Alimentary System
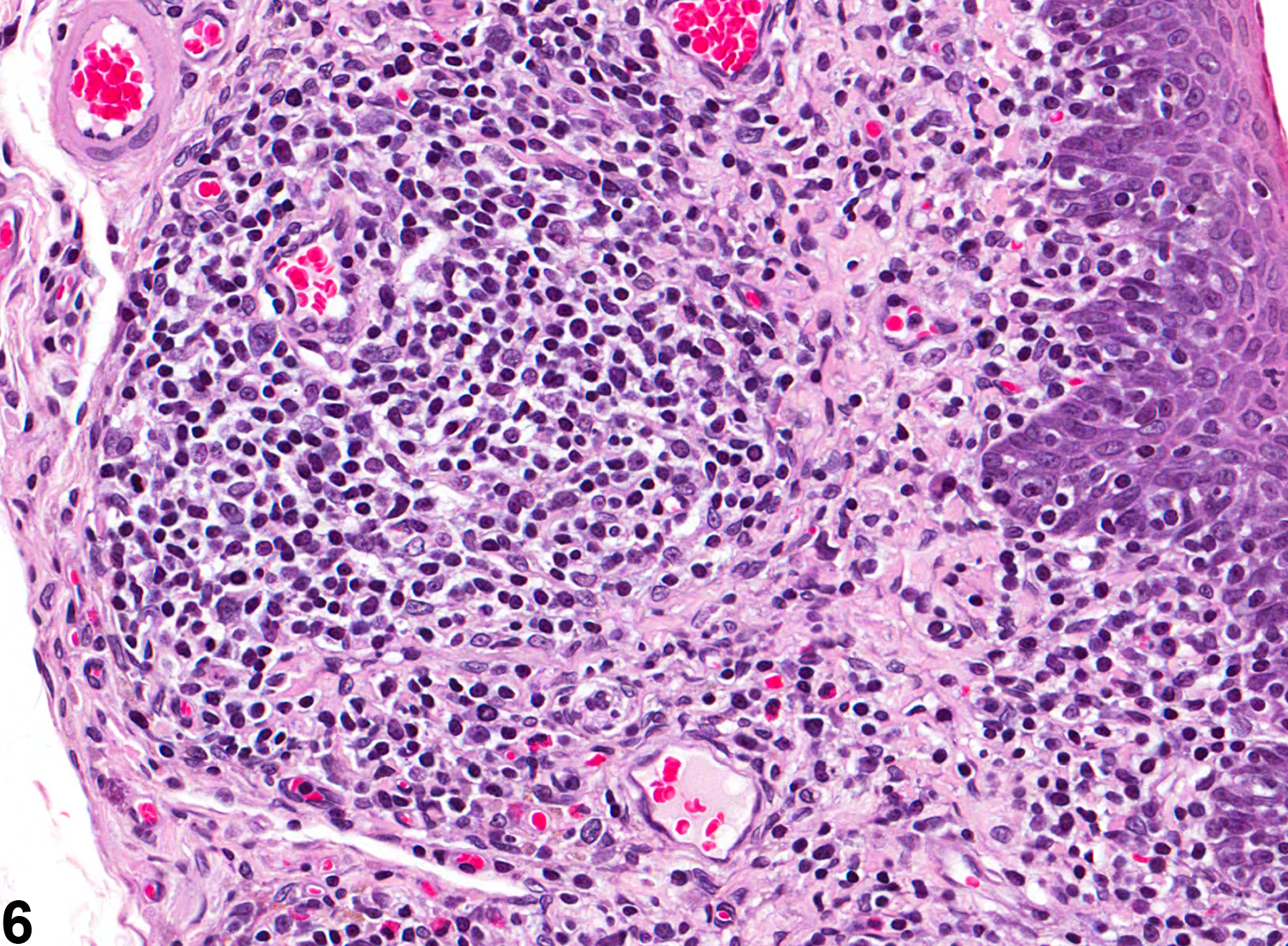
Esophagus - Inflammation
Narrative
Ackermann MR. 2007. Acute inflammation. In: Pathologic Basis of Veterinary Disease, 4th ed (McGavin MD, Zachary JF, eds). Mosby, St Louis, MO, 101-152.
Ackermann MR. 2007. Chronic inflammation and wound healing. In: Pathologic Basis of Veterinary Disease, 4th ed (McGavin MD, Zachary JF, eds). Mosby, St Louis, MO, 153-191.
Brown HR, Hardisty JF. 1990. Oral cavity, esophagus and stomach. In: Pathology of the Fischer Rat (Boorman GA, Montgomery CA, MacKenzie WF, eds). Academic Press, San Diego, CA, 9-30.
Abstract: https://www.ncbi.nlm.nih.gov/nlmcatalog/9002563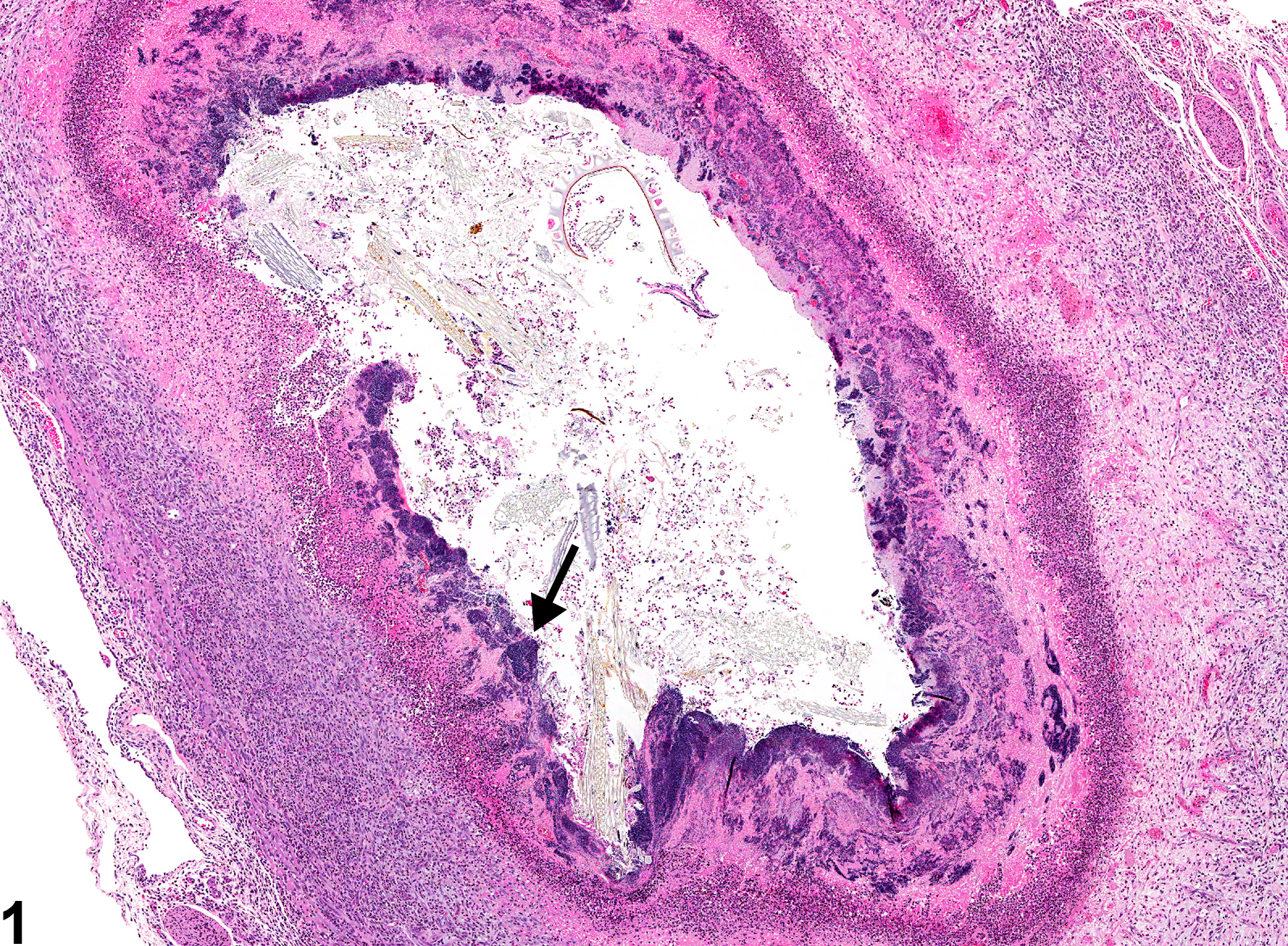
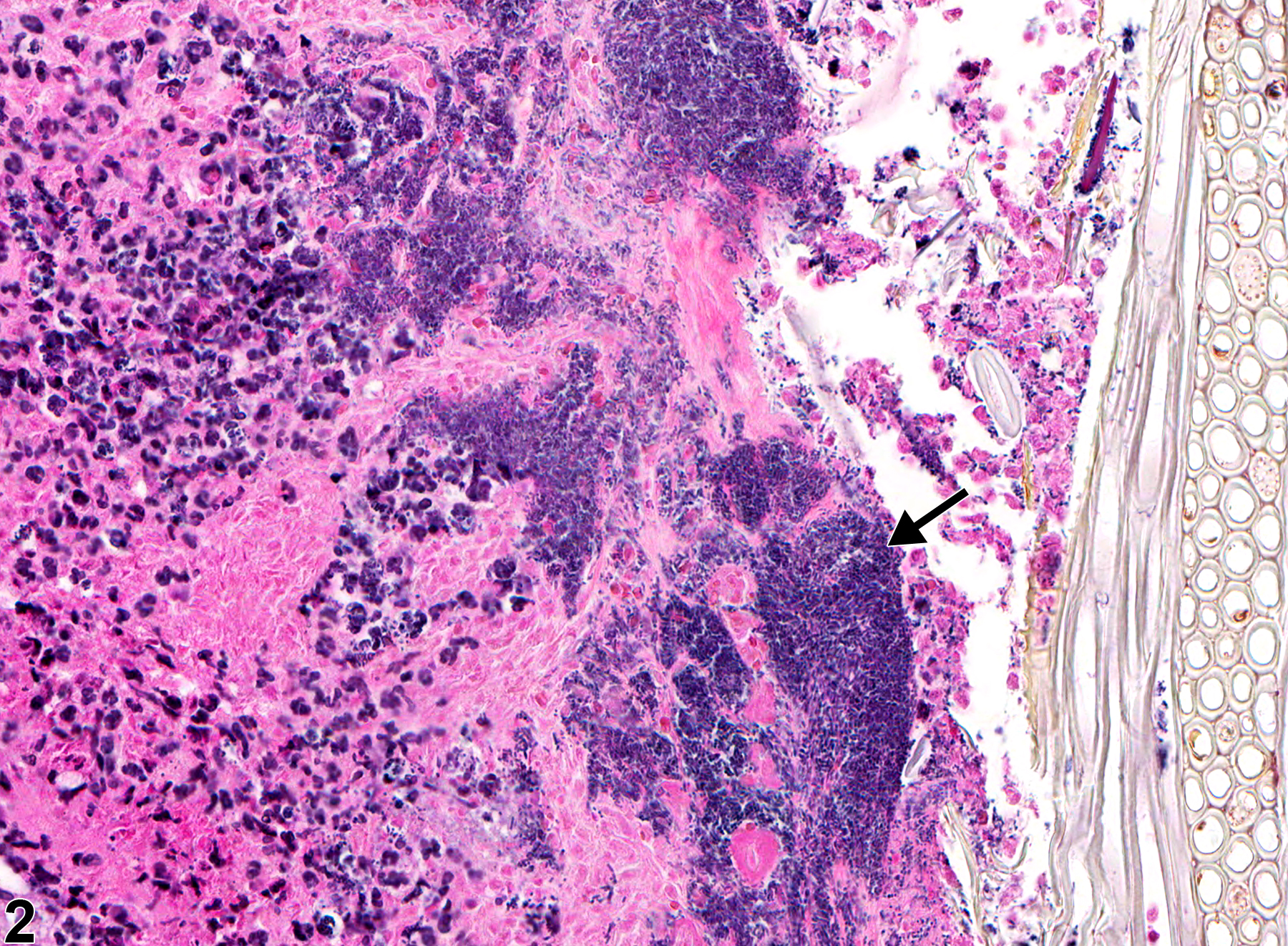
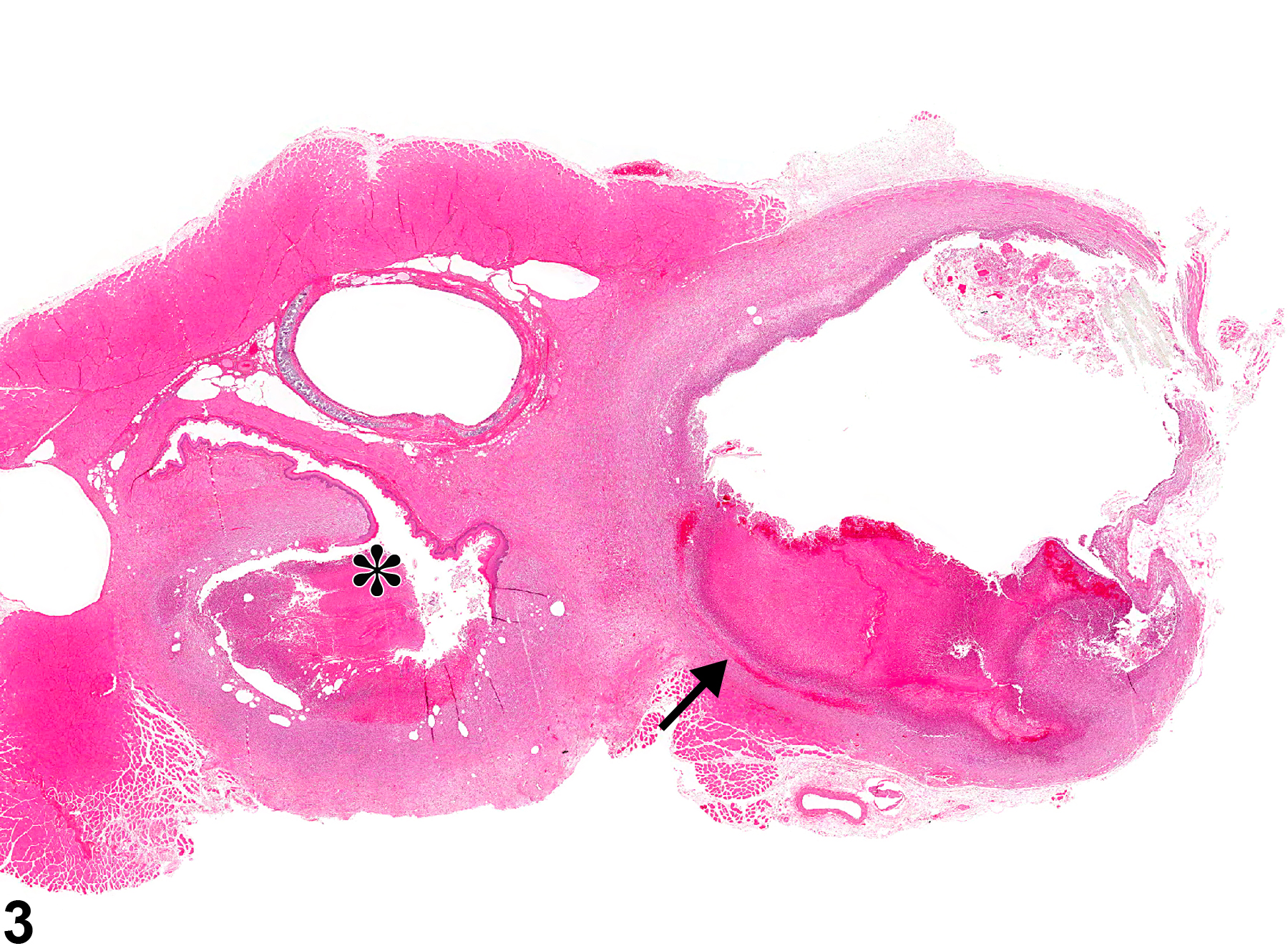
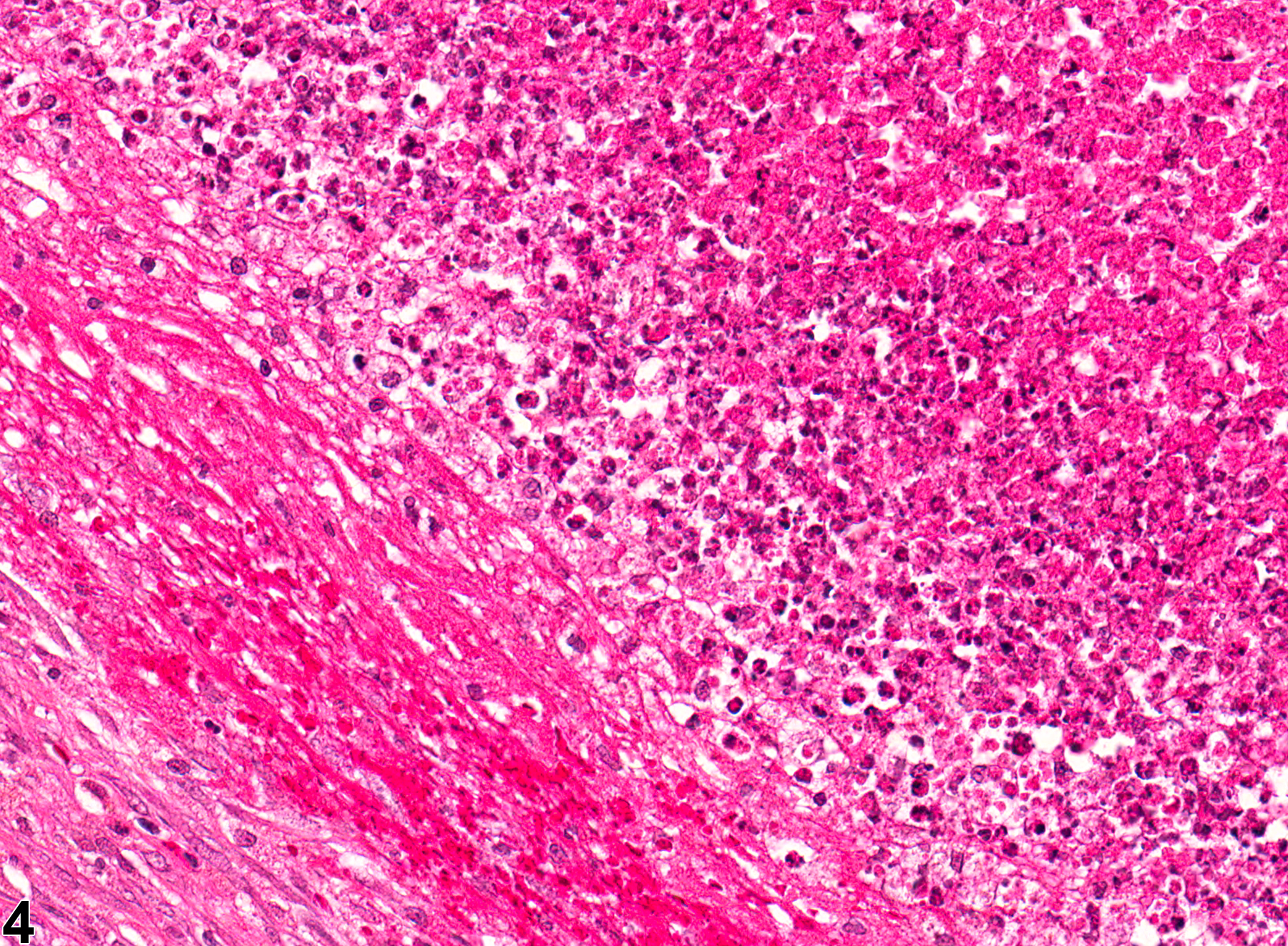
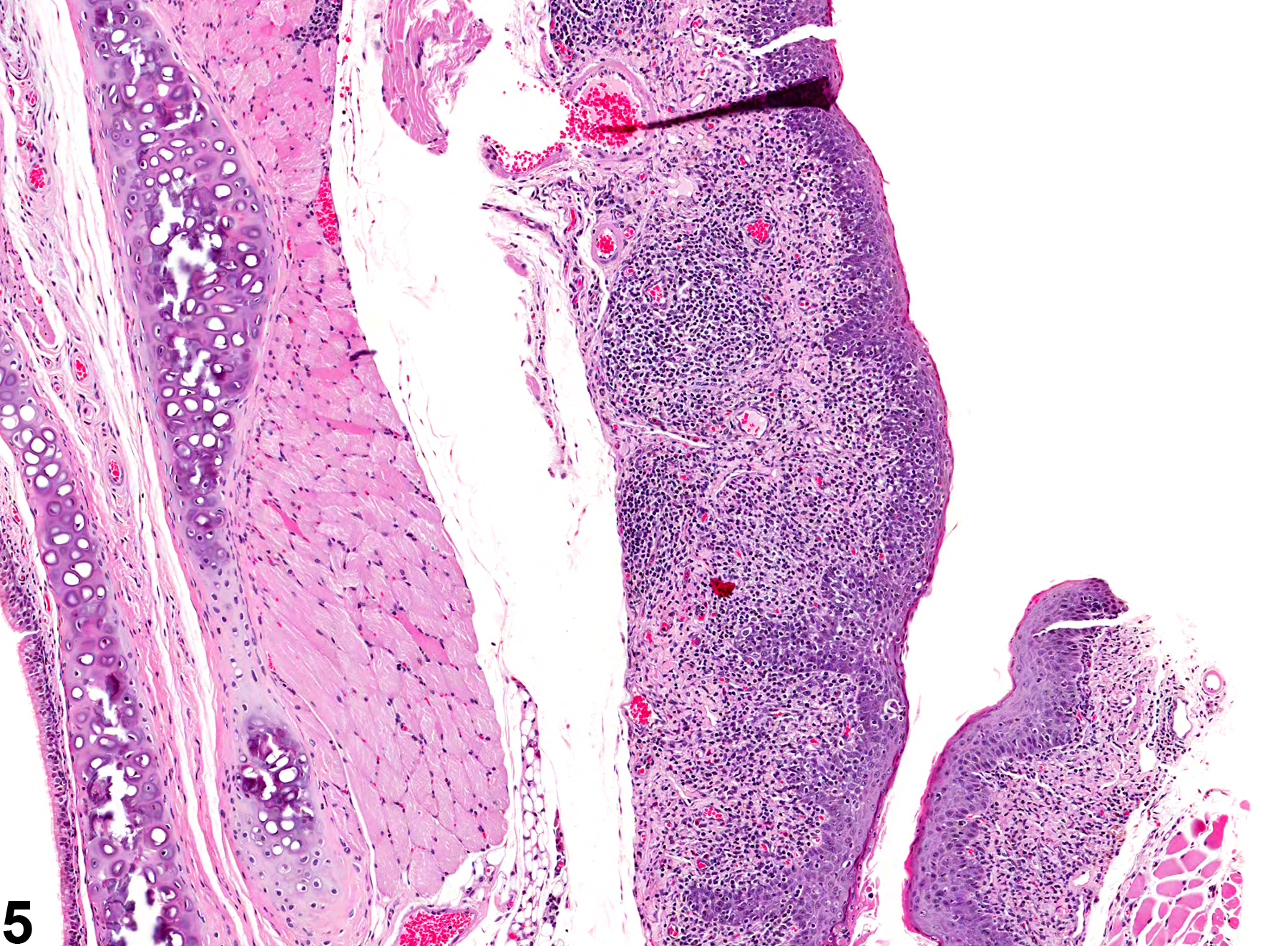
Esophagus - Inflammation, Suppurative in a female F344/N rat from a subchronic study. Note the bacterial colonies (arrow).