Integumentary System
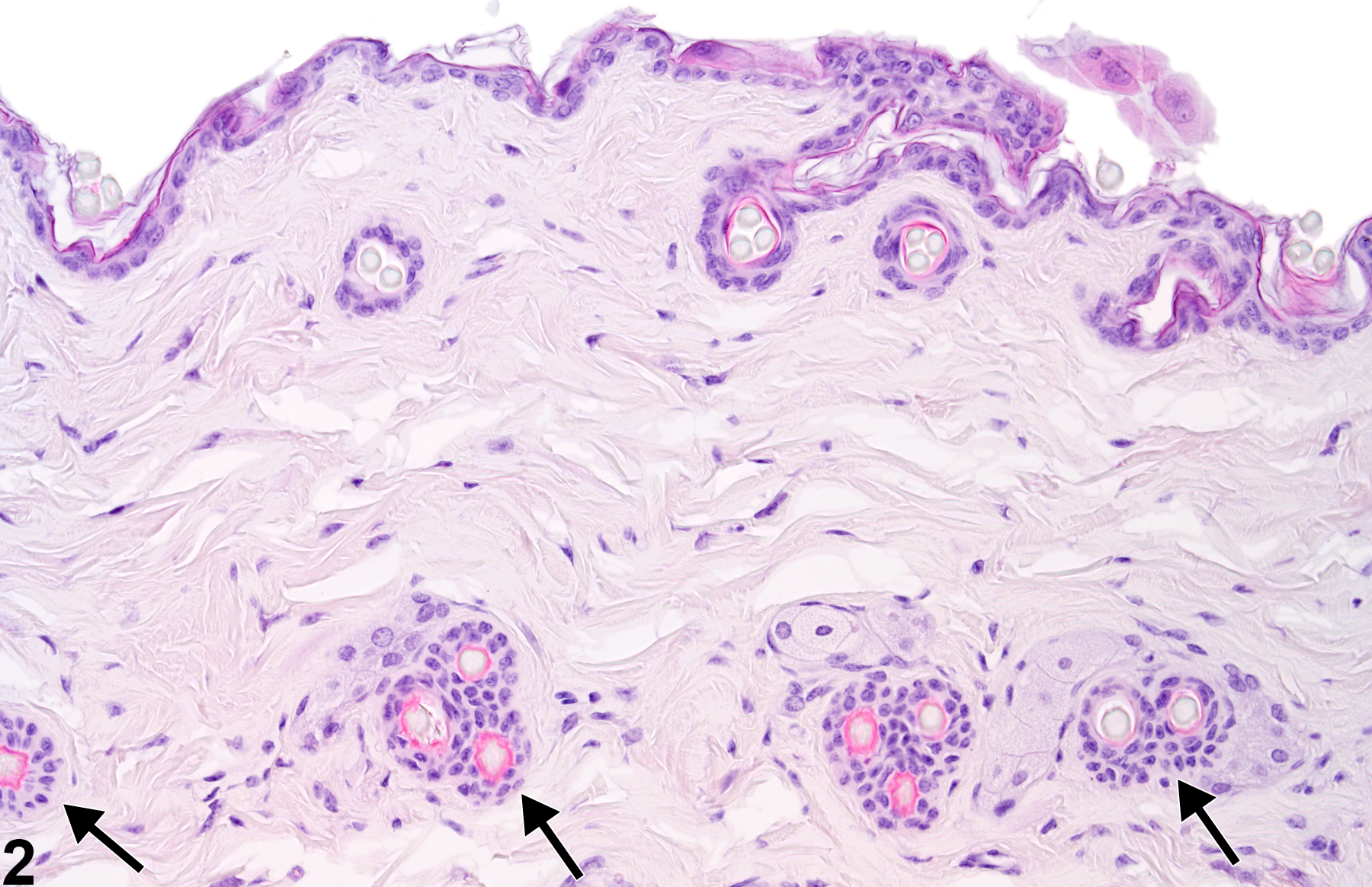
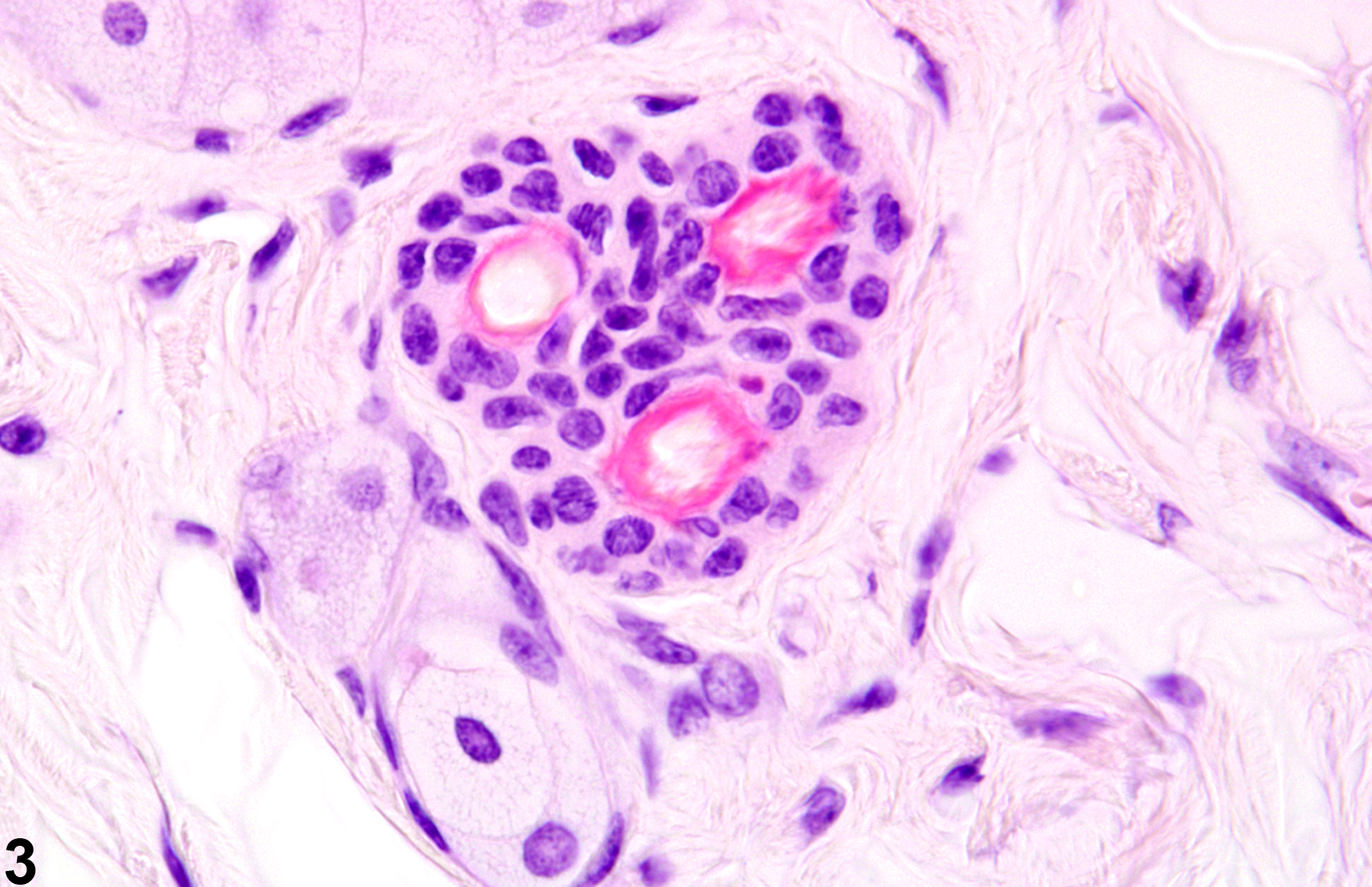
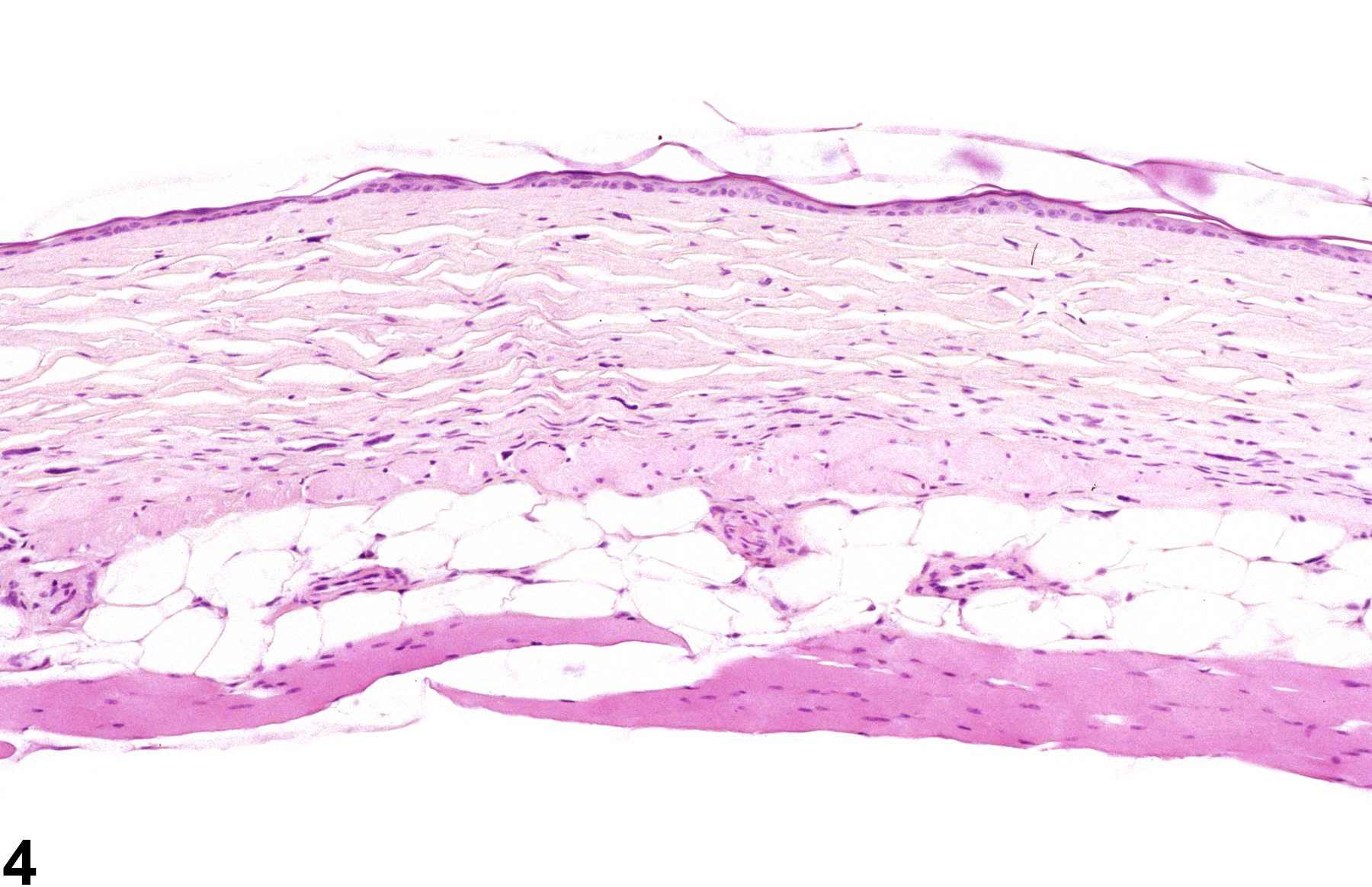
Skin - Atrophy
Narrative
The gross appearance of alopecia may be attributed to behaviors such as hair chewing or barbering, mechanical denuding due to rubbing against poorly constructed openings for feeders or water devices, parasitic infestations, and systemic diseases from hormonal (hypothyroidism) and nutritional imbalances. Some agents may affect a specific phase of the hair cycle, resulting in alopecia. For example, many chemotherapeutic agents interfere with the rapid mitotic activity of hair follicles in the anagen phase. Other compounds are known to affect hair follicles in the telogen phase, such as thallium, triparanol, and coumarin. Some compounds, such as phenyl glycidyl ether and dixyrazine, have effects on both the anagen and telogen phases. Follicles affected in a particular phase are likely to appear atrophied. Alopecia with atrophy or complete loss of hair follicles may also occur in skin over a subcutaneous or dermal neoplasm.
Elwell MR, Stedman MA, Kovatch RM. 1990. Skin and subcutis. In: Pathology of the Fischer Rat: Reference and Atlas (Boorman GA, Eustis SL, Elwell MR, Montgomery CA, MacKenzie WF, eds). Academic Press, San Diego, 261-277.
Abstract: https://www.ncbi.nlm.nih.gov/nlmcatalog/9002563Klein-Szanto AJP, Conti CJ. 2002. Skin and oral mucosa. In: Handbook of Toxicologic Pathology, 2nd ed (Haschek WM, Rousseaux CG, Wallig MA, eds). Academic Press, San Diego, 2:85-116.
Abstract: http://www.sciencedirect.com/science/book/9780123302151Peckham JC, Heider K. 1999. Skin and subcutis. In: Pathology of the Mouse: Reference and Atlas (Maronpot RR, Boorman GA, Gaul BW, eds). Cache River Press, Vienna, IL, 555-612.
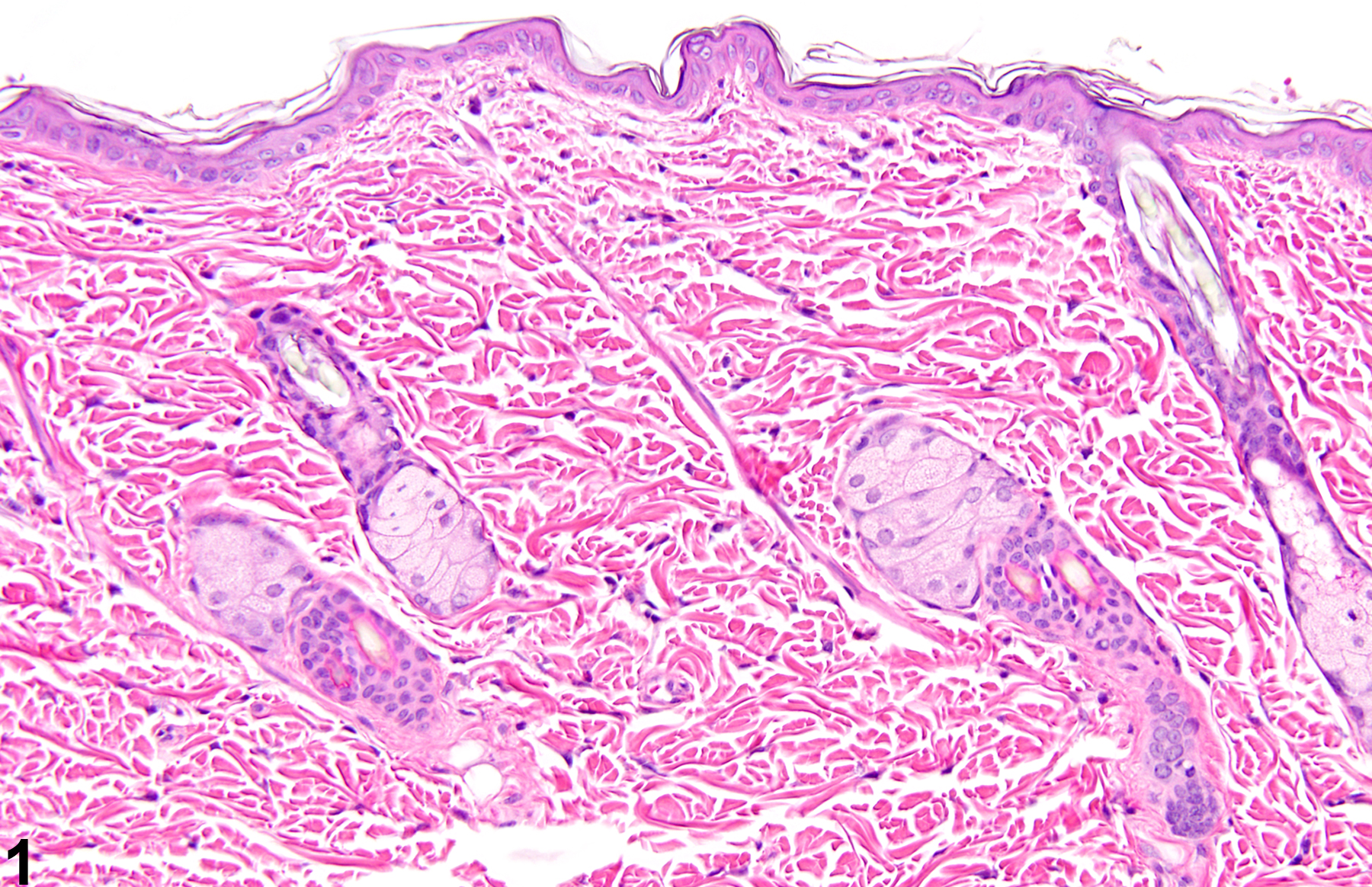
Normal skin in a control female F344/N rat from a 14-day repeated-dose study.