Immune System
Spleen - Hyperplasia, Plasma Cell
Narrative
Cesta MF. 2006. Normal structure, function, and histology of the spleen. Toxicol Pathol 34:455-465.
Full Text: http://tpx.sagepub.com/content/34/5/455.full.pdfElmore SA. 2006. Enhanced histopathology of the spleen. Toxicol Pathol 34:648-655.
Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1828535/Frith CH, Ward JM, Chandra M, Losco PE. 2000. Non-proliferative lesions of the hematopoietic system in rats. HL-1. In: Guides for Toxicologic Pathology. STP/ARP/AFIP, Washington, DC.
Matsuno K, Ezaki T, Kotani M. 1989. Splenic outer periarterial lymphoid sheath (PALS): An immunoproliferative microenvironment constituted by antigen-laden marginal metallophils and ED2-positive macrophages in the rat. Cell Tissue Res 257:459-470.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/2790931Mebius RE, Kraal G. 2005. Structure and function of the spleen. Nat Rev Immunol 5:606-616.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/16056254National Toxicology Program. 1999. NTP TR-488. Toxicology and Carcinogenesis Studies of 60-Hz Magnetic Fields in F344/N Rats and B6C3F1 Mice (Whole-Body Exposure Studies). NTP, Research Triangle Park, NC.
Abstract: https://ntp.niehs.nih.gov/go/10166Van Rees EP, Sminia T, Dijkstra CD. 1996. Structure and development of the lymphoid organs. In: Pathobiology of the Aging Mouse (Mohr U, Dungworth DL, Capen CC, Carlton WW, Sundberg JP, Ward JM, eds). ILSI Press, Washington, DC, 173-187.
Ward JM, Mann PC, Morishima H, Frith CH. 1999. Thymus, spleen, and lymph nodes. In: Pathology of the Mouse (Maronpot RR, ed). Cache River Press, Vienna, IL, 333-360.
Ward JM, Rehg JE, Morse HC III. 2012. Differentiation of rodent immune and hematopoietic system reactive lesions from neoplasias. Toxicol Pathol 40:425-434.
Abstract: https://www.ncbi.nlm.nih.gov/pubmed/22215512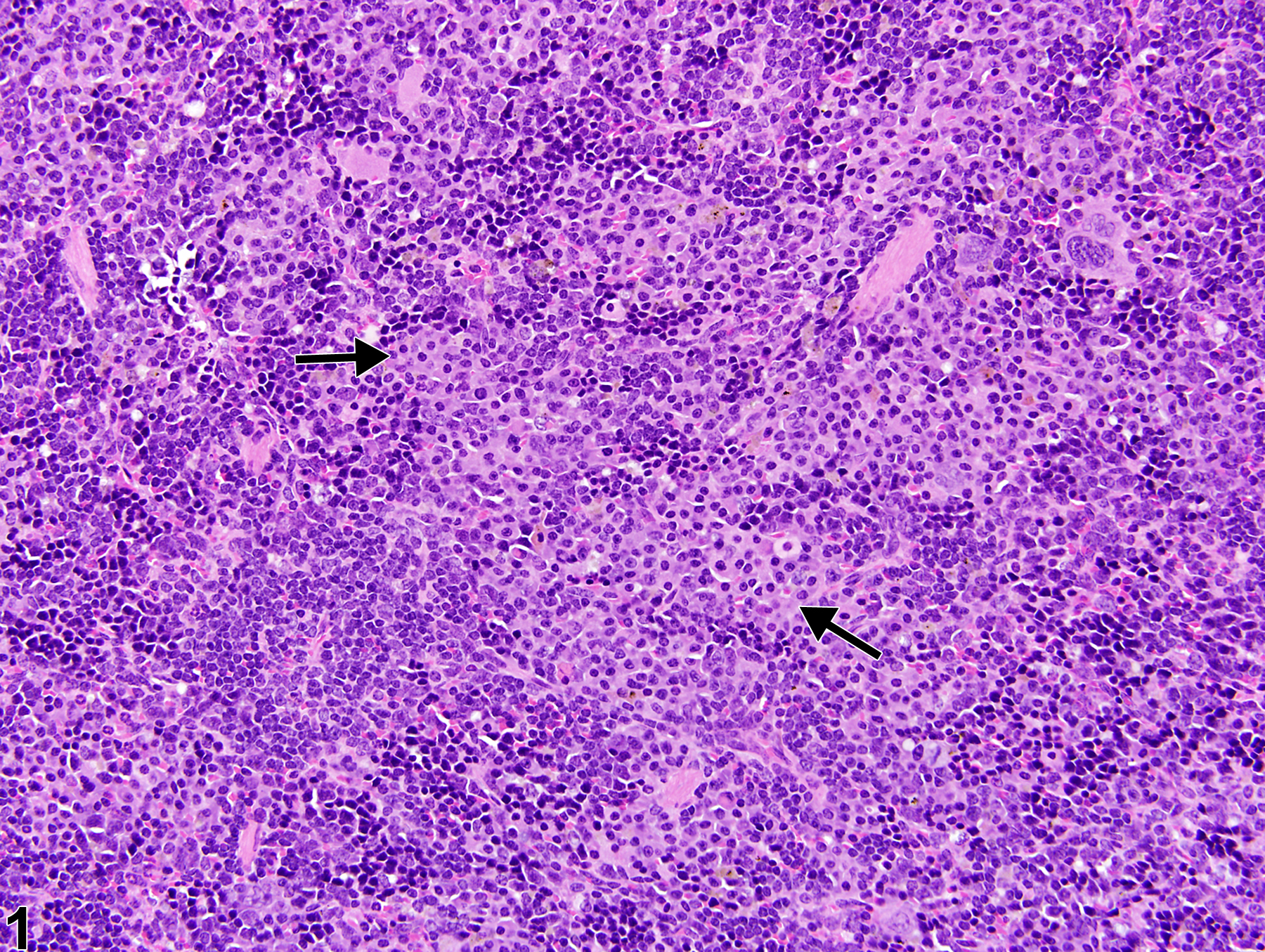
Spleen - Hyperplasia, Plasma cell in a female B6C3F1/N mouse from a chronic study. Small, multifocal aggregates of plasma cells (arrows) are present within the splenic red pulp.
All Images
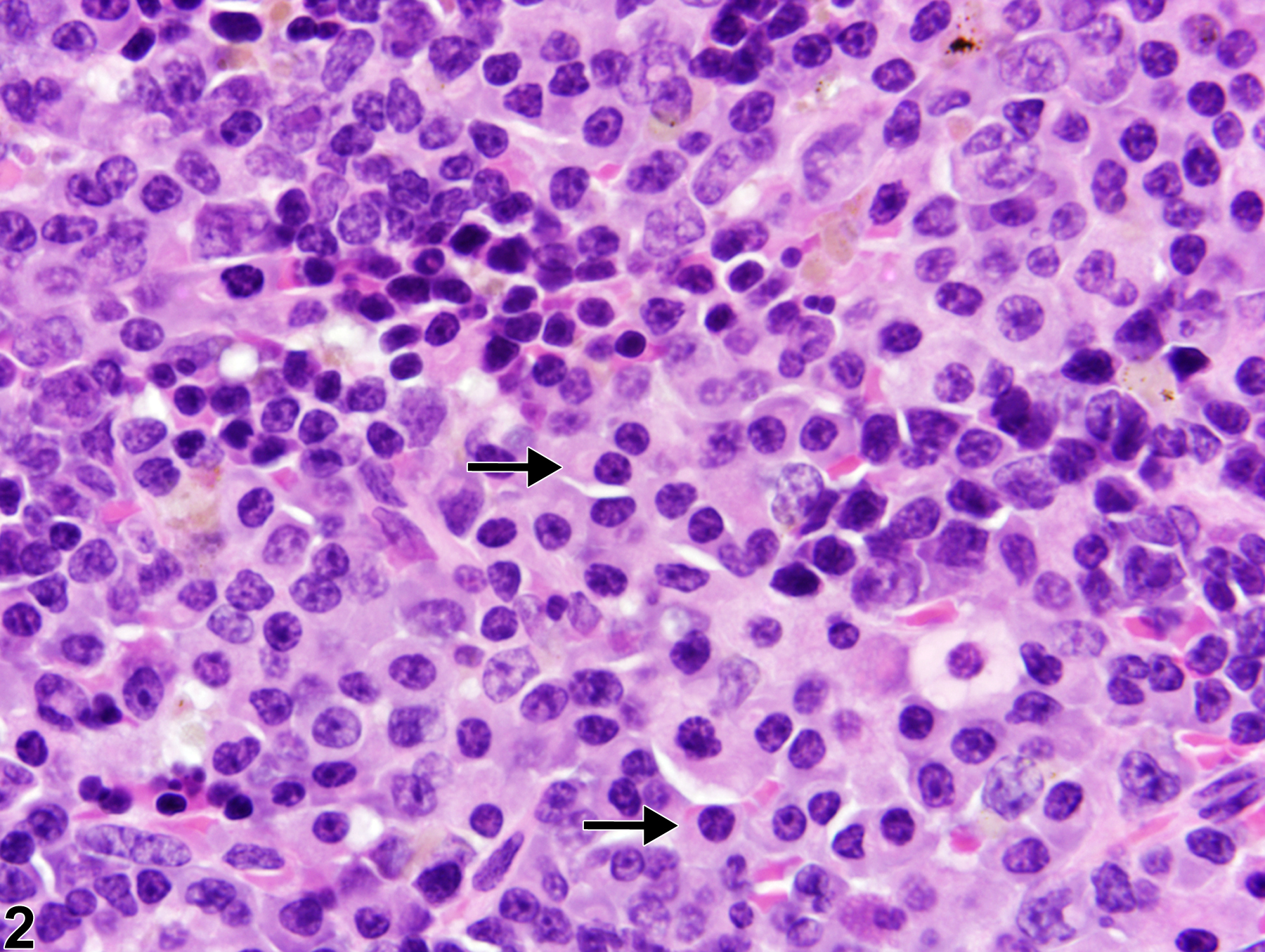
Spleen - Hyperplasia, Plasma cell in a female B6C3F1/N mouse from a chronic study (higher magnification of Figure 1). Plasma cells (arrow) are round to oval with a high nucleus-to-cytoplasm ratio, typically eccentric nucleus with heterochromatin in a characteristic cartwheel or clock face arrangement, and a pale perinuclear region with a Golgi apparatus.


