spermatocytes | Dividing spermatocytes |
| Spermatogonia |
The rete testis, located at the cranial pole of the rat testis, may be present in typical cross sections (Figure 1, Figure 2, Figure 3, Figure 4). The rete testis connects the seminiferous tubules to the efferent duct, and cross sections are lined by simple cuboidal to columnar epithelium (Figure 4). These should not be mistaken for abnormal seminiferous tubules. In addition, the seminiferous tubules immediately leading into the rete testis are normally lined only by Sertoli cells, and these should not be mistaken for focal seminiferous tubule degeneration or atrophy (Figure 2, Figure 3, and Figure 4).
Evaluation of the number and morphologic features of Leydig cells is also a part of the complete testis evaluation.
Creasy DM. 1997. Evaluation of testicular toxicity in safety evaluation studies: The appropriate use of spermatogenic staging. Toxicol Pathol 25:119-131.
Abstract: http://www.ncbi.nlm.nih.gov/pubmed/9125770Creasy DM. 2001. Pathogenesis of male reproductive toxicity. Toxicol Pathol 29:64-76.
Full Text: http://tpx.sagepub.com/content/29/1/64.full.pdfCreasy DM, Foster P. 1991. Male reproductive system. In: Handbook of Toxicologic Pathology (Haschek E, Rousseaux C, eds). Academic Press, New York, 829-889.
Abstract: http://www.sciencedirect.com/science/book/9780123302151Lanning LL, Creasy DM, Chapin RE, Mann PC, Barlow NJ, Regan KS, Goodman DG. 2002. Recommended approaches for the evaluation of testicular and epididymal toxicity. Toxicol Pathol 30:507-520.
Abstract: http://www.ncbi.nlm.nih.gov/pubmed/12187942
